ABSTRACT
Objective: To evaluate the level of disability and identify an association between sociodemographic and clinical variables and disability in patients with bipolar disorder (BD).
Methods: This cross-sectional study was conducted in a tertiary care general hospital psychiatric unit with 100 patients with BD in partial or full remission (DSM-IV-TR criteria) from January 2017 to March 2018. Patients were assessed using a semistructured proforma, the Mini-International Neuropsychiatric Interview 5.0–Hindi version, the Hamilton Depression Rating Scale (HDRS) or the Young Mania Rating Scale (YMRS), and the Indian Disability Evaluation and Assessment Scale (IDEAS).
Results: All patients with BD had at least mild disability. The mean ± SD IDEAS global score was 5.1 ± 2.59. Of the sample, 66% and 34% had mild or moderate, disability, respectively. The global score of disability was associated with the number of episodes, number of manic episodes, frequency of episodes in the past year, YMRS and HDRS scores, partial remission, and hospitalization. Categories of disability were associated with the type of last episode, type of remission, and treatment setting.
Conclusions: Patients with BD had at least a mild level of disability even during remission. Disability worsened with the increasing number, frequency, and severity of episodes; number of manic episodes; partial remission; and hospitalization.
Prim Care Companion CNS Disord 2022;24(5):21m03183
To cite: Sengupta G, Jena S. Disability in patients with bipolar disorder in full or partial remission: a cross-sectional study. Prim Care Companion CNS Disord. 2022;24(5):21m03183.
To share: https://doi.org/10.4088/PCC.21m03183
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Atal Bihari Vajpayee Institute of Medical Sciences and Dr Ram Manohar Lohia Hospital, New Delhi, India
bDepartment of Psychiatry, Maulana Azad Medical College and Govind Ballabh Pant Institute of Postgraduate Medical Education and Research, New Delhi, India
*Corresponding author: Gunja Sengupta, MD, Department of Psychiatry, Dr Ram Manohar Lohia Hospital, Gate No. 9, Baba Kharak Singh Marg, New Delhi, India 110001 ([email protected]).
Bipolar disorder (BD) is characterized by episodes (with or without intervening periods of major mood symptoms) of depressive and manic symptoms that alternate or co-occur with each other that may or may not accompany psychotic symptoms.1 As the subthreshold and milder versions of bipolar disorder have emerged, the prevalence rates have been revised to more than twice the earlier estimates.2 Also, as research progresses, more robust evidence3 has documented the detrimental effects that BD has on the lives of those living with the disease. One such effect, a rather important one, is on the functioning of individuals with BD in different spheres/aspects of life.
Individuals with mental disability, as per the definition adopted for the National Sample Survey Organization survey on disability,4 have difficulty understanding routine instructions, cannot complete activities like others of a similar age, or exhibit behaviors such as talking to self, laughing/crying, staring, violence, fear, and suspicion without reason. According to the 2013 Global Burden of Disease study, BD is one of the top 20 disabling illnesses worldwide.5 It is the 16th leading cause of years lived with disability (YLD) and the fifth leading cause of disability-adjusted life-years (DALY) among mental and substance use disorders. BD accounts for 9.29 million DALYs as of 2017, an increase of 54.4% from the 1990 data.5,6 Although usually thought to only affect functioning during episodic exacerbations, studies5–10 have shown that bipolar patients continue to have functional impairment even during periods of remission.
Although the course of BD has exacerbations followed by interepisodic periods of remission, studies have shown that patients with BD who no longer meet the syndromal or symptomatic criteria after an acute episode continue to display functional impairment.7 Epidemiologic and cross-sectional research has unequivocally shown the burden and functional impairment experienced by patients with BD.
Ferrari et al5 summarized findings relevant to BD according to the 2013 Global Burden of Disease study and compared to those from 1990. In 1990, BD ranked as the 76th leading cause of global DALYs and the 19th leading cause of YLDs. In 2013, it ranked as the 54th leading cause of global DALYs and the 16th leading cause of YLDs. The authors5 found that despite the relatively low prevalence, BD is a disabling illness due to the early age at onset and chronic course. They postulated that population growth and ageing are contributing to the increase in the burden of BD over time.
Judd et al8 conducted a longitudinal study on disability during the course of bipolar I (BD-I) and bipolar II (BD-II) disorder. Psychosocial impairment increases significantly with each increment in depressive symptom severity for BD-I and BD-II, with most increments occurring in manic symptom severity for BD-I. Subsyndromal hypomanic symptoms may even enhance functioning in BD-II. Depressive symptoms are similarly disabling, if not more, compared to manic symptoms. BD-I and BD-II are equally disabling in terms of depressive symptom severity.
In an Indian study, Chacko et al9 compared disability between patients with BD and those with recurrent depressive disorder (RDD) and found higher levels of disability among patients with BD compared to those with RDD. Patients with BD fared worse in the domains of interpersonal activities, communication and understanding, and work compared to patients with RDD, while the domain of self-care was similar in the 2 groups. Swaroopachary et al10 studied disability in inpatients with BD and found that those with less than 10 years of duration of illness had severe disability, and the depressive and manic episodes were associated with moderate and severe disability, respectively. Thomas et al11 studied quality of life (QOL) and disability in patients with BD and found that disability worsened with age, was worse in females and in those who were not the primary breadwinner in their family, and was inversely related to QOL. These studies and others12,13 have concluded that even in the euthymic period of illness, patients with BD have impaired functioning.
The objective of this study was to evaluate the level of disability in patients with BD and identify an association between sociodemographic and clinical variables and disability.
METHODS
This cross-sectional study was conducted in a general hospital psychiatric unit (both outpatient and inpatient) of a tertiary care hospital in New Delhi from January 2017 to March 2018 with 100 patients diagnosed with BD (per DSM-IV-TR criteria14). The study was approved by the institutional ethics committee, and informed consent was received from all patients. Patients with a diagnosis of BD with duration ranging between 1 and 10 years and in partial or full remission were included in the study. Those who were uncooperative, as well as those with clinically severe cognitive deficits, impaired insight, hearing or visual impairment, clinically diagnosed intellectual disability, chronic debilitating physical illness with complications, or requiring hospitalization were excluded. The sample was of available patients (sample of convenience). A total of 100 patients were recruited for the study.
Each patient was interviewed with the Mini-International Neuropsychiatric Interview 5.0–Hindi version.15 Information was collected with a semistructured pro forma designed for this study.
Patients were administered the Hamilton Depression Rating Scale16 (HDRS) in the case of a current depressed episode and the Young Mania Rating Scale17 (YMRS) in the case of a current manic episode to assess severity. The level of disability was assessed with the clinician-administered Indian Disability Evaluation and Assessment Scale18 (IDEAS).
The data were tabulated in Microsoft Excel, and analysis was performed using SPSS version 16.0 software. Qualitative variables were compared using χ2/Fisher exact test. Quantitative variables were compared using Kruskal-Wallis/analysis of variance (for > 2 groups) and unpaired t test/Mann-Whitney test (for 2 groups).
RESULTS
Most of the patients were male (78%), and the mean ± SD age was 34.76 ± 12.34 years. The most common sociodemographic variables among patients were educated to less than the 5th standard (39%), unemployed/dependent (30%), urban background (85%), upper-lower socioeconomic status (39%), and married (54%). The mean ± SD age at onset of BD was 28.89 ± 11.52 years, and their duration of illness was approximately 68.86 ± 38.88 months with multiple episodes. Most patients were assessed at full remission (51%) and during outpatient follow-up (87%).
The mean ± SD IDEAS global score was 5.1 ± 2.59. When divided into levels of disability, 66% and 24% had mild disability and moderate disability, respectively.
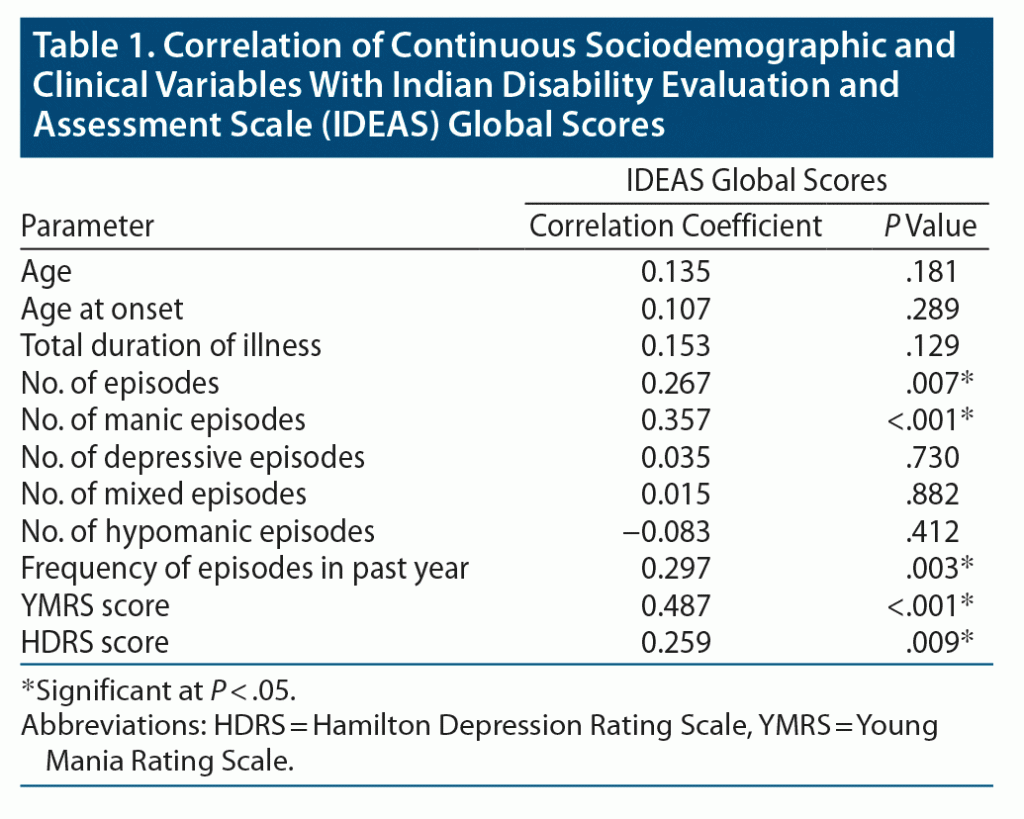
IDEAS global scores were correlated with sociodemographic and clinical variables, as shown in Table 1. A positive correlation was found with the total number of episodes, number of manic episodes, frequency of episodes in the past year, and YMRS or HDRS scores.
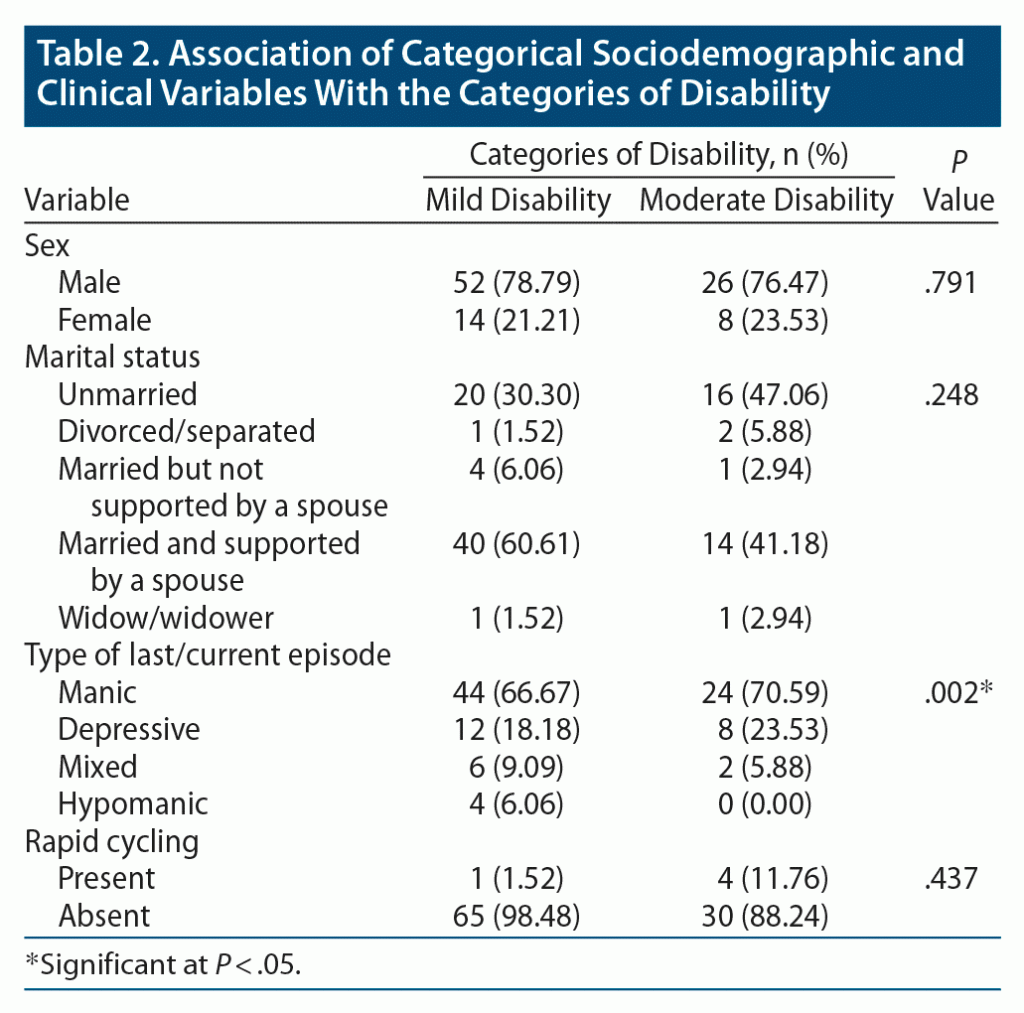
Association of categorical sociodemographic and clinical variables and categories of disability are shown in Table 2. A significant association was found between disability and last/current episode.
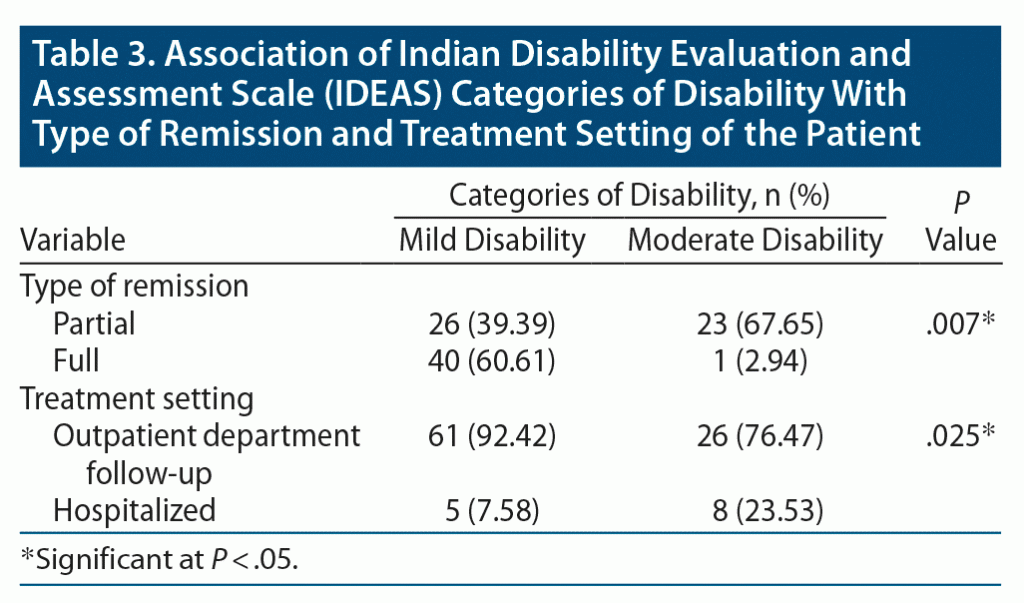
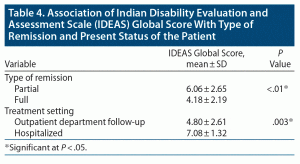
Association of the IDEAS categories of disability with type of remission and treatment setting is shown in Table 3. Association of the IDEAS global score and type of remission and treatment setting is shown in Table 4. A significant association was found between both categories and IDEAS scores with type of remission and treatment setting.
DISCUSSION
In this study, all patients with BD had at least a mild level of disability even during periods of full or partial remission. This finding is in line with that of other studies5–13 on functional impairment in BD. A study by Arnold et al7 found that BD patients had greater functional impairment compared to the general population, as well as similar impairments in mental health and role limitations as patients with chronic back pain.
A review by Sanchez-Moreno et al12 found that BD patients continue to have functional impairment even beyond the acute episodes. Factors associated with such impairment include persistent subsyndromal symptoms, older age, male sex, comorbidities, earlier onset, greater number of episodes and hospitalizations, rapid cycling, and cognitive dysfunction.12
We found that the IDEAS global score of disability had an association with the number of episodes, number of manic episodes, frequency of episodes in the past year, and YMRS and HDRS scores. Therefore, higher number of episodes, number of manic episodes, number of episodes in the past year, and remaining manic/depressive symptoms indicate poorer functioning. Also, patients with BD in partial remission and hospitalized patients had higher IDEAS global scores than that of outpatients. A comparative study in India11 using the same instrument, albeit with a smaller sample size, found that BD patients have higher IDEAS scores than those with recurrent depressive disorder, and duration of illness and number of episodes had a significant association with total IDEAS score. A prospective longitudinal study by Judd et al8 explored the clinical correlates of psychosocial disability over 20 years among 158 BD-I and 133 BD-II patients and found that manic and depressive symptom severity was significantly associated with impairment, and asymptomatic patients had poorer psychosocial functioning than controls.
A significant association was found between the category of disability and type of last/current episode (a higher proportion of those with manic and depressive episodes were in the moderate category, and a higher proportion of patients with mixed and hypomanic episodes were in the mild category), type of remission (a higher proportion of patients with BD with partial remission were in the moderate category), and treatment setting (a higher proportion of inpatients were in the moderate category). No association was found between the sociodemographic variables and disability.
The similar study in India11 also showed that age at onset, duration of illness, number of depressive and hypomanic episodes, female sex, not being the primary breadwinner of the family, and marital status are associated with poorer functioning. The differences in results may be due to the differences in methodology, especially the instrument used (ie, WHO Disability Assessment Schedule), and that the remission criteria of the patients with BD followed that of the ICD-10 rather than the DSM-IV-TR as was used in our study. Another study10 of BD inpatients in India found severe disability in patients with BD of duration < 10 years and found manic and depressive episodes to have an association with the severe and moderate disability categories of disability, respectively. Although the authors10 used the same instrument as that in our study, the patients were exclusively inpatients, and ICD-10 criteria were followed.
There are some limitations of this study. The sample size was small. There was insufficient representation of the whole spectrum of BD. Causal relationships could not be determined due to the cross-sectional prevalence design. The inclusion criteria of 1–10 years of duration of BD had, by the virtue of the duration itself, at least mild disability on the IDEAS. Also, the disability of hospitalized patients may differ from that of outpatients due to their hospital stay.
CONCLUSION
It is significant to note that across various studies over geographically and culturally heterogeneous populations, BD has been shown to cause functional impairment even in periods of remission. This study also found mild to moderate disability in all BD patients in partial or full remission, which worsened with the increasing number, frequency, and severity of episodes; number of manic episodes; partial remission; and hospitalization.
Another important finding is significantly increased disability during partial remission compared to those with full remission. This finding may hold importance given that this is the time that clinical management stabilizes and the patient either goes home from the hospital or decreases the frequency of follow-ups in the outpatient department.
With the shift in focus from symptom relief to rehabilitation,19 the time spent in partial remission is a time rife with possibilities for the rehabilitation of such patients with BD. The acknowledgment of the patient’s impairments in carrying out expected functioning will pave the way for patients with BD to regain functioning and recovery. Further epidemiologic studies and studies based exclusively on outpatient follow-up would provide a better understanding of functioning in patients with BD.
Submitted: October 31, 2021; accepted February 24, 2022.
Published online: September 20, 2022.
Relevant financial relationships: None.
Funding/support: None.
Acknowledgments: The authors thank PS Biswas, MD; Mahima Kapoor, MD; Anurag Jhanjee, MD; and Amandeep Goyal, MD, all faculty members from the Department of Psychiatry, Govind Ballabh Pant Institute of Postgraduate Medical Education and Research, New Delhi, India, for their invaluable support during the development of the protocol and conduct of the study, including identifying patients for recruitment. They have no conflicts of interest to declare.
CLINICAL POINTS
- A focus on disability and rehabilitation is emerging with changing national legislature on mental health and disability.
- Although initially thought to have dysfunction only during episodes, bipolar disorder (BD) has been shown to affect functioning throughout its course, even during periods of remission.
- Identification of potential correlates and assessment of disability and poor functioning in BD may help clinicians identify potential patients with functional impairment and target rehabilitation as well as help patients and their families access resources.
References (19)

- Ramdurg S, Kumar S. Study of sociodemographic profile, phenomenology, course and outcome of bipolar disorder in Indian population. Int J Health Allied Sci. 2013;2(4):260–263. CrossRef
- Merikangas KR, Jin R, He JP, et al. Prevalence and correlates of bipolar spectrum disorder in the World Mental Health Survey Initiative. Arch Gen Psychiatry. 2011;68(3):241–251. PubMed CrossRef
- Wesley MS, Manjula M, Thirthalli J. Interepisodic functioning in patients with bipolar disorder in remission. Indian J Psychol Med. 2018;40(1):52–60. PubMed CrossRef
- National Sample Survey Organization (NSSO) Ministry of Statistics and Programme Implementation Government of India. Disabled Persons in India, NSS 58th round (July–December 2002) Report No. 485 (58/26/1). [Internet]. New Delhi. 2003:6p. Accessed January 31, 2021. http://www.domainb.com/economy/general/2005/pdf/Disability_in_India.pdf
- Ferrari AJ, Stockings E, Khoo JP, et al. The prevalence and burden of bipolar disorder: findings from the Global Burden of Disease Study 2013. Bipolar Disord. 2016;18(5):440–450. PubMed CrossRef
- He H, Hu C, Ren Z, et al. Trends in the incidence and DALYs of bipolar disorder at global, regional, and national levels: results from the Global Burden of Disease Study 2017. J Psychiatr Res. 2020;125:96–105. PubMed CrossRef
- Arnold LM, Witzeman KA, Swank ML, et al. Health-related quality of life using the SF-36 in patients with bipolar disorder compared with patients with chronic back pain and the general population. J Affect Disord. 2000;57(1–3):235–239. PubMed CrossRef
- Judd LL, Akiskal HS, Schettler PJ, et al. Psychosocial disability in the course of bipolar I and II disorders: a prospective, comparative, longitudinal study. Arch Gen Psychiatry. 2005;62(12):1322–1330. PubMed CrossRef
- Chacko D, Narayan KT, Prabhavathy KS. Disability in patients with bipolar and recurrent depressive disorder in remission: a comparative study. Indian J Psychol Med. 2011;33(1):49–53. PubMed CrossRef
- Swaroopachary RS, Kalasapati LK, Ivaturi SC, et al. Disability in bipolar affective disorder patients in relation to the duration of illness and current affective state. Arch Ment Health. 2018;19(1):37. CrossRef
- Thomas SP, Nisha A, Varghese PJ. Disability and quality of life of subjects with bipolar affective disorder in remission. Indian J Psychol Med. 2016;38(4):336–340. PubMed CrossRef
- Sanchez-Moreno J, Martinez-Aran A, Tabarés-Seisdedos R, et al. Functioning and disability in bipolar disorder: an extensive review. Psychother Psychosom. 2009;78(5):285–297. PubMed CrossRef
- Ismail S, Mehar H, Pinto DA. Disability in schizophrenia and bipolar mood disorder in general hospital psychiatry unit. Delhi Psychiatry J. 2011;14(2):258–261.
- Diagnostic and Statistical Manual of Mental Disorders. Fourth Edition. Text Revision. Washington, DC: American Psychiatric Association; 2000.
- Lecrubier Y, Sheehan DV, Weiller E, et al. The Mini International Neuropsychiatric Interview (MINI): a short diagnostic structured interview: reliability and validity according to the CIDI. Eur Psychiatry. 1997;12(5):224–231. CrossRef
- Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56–62. PubMed CrossRef
- Young RC, Biggs JT, Ziegler VE, et al. A rating scale for mania: reliability, validity and sensitivity. Br J Psychiatry. 1978;133(5):429–435. PubMed CrossRef
- Ministry of Social Justice and Empowerment. Document no. 181788. [Internet]. New Delhi. 2018:113p. The Gazette of India website. Accessed August 25, 2022. https://egazette.nic.in/WriteReadData/2018/181788.pdf
- Rössler W. Psychiatric rehabilitation today: an overview. World Psychiatry. 2006;5(3):151–157. PubMed
Enjoy this premium PDF as part of your membership benefits!