ABSTRACT
Objective: To evaluate the effectiveness of a quality improvement (QI) initiative to improve family medicine residents’ metabolic monitoring of second-generation antipsychotics (SGAs) for patients comanaged across nonintegrated community mental health and family medicine clinics.
Methods: Patients were aged ≥ 18 years seen by family medicine residents and prescribed at least 1 SGA (N = 175). Preparative and scheduled QI interventions were nonblinded and included collaboration across organizations, education, and monthly interprofessional care conferences. The QI outcome included evaluation of pre-post metabolic monitoring laboratory data over the 15-month study period. A subset of patients (n = 26) was reviewed at least once at monthly interprofessional care conferences. Patients were stratified by diagnosis of diabetes (n = 45) and no diabetes (n = 130) at baseline. Analyses of the QI intervention outcomes were framed by the time period of monthly care conferences (January 31, 2019–April 30, 2020) and compared to baseline (the historical time period) (October 31, 2017–January 29, 2019).
Results: Improved adherence in glycated hemoglobin (HbA1c) (P = .042) and lipid (P < .001) monitoring per guidelines from baseline to follow-up was seen in the total patient population (N = 175). Patients without diabetes (n = 130) had significant improvement (P = .001) in HbA1c monitoring from baseline to follow-up. The subgroup of patient cases that were discussed at a care conference showed no significant improvement in HbA1c or lipid monitoring.
Conclusion: Preparative and scheduled QI interventions provided family medicine residents powerful reminders of the SGA monitoring guidelines that improved the metabolic monitoring behaviors for all patients on SGAs.
Prim Care Companion CNS Disord. 2023;25(3):22m03432
Author affiliations are listed at the end of this article.
Significant barriers continue to negatively impact effective coordination of behavioral and medical pharmacotherapy management across health systems.1,2 Coordinated management of prediabetes, diabetes, and mental illness is essential for providing the highest quality care.2–5 Antipsychotic therapy for the management of schizophrenia, bipolar disorder, irritability associated with autistic disorder, and treatment-resistant depression is implicated in causing metabolic disorders. Specifically, second-generation antipsychotics (SGAs) such as risperidone, olanzapine, clozapine, and quetiapine have shown to increase the risk of metabolic comorbidities such as obesity, type 2 diabetes, and dyslipidemia.6–11
Metabolic monitoring guidelines for patients taking SGAs were established in 2004, but significant barriers to SGA monitoring continue to exist.6,12–15 Although the current diabetes guidelines recommend screening for all adults starting at age 35 years regardless of risk factors, people with mental illness are less likely to be screened due to racial/ethnic minority status, stigma, and social determinants of health.16–18 Also, current standards of care in diabetes do not directly provide or summarize screening recommendations for patients prescribed SGAs with prediabetes and diabetes and give minimal guidance for monitoring all patients with no history of diabetes.5,19 Moreover, fragmented coordination of antipsychotic (SGA) metabolic monitoring creates unclear division of roles and responsibilities between primary care and mental health providers.20,21
Metabolic adverse events associated with SGAs exemplify the need for an integrated interprofessional team of behavioral and medical health care providers.9,10,22 The barriers to providing this integrated care across separate behavioral health and primary care systems include lack of formal partnerships, separate electronic health records (EHRs), and multiple factors preventing linking of interoperable-ready EHRs.2,23,24 Given the EHR’s central role in care team communication, the lack of interconnected EHRs requires separate organizations to find alternate strategies to comanage the care of mutual patients. Evidence demonstrates that a comprehensive team of both behavioral and primary care providers can ensure safe and effective treatment.2,25–28
CONTEXT AND RATIONALE FOR THE QUALITY IMPROVEMENT INITIATIVE
Barriers, as described previously, are the primary catalyst for implementing the quality improvement (QI) initiative.29 Collaborative partners of this QI initiative included providers from a community mental health clinic (MHC) and family medicine residency program. Although, both clinics are separate organizations, the MHC had a long-established relationship history of providing mental health training to the family medicine residents.
The family medicine faculty/physician residency preceptor, pharmacy resident, nurse care coordinator, and clinic manager were the primary QI project supporters from the family medicine clinic (FMC). The FMC utilizes a large integrated health system’s EHR system by Epic (https://www.epic.com/).
The MHC partners included a psychiatrist, psychiatric nurse practitioners, psychiatric pharmacist, registered nurses, and support staff. The MHC is a nonintegrated community mental health center utilizing the Carelogic (https://www.qualifacts.com/carelogic-ehr/) EHR platform. Although, Carelogic and Epic EHR systems are interoperable, the MHC providers are unable to link to outside EHRs due to multiple barriers to interconnectivity. Predictably, the QI initiative was eagerly supported by the MHC providers to address the time-intensive process of SGA metabolic monitoring.
OVERVIEW AND OBJECTIVES
The phase 2 QI initiative was a nonblinded, 15-month, retrospective, pre-post outcome analysis to evaluate the effectiveness of preparative and scheduled QI interventions. The goal was to increase family medicine residents’ metabolic monitoring of SGAs for patients comanaged across nonintegrated community MHCs and FMCs. The primary aim of this QI initiative was to increase the frequency of glycated hemoglobin (HbA1c) and lipid panel monitoring in accordance with SGA consensus monitoring guidelines by the MHC, residency faculty physician, and family medicine resident providers.
METHODS
Population
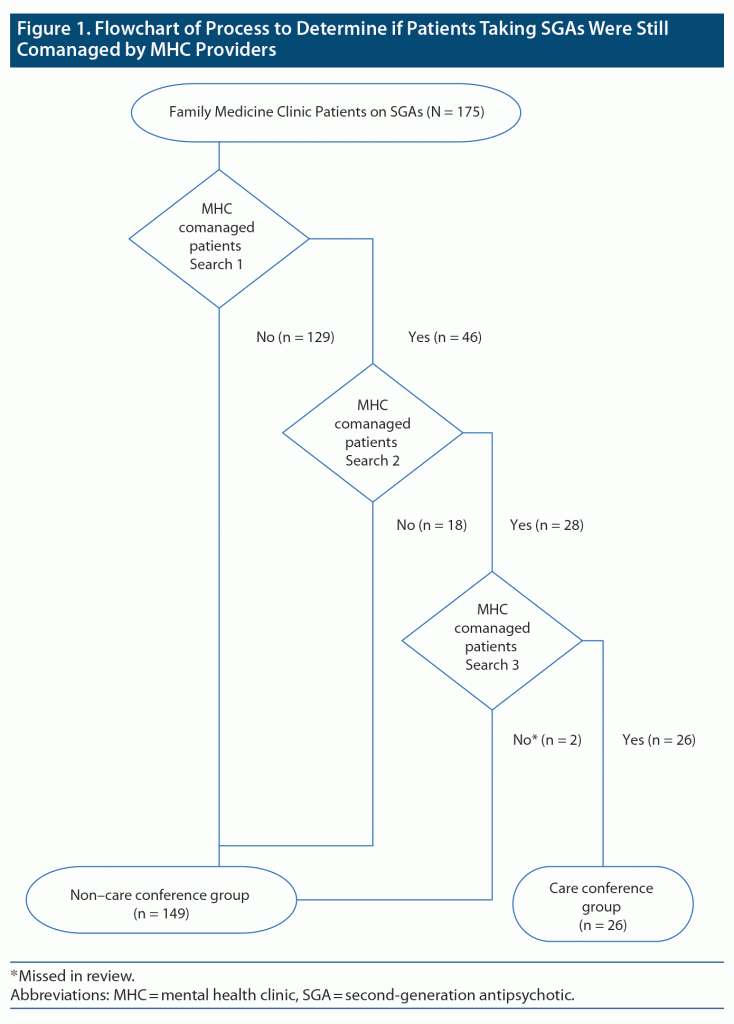
In April 2018, a total of 484 patients historically prescribed SGAs were identified at the FMC. To select comanaged patients for the care conferences, multiple manual and EHR searches were conducted. To validate search findings, family medicine providers were contacted directly to determine if the care conference cohort was still comanaged by MHC providers. As illustrated in Figure 1, almost half of the originally identified comanaged patient cohort was excluded due to no longer receiving MHC services (searches 1 and 2) or being accidently missed in chart review and were thus excluded (search 3). Identification of comanaged patients proved to be more difficult and time consuming than originally expected, since the MHC and FMC EHRs had no searchable data fields to record outside patient care providers. As a result, a large group of patients (n = 149) were excluded (see Figure 1). The study was approved by the FMC institutional review board and was deemed exempt from review by the University of Minnesota Institutional Review Board.
Preparative QI Interventions
Previously published articles30,31 describe the QI interventions in detail. The phase 1 article outlines the QI interventions used to build an infrastructure for the interprofessional relationships related to this study, such as the process of group concept mapping (GCM) that facilitated the MHC and family medicine residency faculty providers to coordinate management of shared patients.30 The GCM analysis resulted in a planned intervention that included consensus SGA metabolic monitoring guidelines, identifying which providers would be responsible for ordering monitoring laboratories, and establishment of a point person at each site (registered nurse care coordinator).30 As a result, MHC and FMC providers reached a consensus on the metabolic monitoring procedures.30 To avoid duplicate laboratory monitoring, both health systems decided that the FMC would be responsible for ordering all laboratory tests and following specific criteria for monitoring frequency for patients on antipsychotic agents (see the Measures and Data Management section).
The second related publication31 focused on family medicine residents and the impact of QI interventions including SGA education and a survey of their knowledge and attitudes related to the QI interventions. Hager et al31 also details the processes, outlining the monthly care conferences with an interprofessional care team from both clinics. The family medicine residents were educated didactically and experientially around the SGA monitoring guidelines and took responsibility for metabolic monitoring and management based on clinical findings. The preparatory QI interventions also included establishment of a point person at each site (registered nurse care coordinator), scheduling of monthly care conferences with an interprofessional care team from both facilities, and assisting the ambulatory pharmacy resident in the medication reconciliation process across clinic sites. Additional details about the intervention and providers were previously published (see SGA consensus monitoring guidelines in Hager et al30; see care conference process and team member roles in Hager et al31).
Scheduled QI Interventions
Scheduled QI interventions occurred at the FMC site with the family medicine residents (n = 11).31 In addition to training seminars, comanaged patient cases were discussed during monthly 75-minute care conferences over the defined study period.31 There was no limit on the number of times the same patient could be discussed at the monthly care conferences. The MHC and family medicine nurses scheduled 2 to 3 patients each month for the care conference, updated releases of information, and shared (faxed) relevant information when necessary. Prior to the monthly conference, the family medicine residents were alerted that their patient would be discussed. The pharmacy practice resident performed medication reconciliation across both clinics to ensure an accurate medication list during the care conference. The monthly care conferences were attended by the family medicine residents presenting the cases, the residency faculty physician leading discussions, the pharmacy practice resident reviewing medications, a licensed therapist, a family medicine clinic nurse, a psychiatrist, a psychiatric pharmacist, and other learners from the colleges of pharmacy and medicine.31 The presenting resident’s patient case EHR information was projected on a large screen to facilitate group discussion. Typically, the care conference discussions include clarifying medical and psychiatric diagnoses, reviewing laboratory results, listing additional providers involved (eg, case managers, therapists, guardians), medication reconciliation, and specific treatment strategies and rationales from medical and psychiatric perspectives. Psychiatric providers contributed by providing details of the patient’s last MHC visits including reviewing diagnoses, mental health and substance use histories, treatment plans, and relevant contact information of involved therapists and case managers associated with the patient case. Likewise, the family medicine providers reviewed chronic disease treatment guidelines and medications that were prescribed by the residents.
Study of the Interventions
For the defined baseline and scheduled intervention time periods, a total of 175 patients aged ≥ 18 years were prescribed at least 1 SGA. For statistical analyses, 2 study groups were included: all patients (n = 175) and care conference patients (n = 26), whose cases were reviewed at a minimum during 1 monthly interprofessional care conference and were comanaged by both MHC and family medicine resident providers. Two additional subgroups of the sample were analyzed based on if they were diagnosed with diabetes at baseline. Analyses of the QI intervention outcomes were framed by the time period of monthly care conferences (January 31, 2019–April 30, 2020) and compared to baseline (the historical time period) (October 31, 2017–January 29, 2019). To measure compliance with guideline laboratory testing during the period, the end date for those endpoints was changed to March 25, 2020, due to COVID-19–related clinic and laboratory closures.
Measures and Analyses
To determine the outcome of the QI interventions, patient data were extracted, unchanged, from the FMC’s existing EHRs for the identification of metabolic testing frequency within established consensus guidelines30 including laboratory values, dates of laboratory testing (HbA1c, lipids), diagnoses of diabetes (ICD-9/ICD-10), and dates of diagnoses. Metabolic monitoring within consensus guidelines were defined using a set of limits compared to 2 known measures: the average time between tests that were done and the number of days between the last test done and the end of the study period. Specifically, analyses of laboratory data were based on the consensus SGA metabolic monitoring guidelines ± 30 days. For HbA1C, acceptable limits were as follows: no diabetes = 365 days (1 year) ± 30 = 395 days; diagnosed diabetes with HbA1c < 7.0% = 183 days (6 months) ± 30 = 213 days; and diagnosed diabetes with HbA1C ≥ 7.0% = 91 days (3 months) ± 30 = 121 days. For lipids, acceptable limits were 365 ± 30 = 395 days for all subjects, and the same process was followed and is described below for both HbA1C and lipids.
Patient data were analyzed in aggregate by patient groups, demographics, antipsychotics (SGAs), laboratory data, and FMC visits. Patient demographics collected at baseline were analyzed with Student t test and included age and the age of patients in subgroups with and without diabetes. Sex distributions of patients with and without diabetes were compared using Pearson χ2 test of significance. Logistic regression was used to identify potential differences in shared care and standard care to evaluate insurance coverage and types of most prescribed SGA medications, as well as differences between care groups within each time period.
Binary outcome variables, including any baseline and follow-up HbA1c and lipid panel testing, SGA medications, and medical insurance, were analyzed using the McNemar test, which assesses baseline to follow-up changes (increased or decreased) in the level of utilization.
Quantitative outcome variables included in the analysis were baseline and follow-up period median HbA1C %, lipid panel values (cholesterol, calculated low-density lipoprotein), and baseline and follow-up period FMC visit frequencies by provider type and encounter. These data were tested for normality prior to evaluation of baseline to follow-up change. Since the data were not normally distributed, the Wilcoxon signed rank test was used to assess the null hypothesis by evaluating if the matched baseline to follow-up differences were equal to zero. For all statistical tests, a P value < .05 was considered significant. All statistics were performed by an independent statistician using SPSS version 23.
RESULTS
Baseline Demographics
Baseline to follow-up metabolic monitoring was analyzed for all patients (n = 175) and care conference patients (n = 26) on SGAs. The patients were stratified into 2 subgroups: patients with a diagnosis of diabetes (n = 45) and those with no history of diabetes (n = 130) at baseline.
Age, Sex, Insurance, Laboratory Values, SGA Medications, and COVID-19
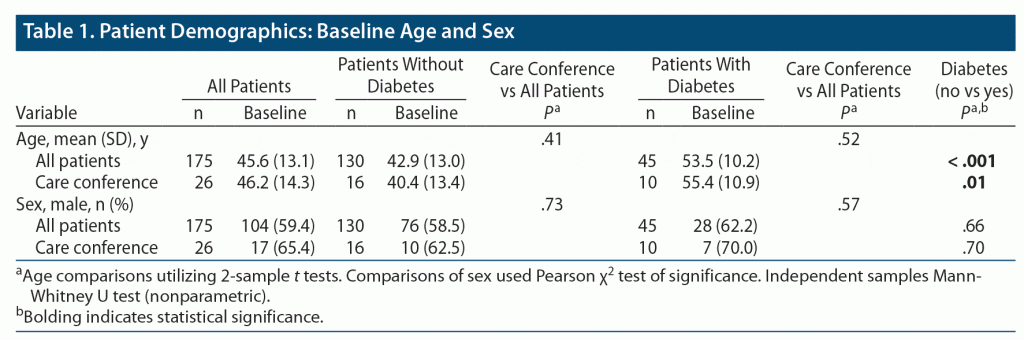
No significant age and sex differences were seen across either group (all patients and care conference patients). Patients diagnosed with diabetes were significantly older than nondiabetic patients at baseline: 53.5 years (SD = 10.2) versus 42.9 years (SD = 13.0), P < .001 (Table 1). Consistent with their mean age difference, significantly more diabetics than nondiabetics were on Medicare at baseline: 60.5% versus 39.4%, respectively, P = .02.
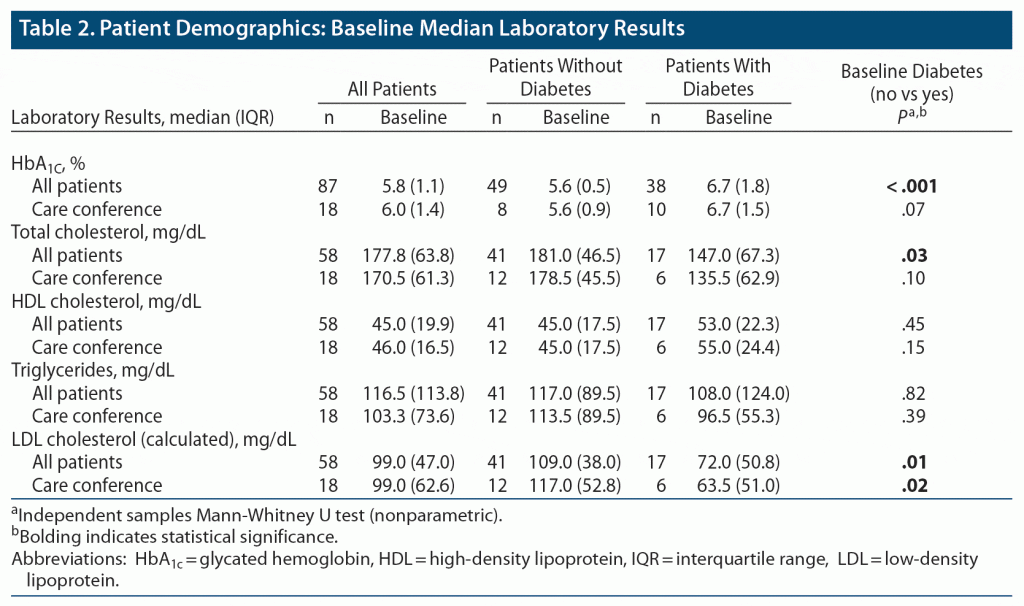
The all-patients group and the subgroup diagnosed with diabetes had significantly (P < .001) higher HbA1c percentages than nondiabetics. For lipid values, the nondiabetic patients had significantly higher levels of total cholesterol (all-patients group, P = .03) and calculated LDL values (all-patients group, P = .01 and care conference group, P = .02) at baseline (Table 2).
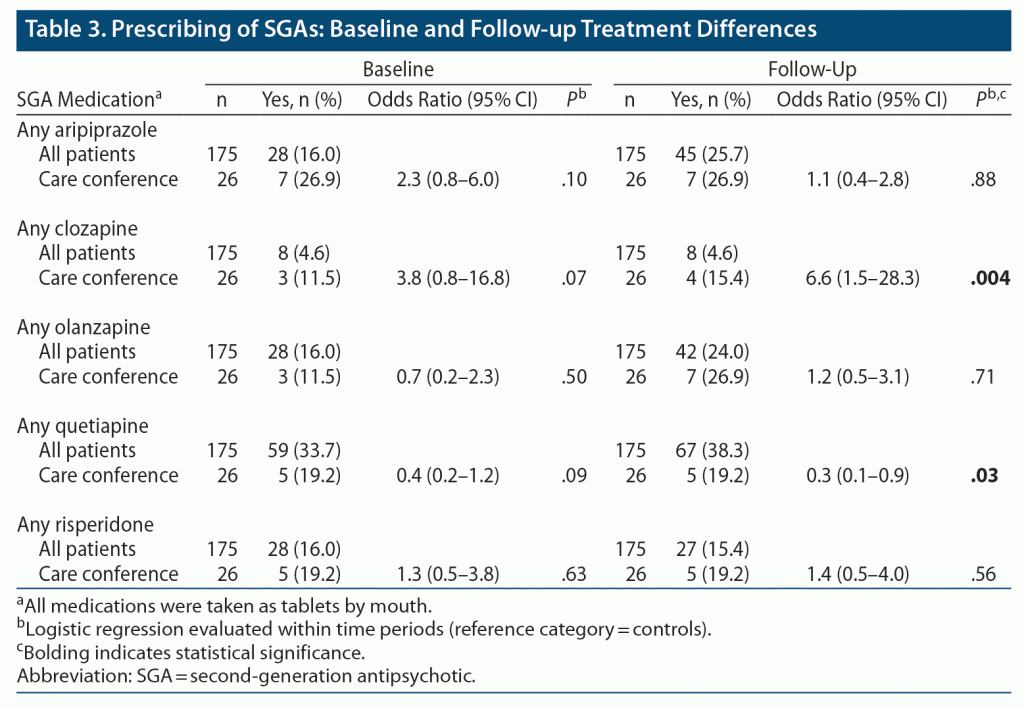
Follow-up clozapine prescribing was statistically higher in the care conference cohort (P = .004) compared to the all-patients group. Conversely, follow-up quetiapine prescribing was statistically higher in the all-patients cohort (P = .03) compared to the care conference cohort. No significant baseline to follow-up changes in prescribing of either of these medications was found in any group (Table 3).
Due to COVID-19 clinic closures, all nonemergency patient care transitioned to telehealth encounters as of March 25, 2020, which automatically resulted in significant baseline to follow-up increases in telehealth encounters among all patients (P < .001), patients with diabetes (P < .001), and patients with no history of diabetes (P = .001).
QI Intervention Outcomes: Metabolic Monitoring
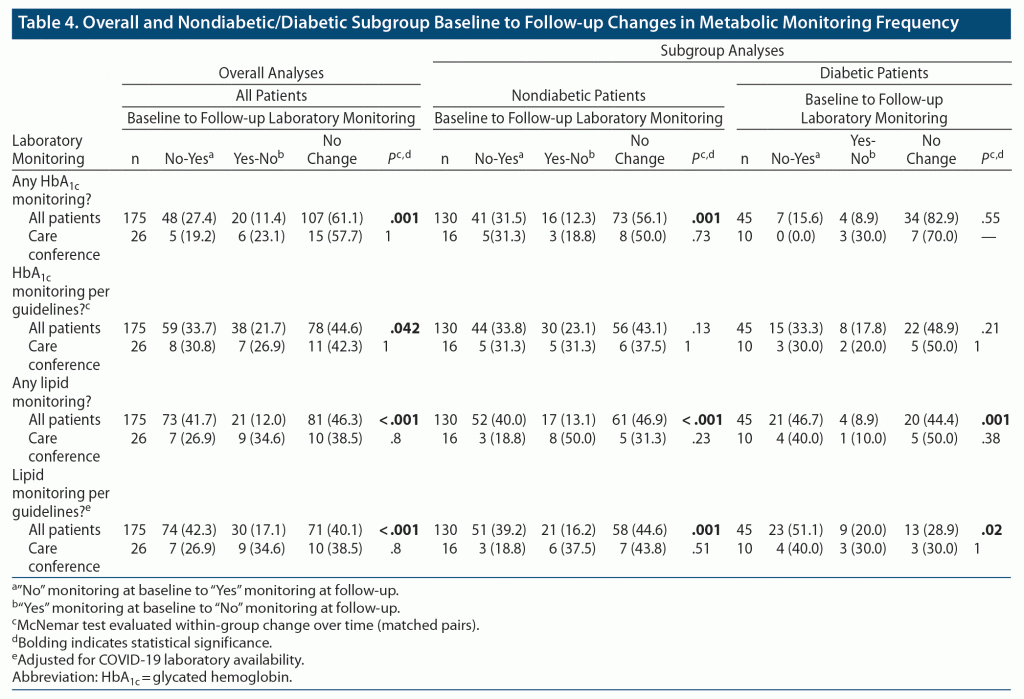
The all-patients group had significant baseline to follow-up improved adherence in any HbA1c results (P = .001) and recommended HbA1c monitoring per guidelines (P = .042) (Table 4). The all-patients group had significant improved adherence in any lipid results (P < .001) and guideline-based lipid (P < .001) monitoring. The nondiabetic all-patients subgroup (P < .001) was observed to have significant improvement in any HbA1c monitoring from baseline to follow-up. Similar significant improvements in recommended lipid monitoring per guidelines were observed in both nondiabetic (P = .001) and diabetic (P = .02) all-patient subgroups (see Table 4).
DISCUSSION
Key findings of the QI intervention analysis found significant overall and guideline-based improvement in SGA monitoring of both HbA1c and lipids in the all-patients group. The scheduled QI interventions served as powerful reminders to the family medicine residents, along with the clarification of responsibilities for monitoring and the relative ease of ordering lipid/HbA1c laboratory studies. As a result, the scheduled QI interventions prompted new clinical routines internalized by the family medicine residents serving all patients taking SGAs.
Additional key findings in the subgroup analyses showed significant increase in any diabetes screening among the nondiabetic patient subgroup nested within the all-patients group prescribed SGAs. Guideline-based lipid monitoring also improved in both nondiabetic and diabetic patient subgroups prescribed antipsychotics. Essentially, the key finding of increased HbA1c monitoring in the nondiabetic subgroup is of considerable importance due to the lack of reference to antipsychotics as a comorbidity risk in established diabetes treatment guidelines, such as those of the American Diabetes Association.19,32,33 Although diabetes guidelines recommend screening for prediabetes and type 2 diabetes in adults aged 35 to 70 years, especially if overweight or obese, people with mental illness may fall outside of this age range and healthy weight at initiation of SGA therapy.8,10,17,18,33 In summary, all patients with severe and persistent mental illness and patients prescribed SGAs require routine diabetes (HbA1c) screening, especially before SGA-related weight gain and obesity becomes established.22,34
Preliminary study results were presented informally at the April 2021 monthly care conference to discuss possible explanations for the increased frequency of metabolic monitoring in the all-patients group taking antipsychotics. Although beyond the scope of this QI outcome analysis, the interprofessional team supported our key findings that the increased metabolic monitoring in the all-patients group was due to the annual in-service training used to review antipsychotic monitoring guidelines, participation in the care conferences, faculty mentoring, and the family medicine residents’ coaching their colleagues to apply the monitoring guidelines to all patients on antipsychotics.
The results of the above informal discussion with the family medicine residents were also corroborated by the published survey results of the participating family medicine residents who responded very positively to the monthly care conferences.31 Similarly, the survey results indicated that the monthly care conferences fostered shared decision-making and interprofessional collaboration, leading to increased knowledge of psychosocial treatment aspects and confidence in providing metabolic monitoring for their patients on SGAs.31
Limitations
Study limitations include the limited number of participating family medicine residents, the nonintegrated mental health and family medicine clinic sites, lack of EHR interoperability, and the small sample size of the care conference group. The difficulty identifying comanaged patients to participate in the care conferences at the onset of the project intervention significantly contributed to the small sample size and subsequent low statistical power to measure the outcome of the QI interventions within this group. Although, clozapine was found to be more often prescribed in the mental health setting, the low sample size of patients prescribed specific SGAs, such as clozapine, limits further secondary analyses on metabolic monitoring.
The inability to obtain reimbursement for setting up and providing the care conference is a potential barrier to replicating this project in other health systems. However, even with the lack of reimbursement for the care conferences, both organizations committed to continue the monthly care conferences as standard of care for shared patients, which provides interprofessional and collaborative opportunities for continuous quality improvement.
Finally, the authors recognized that focusing on only patients prescribed antipsychotics is a significant limitation because of the evidence that people with severe persistent mental illness have lower life expectancy compared to the general population.9 At the time of this writing, our monthly care conferences have expanded to all patients with mental illness. In summary, this QI initiative study highlights the impacts of interprofessional education, peer mentoring, dedication to collaborative patient care, and commitment to quality improvement.35
CONCLUSION
Continual quality improvement strategies such as in-services and monthly care conferences serve as powerful reminders to medical residents and can prompt new clinical routines that become internalized into daily practice such as guideline-based monitoring of patients with severe persistent mental illness and all patients prescribed antipsychotics. This study demonstrates that an increase in communication through monthly care conferences and annual in-services can improve metabolic monitoring for patients taking SGAs and patient care.
Article Information
Published Online: June 27, 2023. https://doi.org/10.4088/PCC.22m03432
© 2023 Physicians Postgraduate Press, Inc.
Submitted: October 16, 2022; accepted January 19, 2023.
To Cite: Schneiderhan ME, O’Donnell C, Jackson SK, et al. Bridging community mental health and primary care to improve medication monitoring and outcomes for patients with mental illness taking second-generation antipsychotics—phase 2: quality improvement initiative over 15 months. Prim Care Companion CNS Disord. 2023;25(3):22m03432.
Author Affiliations: University of Minnesota College of Pharmacy, Department of Pharmacy Practice and Pharmaceutical Sciences, Duluth, Minnesota (Schneiderhan, Jackson, MacDonald, Yapel, Hager); Human Development Center, Department of Psychiatry, Duluth, Minnesota (Schneiderhan); Edward Hines Jr, Veterans Administration Hospital, Hines, Illinois (O’Donnell); Essentia Institute of Rural Health, Essentia Health, Duluth, Minnesota (Renier); Essentia Health, Behavioral Health, Duluth, Minnesota (Albee).
Corresponding Author: Mark E. Schneiderhan, PharmD, BCPP, University of Minnesota—Duluth, Department of Pharmacy Practice and Pharmaceutical Sciences, 232 Life Science 1110 Kirby Drive, Duluth, Minnesota 55812-3003 ([email protected]).
Relevant Financial Relationships: No relevant financial relationships to declare/nor conflicts of interest for all the authors and acknowledged physicians.
Funding/Support: Funding was received from the Minnesota Department of Health through a Rural Family Medicine Residency Award.
Role of the Sponsor: The financial sponsor had no role related to the project (eg, design and conduct of the study; collection, management, analysis, and interpretation of data; preparation, review, or approval of the manuscript).
Previous Presentation: Presented at the College of Psychiatric and Neurologic Pharmacists Annual Meeting; April 24–27, 2022; San Antonio, Texas.
Acknowledgments: The authors thank Jason T. Wall, MD (Department of Family Medicine and Community Health at University of Minnesota and University of Minnesota Duluth Family Medicine Residency Program) for leading the monthly interprofessional patient care conferences and providing medical training as faculty at the University of Minnesota Duluth Family Medicine Residency Program and Steven Bauer, MD (Human Development Center, Duluth, Minnesota) for active engagement, participation, and institutional support of the monthly interprofessional patient care conferences and providing psychiatry education to the medical residents and team. Drs Wall and Bauer have no relevant financial relationships to declare.
ORCID: Mark E. Schneiderhan: https://orcid.org/0000-0002-4239-3354; Carolyn O’Donnell: https://orcid.org/0000-0001-7335-3286; Danielle A. MacDonald: https://orcid.org/0000-0002-4252-9792; Ann M. Yapel: https://orcid.org/0000-0003-2071-2366; Colleen M. Renier: https://orcid.org/0000-0001-5083-5282; Keri D. Hager: https://orcid.org/0000-0002-2075-3910
Clinical Points
- Interprofessional monthly care conferences can improve coordination of care across mental health and primary care settings.
- Continual quality improvement strategies such as in-services and monthly care conferences serve as powerful reminders to medical residents and can prompt new clinical routines that become internalized into daily practice.
- The quality improvement initiative of implementing monthly care conferences and annual in-services improved metabolic monitoring, including diabetes screening for nondiabetic patients, and lipid monitoring in both nondiabetic and diabetic patients prescribed antipsychotics.
References (35)

- Hogan MF. New Freedom Commission Report: The President’s New Freedom Commission: recommendations to transform mental health care in America. Psychiatr Serv. 2003;54(11):1467–1474. PubMed CrossRef
- Tepper MC, Cohen AM, Progovac AM, et al. Mind the gap: developing an integrated behavioral health home to address health disparities in serious mental illness. Psychiatr Serv. 2017;68(12):1217–1224. PubMed CrossRef
- Daly R. Mentally ill people may gain benefits of coordinated care. Psychiatr News. 2009;44(21):6. CrossRef
- Cook JA, Jonikas JA, Steigman PJ, et al. Registry-managed care coordination and education for patients with co-occurring diabetes and serious mental illness. Psychiatr Serv. 2021;72(8):912–919. PubMed CrossRef
- Facilitating Behavior Change and Well-being to Improve Health Outcomes: Standards of Medical Care in Diabetes-2022. Diabetes Care. 2022;45(suppl 1):S60–S82. PubMed CrossRef
- American Diabetes Association; American Psychiatric Association; American Association of Clinical Endocrinologists; North American Association for the Study of Obesity. Consensus development conference on antipsychotic drugs and obesity and diabetes. Diabetes Care. 2004;27(2):596–601. PubMed CrossRef
- Smith RC, Lindenmayer JP, Davis JM, et al. Effects of olanzapine and risperidone on glucose metabolism and insulin sensitivity in chronic schizophrenic patients with long-term antipsychotic treatment: a randomized 5-month study. J Clin Psychiatry. 2009;70(11):1501–1513. PubMed CrossRef
- Lamberti JS, Olson D, Crilly JF, et al. Prevalence of the metabolic syndrome among patients receiving clozapine. Am J Psychiatry. 2006;163(7):1273–1276. PubMed CrossRef
- Mangurian C, Newcomer JW, Modlin C, et al. Diabetes and cardiovascular care among people with severe mental illness: a literature review. J Gen Intern Med. 2016;31(9):1083–1091. PubMed CrossRef
- De Hert M, Detraux J, van Winkel R, et al. Metabolic and cardiovascular adverse effects associated with antipsychotic drugs. Nat Rev Endocrinol. 2011;8(2):114–126. PubMed CrossRef
- Newcomer JW, Sernyak MJ. Identifying metabolic risks with antipsychotics and monitoring and management strategies. J Clin Psychiatry. 2007;68(7):e17. PubMed CrossRef
- Morrato EH, Newcomer JW, Kamat S, et al. Metabolic screening after the American Diabetes Association’s consensus statement on antipsychotic drugs and diabetes. Diabetes Care. 2009;32(6):1037–1042. PubMed CrossRef
- Morrato EH, Druss B, Hartung DM, et al. Metabolic testing rates in 3 state Medicaid programs after FDA warnings and ADA/APA recommendations for second-generation antipsychotic drugs. Arch Gen Psychiatry. 2010;67(1):17–24. PubMed CrossRef
- Mitchell AJ, Delaffon V, Vancampfort D, et al. Guideline concordant monitoring of metabolic risk in people treated with antipsychotic medication: systematic review and meta-analysis of screening practices. Psychol Med. 2012;42(1):125–147. PubMed CrossRef
- Schneiderhan ME, Shuster SM, Davey CS. Twelve-month prospective randomized study of pharmacists utilizing point-of-care testing for metabolic syndrome and related conditions in subjects prescribed antipsychotics. Prim Care Companion CNS Disord. 2014;16(5):1–9. PubMed CrossRef
- Fang M, Wang D, Coresh J, et al. Undiagnosed diabetes in US adults: prevalence and trends. Diabetes Care. 2022;45(9):1994–2002. PubMed CrossRef
- American Diabetes Association. Standards of Medical Care in Diabetes–2022 Abridged for Primary Care Providers. Clin Diabetes. 2022;40(1):10–38. PubMed CrossRef
- Davidson KW, Barry MJ, Mangione CM, et al. US Preventive Services Task Force. Screening for Prediabetes and Type 2 Diabetes: US Preventive Services Task Force Recommendation Statement. JAMA. 2021;326(8):736–743. PubMed CrossRef
- American Diabetes Association Professional Practice Committee. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes–2022. Diabetes Care. 2022;45(suppl 1):S17–S38. PubMed CrossRef
- Mangurian C, Giwa A, Brosey E, et al. Opinions of primary care clinicians and psychiatrists on monitoring the metabolic effects of antipsychotics. J Am Board Fam Med. 2019;32(3):418–423. PubMed CrossRef
- Shenkman E, Thompson L, Bussing R, et al. Provider specialty and receipt of metabolic monitoring for children taking antipsychotics. Pediatrics. 2021;147(1):e20200658. PubMed CrossRef
- Musil R, Obermeier M, Russ P, et al. Weight gain and antipsychotics: a drug safety review. Expert Opin Drug Saf. 2015;14(1):73–96. PubMed CrossRef
- Falconer E, Kho D, Docherty JP. Use of technology for care coordination initiatives for patients with mental health issues: a systematic literature review. Neuropsychiatr Dis Treat. 2018;14:2337–2349. PubMed CrossRef
- Fennelly O, Cunningham C, Grogan L, et al. Successfully implementing a national electronic health record: a rapid umbrella review. Int J Med Inform. 2020;144:104281. PubMed CrossRef
- Gierisch JM, Nieuwsma JA, Bradford DW, et al. Pharmacologic and behavioral interventions to improve cardiovascular risk factors in adults with serious mental illness: a systematic review and meta-analysis. J Clin Psychiatry. 2014;75(5):e424–e440. PubMed CrossRef
- Maragakis A, RachBeisel J, Blount A. Preliminary results from a newly established behavioral health home: early identification of glucose metabolism disorders in individuals with serious mental illness. Health Serv Res Manag Epidemiol. 2015;2:2333392815587507. PubMed CrossRef
- McGough PM, Bauer AM, Collins L, et al. Integrating behavioral health into primary care. Popul Health Manag. 2016;19(2):81–87. PubMed CrossRef
- McGovern M, Dent K, Kessler R. A unified model of behavioral health integration in primary care. Acad Psychiatry. 2018;42(2):265–268. PubMed CrossRef
- Ogrinc G, Davies L, Goodman D, et al. SQUIRE 2.0 (Standards for QUality Improvement Reporting Excellence): revised publication guidelines from a detailed consensus process. BMJ Qual Saf. 2016;25(12):986–992. PubMed CrossRef
- Hager K, Kading M, O’Donnell C, et al. Bridging community mental health and primary care to improve medication monitoring and outcomes for patients with mental illness taking second-generation antipsychotics-HDC/DFMC Bridge Project, phase 1: group concept mapping. Prim Care Companion CNS Disord. 2019;21(4):19m02452. PubMed CrossRef
- Hager KD, Albee JN, O’Donnell C, et al. Impact of interprofessional care conferences across primary care and mental health organizations on family medicine resident learning. Fam Med. 2021;53(4):289–294. PubMed CrossRef
- American Diabetes Association Professional Practice Committee. 3. Prevention or Delay of Type 2 Diabetes and Associated Comorbidities: Standards of Medical Care in Diabetes–2022. Diabetes Care. 2022;45(suppl 1):S39–S45. PubMed CrossRef
- American Diabetes Association Professional Practice Committee. 4. Comprehensive Medical Evaluation and Assessment of Comorbidities: Standards of Medical Care in Diabetes–2022. Diabetes Care. 2022;45(suppl 1):S46–S59. PubMed CrossRef
- Al-Goblan AS, Al-Alfi MA, Khan MZ. Mechanism linking diabetes mellitus and obesity. Diabetes Metab Syndr Obes. 2014;7:587–591. PubMed CrossRef
- Hockey PM, Marshall MN. Doctors and quality improvement. J R Soc Med. 2009;102(5):173–176. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!