ABSTRACT
Objective: The mental health community expected that seriously mentally ill (SMI) patients would be especially vulnerable to coronavirus disease 2019 (COVID-19) infection due to a higher medical comorbidity rate than the general population and disparities in access to medical care. Concern was voiced as to the impact on the psychiatric stability of this population due to anxiety about the pandemic, recommended isolation, and limited in-person interactions with treatment providers and support systems. The objective of this study was to evaluate the impact of COVID-19 on a cohort of involuntarily hospitalized SMI patients.
Methods: The electronic medical records from March 28 through December 31, 2020 of all COVID-positive psychiatric inpatients were retrospectively reviewed. No outpatients or readmissions were included in the sample.
Results: During the study period 238, COVID-positive inpatients were identified out of approximately 12,859 discreet admissions. The sample consisted of 158 men (66%) and 80 women (34%). The mean age of positive patients was 41 years. Eight patients (3%) required medical hospitalizations related to COVID-19, with 1 death. Ninety-seven patients (41%) had at least 1 or more of the known medical comorbidities related to increased risk for COVID-19 infection. Seclusion, restraints, and administration of as-needed medications (PRN) for anxiety or psychotic agitation occurred less frequently in the COVID-positive patients compared to those without infection.
Conclusions: Medical hospitalizations were infrequent in the study sample. Medical comorbidities were much higher in this group relative to statewide data. Seclusion, restraint, and PRN administration were lower in the COVID-positive cohort compared to COVID-negative inpatients. Overall, the sample group did not experience significant negative outcomes as might have been expected for this population.
Prim Care Companion CNS Disord 2021;23(5):21m03003
To cite: Levitt G. COVID-19 infection in an inpatient psychiatric hospital setting: demographics, outcomes, and impact on well-being. Prim Care Companion CNS Disord. 2021;23(5):21m03003.
To share: https://doi.org/10.4088/PCC.21m03003
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, District Medical Group, Phoenix, Arizona
bCreighton University Medical School, Omaha, Nebraska
cUniversity of Arizona Medical School-Phoenix, Phoenix, Arizona
dMayo Hospital Medical School, Scottsdale, Arizona
eMidwestern University Medical School, Glendale, Arizona
*Corresponding author: Gwen Levitt, DO, DFAPA, Valleywise Health Systems, Behavioral Health Annex, 2619 East Peirce St, Phoenix, AZ 85008 ([email protected]).
Individuals with serious mental illness (SMI) may be more susceptible to coronavirus disease 2019 (COVID-19) than the general population for medical and psychosocial reasons.1 Research has found that SMI patients are at high risk for medical comorbidities and die approximately 25 years earlier than individuals in the general population.2 Cardiovascular disease, respiratory conditions, and metabolic syndromes are the most common medical conditions identified in the SMI population.2 These are the same comorbidities determined to be high risk factors for COVID-19 infection in the general population.3,4
Mental health providers have voiced concerns that the COVID-19 pandemic will exacerbate psychiatric symptoms and decrease the overall well-being of SMI patients.5 Previous studies6 have identified an increase in psychological distress among SMI patients during a pandemic, but not necessarily due to the pandemic itself. It has been posited that SMI patients may be at a higher risk of contracting COVID-19 and have worse medical outcomes from infection.6 Quarantine is suspected to have adverse effects on SMI patients due to disruption in treatment services, increased life stress, and isolation.6,7
In this retrospective study, records of COVID-positive inpatients were reviewed. The hospital has a population that is comprised primarily of SMI patients living at or near the poverty level. One aim of this study was to examine the demographics and comorbid medical risk factors of the COVID-positive sample and compare them with the general population. A second goal was to assess how the pandemic may have affected the well-being and psychiatric stability of the study cohort.
The inpatients in the facilities cohabitate with shared rooms, baths, dayrooms, recreational areas, and dining. Areas with a single bed and bathroom were created at each of the 3 psychiatric hospitals involved in the study and designated as admission units. All newly admitted patients were quarantined to these admission rooms and tested immediately for COVID-19. In the first few months, when knowledge of the virus was in its infancy, once a patient tested negative for COVID-19, he/she was moved to a communal unit. As information became known about the incubation period of the virus and its spread, patients were held in quarantine for 72 hours after a negative admission test result to monitor for any signs of infection. If a positive patient was identified on the communal units, the entire unit was placed on quarantine and point-prevalence testing was completed over a 14-day period. At any time, a patient who showed signs of possible infection or those exposed to a COVID-positive person was tested again for the virus. Patients who refused to be tested remained in quarantine until a negative test was obtained or for 14 days.
METHODS
Valleywise Health Medical Center in Phoenix, Arizona is a government-supported hospital with 3 psychiatric facilities housing over 300 inpatients. The psychiatric hospitals have 1 adolescent unit (for patients aged 12 to 17 years), a geriatric unit, and a unit for medically challenging patients. The remainder of the hospital serves an adult population. The study facilities are the only ones in the area that accept patients involuntary (court ordered). Patients are transferred from local emergency rooms, hospitals, and psychiatric urgent care centers for admission. Nursing administration maintained a log of COVID-positive patients. Using this log, the authors retrospectively collected data from electronic records of COVID-positive patients from March 28 (the date of the first COVID-positive patient) through December 31, 2020. Data collected included demographic variables, admission date, COVID-19 test data, length of stay (LOS), psychiatric and medical diagnoses, and clinical outcomes of COVID-19 infection. Data on seclusion and restraint episodes were provided by administration, and as-needed medication (PRN) administration data were obtained from the hospital’s pharmacy. The Valleywise Health Medical Center Institutional Review Board approved the study (#2020-096, April 30, 2020).
RESULTS
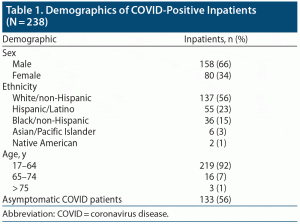
From April 1, 2020, through December 31, 2020, 12,859 patients were admitted to the hospital’s 3 inpatient psychiatric units. Only monthly statistics were available for review, so the last 2 days in March (that encompass the time frame of study) were not included. The mean daily admission rate for 2020 was 16 patients a day. During the study period, 238 patients tested positive for COVID-19. Eight of these patients had positive COVID antibody tests, and per hospital infection control policy they were treated as a patient with active disease. The age range of the COVID-positive group was 17 to 83 years with a mean of 41 years. Sixteen COVID-positive patients (7%) were aged 65 to 74 years, and 3 positive patients (1%) were 75 years or older. In the COVID-positive group, there were 158 men (66%) and 80 women (34%). There were 137 White/non-Hispanic (56%), 55 Hispanic/Latino (23%), 36 Black/non-Hispanic (15%), 6 Asian/Pacific Islander (3%), and 2 Native American COVID-positive patients (1%) in the sample (Table 1). The mean LOS of the positive cohort was 33 days. (During the study period, 120 staff members in the Department of Psychiatry tested positive as well.)
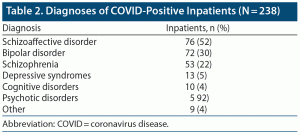
Schizoaffective disorder was the primary diagnosis of 76 (32%) of the COVID-positive patients; 55 positive patients (22%) were diagnosed with schizophrenia, and 5 COVID-positive individuals (5%) were diagnosed with psychotic disorders (delusional disorder, drug-induced psychosis, and brief psychotic disorder). Seventy-two COVID-positive patients (30%) were diagnosed with bipolar disorder, and 13 positive individuals (5%) had depressive syndromes such as major depressive disorder, depressive disorder, and mood disorder. Cognitive disorder was listed for 10 positive patients (4%) in the study. Other categories such as borderline personality disorder, anxiety disorder, adjustment disorder, anorexia, and autism spectrum disorder were found in 9 COVID-positive patients (4%) (Table 2).
Eight positive patients (3%) required medical hospitalizations related to COVID-19. Of these, 4 patients developed pneumonia and made a full recovery. One patient required intubation for weeks and was discharged to a nursing facility. A 79-year-old man, with a “do not resuscitate” directive, was removed from life support and died. Over half of the COVID-positive patients (n = 133 or 56%) were asymptomatic. Many of these cases were detected from testing patients who were exposed to a COVID-positive peer.
Ninety-seven COVID-positive patients (41%) in the sample had at least 1 or more of the known medical comorbidities related to risk for COVID-19 infection (Table 3). Fifty-two patients (54%) in the positive cohort had 1 comorbidity. Twenty-seven positive patients (28%) were identified as having 2 comorbidities, with 17 individuals (63%) having diabetes and hypertension. Three comorbidities were noted in 8 (8%) of the COVID-positive population.
All admissions were placed in designated quarantine areas and received COVID testing, so most patients in the sample were identified within hours of admission. Twenty-nine patients (12%) were found to be positive between 72 hours and 14 days. Fifty-nine individuals (25%) tested positive 14 days or more after admission. Infection spread quickly on the psychiatric units. One patient tested positive for COVID-19, and within a few days 14 other patients on the same housing unit became infected.
The mean LOS in 2020 for the study facilities was 28 days and 33 days for the COVID-positive sample. In previous years, the mean LOS was about 21 days. Records indicated that 45 positive patients (20%) were noted to be ready for discharge from a psychiatric standpoint. Duration of delay was predicated on how long the patient was required to remain on quarantine and proof of a negative COVID-19 test. Once cleared from quarantine, discharge would proceed but may have been impacted by bed availability if the patient was to be discharged to a program or facility. If the patient was returning home, the discharge would be completed as soon as the patient was released from quarantine.
Almost 80% of the discharge-ready COVID-positive patients were to be placed in residential programs, group homes, assisted living, or nursing homes. These patients were denied transfer due to having a positive COVID-19 test. (In the summer of 2020, 1 skilled facility agreed to accept quarantined, exposed COVID-negative patients before the end of the quarantine period.) Other positive patients (9%) had housing, but the patient would not be able to continue quarantine at home, as the home may have had no single room and bath or ability to isolate, the patient voiced unwillingness to continue quarantine, or other residents of the home were at high risk for infection. Another group of COVID-positive patients (6%) were homeless and were unwelcome at shelters of halfway houses as long as on quarantine. (One positive patient [2%] was on conditional release from jail and denied return while still on quarantine.) The last group comprised COVID-positive patients (2%) who refused housing options and would have been discharged to themselves with no plan or intent to quarantine (Table 4). Diagnoses of these positive patients with extended LOS mirrored the study sample as a whole and were not related to the delay in placement.
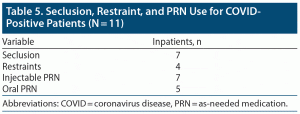
During the study period, 11 seclusion and/or restraint (S&R) events for severe behavioral management issues occurred related to a COVID-positive patient’s inability to remain in quarantine. In 2020, the mean rate of S&R per month in the study facilities was 19 events. During 7 of these COVID-related events, injectable PRN medications were given for severe agitation, and in 5 events oral PRN medications were accepted. Between June 1 and December 31, 2020, PRN medications were administered 334 times on the COVID-positive units compared to 892 doses of PRN medications administered during the same period on a comparable non-COVID treatment unit.
Four COVID-positive patients, all male, required mechanical restraints and injectable PRN medications. With all these patients, the restraints were precipitated by the patients’ refusals to abide by quarantine protocols. Three of the 4 patients were not described in notations as being actively psychotic or impaired at the time of the restraint. One had repeated issues with inappropriate behavior before becoming infected such as disrobing in public areas, jumping on furniture, and going into other peers’ rooms. He was on 1-to-1 supervision before and at the time of the restraint and was still displaying significant psychotic symptoms. The other 7 COVID-positive patients were placed behind a locked door (considered a form of restraint by local regulations) for refusing to remain in their room. Three of the patients in locked seclusion were also given injectable PRN medications. The other positive patients in seclusion received oral PRN medications 5 times (one had repeat doses). Seclusion and restraint events in this group did not directly impact the overall length of stay (Table 5).
Comparisons to County COVID-19 Data
The influx of COVID-positive inpatients mirrored state and national trends, with the first peak occurring in April 2020 and larger spikes seen in July and December 2020 (ongoing into January 2021). The ethnic and racial demographics and sex distribution of the study population differed from data collected for each county by the Arizona Department of Health Services (Dashboard).8 White/non-Hispanic patients comprised 56% of the COVID-positive sample compared to 34% of the same background identified in the general population. Fifteen percent of the positive group was Black/non-Hispanic compared to 3% in the community. The study facilities had slightly lower rates of positivity in the Hispanic/Latino (23% vs 29%) and Native American categories (3% vs 5%) than did the general population. One possible explanation for these disparities is that patients may not fully cooperate during admission, so the ethnic and racial designation is then gathered from records, legal documents, or assumptions made by hospital staff or other agencies. The lower rate of admissions of Native Americans is not surprising because the tribes manage their own mental health care system.
In the study cohort, 67% of COVID-positive inpatients were male compared to 48% in the community at large as found on the Dashboard, and 34% of female patients were infected compared to 52% in the general population.8 One likely explanation for this difference is that the facilities have several single-sex units. The first COVID-19 outbreak in April 2020 occurred on an all-male unit resulting in 34 positive cases compared to only 5 female patients testing positive during the same period. Several other outbreaks during the study period also occurred on all-male units.
The Dashboard reported that 13% of the COVID-positive population was over the age of 65 years.8 In the study’s hospitals, 5% of the infected patients were over 65 years of age. The hospital has an identified geropsychiatry/medical unit and is equipped to manage the needs of elderly dementia patients and those with complex medical illnesses. Capacity on this unit, however, is limited, which may have affected the data.
The Dashboard indicated that the medical hospitalization rate for the community was 7% for 2020.8 The psychiatric inpatient rate of medical hospitalization was 3%. The state recorded a death rate of 0.13% out of 4.5 million COVID-positive community cases.8 Only 1 patient in the cohort died, which represents 0.4% of a very small sample in comparison. The patient’s family made the determination to terminate life support, so, ultimately, it remains a question as to whether he may have survived.
Twenty-nine percent of the COVID-positive sample had at least 1 of the identified high-risk medical comorbidities known for increased risk for COVID-19 infection. The state reported that 16% of the COVID-positive general population had at least 1 of these comorbidities.8 Cardiac conditions were the most common disorders noted in the study, followed by lung diseases and diabetes. Diabetes and hypertension were found in 63% of inpatients with 2 comorbidities.
Unfortunately, the Dashboard does not collect data specifically on the population with mental illness. Although the study’s health system has several outpatient mental health clinics, COVID-19 testing results were not routinely being collected.
DISCUSSION
There is no doubt that COVID-19 is highly contagious. Early in the pandemic, the study facilities’ newly admitted patients were placed in quarantine until a negative COVID-19 test resulted and then were moved to an open unit. With the 14-day incubation period of COVID-19, it is difficult to trace the nexus of spread of the infection. In the first group of infected inpatients, the first 2 positive patients were thought to represent the epicenter of subsequent spread on the same unit. It is suspected that other positive patients on an adjacent unit could have been infected by an asymptomatic peer (who may have tested negative at first) or staff. As a result of this first wave of positive patients, admitted patients were kept in quarantine for 72 hours after a negative COVID-19 test to monitor them further in case of a false-negative result. Staff members, who often move between units, were assigned to only 1 unit to decrease potential exposures. Despite these added measures, COVID-19 outbreaks still occurred, and in some cases, there were no identifiable positive patients, which suggests that staff may have been the carrier.
Another factor that contributed to the spread of COVID-19 in the study setting was patients’ difficulties adhering to guidelines for social distancing, wearing masks, and frequent handwashing. In quarantined areas, therapeutic group activities were suspended to diminish person-to-person contact; however, on nonquarantined units, group activities continued with social distancing. Furniture on the units was reduced to create distance between people, but common areas had limited space. Regardless of the risk and staff admonitions, patients tended to gather in small groups to socialize or during meals. In the study locations, patients share rooms, showers, and bathrooms. Some patients were vigilant about wearing masks, but many were not. Hand sanitizers were available for use, but some patients were inattentive to hand cleaning. As the pandemic continued, many became weary of following infection control guidelines.
Although several inpatients expressed delusions about the pandemic being connected to government conspiracies or supported “anti-pandemic” rhetoric, no known patient refused to cooperate with infection control procedures, believing that the pandemic was a falsehood. More commonly, patients voiced realistic concerns of paranoia about contracting COVID-19 and the potential to develop serious illness. Some patients were too psychiatrically impaired to appreciate the gravity of the pandemic or were unable to adhere to infection control protocols. A small number of patients never fully understood that there was a public health crisis. A recently published study9 found that three-quarters of patients surveyed were not concerned about contracting COVID-19 and lacked adequate knowledge about the symptoms of the illness. Two-thirds of the respondents lacked knowledge of necessary precautionary measures to protect from infection, and 30% had a relapse of their psychiatric symptoms while on lockdown.9
Many feared the devastating effects of COVID-19 on the vulnerable SMI population due to a higher morbidity rate than seen in the general population, high rates of comorbid medical issues that are risk factors for COVID-19 infection, homelessness, poverty, limited access to medical and psychiatric care, and lack of a support network. The study cohort had fewer medical hospitalizations for COVID-19 than did the public, and of 238 patients there was only 1 death. From a statistical standpoint, this was almost 4 times greater than the death rate in the community; however, the state’s statistics are based on over 4 million cases. Even though the inpatient sample had a higher rate of COVID-related medical comorbidities than did the general population, the sample had fewer hospitalizations than the public and were either asymptomatic or had mild symptoms from infection. Only 1 patient required placement in a nursing facility after recovering from COVID-19. No patients had any noted complaints after recovering from COVID-19 during the remainder of their inpatient stay.
There was a concern that COVID-19 would adversely affect the well-being of SMI patients. Well-being, often defined as the experience of health, happiness, and prosperity, includes good mental health, high life satisfaction, a sense of meaning or purpose, and an ability to manage stress. Many variables influence and promote well-being that are hard to quantify. In a study by Liu et al,10 hospitalized patients with schizophrenia and suspected COVID-19 infection showed higher scores on the Perceived Stress Scale, the Hamilton Anxiety and Depression Inventory, and the Pittsburgh Sleep Quality Index. In a study11 of SMI patients evaluated after 1-month quarantine, elevations were found on the 7-item Generalized Anxiety Disorder Scale, the 9-item Patient Health Questionnaire, and the Specific and Psychotic Experience Questionnaire.
In this study, variables related to a psychiatric hospitalization that might impact patients’ well-being or increase psychiatric symptoms causing decompensation were examined. LOS may serve as an indirect indicator of patient well-being, and it was affected by COVID-19 in the study. There was documentation in the records of 45 patients (19%) for whom discharge was hindered due to COVID-19 infection. There are 3 probable explanations for this finding. First, many patients in the study facilities are discharged to residential housing programs. Most of these placements refused to accept a COVID-positive patient until after the completion of a 14-day quarantine. A second reason was that many patients did not have the capacity to self-quarantine either due to the physical limitations of their housing (eg, shared space) or an inability to follow quarantine requirements. Lastly, some patients experienced worsening of their mental health symptoms due to the prolonged LOS. Extension of the LOS can be demoralizing and impact well-being of the patient while remaining in an acute locked facility when ready and able to move on to community living.
This study examined S&R events as another indirect indicator of patient well-being. The need for S&R suggests that those requiring such interventions are significantly impaired and unable to manage their behavior in a nonaggressive manner. In the sample, there were 11 S&R events, all related to patients endangering staff, peers, or themselves by becoming physically aggressive related to being quarantined. Interestingly, all these events occurred in April 2020 when staff were first learning to manage COVID-positive patients. This finding suggests that, with time, staff became more adept at managing aggression with quarantined patients. It may also reflect the recognition that boredom and lack of stimulation while in quarantine were problematic for the patients and resources were developed to engage quarantined patients. These resources included more varied recreational material, internet use (not approved for COVID-negative peers) with access to preselected games and movies, and e-mail and cell phones (also not approved for COVID-negative patients).
Use of PRN medication is another indirect measure of patient well-being. Patients may request extra medications to address breakthrough symptoms such as anxiety, agitation, or psychosis. During the study, PRN medication administration on the COVID-positive units was almost two-thirds less than what was given on the COVID-negative units. It is possible that being in quarantine, with the accompanying decrease in stimulation, less ambient noise, and fewer interactions with others, was less provoking compared to a typical day on the unit.
CONCLUSION
The data from the study cohort offered a few surprises. The inpatient population fared better than anticipated in several ways, including fewer medical hospitalizations, minimal medical sequalae from COVID infection, and fewer elderly patients contracting COVID-19 compared to the general population’s statistics. On indirect measures of well-being, the sample also did relatively well in comparison to noninfected peers with respect to the number of S&R events and administration of PRN medication.
The sample did have a much higher rate of medical comorbidities than seen in the community. This finding emphasizes the importance of identifying and treating coexisting medical conditions collaboratively in the SMI community.
The increased LOS in the study population was a regrettable finding and may have had a negative impact on the well-being of the study sample. The extended LOS also impacts the community’s mental health resources. Increasing LOS for patients who are otherwise ready to be discharged prevents admissions of acutely ill psychiatric patients to the hospital due to limited bed capacity. This situation forces those awaiting admission to remain in psychiatric urgent care, medical hospitals, and emergency room beds. These patients are being managed in these settings but are not receiving active psychiatric treatment.
As we learn more about COVID-19 infection, sequelae, and long-term consequences of the pandemic, psychiatric providers become better informed about treating patients during a pandemic and learn ways to mold policies and processes to optimize care. More research is needed to clarify the ways in which this pandemic and its aftermath may specifically impact the SMI population.
Submitted: April 30, 2021; accepted July 15, 2021.
Published online: September 9, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Acknowledgments: Jennifer Weller, PhD (Department of Psychiatry, District Medical Group, Phoenix, Arizona) for her editorial assistance. Dr Weller has no conflicts of interest related to the subject of this article.
Clinical Points
- A cohort of psychiatric inpatients with coronavirus disease 2019 (COVID-19) had positive outcomes from a medical and psychiatric standpoint.
- COVID-19 positivity had no significant impact on patient well-being compared to COVID-negative patients in the study.
- Some COVID-positive inpatients had longer lengths of stay in the hospital due to having the infection and needing quarantine.
References (11)

- Yao H, Chen JH, Xu YF. Patients with mental health disorders in the COVID-19 epidemic. Lancet Psychiatry. 2020;7(4):e21. PubMed CrossRef
- Park J, Svendsen D, Singer P, et al. Morbidity and mortality in people with serious mental illness. National Association of State Mental Health Program Directors, Medical Director’s Council Technical Reports. Accessed June 15, 2020. https://www.nasmhpd.org/content/morbidity-and-mortality-people-serious-mental-illness.
- COVID-19: Interim Considerations for State Psychiatric Hospitals. Substance Abuse and Mental Health Services Administration. Accessed August 26, 2021. https://www.samhsa.gov/sites/default/files/covid19-interim-considerations-for-state-psychiatric-hospitals.pdf
- COVID-19 Hospitalizations and Death by Race and Ethnicity. Accessed January 28, 2021. https://stacks.cdc.gov/view/cdc/91857
- Hamada K, Fan X. The impact of COVID-19 on individuals living with serious mental illness. Schizophr Res. 2020;222:3–5. PubMed CrossRef
- Barber S, Reed L, Syam N, et al. Severe mental illness and risks from COVID-19. The Centre for Evidence-Based Medicine: Evidence Service to support the COVID-19 response. Accessed August 26, 2021. https://www.cebm.net/covid-19/severe-mental-illness-and-risks-from-covid-19/
- Linz SJ, Sturm BA. The phenomenon of social isolation in the severely mentally ill. Perspect Psychiatr Care. 2013;49(4):243–254. PubMed CrossRef
- COVID-19 Data Dashboard. Arizona Department of Health Services. Accessed August 20, 2021. https://www.azdhs.gov/preparedness/epidemiology-disease-control/infectious-disease-epidemiology/covid-19/dashboards/index.php
- Muruganandam P, Neelamegam S, Menon V, et al. COVID-19 and severe mental illness: impact on patients and its relation with their awareness about COVID-19. Psychiatry Res. 2020;291:113265. PubMed CrossRef
- Liu X, Lin H, Jiang H, et al. Clinical characteristics of hospitalised patients with schizophrenia who were suspected to have coronavirus disease (COVID-19) in Hubei Province, China. Gen Psychiatr. 2020;33(2):e100222. PubMed CrossRef
- Iasevoli F, Fornaro M, D’Urso G, et al; COVID-19 in Psychiatry Study Group. Psychological distress in patients with serious mental illness during the COVID-19 outbreak and one-month mass quarantine in Italy. Psychol Med. 2021;51(6):1054–1056. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!