ABSTRACT
The coronavirus disease 2019 (COVID-19) pandemic prevented a group-based partial hospitalization program (PHP) from running in-person care due to social distancing guidelines. However, the crisis also simultaneously increased stress on families while decreasing their desire to hospitalize youth for a nonmedical issue. Hence, the need for a PHP remained high. Health care organizations worked diligently to create a secure telehealth platform (tele-PHP) to be delivered to patients in their home environments. This article describes the development and implementation of child and adolescent tele-PHPs in response to the COVID-19 pandemic. These new programs were started in mid-March 2020, and changes were implemented over the next 3 to 4 weeks. Overall, patients and families have been receptive to behavioral health services delivered through telemedicine. While tele-PHPs are the most plausible solution to continue behavioral health care for these patients, some challenges were observed during this process. Besides procedural and technological challenges associated with creating a virtual setup, other difficulties include variable patient engagement, specific treatment-related challenges, and system-related changes. These challenges are addressed through psychoeducation, provision of online measures to assess treatment outcomes, and efforts to optimize parent engagement prior to treatment initiation for better treatment adherence. Initial experiences during a time of crisis suggest that tele-PHP services can be a viable long-term treatment option in the future during both a disaster and routine times to improve access for those who otherwise cannot take advantage of such services. Long-term effectiveness of these interventions still needs to be explored.

Development of a Child and Adolescent Tele-Partial Hospitalization Program (tele-PHP) in Response to the COVID-19 Pandemic
ABSTRACT
The coronavirus disease 2019 (COVID-19) pandemic prevented a group-based partial hospitalization program (PHP) from running in-person care due to social distancing guidelines. However, the crisis also simultaneously increased stress on families while decreasing their desire to hospitalize youth for a nonmedical issue. Hence, the need for a PHP remained high. Health care organizations worked diligently to create a secure telehealth platform (tele-PHP) to be delivered to patients in their home environments. This article describes the development and implementation of child and adolescent tele-PHPs in response to the COVID-19 pandemic. These new programs were started in mid-March 2020, and changes were implemented over the next 3 to 4 weeks. Overall, patients and families have been receptive to behavioral health services delivered through telemedicine. While tele-PHPs are the most plausible solution to continue behavioral health care for these patients, some challenges were observed during this process. Besides procedural and technological challenges associated with creating a virtual setup, other difficulties include variable patient engagement, specific treatment-related challenges, and system-related changes. These challenges are addressed through psychoeducation, provision of online measures to assess treatment outcomes, and efforts to optimize parent engagement prior to treatment initiation for better treatment adherence. Initial experiences during a time of crisis suggest that tele-PHP services can be a viable long-term treatment option in the future during both a disaster and routine times to improve access for those who otherwise cannot take advantage of such services. Long-term effectiveness of these interventions still needs to be explored.
Prim Care Companion CNS Disord 2020;22(5):20m02743
To cite: Baweja R, Verma S, Pathak M, et al. Development of a child and adolescent tele-partial hospitalization program (tele-PHP) in response to the COVID-19 pandemic. Prim Care Companion CNS Disord. 2020;22(5):20m02743.
To share: https://doi.org/10.4088/PCC.20m02743
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry and Behavior Health, Penn State University College of Medicine, Hershey Pennsylvania
bPennsylvania Psychiatric Institute, Harrisburg, Pennsylvania
cDepartment of Psychiatry and Behavioral Health, Rosalind Franklin University of Medicine and Science, North Chicago, Illinois
dRogers Behavioral Health, Kenosha, Wisconsin
*Corresponding author: Shikha Verma, MD, Rogers Behavioral Health, 9916 75th St #205, Kenosha, WI 53142 ([email protected]).
The continuum of acute pediatric behavioral health care ranges from inpatient stabilization, wherein patients receive 24/7 supervised care, to outpatient settings. However, a sizable subset of youth does not meet inpatient admission criteria, yet need more than weekly outpatient visits. Children and adolescent partial hospitalization programs (PHPs) are that next step, falling between inpatient hospitalization and outpatient treatment and providing care in the least restrictive settings. PHPs offer 6 hours of an intensive group therapy-based program 5 days per week, typically lasting for 2-4 weeks. Content is tailored for children and adolescents 6-18 years of age and includes individual, family, and experiential/art therapy and psychiatry/medication management services.1
In response to the coronavirus disease 2019 (COVID-19) pandemic, all nonessential medical visits were placed on hold during the transition to telemedicine. However, the pandemic increased stress for families, ranging from financial to medical needs, with the additional burden on parents to supervise their child’s education. Furthermore, social distancing guidelines limited access to peers, healthy activities, and, in many cases, professional services such as wraparound and other family based services. Natural disasters are associated with increased rates of anxiety, depression, and illicit substance use.2,3 Even in the absence of a pandemic, mental health and substance use disorders are the leading cause of disability in youth.4 These associations are likely to only strengthen during the pandemic.
At the beginning of the COVID-19 crisis, schools were abruptly closed to mitigate the spread of infection before e-learning curriculums could be developed. Along with depriving youth of essential social and educational components, school closures also resulted in considerable unstructured time at home. For adolescents, these changes may increase uncertainties about major life milestones, including graduation, college applications, leaving their parents to live independently, employment, and maintaining dating and other social relationships. For almost all youth, the closure of schools has also markedly increased screen time, particularly social media use, decreased exercise, and most likely led to highly variable sleep patterns, all of which are risk factors for mental illness.5-7 For younger children, school closures markedly increased commands that parents had to make every day, as they now absorbed responsibility for education and daytime supervision of their children. Each command can be a potential trigger for anger outbursts. These outbursts are one of the main reasons parents seek mental health care for a child.8 At the same time, many parents were attempting to work from home with a similar abrupt transition as that of their child’s education, while also facing a wide variety of increased stressors and reduced supports. Furthermore, the closing of schools reduced access to school-based mental health programs.
Over a period of a few weeks, almost all medical care transitioned to telemedicine.9,10 Fortunately, there is a long track record of providing behavioral health services through telemedicine.11,12 It has been very helpful to address the unmet mental health needs of the community and provide improved access to care, and parents have expressed high satisfaction with telemedicine services.13,14 However, almost all telemedicine for behavioral health has been done in outpatient settings.
PHP is a group-based service. With stay-at-home or shelter-in-place orders, services could not be continued as is. PHPs have a strong family therapy component and require weekly face-to-face family meetings. Both group and family therapy can be more challenging to transition to teleformats than individual therapy. Given these barriers, there had been very limited experience with virtual PHPs prior to the pandemic. The abruptness and scope of the pandemic greatly increased the challenge of creating secure platforms to provide quality behavioral health care in a PHP. In this article, we discuss the development of child and adolescent tele-PHPs in 2 US states: 1 program from an academic setting in Pennsylvania and another from a community-based setting in Wisconsin.
NEW VIRTUAL SETUP
Prior to the COVID-19 pandemic, PHPs included up to 8 children and 32 adolescents with 22 staff. As mentioned previously, PHPs offer 6 hours of intensive group therapy, including 1 1/2 hours of an educational program 5 days per week usually for 2-4 weeks. We present our transition to a virtual platform as an example for other programs that may be considering or are in the midst of such a transition. These new programs were started in mid-March, and changes were implemented over the next 3 to 4 weeks.
First Week
The first step was to obtain the necessary approval of the HIPPA-compliant virtual platform (Zoom/Webex/Microsoft Teams) from the regulatory committees, including information technology, compliance, health information services, and medical group, in our health system.
To ease the transition and to develop policies, we transitioned only follow-up/continued care of patients being discharged from our inpatient facilities, as they were already established in the system. New intakes were evaluated in person by the therapist and psychiatrist on the same day, as the staff was onsite to receive training for the virtual platform.
The next step was to create a workflow to confirm parents’ or patients’ e-mail addresses and to have families download the specific apps on their devices. These platforms were selected due to ease of setup, and little formal training was needed. Families could easily log in by clicking on the link shared by the treatment team. The virtual platform was started as a pilot to run the group (8 adolescents) for 2 hours. Individual links had to be created for each hourly group and for appointments with a team member. Individual links worked well for group therapy. However, at times the family member would also join with the patient, raising concerns about the confidentiality of the group, and families needed reminders that only the patient should be present in group settings.
These specific platforms have additional benefits such as virtual waiting room options, wherein the family can log in to the system in advance, and treatment team members can connect them at the scheduled appointment time. However, the virtual platforms had another challenge: unexpected "call drop/ended" because of connectivity or other technical issues, and families would at times become frustrated waiting in the virtual waiting room if an earlier appointment lasted longer than expected, as they had no estimate of when theirs would begin.

- The COVID-19 pandemic has negatively impacted mental health and prevented a group-based partial hospitalization program (PHP) from running in-person care due to social-distancing guidelines.
- Tele-PHPs for children and adolescents during the COVID-19 pandemic improved access to care and provided behavioral health care services to those in need in their homes.
- Tele-PHP services can be a viable long-term treatment option during emergencies and routine times to improve access to care.
We were able to implement the same content for the psychotherapy and psychoeducational groups, so it may not be necessary to create a new format for tele-PHPs. However, art and music therapy group activities were modified so that they could easily be done at home. Medication management and discharge meetings have similar formats except for the inability to perform vitals and clinician-administered examinations such as the Abnormal Involuntary Movement Scale.15 Patients were asked weekly if they had muscle stiffness, tremors, or any abnormal tongue movements. A body weight scale was provided to those families who did not have one at home so that they could track their child’s weight weekly. During the week, if parents needed to communicate concerns with the treatment team, they were able to contact team members by phone.
Crisis intervention plans were also implemented from the beginning of the transition to tele-PHP and were discussed with families in detail. If a patient did not join the program in the morning or logged out unexpectedly, the assigned treatment team member made 2 attempts to reach the parents in the next hour. If parents did not respond within 30 minutes of the second phone call, local crisis intervention teams were notified. If a patient expressed safety concerns during group or individual sessions, the treatment team completed risk assessments, and parents were notified. If the treatment team and families agreed about the need for a higher level of care, the availability of beds was determined in nearby inpatient hospitals, and transfers were facilitated once patients were accepted. If there were safety concerns with patients but families did not agree with the treatment team’s recommendations about a higher level of care, local crisis intervention teams were notified.
Second Week
Patient care was completely transferred to the virtual platform by the second week, including new intakes, and we also started enrolling new patients from the community. Over time, incremental adaptations to the program were made. For example, elementary program hours were reduced from 6 hours to 1 hour daily because children were unable to sit in place for a longer duration. The adolescent curriculum decreased to 4 hours daily after feedback from parents and adolescents that it was challenging for youth to stay focused online for 6 hours.
Before COVID-19, most outcome measures were done on paper with staff present. By the end of the second week, electronic measures were integrated. Freely available instruments like the 9-item Patient Health Questionnaire16 and Vanderbilt ADHD Diagnostic Parent Rating Scale17 were attached with intake links.18 These rating scales were directly connected with electronic databases. The rate of scale completion did decline due to a mix of technological barriers and perceived burden of completing ratings at home. From the second week, 1-hour weekly virtual family sessions were resumed with patients, families, and the treatment team to discuss patients’ progress, challenges in treatment, and aftercare.
Third Week Onward
Before COVID-19, urine drug screening was usually completed every other week and as needed for youth with co-occurring mental health and substance use. As urine drug screening now could not be completed, from the third week onward saliva swab drug tests were mailed to patients. To maintain the fidelity of treatment, nurses are trained to observe patients for 10 minutes during the telesession while the swab test is completed, and results are documented.
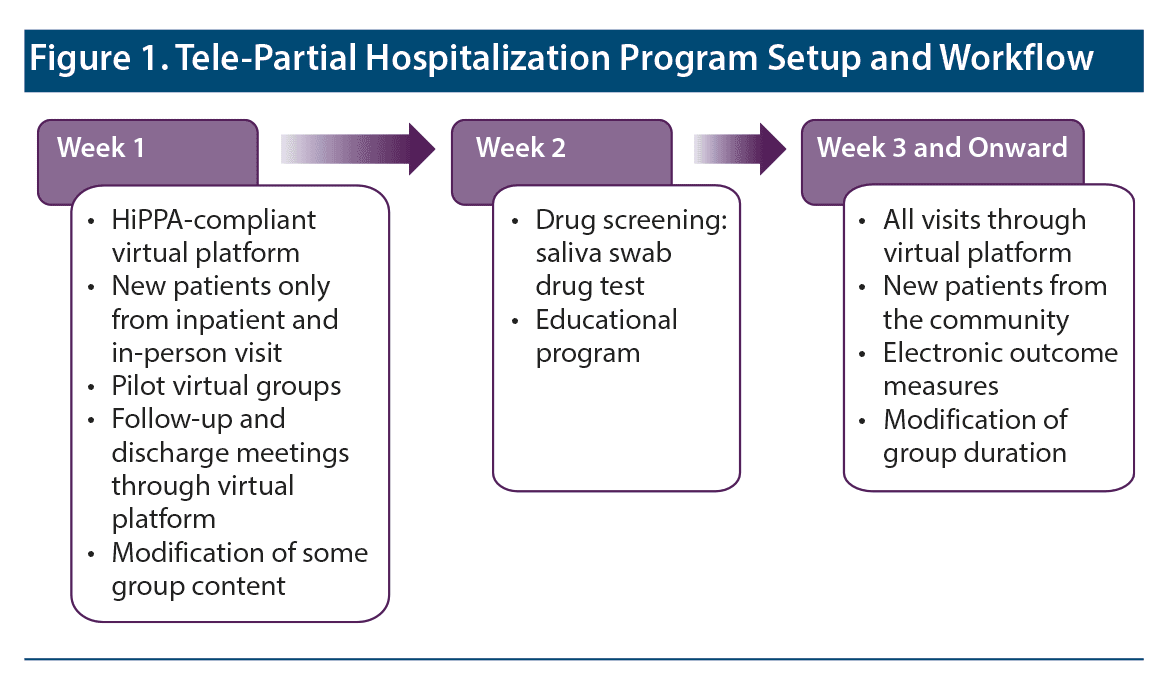
One hour of a modified education program per day was also introduced as local schools started distant learning. School liaison staff provided instruction to the patients through the virtual platform. Figure 1 provides an overview of the tele-PHP setup and workflow in weeks 1-3.
Challenges in Operations
Patient-related factors. Over the first few weeks, patient-related barriers were identified, including the strength of internet connection, technological fluency of families, patients’ and parents’ understanding of the new treatment flow, and logging in on time for scheduled sessions.
The major barrier was creating sufficient engagement with patients. Many patients referred for partial treatment already had limited motivation for care. This lack of motivation proved to be more challenging compared to when all sessions occurred face to face for a variety of reasons. As schools were closed, the youth had lapses in their daily schedule and sleep hygiene as they were no longer required to be up by certain times, so early start times proved problematic. Even when the youth did log on in time for sessions, participation varied significantly as some noticeably disengaged, logged on to other devices simultaneously, were inactive during in-group meetings, turned off their videos, or logged off from the groups. Both early starts and extended on-screen treatment hours were the best predictors of poor engagement. These challenges were greatest for children versus adolescents. Some patients requested early discharge because they did not find virtual groups to be effective.
As the process started becoming more familiar to existing patients, the following groups went more smoothly. New patients joining the program introduced significant unpredictability, as there was a bit of a contagion effect for disengagement (ie, if one patient was disengaged, the engagement for others declined as well). Therefore, several changes were implemented to optimize engagement and were started at the time of assessment and continued throughout treatment. These changes included using components of motivational enhancement therapy for the adolescent group.19 We found that offering parents training along with conflict resolution, using components of multifamily psychoeducational psychotherapy,20 and assisting with structuring home routines early in treatment helped parents both with scheduling and getting their child to log in to tele-PHP appointments. Multiple psychosocial interventions could be implemented such as working with parents to create daily home rewards to incentivize participation.
Adolescents had no difficulties setting up the technology. However, children needed help from parents to log in every day and throughout the day whenever they had to move to different links or encountered poor connectivity, which added additional stress for parents who were also trying to work from home. At times, adolescents were attending telesessions in the common areas of the house and family members would walk in during the session. Therefore, teleprivacy rules were reviewed at intake, and families were reminded periodically so that confidentiality would be maintained.
Therapy-related challenges. For patients with obsessive-compulsive disorder and other anxiety disorders, exposure and response prevention-based programs are a core component of treatment. For some patients, identification of in vivo exposures at home that were feasible and sufficiently challenging was difficult. Others struggled to engage in more anxiety-provoking exposures without staff physically present to prompt participation. Moreover, exposures related to contamination fears such as resisting hand-washing restrictions needed to be modified in light of prevention guidelines. An exposure hierarchy was modified on a case-by-case basis.
The inability to create a therapeutically intensive exposure hierarchy was common for socially anxious youth. Most of their challenging exposures do not occur at home, and with school closures, their impairment was acutely reduced. In such cases, motivation was greatly reduced, and premature discontinuation was more common. However, for those who were motivated at program entry, group participation did improve social anxiety.
Practice-Based Learning
Prescriptions. Before COVID-19, patients would be discharged with a 30-day medication supply and an appointment with an ambulatory provider within a month. The program increased care coordination efforts by utilizing staff who had reduced demands due to the virtual transition to ensure that patients had follow-up appointments with their outpatient providers at the time of discharge. Due to outpatient clinics placing limits on new patients during the transition to telemedicine, prior discharge policies were modified. All patients were given up to 90-day prescriptions, except for controlled substances, which allowed only 30 days at a time with no refills. Families were advised to call for a refill of controlled substances before running out.
Licensure restrictions. One of the license requirements is that physicians should have a license from the states wherein they see patients. With the tele-PHP setup, patients from other states could not be enrolled in the program. Therefore, it is important to have centralized billing and licensure support to keep abreast of rapid policy changes. Most states acted quickly and allowed providers to see patients in other states. Fast-track temporary licensure services are also provided by some states. However, similar reciprocal relaxations have not occurred for therapists and behavioral specialists in some states, who are core team members for this level of care. Patients from the same state continued to participate in the tele-PHP, while patients from other states were transferred to their respective state’s PHP.
FUTURE CONSIDERATIONS
Although patients and families have expressed overall satisfaction with telemedicine services in the past,12 physicians have used this mode of treatment conservatively. Studies21,22 have shown that after long-term use, more physicians felt comfortable about delivering care through telemedicine. Therefore, we expect a similar trajectory for PHPs, but these outcomes would depend on telemodels continuing after the pandemic. In our experience, the telemodels worked best for patients who have reliable internet services, are technology savvy, have optimal supervision at home, are adolescents, and are motivated for and comfortable with group therapy. One of the main challenges was poor patient engagement related to extended on-screen treatment hours, thus future programs should consider brief 1- to 2-hour sessions twice a day for children and adolescents. Therefore, it may be advisable to assess these variables at intake and focus post-pandemic telehealth efforts on these subgroups. However, even these focused efforts would require the continuation of several of the telehealth policy changes that were made during the pandemic. Moreover, some commercial payers do not cover telemedicine or cost reimbursed is not enough for sustaining infrastructural costs.22 Therefore, advocacy for policies promoting teleservices will be an essential component of future efforts to expand access. Additionally, the tele-PHP could be used as an initial step in the exposure hierarchy for socially anxious youth or those patients with autism spectrum disorder, who have significant challenges in new settings.
Telemedicine has been shown to be an effective way to provide psychiatric services to rural and remote clients.13 Telesessions reduce travel burdens and allow the continuation of services when transportation is a barrier. Therefore, future models may want to consider integrating face-to-face and telemodalities for both planned and unplanned issues. Giving families options to pick the treatment modality and method of communication improves engagement.22 However, there are no data on hybrid tele/face-to-face models for PHPs.
CONCLUSIONS
Over the last 2 decades, there have been multiple endemic, international health emergencies, with the COVID-19 pandemic being one of the largest in recent history.23 It is likely that the pandemic will resolve gradually and unpredictably with potential recurrences along the way. Therefore, there is a high likelihood that traditional PHP services will not be practical for an extended time. Even when we return patient care from home to the clinic, modifications will most likely be necessary. Models feasible for this pandemic will likely have broad applicability to a range of health emergencies, which are known to have a negative impact on the mental health of the masses. The benefits of telemedicine will not fade even if future disasters fail to manifest, as there is extensive research supporting the advantages of telemedicine for the treatment of mental health disorders in outpatient settings.24 Tele-PHPs should be considered as a sustainable long-term solution for care, both in periods of crisis and tranquility.
The adaptability of the health care system during a time of very high stress to develop novel and feasible care models is truly impressive. This real-time testing of a significant portion of health care moving to virtual platforms provided clear insight that efficient lifesaving care can be delivered without direct patient contact. For all these reasons, it is prudent to continue to develop telemodels for high-quality PHP care for children and adolescents who could be at the brink of decompensation. The good news is that it should be much easier to develop models during periods of economic and health stability as long as we do not forget the lessons learned during crises.
Submitted: July 7, 2020; accepted July 23, 2020.
Published online: October 15, 2020.
Potential conflicts of interest: Dr Waxmonsky has received research funding from National Institutes of Mental Health, Supernus, and Pfizer. Drs Baweja, Verma, and Pathak report no conflicts of interest related to the subject of this article.
Funding/support: None.
REFERENCES
1.Milin R, Coupland K, Walker S, et al. Outcome and follow-up study of an adolescent psychiatric day treatment school program. J Am Acad Child Adolesc Psychiatry. 2000;39(3):320-328. PubMed CrossRef
2.Kessler RC, Galea S, Jones RT, et al; Hurricane Katrina Community Advisory Group. Mental illness and suicidality after hurricane Katrina. Bull World Health Organ. 2006;84(12):930-939. PubMed CrossRef
3.Thienkrua W, Cardozo BL, Chakkraband ML, et al; Thailand Post-Tsunami Mental Health Study Group. Symptoms of posttraumatic stress disorder and depression among children in tsunami-affected areas in southern Thailand. JAMA. 2006;296(5):549-559. PubMed CrossRef
4.Erskine HE, Moffitt TE, Copeland WE, et al. A heavy burden on young minds: the global burden of mental and substance use disorders in children and youth. Psychol Med. 2015;45(7):1551-1563. PubMed CrossRef
5.Boers E, Afzali MH, Newton N, et al. Association of screen time and depression in adolescence. JAMA Pediatr. 2019;173(9):853-859. PubMed CrossRef
6.Gregory AM, Sadeh A. Annual research review: sleep problems in childhood psychiatric disorders—a review of the latest science. J Child Psychol Psychiatry. 2016;57(3):296-317. PubMed CrossRef
7.Huang Y, Li L, Gan Y, et al. Sedentary behaviors and risk of depression: a meta-analysis of prospective studies. Transl Psychiatry. 2020;10(1):26. PubMed CrossRef
8.Safer DJ. Irritable mood and the diagnostic and statistical manual of mental disorders. Child Adolesc Psychiatry Ment Health. 2009;3(1):35. PubMed CrossRef
9.Smith AC, Thomas E, Snoswell CL, et al. Telehealth for global emergencies: implications for coronavirus disease 2019 (COVID-19). J Telemed Telecare. 2020;26(5):309-313. PubMed CrossRef
10.Zhou X, Snoswell CL, Harding LE, et al. The role of telehealth in reducing the mental health burden from COVID-19. Telemed J E Health. 2020;26(4):377-379. PubMed CrossRef
11.Swanson CL, Trestman RL. Rural assertive community treatment and telepsychiatry. J Psychiatr Pract. 2018;24(4):269-273. PubMed CrossRef
12.Salmoiraghi A, Hussain S. A systematic review of the use of telepsychiatry in acute settings. J Psychiatr Pract. 2015;21(5):389-393. PubMed CrossRef
13.Griffiths L, Blignault I, Yellowlees P. Telemedicine as a means of delivering cognitive-behavioural therapy to rural and remote mental health clients. J Telemed Telecare. 2006;12(3):136-140. PubMed CrossRef
14.Myers KM, Valentine JM, Melzer SM. Child and adolescent telepsychiatry: utilization and satisfaction. Telemed J E Health. 2008;14(2):131-137. PubMed CrossRef
15.Guy W. ECDEU Assessment Manual for Psychopharmacology: Revised (DHEW publication number ADM 76-338). Rockville, MD, US Department of Health, Education and Welfare, Public Health Service, Alcohol, Drug Abuse and Mental Health Administration, NIMH Psychopharmacology Research Branch, Division of Extramural Research Programs, 1976: 534-7
16.PHQ9. L Spitzer RL, Kroenke K, Williams JB, Patient Health Questionnaire Primary Care Study Group. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. JAMA. 1999;282(18):1737-1744. PubMed
17.Wolraich ML, Lambert W, Doffing MA, et al. Psychometric properties of the Vanderbilt ADHD Diagnostic Parent Rating Scale in a referred population. J Pediatr Psychol. 2003;28(8):559-567. PubMed
18.Toolbox of Forms. American Association of Child & Adolescent Psychiatry website. https://www.aacap.org/AACAP/Member_Resources/AACAP_Toolbox_for_Clinical_Practice_and_Outcomes/Forms.aspx. Accessed May 7, 2020.
19.Lindsey MA, Brandt NE, Becker KD, et al. Identifying the common elements of treatment engagement interventions in children’s mental health services. Clin Child Fam Psychol Rev. 2014;17(3):283-298. PubMed CrossRef
20.MacPherson HA, Mackinaw-Koons B, Leffler JM, et al. Pilot effectiveness evaluation of community-based multi-family psychoeducational psychotherapy for childhood mood disorders. Couple Family Psychol. 2016;5(1):43-59. PubMed CrossRef
21.Myers KM, Valentine JM, Melzer SM. Feasibility, acceptability, and sustainability of telepsychiatry for children and adolescents. Psychiatr Serv. 2007;58(11):1493-1496. PubMed CrossRef
22.Anton MT, Jones DJ. Adoption of technology-enhanced treatments: conceptual and practical considerations. Clin Psychol (New York). 2017;24(3):223-240. PubMed
23.Heymann DL, Rodier G. Global surveillance, national surveillance, and SARS. Emerg Infect Dis. 2004;10(2):173-175. PubMed CrossRef
24.Bashshur RL, Shannon GW, Bashshur N, et al. The empirical evidence for telemedicine interventions in mental disorders. Telemed J E Health. 2016;22(2):87-113. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!