ABSTRACT
Objective: In the context of the coronavirus disease 2019 (COVID-19) pandemic, anxiety during pregnancy should be assessed from a composite context of anxiety/fear of COVID-19 infection and pregnancy-specific anxiety. The objective of this study was to develop and validate a scale that measures anxiety related to situations specific to pregnancy during the COVID-19 pandemic—the Antenatal COVID-19 Anxiety (AnCAn) Scale.
Methods: Items were generated based on a literature review and focused group discussions. Face and content validation was completed. Data were collected from 557 pregnant women attending antenatal clinics of 5 tertiary care general hospitals in India. An exploratory factor analysis was conducted to measure structural validity and to identify latent factors. Screening accuracy was assessed using scores on the 7-item Generalized Anxiety Disorder scale. Data were collected between July and October 2020.
Results: The principal component analysis showed that the 12 items of the scale significantly loaded onto 2 latent factors, with Eigen values of 6.575 and 1.213, respectively. Factor solution showed that 6 items correlated with each of the 2 factors. Both sensitivity and specificity of AnCAn total and subscores were > 70%.
Conclusions: We conclude that the AnCAn Scale holds good psychometric properties, and it identifies and distinguishes 2 latent factors: (1) anxiety related to acquiring infection and (2) anxiety related to spreading infection and social role obligations, which are compositely related to anxiety specific to COVID-19 and pregnancy.
Prim Care Companion CNS Disord 2021;23(6):21m03038
To cite: Tikka SK, Parial S, Lahiri D, et al. Development and validation of a scale to measure anxiety specific to pregnancy during the COVID-19 pandemic: the Antenatal COVID-19 Anxiety Scale. Prim Care Companion CNS Disord. 2021;23(6):21m03038.
To share: https://doi.org/10.4088/PCC.21m03038
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, All India Institute of Medical Sciences, Bibinagar, India
bDhanwantari Clinic and Hospital, Raipur, India
cDepartment of Clinical Psychology, Postgraduate Institute of Behavioral and Medical Sciences, Raipur, India
dAuckland District Health Board, Auckland, New Zealand
eDepartment of Psychiatry, National Institute of Mental Health and Neurosciences, Bengaluru, India
fCAn Study Group Collaborators are listed at the end of this article.
*Corresponding author: Prabha S. Chandra, MD, Department of Psychiatry, National Institute of Mental Health and Neurosciences, Hosur Rd, Bengaluru 560029, India ([email protected]).
The coronavirus disease 2019 (COVID-19) pandemic has now spanned more than a year. The second wave of the pandemic in India is taking a heavy toll on people’s lives as well as on health and human resources. Older adults and people with long-standing systemic health conditions such as cancer, chronic kidney and lung diseases, and diabetes are particularly more likely to become severely ill. The Centers for Disease Control and Prevention (CDC) has stated that pregnant women who acquire COVID-19 infection are at greater risk of developing severe illness and requiring intensive care, including ventilator support, than women who are not pregnant.1 Recent evidence also suggests that COVID-19 infection during pregnancy is associated with potentially serious consequences on neonatal health such as preterm delivery and abnormal neonatal brain development.2 Since the COVID-19 outbreak began, pregnant women were cautioned by the CDC to be “at an increased risk of severe illness from COVID-19” and it was recommended that they take extra precautions.3 In general, the “precautionary behaviors,” which consequently would reduce the risk of infection, have been found to be directly related to anxiety about COVID-19 infection.4 While pregnant women with higher levels of COVID-19–related anxiety may use greater precautionary behaviors, they may also be at risk of developing an anxiety disorder.5
Clinically significant levels of such specific anxiety or fear of COVID-19 (“coronaphobia”) is now being understood as a distinct entity that is associated with dysfunction similar to other anxiety disorders.6 This specific anxiety related to COVID-19 has certain cognitive (eg, “my family is in danger and they may die”) and behavioral (eg, marked fear of using public transportation and subsequent avoidance) components.6 In pregnant women, the presentation of such specific anxiety may be distinct and more focused toward her pregnancy and unborn fetus. Pregnancy-specific anxiety (PSA),7 which is specifically related to worries and fears about pregnancy, childbirth (tocophobia), infant health, and parenting, has been found to be significantly higher during the pandemic.8 A survey among obstetricians indicated high levels of concern among pregnant and postpartum women regarding contracting COVID-19 infection, safety of their infant, safety related to hospital visits, methods of protection against COVID-19, and anxieties related to social media messages.9 As anxiety/fear of COVID-19 during pregnancy and PSA are closely related,10 assessing anxiety that is specific to the composite context of COVID-19 and pregnancy is important.
We aimed to develop and validate a scale with items that measure anxiety related to situations specific to pregnancy during the COVID-19 pandemic.
METHODS
Development and validation of the Antenatal COVID-19 Anxiety (AnCAn) Scale was part of the COVID-19 Antenatal Anxiety (CAn) Study, a multicenter study assessing various aspects of anxiety in pregnant women during the COVID-19 pandemic. The study was approved by the institutional ethics committee (1147/IEC-AIIMSRPR/2020).
Item Generation
The item generation was based on a review of the literature for various available tools pertinent to “anxiety specific to pregnancy during the COVID-19 outbreak” and on group discussions by experts.
Face and Content Validation
Face and content validation was performed in 2 steps. The scale and validity questionnaire were sent to experts (mental health professionals or obstetricians) with > 10 years of experience. Experts rated each item of the scale on 3 assertions (relevance to COVID-19 and antenatal/pregnancy–related anxiety, proper framing of the question, and appropriateness of the Likert scale to the item) on a 5-point Likert scale (1 = strongly disagree, 5 = strongly agree) and provided remarks reasoning the score provided. In the first step, assertions for items that received a score < 4 (agree) from > 25% of the experts were identified and modified as per remarks of the experts. In the second step, the revised scale was sent back for a review and rescoring. The responses were reassessed according to the above criteria. The final version (English) was then translated into Hindi by 2 language experts.
Data Collection
Data analyzed for validation of the scale were collected from pregnant women attending the antenatal clinics of 5 centers in North, Central, and East India (All India Institute of Medical Sciences [AIIMS] Raipur [primary study site]; Lady Hardinge Medical College, New Delhi; Pt. JNM Medical College, Raipur; Shri Guru Ram Rai Institute of Medical and Health Sciences, Dehradun; and Hi-Tech Medical College, Bhubaneshwar). Written informed consent was obtained from all participants. Data were collected between July and October 2020. A uniform standard operating procedure for data collection was followed across the 5 centers. Data were collected by trained residents in psychiatry/obstetrics under the supervision of a teaching faculty from the department of psychiatry at each study site. Data collected using the Hindi version of the scale were used for the analysis.
Women attending antenatal clinics at the study centers (1) with confirmed pregnancy, (2) with gestational period < 36 completed weeks, and (3) who were willing to provide written informed consent were included in the study. Pregnant women with current history of any psychotic disorder were excluded. Sample characteristics are described in Supplementary Table 1.
Pilot Testing
The data collected from pregnant women in the first week of the study at the primary study site (antenatal clinic of AIIMS Raipur) were considered as pilot testing data and were reassessed for comprehensibility and relevance of the scale items.
Structural Validity
Exploratory factor analysis was conducted to determine the structural validity of the 12-item scale. Completed forms of the 12-item Hindi version of the scale from 557 pregnant women were analyzed. Analysis was conducted using Statistical Package for Social Sciences version 23 (IBM Corporation, New York, New York). Assumptions for the exploratory factor analysis were analyzed using the Kaiser-Meyer-Olkin test (for sample size adequacy), the Bartlett test of sphericity (for inter-item correlation significance), and the communality assessment (for strength of factor extraction). Factor extraction was done using the principal component analysis (PCA) and confirmed using the parallel analysis (https://analytics.gonzaga.edu/parallelengine/). As the component correlation matrix showed the 2 factors were obliquely related (ie, correlation between the 2 factors was > 0.5 [0.611]), the oblique (direct Oblimin) rotation method was used for the factor solution rotation. Quartile scores were noted.
Factor Reliability
The items that correlated with each of the extracted factors were assessed for reliability using Cronbach α. Item deletion was planned if the factor reliability (ie, Cronbach α) for any of the extracted factors was < 0.07.
Screening Accuracy
To test for screening accuracy, the sample was simultaneously rated on the Hindi translated version of the 7-item Generalized Anxiety Disorder (GAD-7) scale,11 which is the most common tool used to screen for anxiety disorders. The GAD-7 has also been used specifically in the context of COVID-19 in pregnant women.12 A score of 10 on the GAD-7 was interpreted as the cutoff for significant anxiety. The cutoff scores for the AnCAn were based on the third quartile (ie, Q3) score; a score greater than or equal to the Q3 was considered the cutoff. This cutoff was chosen because the distribution of AnCAn total and both factor scores in our sample was positively skewed (Supplementary Figures 1A–1C). Using these cutoffs, the sample was binarily classified. Contingency tables were formulated to assess for measures of screening accuracy (ie, sensitivity, specificity, precision, and accuracy) for AnCAn total and subscale scores. The McNemar test was conducted to assess for accuracy homogeneity.
RESULTS
Item Generation
Initially, 25 items were generated based on expert opinion by 3 perinatal psychiatrists who conducted and were informed by an extensive literature review of anxiety among pregnant women during the pandemic. These experts then held an online meeting, during which items were finalized by consensus. The 3 mental health professionals had a mean experience of 13.3 years. Items from the Pregnancy-Related Anxiety Scale (PRAS),13 the Perinatal Anxiety Screening Scale (PASS),14 the questionnaire on attitudes and behavior relating to COVID-19 by Corbett et al,10 the Coronavirus Anxiety Scale (CAS),15 survey findings of the COVID-19–related anxiety and concerns expressed by pregnant and postpartum women to obstetricians in India,9 and the NIMHANS Perinatal Mental Health Services–Guidance Note for Pregnant and Postpartum Women16 were reviewed during these discussions. A Likert scale of 0–3 (never, rarely, sometimes, and very often) was also added to the items. Qualitative item reduction was then carried out based on expert advice from 2 mental health professionals with specific expertise in perinatal psychiatry/maternal mental health. Items were reduced to 14 by combining the content of 2 or more items and by deleting items that were conceptually similar to others.
Face and Content Validation
Face and content validation of the 14-item scale was then performed in 2 steps. The scale and validity questionnaire were sent to 21 experts (with > 10 years of experience) who were either mental health professionals or obstetricians. Eighteen experts (7 psychiatrists, 6 clinical psychologists, and 5 obstetricians) returned the questionnaire, and 16 response sheets were deemed valid. In the first step, 7 cells (2 items on the first assertion and 5 items on the second assertion) received a score < 4 (agree) from > 25% of the experts. As per the remarks, 2 items were combined, 1 item was removed, and 4 items were reframed. In the second step, the revised scale with 12 items was sent back for review and rescoring. When the responses were reassessed using the above criteria, none of the assertions received a score < 4 (agree) from > 25% of the experts. The final 12-item scale with average scores for each assertion for each item on the face/content validation are provided in Supplementary Table 2.
Pilot Testing
The scale was administered to 11 pregnant women as part of the pilot testing. All women understood the items and found them to be relevant. None of the women reported ambiguity with respect to content of any of the items.
Structural Validity
The mean AnCAn score for the participants was 9.76 (SD = 8.01); first, second, and third quartile (ie, Q1, Q2, and Q3) AnCAn scores for the participants were 3, 8, and 16, respectively. The assumptions for exploratory factor analysis were assessed and found to be satisfactory.
- The sample size of 557 was sufficiently larger than the recommended sample size of 180 (ie, 15 participants per item [12 items]). This sample size adequacy was further confirmed using the Kaiser-Meyer-Olkin test measure, which was found to be 0.919.
- The correlations between each of the 12 items were found to be statistically significant (P < .001) (Supplementary Table 3). The Bartlett test of sphericity was also found to be statistically significant (χ2 = 4,063.15; P < .001).
- The strength of extraction (ie, communality) for all the items was found to be greater than > 0.5.
The PCA showed that the Eigen values were > 1 for 2 extracted factors (6.575 and 1.213, respectively; the screen plot is provided in Figure 1). The PCA-calculated Eigen values for the 2 factors were greater than the mean Eigen values of the parallel analysis (1.243 and 1.181, respectively).
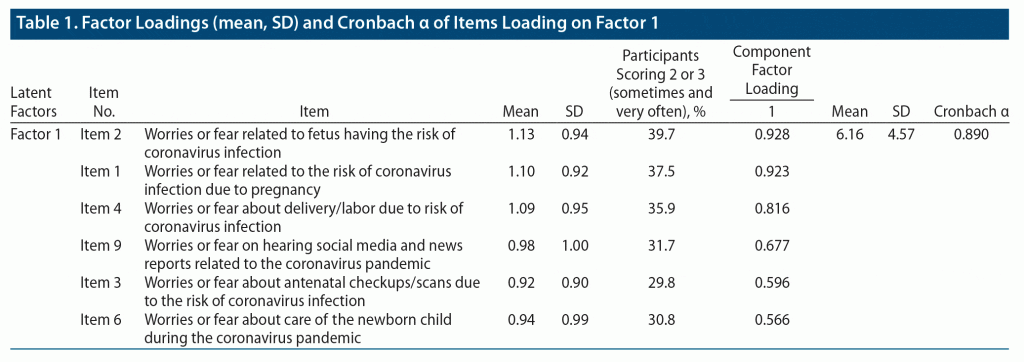
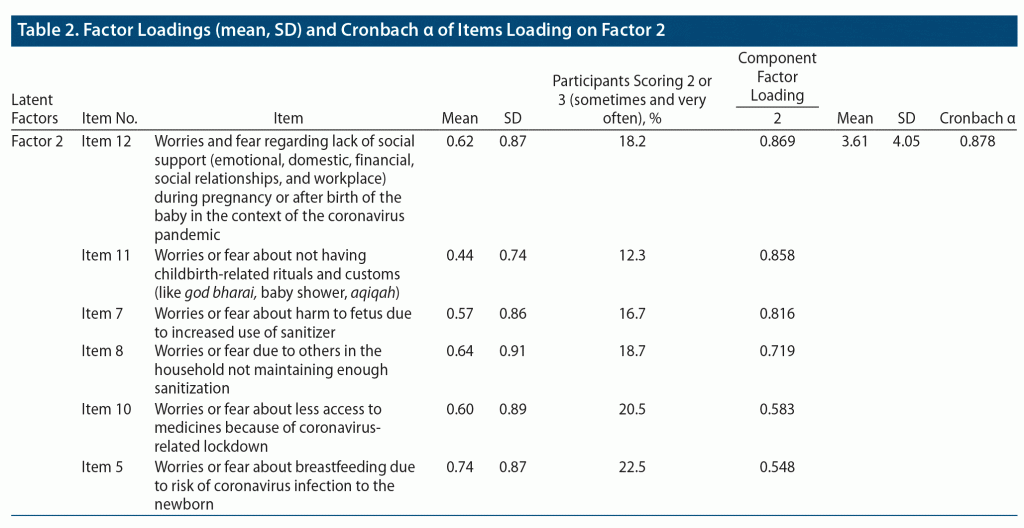
The rotated component matrix (Table 1 and Table 2) showed that items 1, 2, 3, 4, 6, and 9 are related to latent factor 1, and items 5, 7, 8, 10, 11, and 12 are related to latent factor 2. The correlation of items within those that loaded onto each of the 2 factors was significant (ie, > 0.5). The mean AnCAn scores for items that loaded onto latent factor 1 and latent factor 2 were 6.16 (SD = 4.57) and 3.61 (SD = 4.05), respectively. While Q1, Q2, and Q3 for AnCAn scores on items that loaded onto latent factor 1 were 2, 6, and 10, respectively, they were 0, 2, and 6 for AnCAn scores on items that loaded onto latent factor 2.
Factor Reliability
The factor reliability for both extracted factors was found to be good. The Cronbach α for factor 1 was 0.890 and for factor 2 was 0.878 (Table 1 and Table 2). No items were required to be deleted.
Screening Accuracy
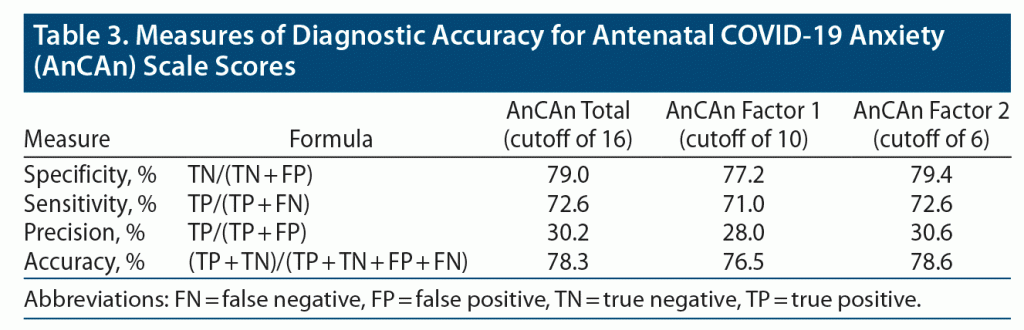
The cutoff scores used to classify the sample based on AnCAn total, factor 1, and factor 2 scores were 16, 10, and 6, respectively. Table 3 shows measures of screening accuracy: sensitivity, specificity, precision, and accuracy for the AnCAn Scale scores. Supplementary Tables 4a–4c show 2 × 2 tables for AnCAn total, factor 1, and factor 2 cutoffs versus the GAD-7 cutoff and corresponding results from the McNemar test showing significant accuracy heterogeneity.
DISCUSSION
We found that the AnCAn Scale holds good psychometric properties. The analysis shows that the AnCAn Scale identifies and distinguishes responses on 2 latent factors. The 2 latent factors identified in the analysis can be interpreted as those related to (1) acquiring infection and (2) spreading infection and social role obligations. From the context of how the pandemic implications have panned out, we argue that these 2 factors might represent a principal (P) and a contingent (C) factor, respectively. We surmise that both factors are pertinent to the composite context of COVID-19 and pregnancy-specific anxiety and that the AnCAn Scale can contribute to the understanding of anxiety among pregnant women during the COVID-19 pandemic.
First, the P factor for antenatal COVID-19 anxiety is primarily related to worries/fears of acquiring the infection. While 2 items (items 1 and 2) that loaded on this factor directly relate to risk of acquiring infection, 2 items (items 3 and 4) relate to acquiring infection from accessing perinatal health services. While the former 2 items imply cognitive aspects of anxiety, the latter 2 items suggest avoidance, which is the behavioral aspect of anxiety. This factor loaded onto 2 more items: fear related to media updates and fear of newborn care. These 2 items, first behavioral and second cognitive, imply “catastrophizing” related to acquiring the COVID-19 infection. The media portrayal of deaths and the horrific visuals of COVID-19–related funerals invoke extreme catastrophizing thoughts and subsequent personalization to care of self and the unborn baby, which heightens anxiety further. Item 10, anxiety related to breastfeeding, is also related to catastrophizing and personalization. Surprisingly, however, it loaded onto the C factor, albeit small factor loading. A plausible reason for this finding might be that these women were not primarily concerned about breastfeeding their newborns at the stage of pregnancy in which they were assessed.
Next, the items loaded on the second factor, the C factor, represent worries and fears contingent upon those in factor P. The first set of items (items 7 and 8) are those related to spread of infection within the family and spread of harm from measures of safety against infection. The rest of the 4 items relate to the social role of the pregnant woman. While items 5 and 10 represent the worry of inability to perform a social obligation, ie, providing optimum health care to one’s own pregnancy and therefore the child, item 11 represents worry of inability to perform a cultural ritual that is believed to bring good health to the woman and the unborn child. Item 12 represents worries regarding the inability of family to perform their social roles toward the woman’s and unborn baby’s health. While, item 8 mostly implies the behavioral aspect of anxiety, all other items loading onto factor C denote cognitive anxiety.
The participants responded to the items of the P factor with higher scores compared to the items of the C factor. There was a noticeable difference between the 2 factors in the mean scores and the percentage of participants scoring “sometimes” and “very often”. This finding might reflect the population perception during the months of data collection. Data for this study were collected between July and October 2020, and although the number of active cases was peaking during this time, public restrictions began to be waived. Health education from reliable scientific sources was more accessible. As the number of active cases was at its peak, the worries of acquiring infection were still high, especially from hospitals, which had the maximum case load. On the other hand, information regarding “no or only minimal” additional risk among pregnant women for adverse outcomes as well as vertical transmission and transmission of the virus through human milk/breastfeeding17–19 started to circulate. Also, complete access to outdoor “social” spaces became more common. These factors might have led to the distinction in the scoring pattern for the items loading onto the 2 latent factors.
The screening accuracy assessment showed that the AnCAn Scale has optimum validity and can be used to determine severity of antenatal COVID-19 anxiety. The AnCAn total, factor 1, and factor 2 scores of 16, 10, and 6, respectively, may be considered as cutoffs for significantly higher levels of anxiety. With both sensitivity and specificity of the AnCAn total, factor 1, and factor 2 scores > 70%, we deem that our scale may generate meaningful probability of a woman having or not having significant anxiety levels. However, women screening positive with these cutoffs are less likely to have generalized anxiety, as the precision values for the AnCAn total, factor 1, and factor 2 scores were only about 30%. Also, there was significant accuracy heterogeneity between GAD-7 and AnCAn scores.
Worries and fears regarding COVID-19 infection compound the already elevated rates of anxiety in pregnant women, which is particularly important in low- and middle-income countries20 and especially in India, which has reported rates of anxiety > 50% in pregnant women.21,22 Perhaps the worries and fears pertinent to factor P are those that are commonly reported by pregnant women to their obstetricians in India.9 The already known factors that distinctly determine COVID-19 anxiety—uncertainties; human ability to acquire new behaviors and modify and avoid old ones, including those related to faith and media portrayals6; and pregnancy-specific anxiety (family and marital support, domestic violence, and preferred sex of the baby)7,23—may have complex interaction in determining antenatal COVID-19 anxiety.
Strengths, Limitations, and Future Directions
The development of the AnCAn Scale is based on a strong methodology and integrates content from several related tools. It is the first tool to assess the composite context of COVID-19 and pregnancy–related anxiety. That the AnCAn Scale can be administered in a very short time frame adds to its value given the restricted time for person-to-person interaction and other COVID protocols.
However, we understand that owing to the ever-changing rates of COVID-19 infection, emergence of local virus variants with varying levels of infectivity, revised government policies with respect to pandemic-led restrictions and vaccination, and resultant changes in public perception might influence the response scores for each of the factors identified. It remains to be examined whether the factor solution we obtained is stable across various phases of the pandemic. Similarly, the cutoffs for significant antenatal COVID-19 anxiety that we propose also need to be assessed for stability in future studies.
Although the basic construct of the GAD-7 and AnCAn is assessment of anxiety, there are apparent differences in the context of anxieties assessed, which has been reflected in the low precision values and significant accuracy heterogeneity. Clinically, like other anxiety scales, AnCAn scores may be influenced by any preexisting depressive or anxiety disorder or trait anxiety. Moreover, our scale has no items that represent autonomic aspects of anxiety because the AnCAn is specific to the context of pregnancy, wherein there is significant overlap of physical symptoms of pregnancy and autonomic symptoms of anxiety. Therefore, although useful to identify significant anxiety, the sensitivity and specificity we found may not be directly translatable to day-to-day clinics to determine a “disorder” status. To further demonstrate the clinical value, additional study is needed to determine which cutoff scores of the AnCAn might relate to functional impairments, pregnancy outcomes, and antenatal health utilization. Factors such as partner support, COVID-19–related care, and prevalence rates of COVID-19 infection in a specific area as well as quality of COVID-19–related medical care may also influence the scores. Future research will be needed to assess how the AnCAn Scale can be used in rural and community antenatal settings as well as the change in scores with specific health interventions.
CONCLUSION
We conclude that the AnCAn Scale holds good psychometric properties, and it identifies and distinguishes 2 latent factors that are compositely related to anxiety specific to COVID-19 and pregnancy. Our results also suggest that the AnCAn Scale can be used to screen women with significant antenatal COVID-19 anxiety with fairly good validity.
Submitted: June 6, 2021; accepted September 2, 2021.
Published online: December 2, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Acknowledgments: The authors thank Anindya Das, MD (Department of Psychiatry, All India Institute of Medical Sciences, Rishikesh, India); J. Saroj Naidu, DGO (Saroj Nursing Home, Raipur, India); Jyoti Mishra, PhD (Department of Psychiatry, GMCH, Chandigarh, India); M. Aleem Siddique, MD (Department of Psychiatry, GSVM Medical College, Kanpur, India); Nishant Goyal, MD (Department of Psychiatry, CIP, Ranchi, India); Preeti Gupta, PhD (Department of Clinical Psychology, CIP, Ranchi, India); Preeti Mishra, PhD (Department of Psychiatry, SGRRIMS, Dehradun, India); Pushpawati Thakur, MD (Department of Obstetrics and Gynecology, All India Institute of Medical Sciences, Raipur, India); Rajani Chatterjee, MD (Bhopal Memorial Hospital and Research Centre, Bhopal, India); Shahul Ameen, MD (St. Thomas Hospital, Changanacherry, India); Shashi Rai, MD (Sambal Drug De-addiction and Psychiatric Hospital, Lucknow, India); Sujit Sarkhel, MD (Institute of Psychiatry, Kolkata, India); Sukanto Sarkar, MD (Department of Psychiatry, All India Institute of Medical Sciences, Kalyani, India); Thomas Kishore, PhD (Department of Clinical Psychology, NIMHANS, Bengaluru, India); Uma Ram, MD (Seethapathy Clinic and Hospital, Chennai, India); and Vikram Singh Rawat, MD (Department of Psychiatry, All India Institute of Medical Sciences, Rishikesh, India) for their assistance during the content validation exercise. These individuals report no conflicts of interest related to the subject of this article. The authors also thank the nursing and support staff at each of the 5 centers for their cooperation during data collection, as well as the staff of Dhanwantari Clinic and Hospital, Raipur, for their help during the translation process.
CAn Study Group Collaborators: Amrit Pattojoshi, MD (Department of Psychiatry, Hi-Tech Medical College and Hospital, Bhubaneshwar, India); Ashlesha Bagadia, MRCPsych (Green Oak Initiative, Bengaluru, India); Jyoti Jaiswal, MD (Department of Obstetrics and Gynecology, Pt. Jawaharlal Nehru Memorial Medical College, Raipur, India); Manju Puri, MD (Department of Obstetrics and Gynecology, Lady Hardinge Medical College, New Delhi, India); Prerna Kukreti, MD (Department of Psychiatry, Lady Hardinge Medical College, New Delhi, India); Rabindra Nath Behera, MD (Department of Obstetrics and Gynecology, Hi-Tech Medical College and Hospital, Bhubaneshwar, India); Sarita Agarwal, MD (Department of Obstetrics and Gynecology, All India Institute of Medical Sciences, Raipur, India); Shobit Garg, MD (Department of Psychiatry, Shri Guru Ram Rai Institute of Medical and Health Sciences, Dehradun, India); Surbhi Dubey, MD (Department of Psychiatry, Pt. Jawaharlal Nehru Memorial Medical College, Raipur, India); Vineeta Gupta, MD (Department of Obstetrics and Gynecology, Shri Guru Ram Rai Institute of Medical and Health Sciences, Dehradun, India); Akanksha Agrawal, MBBS (Department of Obstetrics and Gynecology, Pt. Jawaharlal Nehru Memorial Medical College, Raipur, India); Chhaya Singour, MD (Department of Psychiatry, Pt. Jawaharlal Nehru Memorial Medical College, Raipur, India); Geetanjali Patel, MBBS (Department of Obstetrics and Gynecology, Pt. Jawaharlal Nehru Memorial Medical College, Raipur, India); Megha Maghade, MD (Department of Psychiatry, All India Institute of Medical Sciences, Raipur, India); Purushotham A, MD (Department of Psychiatry, All India Institute of Medical Sciences, Raipur, India); Sanjaya Kumar Pany, MD (Department of Psychiatry, Hi-Tech Medical College and Hospital, Bhubaneshwar, India); Saurabh, MD (Department of Psychiatry, Lady Hardinge Medical College, New Delhi, India); Simran Doria, MD (Department of Psychiatry, Lady Hardinge Medical College, New Delhi, India); and Veena Tejan, MD (Department of Psychiatry, Shri Guru Ram Rai Institute of Medical and Health Sciences, Dehradun, India).
Supplementary material: See accompanying pages.
Clinical Points
- The Antenatal COVID-19 Anxiety (AnCAn) Scale has been developed to aid in the assessment of anxiety among pregnant women in the context of the COVID-19 pandemic.
- The AnCAn Scale demonstrates optimum validity among pregnant women with 2 distinct factors related to anxiety due to (1) acquiring infection and (2) spreading infection and social role obligations.
- The AnCAn Scale can be used to assess the role of anxiety related to the COVID-19 pandemic in determining antenatal health care utilization, pregnancy outcomes, and postpartum mental health among pregnant women.
References (23)

- Pregnant and Recently Pregnant People: At Increased Risk for Severe Illness from COVID-19. Centers for Disease Control and Prevention. Accessed May 11, 2021. https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/pregnant-people.html
- Joma M, Fovet CM, Seddiki N, et al. COVID-19 and pregnancy: vertical transmission and inflammation impact on newborns. Vaccines (Basel). 2021;9(4):391. PubMed CrossRef
- Breastfeeding and Caring for Newborns if You Have COVID-19. Centers for Disease Control and Prevention. Accessed November 9, 2020. https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/pregnancy-breastfeeding.html
- Shiina A, Niitsu T, Kobori O, et al. Relationship between perception and anxiety about COVID-19 infection and risk behaviors for spreading infection: a national survey in Japan. Brain Behav Immun Health. 2020;6:100101. PubMed CrossRef
- Salehi L, Rahimzadeh M, Molaei E, et al. The relationship among fear and anxiety of COVID-19, pregnancy experience, and mental health disorder in pregnant women: a structural equation model. Brain Behav. 2020;10(11):e01835. PubMed CrossRef
- Arora A, Jha AK, Alat P, et al. Understanding coronaphobia. Asian J Psychiatr. 2020;54:102384. PubMed CrossRef
- Chandra PS, Nanjundaswamy MH. Pregnancy specific anxiety: an under-recognized problem. World Psychiatry. 2020;19(3):336–337. PubMed CrossRef
- Moyer CA, Compton SD, Kaselitz E, et al. Pregnancy-related anxiety during COVID-19: a nationwide survey of 2740 pregnant women. Arch Women Ment Health. 2020;23(6):757–765. PubMed CrossRef
- Nanjundaswamy MH, Shiva L, Desai G, et al. COVID-19-related anxiety and concerns expressed by pregnant and postpartum women-a survey among obstetricians. Arch Women Ment Health. 2020;23(6):787–790. PubMed CrossRef
- Corbett GA, Milne SJ, Hehir MP, et al. Health anxiety and behavioral changes of pregnant women during the COVID-19 pandemic. Eur J Obstet Gynecol Reprod Biol. 2020;249:96–97. PubMed CrossRef
- Spitzer RL, Kroenke K, Williams JBW, et al. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092–1097. PubMed CrossRef
- Zhang J, Yu H, Gao Y, et al. Prevalence of anxiety and depression among pregnant women during the COVID-19 pandemic: a systematic review and meta-analysis. Researchsquare. Preprint posted October 6, 2020. Accessed May 11, 2021. https://www.researchsquare.com/article/rs-87129/v1
- Brunton RJ, Dryer R, Krägeloh C, et al. The Pregnancy-Related Anxiety Scale: a validity examination using Rasch analysis. J Affect Disord. 2018;236:127–135. PubMed CrossRef
- Somerville S, Dedman K, Hagan R, et al. The Perinatal Anxiety Screening Scale: development and preliminary validation. Arch Women Ment Health. 2014;17(5):443–454. PubMed CrossRef
- Lee SA. Coronavirus Anxiety Scale: a brief mental health screener for COVID-19 related anxiety. Death Stud. 2020;44(7):393–401. PubMed CrossRef
- Ganjekar S, Chandra PS. Addressing Mental Health Issues among Pregnant and Postpartum Women During COVID-19. Mental Health in the Times of COVID-19 Pandemic-Guidance for General Medical and Specialized Mental Health Care Settings. Bengaluru, India: NIMHANS; 2020:41–45.
- Adhikari EH, Moreno W, Zofkie AC, et al. Pregnancy outcomes among women with and without severe acute respiratory syndrome coronavirus 2 infection. JAMA Netw Open. 2020;3(11):e2029256. PubMed CrossRef
- Di Mascio D, Khalil A, Saccone G, et al. Outcome of coronavirus spectrum infections (SARS, MERS, COVID-19) during pregnancy: a systematic review and meta-analysis. Am J Obstet Gynecol MFM. 2020;2(2):100107. PubMed CrossRef
- Lackey KA, Pace RM, Williams JE, et al. SARS-CoV-2 and human milk: what is the evidence? Matern Child Nutr. 2020;16(4):e13032. PubMed CrossRef
- Dennis CL, Falah-Hassani K, Shiri R. Prevalence of antenatal and postnatal anxiety: systematic review and meta-analysis. Br J Psychiatry. 2017;210(5):315–323. PubMed CrossRef
- Nath A, Venkatesh S, Balan S, et al. The prevalence and determinants of pregnancy-related anxiety amongst pregnant women at less than 24 weeks of pregnancy in Bangalore, Southern India. Int J Womens Health. 2019;11:241–248. PubMed CrossRef
- Priya A, Chaturvedi S, Bhasin SK, et al. Depression, anxiety and stress among pregnant women: a community-based study. Indian J Psychiatry. 2018;60(1):151–152. PubMed CrossRef
- Supraja TA, Varghese M, Desai G, et al. The relationship of gender preference to anxiety, stress and family violence among pregnant women in urban India. Int J Cult Ment Health. 2016;9(4):356–363. CrossRef
Please sign in or purchase this PDF for $40.