The Psychiatric Consultation Service at Massachusetts General Hospital (MGH) sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.
Dr Lokko is a third-year resident in the Massachusetts General Hospital/McLean Hospital Psychiatry Residency Training Program and a clinical fellow in psychiatry at Harvard Medical School, Boston, Massachusetts. Dr Stern is chief of the Avery D. Weisman Psychiatry Consultation Service at Massachusetts General Hospital and the Ned H. Cassem professor of psychiatry in the field of psychosomatic medicine/consultation at Harvard Medical School, Boston, Massachusetts.
Dr Stern is an employee of the Academy of Psychosomatic Medicine, has served on the speaker’s board of Reed Elsevier, is a stock shareholder in WiFiMD (Tablet PC), and has received royalties from Mosby/Elsevier and McGraw Hill. Dr Lokko reports no conflict of interest related to the subject of this article.
Collaboration and Referral Between
Internal Medicine and Psychiatry
Have you ever had a patient with active medical problems coupled with a problematic psychiatric disorder? Have you ever wondered whose role it was to assess psychiatric symptoms and how much of a medical workup should be initiated before requesting psychiatric consultation? If you have, then the following case vignette and discussion should prove useful for evaluating psychiatric problems that arise in the context of ongoing medical problems.
CASE VIGNETTE
Mr A, a 49-year old Cambodian immigrant with a history of paranoia and a positive purified protein derivative test, presented to the hospital with chills, night sweats, and worsening pain associated with an abscess in his rectum that began 3 weeks earlier. His initial workup was for active tuberculosis. In addition, several physicians and nurses who interacted with Mr A noticed that he had odd mannerisms and provided guarded responses to questions.
Although he denied having current symptoms of depression, mania, or psychosis, he acknowledged feeling anxious about his ongoing treatment for tuberculosis and persistent pain from his rectal abscess. Nevertheless, given his guardedness and history of paranoia, a psychiatric consultation was requested to evaluate “weirdness.”
HOW OFTEN ARE MEDICAL AND PSYCHIATRIC CONDITIONS COMORBID IN GENERAL HOSPITALS?
Among inpatients, nearly one-third of patients (30%) in general medical settings have a psychiatric disorder,1–3 and roughly 10% develop delirium; however, the incidence of delirium often increases to 80% in critically ill, intensive care unit patients.4 Despite the fact that many general hospital inpatients have psychiatric disturbances, only a small fraction of them are identified and treated in a timely and effective fashion. Rates of consultation for these conditions vary among institutions (from < 1% to as high as 13%).5,6 Comorbid psychiatric illness complicates care, and several studies have shown that psychiatric comorbidities are associated with an increase in hospital length of stay and health care costs.7–9
WHO PERFORMS INPATIENT PSYCHIATRIC CONSULTATIONS?
Psychiatric consultation services vary substantially from institution to institution. In some large academic medical centers, the consultation service is comprised of a team of psychiatrists, psychologists, residents, fellows, nurses, social workers, and medical students. In other centers, the consultation service is staffed only by an attending psychiatrist, a psychologist, or a chaplain; however, there has been debate as to the appropriateness of using nonmedical providers for the purpose of consultation, as the comprehensive mental health evaluation and treatment requires complex clinical skills derived from specialized training.5 Table 1 outlines some of the skills needed to perform a psychiatric consultation.10

In addition to these skills, the psychiatric consultant must be familiar with the nuances of medical/surgical illness, the medical/surgical environment, and medication side effects. In situations wherein nonpsychiatrists conduct some evaluations, a consultation psychiatrist should be available to oversee the process.
WHAT DOES THE PSYCHIATRIC
CONSULTATION ENTAIL?
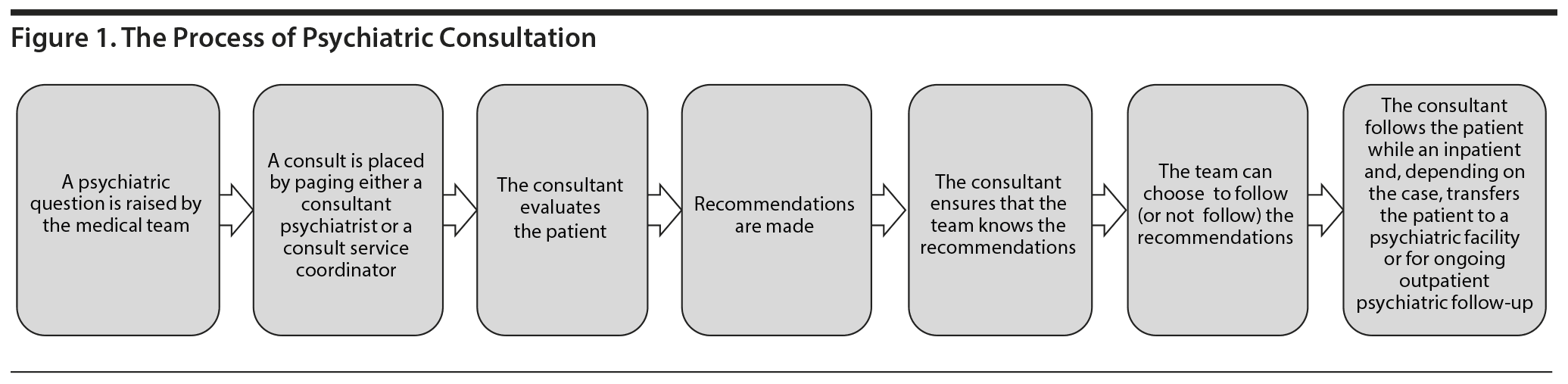
The process of psychiatric consultation varies across institutions and clinical environments (eg, whether it is a major academic medical center with a well-staffed psychiatric consultation service or an outpatient clinic or a community clinic that lacks an in-house psychiatric consultation service). A well-established consultation service is familiar with the practices of clinical teams (eg, with specialists dedicated to taking care of discrete groups of patients, such as oncology or trauma patients) and is invaluable.11 The consultation process (Figure 1) starts with a referral and a question; then, the psychiatric consultant sees the patient. Depending on the clinical setting, the consulting psychiatrist may manage or delegate to another mental health professional (under the supervision of the consulting psychiatrist). After the initial consultation, a follow-up examination is conducted, and ongoing management is reviewed. Disposition planning follows. Some patients are determined to have no psychiatric disorders, other patients require treatment on medical/surgical units or on an in-patient psychiatric unit, while others will benefit from outpatient psychiatric care. The referral should be made in conjunction with the primary care physician, subspecialty physicians, and the patient.
HOW SPECIFIC OR “SOPHISTICATED”
SHOULD A REFERRAL QUESTION BE?
No questions asked of a psychiatric consultant should be disregarded or minimized; in fact, many believe there is no such thing as an inappropriate consultation. Categorizing questions as good or bad can serve as a barrier for physicians to reach out to consultants. When both objective and subjective information is provided, psychiatric consultants can target their evaluation and management suggestions to facilitate patient care.
Many practitioners have sought to encourage refinement of the question posed to psychiatric consultants and have characterized good consult questions based on a patient’s symptoms (eg, depression, hallucinations, disorientation, substance use, or withdrawal). Questions can also be framed by the practitioner’s countertransference reactions or feelings (eg, sadness, anxiety, worry, fear) experienced when interacting with patients, by behavioral issues (eg, agitation or aggression toward oneself or others that arise during the hospital stay), by laboratory work or brain imaging abnormalities, or by collateral sources (eg, from family or from outpatient providers who have a longitudinal perspective on a patient’s behavior, which may differ from the history provided by the patient). Regardless of the framework of the question being asked, it is important for practitioners to indicate the urgency with which the question needs to be answered, so as to help the consultant prioritize the assessment and the interventions.
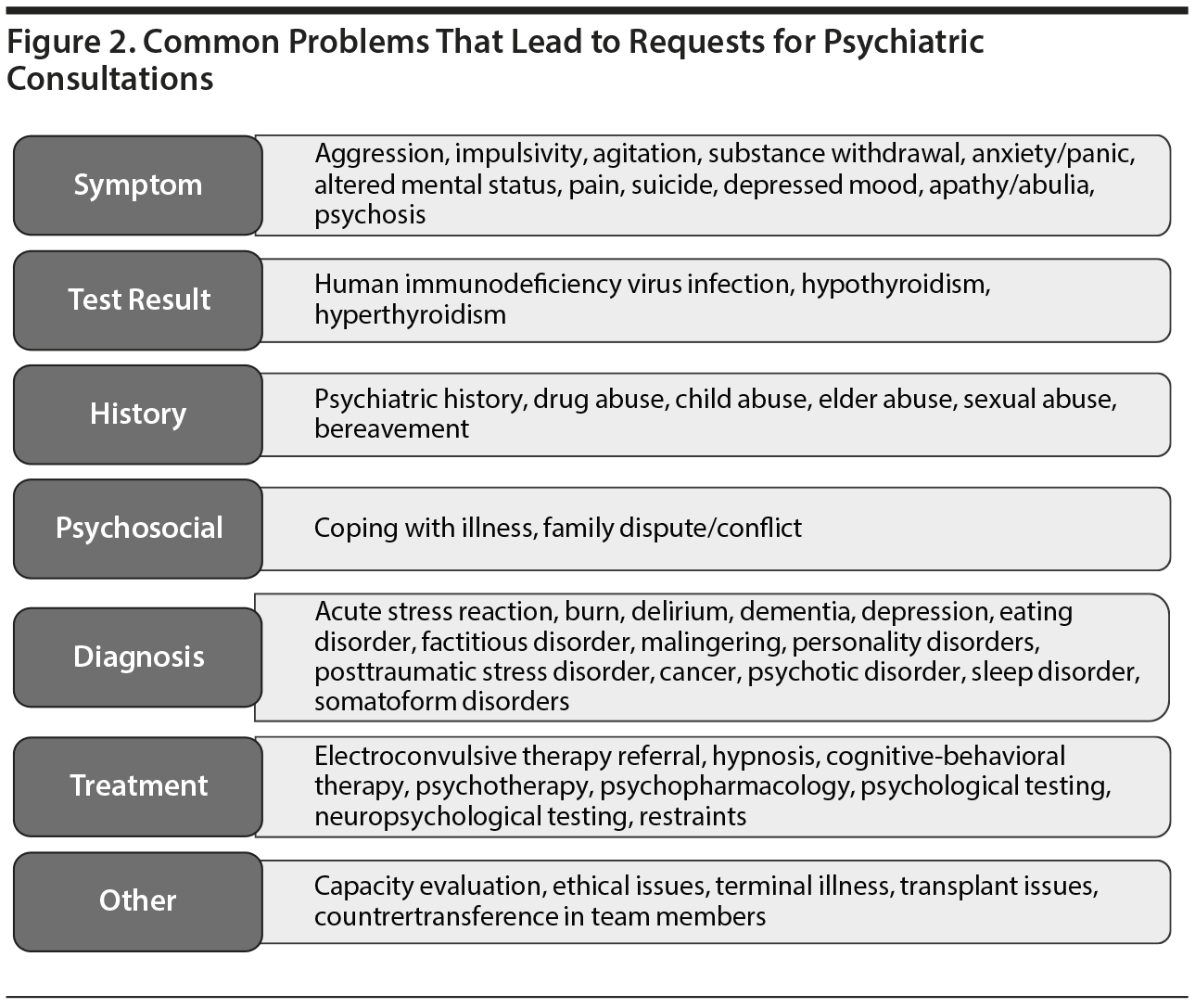
The problems that usually lead to a psychiatric consultation are quite broad. Figure 2 outlines common problems that lead to psychiatric consultation (eg, symptoms, test results, history, psychosocial context, diagnosis, treatment options).10
WHAT PRELIMINARY WORKUP
SHOULD BE COMPLETED BEFORE REQUESTING
A PSYCHIATRIC CONSULTATION?
Practitioners are well served by obtaining a history from their patients to flesh out the questions that are formulated for the consultant. Depending on the patient’s illness acuity, it is helpful for the referring team to start a medical workup (that might include a basic metabolic panel, a complete blood count, liver function tests, urine culture, thyroid-stimulating hormone, and basic imaging). It is often helpful to obtain toxicology/drug screens as part of the initial laboratory workup, since the period for detection of some drugs is hours to days. Additional tests can be arranged by the psychiatric consultant as needed. It is also useful to discuss with the patient that a psychiatrist will be involved in his/her care—a step that builds collaboration and minimizes adversarial relationships.
In clinical settings (such as outpatient primary care clinics, community hospitals, or medical centers with limited access to a psychiatric consultation), the primary provider of care may need to initiate a basic psychiatric screening while awaiting the arrival of a psychiatric consultant. In those situations, the guidelines for assessing common conditions (eg, mood disorders and psychotic disorders) include the following:
Depression: The patient should be asked if he/she feels depressed or is anhedonic (has lost pleasure in activities). One can follow up that single question screen with inquiry into other symptoms, recalled via use of the mnemonic SIG: E CAPS (developed by Dr Carey Gross following the format for writing prescriptions; a prescription label [SIG] for energy capsules) that assesses the amount and quality of sleep, interest, guilt, energy, concentration, appetite, psychomotor activity (retardation or agitation), and suicidal ideation present. A diagnosis of depression can be made if a patient endorses being depressed or anhedonic in addition to having 4 of the SIG: E CAPS criteria. Administration of the Patient Health Questionnaire-9 (PHQ-9), a 9-item self-administered tool, quantifies a patient’s neurovegetative symptoms of depression and can help to diagnose depression.12
Mania: To evaluate mania, the mnemonic DIG FAST (which represents distractibility, impulsivity, grandiosity, flight of ideas, activity increase, sleep decrease, and talkativeness) can be used. Patients meet criteria for mania if they endorse at least 3 of 7 criteria, with euphoria, or have at least 4 of 7 criteria, with irritability, for 1 week.
Psychosis: To evaluate if a patient has psychosis, one should ask about hallucinations (eg, visual, auditory, tactile, olfactory, gustatory), paranoia, delusions, thought insertion, thought broadcasting, thought withdrawal, and referential thinking.
In addition to the screening questions for depression, mania, and psychosis, one should conduct a mental status examination to help inform the differential diagnosis.
WHAT CONSTITUTES A GOOD OUTCOME FROM PSYCHIATRIC CONSULTATION?
Good outcomes from psychiatric consultations depend on several factors. These include a patient receiving the appropriate diagnosis and management of a psychiatric problem and the medical team receiving the necessary assistance needed to manage the psychiatric or behavior problem (eg, to help the team navigate difficult family conversations, to calm an agitated patient, or to unveil an important piece of history or information that is critical for patient care). A good outcome depends heavily on the situation and on the question asked. The disposition for patients evaluated by an inpatient psychiatric consultation service varies depending on the situation. While some patients are deemed to be free from psychiatric problems, others are treated while on medical/surgical floors or are scheduled for follow-up with an outpatient psychiatrist or a primary care physician or transferred to an inpatient psychiatric unit for further diagnostic evaluation, management, and stabilization.
CASE VIGNETTE: CONTINUED
Mr A underwent a psychiatric evaluation and was found to have no acute psychiatric problems despite his reported history of paranoia. After thorough medical workup (which yielded negative results for syphilis and human immunodeficiency virus) and stabilization, a follow-up appointment was arranged with his primary care physician.
HOW OFTEN ARE MEDICAL AND
PSYCHIATRIC CONDITIONS COMORBID IN THE PRIMARY CARE CLINIC SETTING?
Comorbid medical and psychiatric problems are prevalent and problematic in primary care clinics. Roughly 50% of all adult primary care patients have a psychiatric disorder, and an additional 12% have subthreshold conditions.13–17 Moreover, at least 10% of primary care patients have depression.18,19 Anxiety disorders are even more common (11%–25%), especially in those with chest pain, pulmonary disease, cerebrovascular disease, irritable bowel syndrome, and diabetes.20 Several studies have revealed that the recognition and treatment of psychiatric illnesses in the primary care population are suboptimal (ie, only half of the patients with a psychiatric disorder are recognized, and only 50% of those treated are treated effectively).13,21–26 Moreover, patients with untreated mental illness have more visits to primary care providers each year for somatic complaints than those without psychiatric illness, and those with somatoform disorders use significantly more medical resources than general medical patients without a somatoform disorder.27 Furthermore, psychiatric comorbidities, such as depression and anxiety, can be detected in close to two-thirds of high utilizers of medical care.28,29 All told, about two-thirds of high utilizers of medical care have undertreated psychiatric conditions.20,30
WHY IS COLLABORATION BETWEEN PRIMARY CARE PROVIDERS AND PSYCHIATRISTS IMPORTANT?
Several researchers have shown that a collaborative approach between psychiatrists and other health care providers significantly facilitates timely diagnosis and effective treatment of patients with both psychiatric and medical problems.31,32 Although primary care physicians can recognize most psychiatric symptoms, symptom recognition does not always translate into adequate treatment of psychiatric problems.33 Despite recent advancements in psychopharmacologic care and improved treatment of the mentally ill in the community,34 patient-driven, physician-driven, and health care system factors impact the diagnosis and treatment of psychiatric illness in primary care settings.20
Patient-driven factors include stigma and shame of their psychiatric problems, minimizing mood symptoms that accompany certain somatic symptoms, medical illness obscuring psychiatric illness, denial of psychiatric symptoms, fear of abandonment by one’s primary care provider if psychiatric referral were to be made, fear of addictive properties of certain psychiatric medications, and fear of cost of treatment should insurance not cover it.
Physician-driven factors include a lack of time to evaluate psychiatric symptoms, uncertainty about when and how to make referrals, and a lack of knowledge. Health system–driven factors include the structure of the American health care system for visits to primary care providers, including short visit times, fewer reimbursement initiatives, and carve outs for behavioral health, which create additional barriers.
HOW CAN COLLABORATION BETWEEN PRIMARY CARE PROVIDERS AND PSYCHIATRISTS PROCEED?
Several models20 (outlined below and summarized in Figure 3) of collaboration between primary care providers and psychiatrists exist for the management of psychiatric disorders. However, studies of the efficacy of these models are limited.
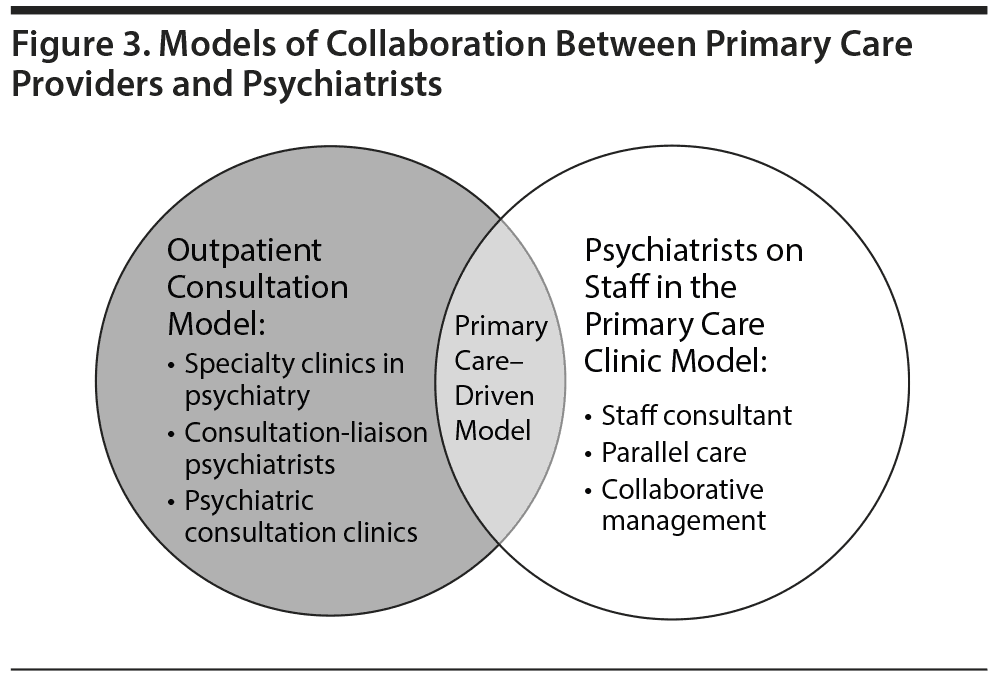
OUTPATIENT CONSULTATION MODEL
Specialty clinics in psychiatry are found in major academic health care centers. These clinics manage patients with well-defined psychiatric problems (eg, eating disorders, dissociation, substance abuse, or borderline personality disorder). Primary care providers can collaborate with these experts in their clinics for comprehensive management of their patients.
Consultation-liaison psychiatrists are not always restricted to inpatient hospital settings.35,36 In the outpatient setting, a consultation-liaison psychiatrist can make recommendations to primary care physicians (after 1-time consultation or with ongoing care). They foster ongoing exchanges of knowledge between the primary care provider and the psychiatrist.
Psychiatric consultation clinics are specialized clinics (staffed by psychiatrists, residents, psychologists, or social workers) that serve patients referred by primary care providers. These clinics are often located in the medical clinic. The diversity of staff allows for a diverse range of treatment modalities.
PSYCHIATRIST ON STAFF IN THE
PRIMARY CARE CLINIC MODEL
Staff consultants (psychiatrists) serve on the staff of medical clinics; this allows for a more robust consultant–primary care provider relationship that shares knowledge and information about patients and that provides continuity of care.37 Parallel care entails ongoing psychiatric care of patients in concert with the primary care. These medical clinics have incorporated psychiatric units as part of the clinic.
Collaborative management38,39 was initially developed for research purposes to assess the management of severely depressed primary care patients. Collaborative management involves alternating care between a psychiatrist and primary care provider after the initial primary care provider’s referral. The primary care provider then takes responsibility for the patient’s psychopharmacologic treatment.
Primary care–driven models combine elements of the consultation and collaborative management models with the goal of optimizing treatment of psychiatric problems in the primary care setting.40 These clinics provide psychiatric training for both psychiatric and primary care residents and establish criteria to identify cases that primary care providers can manage. Psychiatrists in these models help primary care providers to triage patients who need ongoing specialty care and assist them with referrals. Psychiatrists also help to evaluate and stabilize patients before the primary care provider takes on the full responsibility of managing patients.
CASE VIGNETTE: CONTINUED
Mr A, like many patients admitted to general hospitals, presented with more than 1 active medical problem (a rectal abscess and tuberculosis). However, a history of paranoia coupled with his providers’ uneasiness and belief that Mr A was weird prompted a psychiatric evaluation. His providers could have accepted their perceptions and assumed that a personality disorder was the source, or wondered if the behavior indicated a psychotic disorder, a substance abuse disorder, a mood disorder, or a disorder that would have invariably impacted his hospital course and management. Not recognizing and treating an active psychiatric problem in a patient like Mr A could have resulted in more aggressive behavior or agitation and put the patient and staff in harm’s way, or could have prolonged his hospital stay, while decreasing his treatment adherence and follow-up.
Further workup failed to reveal infection of the central nervous system or evidence of an immune-deficient state. Mr A was discharged with instructions to follow up with his primary care physician and an infectious disease specialist to manage his tuberculosis and monitor any change in his psychiatric symptoms (which were under control at the time of his hospitalization).
CONCLUSIONS
Psychiatric comorbidity is prevalent among patients on general medical and surgical services. Hence, there is a high likelihood that clinicians could benefit from assistance with the management of psychiatric comorbidities. Importantly, there is no such thing as an inappropriate psychiatric consultation request; nonpsychiatric health care providers typically know that something is awry (eg, signs and symptoms, laboratory test results, and countertransference reactions), and the referral question helps to guide psychiatric consultation.
Psychiatric consultants acquire certain skill sets and expertise. Unfortunately, not all medical facilities have in-house psychiatric consultants; therefore, the preliminary evaluation varies depending on the hospital setting and the existing resources. Several models of collaboration for psychiatrists and primary care providers are available; physicians should know which model of collaboration or resources they can access to facilitate and effectively treat the psychiatric problems of their patients in general medical and primary care settings. Good outcomes (even for patients like Mr A with no acute psychiatric diagnosis) depend on the consult question, on clear communication regarding the evaluation and management recommendations, on the disposition to an appropriate level of care, and on a patient’s response to treatment.
REFERENCES
1. Strain JJ. Needs for psychiatry in the general hospital. Hosp Community Psychiatry. 1982;33(12):996–1001. PubMed
2. vonAmmon Cavanaugh S, Wettstein RM. Emotional and cognitive dysfunction associated with medical disorders. J Psychosom Res. 1989;33(4):505–514. doi:10.1016/0022-3999(89)90012-3 PubMed
3. Spitzer RL, Kroenke K, Linzer M, et al. Health-related quality of life in primary care patients with mental disorders: results from the PRIME-MD 1000 Study. JAMA. 1995;274(19):1511–1517. doi:10.1001/jama.1995.03530190025030 PubMed
4. Lipowski ZJ. Delirium (acute confusional states). JAMA. 1987;258(13):1789–1792. doi:10.1001/jama.1987.03400130103041 PubMed
5. Lipowski ZJ. Review of consultation psychiatry and psychosomatic medicine: II. Clinical aspects. Psychosom Med. 1967;29(3):201–224. doi:10.1097/00006842-196705000-00001 PubMed
6. Pablo RY, Lamarre CJ. Psychiatric consultation in a general hospital. Can J Psychiatry. 1988;33(3):224–230. PubMed
7. Fink P. The use of hospitalizations by persistent somatizing patients. Psychol Med. 1992;22(1):173–180. doi:10.1017/S0033291700032827 PubMed
8. Fulop G, Strain JJ, Vita J, et al. Impact of psychiatric comorbidity on length of hospital stay for medical/surgical patients: a preliminary report. Am J Psychiatry. 1987;144(7):878–882. doi:10.1176/ajp.144.7.878 PubMed
9. Huyse FJ, Strain JJ, Hammer JS. Psychiatric comorbidity and length of hospital stay. Am J Psychiatry. 1988;145(10):1319. doi:10.1176/ajp.145.10.1319b PubMed
10. Bronheim HE, Fulop G, Kunkel EJ, et al; The Academy of Psychosomatic Medicine. The Academy of Psychosomatic Medicine practice guidelines for psychiatric consultation in the general medical setting. Psychosomatics. 1998;39(4):S8–S30. doi:10.1016/S0033-3182(98)71317-9 PubMed
11. Wallen J, Pincus HA, Goldman HH, et al. Psychiatric consultations in short-term general hospitals. Arch Gen Psychiatry. 1987;44(2):163–168. doi:10.1001/archpsyc.1987.01800140073010 PubMed
12. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606–613. doi:10.1046/j.1525-1497.2001.016009606.x PubMed
13. Wittchen HU, Mühlig S, Beesdo K. Mental disorders in primary care. Dialogues Clin Neurosci. 2003;5(2):115–128. PubMed
14. WHO International Consortium in Psychiatric Epidemiology. Cross-national comparisons of the prevalences and correlates of mental disorders. Bull World Health Organ. 2000;78(4):413–426. PubMed
15. Wittchen HU, Nelson CB, Lachner G. Prevalence of mental disorders and psychosocial impairments in adolescents and young adults. Psychol Med. 1998;28(1):109–126. doi:10.1017/S0033291797005928 PubMed
16. Jacobi F, Wittchen HU, Holting C, et al. Prevalence, co-morbidity and correlates of mental disorders in the general population: results from the German Health Interview and Examination Survey (GHS). Psychol Med. 2004;34(4):597–611. doi:10.1017/S0033291703001399 PubMed
17. Carbone LA, Barsky AJ, Orav EJ, et al. Psychiatric symptoms and medical utilization in primary care patients. Psychosomatics. 2000;41(6):512–518. doi:10.1176/appi.psy.41.6.512 PubMed
18. Spitzer RL, Williams JB, Kroenke K, et al. Utility of a new procedure for diagnosing mental disorders in primary care. The PRIME-MD 1000 study. JAMA. 1994;272(22):1749–1756. doi:10.1001/jama.1994.03520220043029 PubMed
19. Barrett JE, Barrett JA, Oxman TE, et al. The prevalence of psychiatric disorders in a primary care practice. Arch Gen Psychiatry. 1988;45(12):1100–1106. doi:10.1001/archpsyc.1988.01800360048007 PubMed
20. Stern TA, Herman JB, Slavin PL. The Massachusetts General Hospital Guide to Primary Care Psychiatry. 2nd ed. New York, NY: McGraw-Hill Health Professions Division; 2004.
21. Coyne JC, Schwenk TL, Fechner-Bates S. Nondetection of depression by primary care physicians reconsidered. Gen Hosp Psychiatry. 1995;17(1):3–12. doi:10.1016/0163-8343(94)00056-J PubMed
22. Tiemens BG, Ormel J, Simon GE. Occurrence, recognition, and outcome of psychological disorders in primary care. Am J Psychiatry. 1996;153(5):636–644. doi:10.1176/ajp.153.5.636 PubMed
23. Simon GE, Goldberg D, Tiemens BG, et al. Outcomes of recognized and unrecognized depression in an international primary care study. Gen Hosp Psychiatry. 1999;21(2):97–105. doi:10.1016/S0163-8343(98)00072-3 PubMed
24. Simon GE, VonKorff M. Recognition, management, and outcomes of depression in primary care. Arch Fam Med. 1995;4(2):99–105. doi:10.1001/archfami.4.2.99 PubMed
25. Williams JW Jr, Mulrow CD, Kroenke K, et al. Case-finding for depression in primary care: a randomized trial. Am J Med. 1999;106(1):36–43. doi:10.1016/S0002-9343(98)00371-4 PubMed
26. Simon GE, Fleck M, Lucas R, et al; LIDO Group. Prevalence and predictors of depression treatment in an international primary care study. Am J Psychiatry. 2004;161(9):1626–1634. doi:10.1176/appi.ajp.161.9.1626 PubMed
27. Smith GR Jr. The course of somatization and its effects on utilization of health care resources. Psychosomatics. 1994;35(3):263–267. doi:10.1016/S0033-3182(94)71774-6 PubMed
28. Katon W, Von Korff M, Lin E, et al. A randomized trial of psychiatric consultation with distressed high utilizers. Gen Hosp Psychiatry. 1992;14(2):86–98. doi:10.1016/0163-8343(92)90033-7 PubMed
29. Von Korff M, Ormel J, Katon W, et al. Disability and depression among high utilizers of health care: a longitudinal analysis. Arch Gen Psychiatry. 1992;49(2):91–100. doi:10.1001/archpsyc.1992.01820020011002 PubMed
30. Katzelnick DJ, Simon GE, Pearson SD, et al. Randomized trial of a depression management program in high utilizers of medical care. Arch Fam Med. 2000;9(4):345–351. doi:10.1001/archfami.9.4.345 PubMed
31. Katon WJ, Lin EH, Von Korff M, et al. Collaborative care for patients with depression and chronic illnesses. N Engl J Med. 2010;363(27):2611–2620. doi:10.1056/NEJMoa1003955 PubMed
32. Huffman JC, Mastromauro CA, Beach SR, et al. Collaborative care for depression and anxiety disorders in patients with recent cardiac events: the Management of Sadness and Anxiety in Cardiology (MOSAIC) randomized clinical trial. JAMA Intern Med. 2014;174(6):927–935. doi:10.1001/jamainternmed.2014.739 PubMed
33. Shapiro S, German PS, Skinner EA, et al. An experiment to change detection and management of mental morbidity in primary care. Med Care. 1987;25(4):327–339. doi:10.1097/00005650-198704000-00006 PubMed
34. Eisenberg L. Treating depression and anxiety in primary care: closing the gap between knowledge and practice. N Engl J Med. 1992;326(16):1080–1084. doi:10.1056/NEJM199204163261610 PubMed
35. Kates N, Craven MA, Crustolo AM, et al. Sharing care: the psychiatrist in the family physician’s office. Can J Psychiatry. 1997;42(9):960–965. PubMed
36. Oxman TE, Dietrich AJ, Williams JW Jr, et al. A three-component model for reengineering systems for the treatment of depression in primary care. Psychosomatics. 2002;43(6):441–450. doi:10.1176/appi.psy.43.6.441 PubMed
37. Nickels MW, McIntyre JS. A model for psychiatric services in primary care settings. Psychiatr Serv. 1996;47(5):522–526. doi:10.1176/ps.47.5.522 PubMed
38. Katon W, Von Korff M, Lin E, et al. Collaborative management to achieve depression treatment guidelines. J Clin Psychiatry. 1997;58(suppl 1):20–23. PubMed
39. Katon W, Von Korff M, Lin E, et al. Stepped collaborative care for primary care patients with persistent symptoms of depression: a randomized trial. Arch Gen Psychiatry. 1999;56(12):1109–1115. doi:10.1001/archpsyc.56.12.1109 PubMed
40. Pirl WF, Beck BJ, Safren SA, et al. A Descriptive Study of psychiatric consultations in a community primary care center. Prim Care Companion J Clin Psychiatry. 2001;3(5):190–194. doi:10.4088/PCC.v03n0501 PubMed
LESSONS LEARNED AT THE INTERFACE OF MEDICINE AND PSYCHIATRY
The Psychiatric Consultation Service at Massachusetts General Hospital (MGH) sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.
Dr Lokko is a third-year resident in the Massachusetts General Hospital/McLean Hospital Psychiatry Residency Training Program and a clinical fellow in psychiatry at Harvard Medical School, Boston, Massachusetts. Dr Stern is chief of the Avery D. Weisman Psychiatry Consultation Service at Massachusetts General Hospital and the Ned H. Cassem professor of psychiatry in the field of psychosomatic medicine/consultation at Harvard Medical School, Boston, Massachusetts.
Dr Stern is an employee of the Academy of Psychosomatic Medicine, has served on the speaker’s board of Reed Elsevier, is a stock shareholder in WiFiMD (Tablet PC), and has received royalties from Mosby/Elsevier and McGraw Hill. Dr Lokko reports no conflict of interest related to the subject of this article.
Prim Care Companion CNS Disord 2015;17(1):doi:10.4088/PCC.14f01746
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: November 11, 2014; accepted December 19, 2014.
Published online: February 26, 2015.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Corresponding author: Hermioni N. Lokko, MD, MPP, Department of Psychiatry, Massachusetts General Hospital and McLean Hospital, 15 Parkman St Wang ACC-812, Boston, MA 02114 ([email protected]).
Enjoy this premium PDF as part of your membership benefits!





