ABSTRACT
Objective: To focus on the first feelings, attitudes, and planned reactions of psychiatric workers in Hungary to the news of the appearance of coronavirus disease 2019 (COVID-19) and to examine any differences between psychiatrists/psychologists and nurses/other professionals regarding these attitudes.
Methods: Hungarian psychiatric workers (N = 119) including psychiatrists/psychologists (n = 78) and nurses/other professionals (n = 41) participated in the study. To measure attitudes, a questionnaire was designed consisting of 7 questions and filled out within 1–3 days after the declaration of emergency in response to COVID-19 in Hungary on March 11, 2020.
Results: Psychiatric workers, especially psychiatrists/psychologists, regarded information gathering from valid sources as important. When examining the first feelings, we found that the psychiatrists/psychologists group tended to feel higher extent of anxiety, while the nurses/other professionals group showed higher extent of hope. When investigating willingness to work in the pandemic situation, a lower percentage of Hungarian psychiatric workers (58%) would choose to continue working compared to previous research. Answers to open-ended questions revealed that denial was the most frequent coping reaction.
Conclusions: These differences could be attributed to the finding that psychiatrists/psychologists, who had faced the reality of the virus situation via the news, tended to have more realistic attitudes toward the virus, while nurses/other professionals, who had avoided valid information, tended to have less realistic attitudes.
Prim Care Companion CNS Disord 2021;23(3):20m02850
To cite: Csigó K, Ritzl A. First reactions and attitudes of psychiatric workers in Budapest psychiatric care units regarding the COVID-19 pandemic. Prim Care Companion CNS Disord. 2021;23(3):20m02850.
To share: https://doi.org/10.4088/PCC.20m02850
© Copyright 2021 Physicians Postgraduate Press, Inc.
aNational Institute of Mental Health, Neurology and Neurosurgery, Budapest, Hungary
*Corresponding author: Katalin Csigó, PhD, National Institute of Mental Health, Neurology and Neurosurgery, 1135 Budapest Lehel u, 57-59, Budapest, Hungary ([email protected]).
The coronavirus disease 2019 (COVID-19) epidemic has had an extraordinary impact on mental health. In addition to the direct effect of the virus, we must take into account increasing disease anxiety due to the risk of infection, insecurity, confusing media activity, social isolation due to quarantine, socioeconomic impact, and reduced capacity of the health care system.
The presence of the COVID-19 virus was confirmed in Hungary for the first time on March 4, 2020. On March 11, 2020, the Hungarian government declared a state of emergency, which also fundamentally changed health care operations. In Hungary, 576 health care workers were infected with COVID-19 by June 1, 2020, which was 14.8% of all cases at that time.1
Previous studies have explored the knowledge and attitudes of medical staff toward infectious diseases and their willingness to work during an epidemic. Bai et al2 investigated stress reactions among medical staff members in Taiwan during the severe acute respiratory syndrome (SARS) outbreak and found that 5% of medical staff suffered from an acute stress disorder, 20% felt stigmatized and rejected in their neighborhood because of their hospital work, and 9% reported reluctance to work or considered resignation. Health professionals who worked in SARS units and hospitals during the SARS outbreak reported depression, anxiety, fear, and frustration as well as posttraumatic stress disorder symptoms.3
In contrast, in another study4 there were no significant differences in stress levels between health care workers and the control group. Each group showed increased stress levels, but health care workers’ adaptive responses to stress and the positive effects of infection control training may have been protective factors.4 Ma et al5 reported on the knowledge and attitudes of critical care clinicians during the 2009 H1N1 influenza pandemic. They found that 82.3% of medical staff expressed a willingness to care for H1N1 patients.5
Health professionals, especially those working in hospitals caring for people with confirmed or suspected COVID-19 infection, are vulnerable to both high risk of infection and mental health problems.3 They may also experience fear of contagion and spreading the virus to their families, friends, or colleagues.
Tan et al6 examined the psychological distress, depression, anxiety, and stress experienced by health care workers in Singapore in the midst of the COVID-19 outbreak and comparisons were made between medically (physicians, nurses) and non–medically (allied health professionals, pharmacists, technicians, administrators, clerical staff, and maintenance workers) trained hospital personnel. They6 found depression, stress, anxiety, and posttraumatic stress disorder among all health care workers. The prevalence of anxiety was higher among nonmedical health care workers compared with medical staff.6
It is important to examine what increases anxiety and fear among health care workers. Shanafelt et al7 interviewed groups of physicians and nurses in 8 listening sessions and found the following 8 sources of anxiety: (1) lack of access to appropriate personal protective equipment, (2) being exposed to COVID-19 at work and taking the infection home to their family, (3) not having rapid access to testing if they develop COVID-19 symptoms and concomitant fear of propagating infection at work, (4) uncertainty that their organization will support/take care of their personal and family needs if they develop infection, (5) access to childcare during increased work hours and school closures, (6) support for other personal and family needs as work hours and demands increase (food, hydration, lodging, transportation), (7) being able to provide competent medical care if deployed to a new area (eg, non–intensive care unit nurses having to function in this capacity), and (8) lack of access to up-to-date information and communication.
Today, we also have data on the attitudes, knowledge, and perception of health care workers regarding COVID-19 from Egypt,8 Pakistan,9 Ethiopia,10 and Nepal.11 The knowledge and attitudes of medical staff regarding COVID-19 are important in achieving effective coping strategies during the extraordinary pandemic situation. However, so far only 1 study12 has focused on psychiatric medical staff during an epidemic outbreak.
Shia and colleagues12 examined the knowledge and attitudes of psychiatric hospital staff toward infectious diseases and their willingness to work during the COVID-19 outbreak. The authors12 found that during the COVID-19 epidemic, 89.51% of the medical staff in psychiatric hospitals studied had extensive knowledge of COVID-19, 64.63% received the relevant training in hospitals, and 77.17% expressed a willingness to care for psychiatric patients with COVID-19. The most common reasons for being unwilling to care for these patients included concerns about catching the virus and infecting family members. There was no difference between psychiatrists and nurses in willingness to care for psychiatric patients with COVID-19.12
The psychological response of health care workers to the epidemic of infectious diseases is complex. Sources of anxiety may include vulnerability or loss of control, as well as concerns about one’s own health, the spread of the virus, the health of family and others, job changes, and isolation. We know that the risk of infection is much higher in the psychiatric care system (inpatient care and psychiatric care facilities) than in the general hospital wards.13
In this study, we aim to examine the first reactions and attitudes of psychiatric workers to the news of the appearance of COVID-19. In contrast to previous research, the timing of data collection in our study occurred immediately after the declaration of the state of emergency, and we examined differences in attitudes between physicians and nurses in many areas, not just in terms of willingness to work. An understanding of the psychological impact of the COVID-19 outbreak among health care workers is crucial in guiding policies and interventions to maintain their psychological well-being.
METHODS
Survey Questionnaire and Protocol
We designed a questionnaire consisting of 7 questions related to COVID-19 to assess the attitudes of the medical staff working in psychiatric hospitals in Budapest. Questionnaires were sent electronically to several psychiatric departments, and the questionnaire was completed anonymously. The questionnaire was filled out within 1–3 days after the declaration of the emergency situation in Hungary (March 11, 2020).
The questionnaire included 2 open-ended questions and 3 optional questions to be scored. In the case of 7 predetermined feelings, the strength of the given feeling had to be scored on a 5-point Likert scale (1 not characteristic at all and 5 completely characteristic). The data were collected anonymously, and implied consent was used based on the freedom to respond or not.
The questionnaire included the following questions:
- How did you first hear about the coronavirus epidemic?
- News
- Social media
- Colleagues/workplace
- What was your first thought, feeling, reaction to the news?
- What thoughts, feelings, reactions, actions followed this? What did you do after some days?
- Which statement is closest to your opinion?
- “Coronavirus is just another influenza virus.”
- “Coronavirus needs to be taken seriously.”
- “Reactions to coronavirus (quarantine, travel restrictions) are exaggerated.”
- “It is worth waiting for more information before reacting.”
- “Hungary should introduce more serious protective interventions.”
- Which state or feeling characterizes your first reactions to the news of a viral infection best? Mark the strength of the feeling from 1 to 5:
- Concern
- Anxiety
- Panic
- Hope
- Helplessness
- Carefulness
- Focusing on work
- Who did you worry about most when you heard about the virus infection?
- Family members
- Patients in the hospital
- Colleagues
- What will you do if the virus infection gets worse in Hungary?
- “I will continue working in the hospital.”
- “I will be with my family.”
- “I will stay at home and try to gather information.”
Participants
The questionnaire was completed by 119 individuals. They all were psychiatrists, psychologists, nurses, and other professionals (eg, social workers, art therapists) working in psychiatric inpatient units in Budapest. In the data analysis, psychiatrists and psychologists were included in 1 group, and nurses and other professionals were included in another.
Statistical Analysis
All analyses were conducted in the SPSS 16.0 for Windows statistical program. Before investigating the differences in attitudes toward COVID-19 between the psychiatrists/psychologists and nurses/other professionals, normal distribution was investigated by Kolmogorov-Smirnov tests. Given the non-normal distribution of the scale variables, nonparametric tests were applied.
To assess the associations of categorical variables, χ2 tests were used to assess associations of categorical variables, and Mann-Whitney U tests were applied to compare group mean scores of scale variables. Psychiatric worker groups served as independent variables, while the source of the first information, different types of attitudes, the strength of given feelings (concern, anxiety, panic, hope, helplessness, carefulness, focusing on work, and caring about patients), the subject of concern, and planned reactions in case of deterioration of the pandemic situation served as dependent variables.
RESULTS
Descriptive Statistics
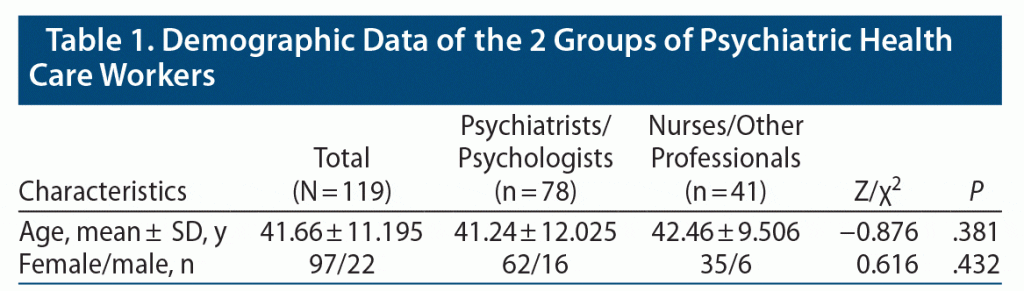
The demographic data of our sample are presented in Table 1. The distribution of age proved to be non-normal (Kolmogorov-Smirnov test, P = .016). The nonparametric Mann-Whitney U test showed no significant differences between groups regarding age (Z = −0.876, P = .381). The χ2 test indicated no significant differences between groups regarding the distribution of sex ratio (χ21 = 0.616, P = .432). In both groups, more female than male subjects participated.
Investigating Differences Between Psychiatrists/Psychologists and Nurses/Other Professionals Groups
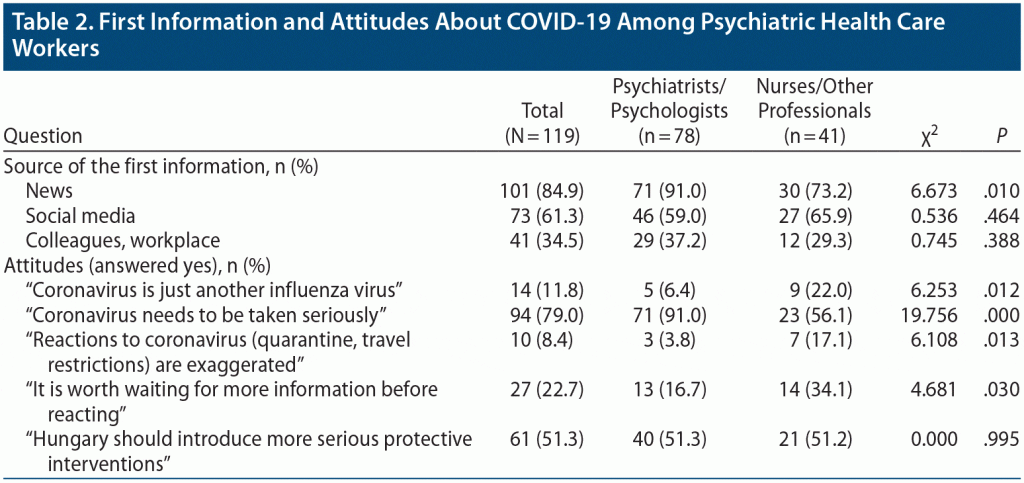
First, we investigated the source of the first information about and different types of attitudes regarding COVID-19 (Table 2).
With regard to the total sample, participants gathered information mainly from the news (84.9%), social media (61.3%), and colleagues (34.5%). When examining differences between the 2 groups, we found that psychiatrists/psychologists used the news significantly more frequently as a source of information about the pandemic than did nurses/other professionals (χ21 = 6.673, P = .010), while we found no differences regarding the usage of social media (χ21 = 0.536, P = .464) and workplace information (χ21 = 0.745, P = .388).
With regard to attitudes about COVID-19, most participants (79.0%) agreed with the statement “the coronavirus needs to be taken seriously,” and most (91.6%) disagreed that the governmental reactions to coronavirus (quarantine, travel restrictions) would be exaggerated. But, compared to nurses/other professionals, psychiatrists/psychologists tended to respond more frequently that COVID-19 is not just another influenza virus (χ21 = 6.253, P = .012), needs to be taken seriously (χ21 = 19.756, P = .000), and is not worth waiting for more information before reacting (χ21 = 4.681, P = .030), and they were more frequently satisfied with governmental restrictions (χ21 = 6.108, P = .013). In both groups, a similar proportion of participants agreed that Hungary should introduce more serious protective interventions (χ21 = 0.000, P = .995).
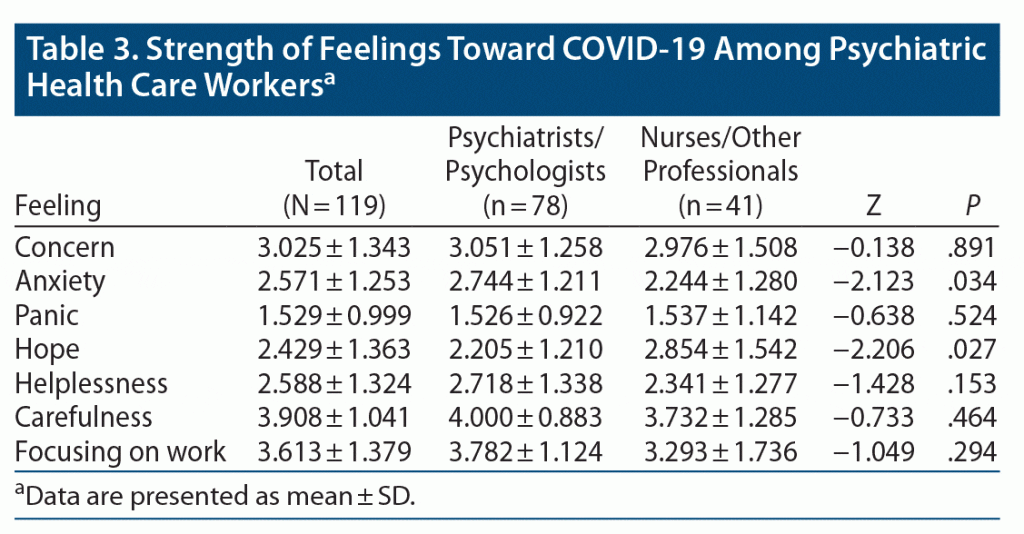
We also assessed the strength of certain feelings (concern, anxiety, panic, hope, helplessness, carefulness, focusing on work, and caring about patients) toward COVID-19 by using a 5-point Likert scale for each feeling (Table 3). The overall sample was characterized by higher points on the carefulness (3.908 ± 1.041) and focusing on work (3.613 ± 1.379) scales, but lower points on the panic scale (1.529 ± 0.999). A significant difference was found between groups regarding the anxiety (Z = −2.123, P = .034) and hope (Z = −2.206, P = .027) scales. The psychiatrists/psychologists group showed higher extent of anxiety, while the nurses/other professionals group had higher extent of hope.
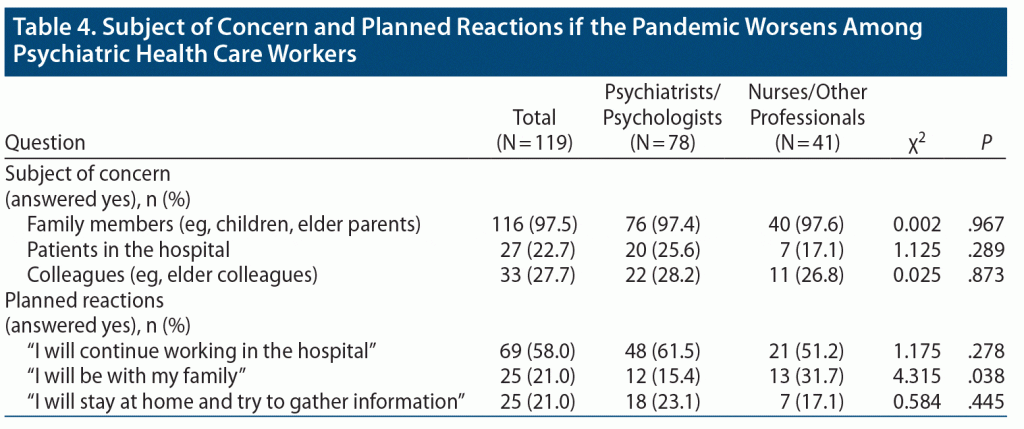
Lastly, we focused on measuring the subject of concern and planned reactions in case of deterioration of the pandemic situation (Table 4). Most participants were concerned about their family members (97.5%), and there was no significant difference between groups with respect to the subject of concern. Both groups indicated that they worried most frequently about their family members (χ21 = 0.002, P = .967) and less frequently about patients in the hospital (χ21 = 1.125, P = .289) and elderly colleagues (χ21 = 0.025, P = .873). In contrast with these findings, when planned reactions were analyzed we found that most workers (58%) would choose to continue working if the pandemic situation became more serious. The responses of the 2 groups showed no significant differences. Both groups responded more frequently that they would continue working (χ21 = 1.175, P = .278) rather than be with their families (χ21 = 5.377, P = .068) or stay at home and try to gather more information (χ21 = 0.584, P = .445). But, compared to psychiatrists/psychologists, nurses/other professionals stated more frequently that they would choose to be with their families (χ21 = 4.315, P = .038).
Qualitative Analysis of Open Questions
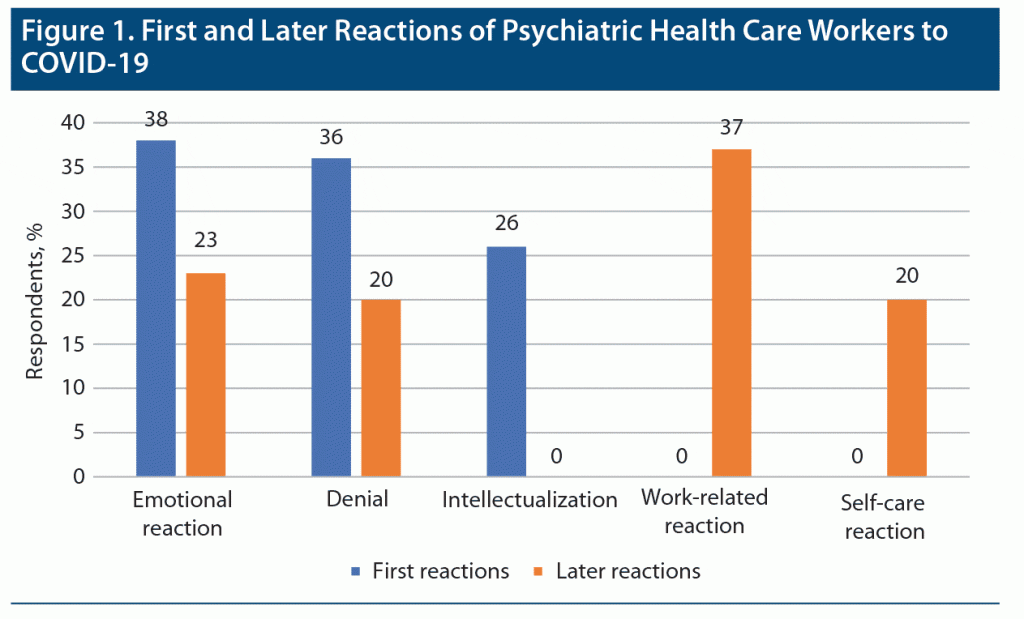
The first of the open questions (What was your first thought, feeling, reaction to the news?) was answered by 100 of 119 people. On the basis of the content analysis of the answers, they were divided into 3 categories (Figure 1).
It was considered an emotional reaction if a respondent wrote in the free statements about, for example, different emotions such as feelings of fright, anxiety, fear, agitation, anger, or panic. Of the respondents, 38% had an emotional response.
Reactions of denial included, for example, “It’s just fake news,” “It’s just panic,” “China is far away,” “The virus won’t reach here,” and “This is not our problem.” Of the respondents, 36% gave a denial reaction.
The category of intellectualization included professional reactions, for example, how to reorganize health care, description of reactions related to the knowledge, and news about the virus (eg, this virus differs from the influenza virus, what the rate of spread of the epidemic is, what we know about the virus, how pathogenic it is). Of respondents, 26% had an intellectualizing reaction among the first reactions.
With regard to later reactions (What thoughts, feelings, reactions, actions followed this? What did you do after some days?), 100 of 119 respondents replied to the questionnaire. Their responses were divided into 4 groups (see Figure 1).
The most common reaction was the work-related reaction, which included answers related to work and task performance at work (eg, how we organize patient care, what patients need to be informed about, how we can switch to work online). We also included reactions related to following the news and gathering valid professional information. Coping responses were provided by 37% of respondents.
The second most common reaction, 23%, was the appearance of emotional reactions, which refers to expressing negative feelings: respondents report feeling anxious and increasing fear.
Self-care reactions included naming self-care steps for family members and themselves (eg, buying nonperishable food, getting vitamins, expressing care for family members). Of the respondents, 20% gave reactions that can be classified as self-care.
The reaction of denial was also present in the later reactions. Of the respondents, 20% answered, for example, “I still don’t deal with the news,” “I continued skiing,” “I do nothing differently than before,” and “I still think the whole virus news is fake news and hysteria.”
DISCUSSION
In this study, our objective was to investigate the first feelings, attitudes, and planned reactions of psychiatric workers toward COVID-19 in Hungary. Is there a symptomatic level of anxiety, panic, or fear in this group? How do they cope with this crisis? Furthermore, we intended to support the hypothesis that there might be differences between the 2 examined groups of psychiatrists/psychologists and nurses/other professionals regarding their attitudes and reactions.
According to our results, we can state that psychiatric workers regard information gathering from valid sources (eg, the news) important. However, the psychiatrists/psychologists group relies on the news more frequently; therefore, in the case of nurses, it is particularly important to provide adequate information.
On the basis of the questionnaire data, it appears that the psychiatric workers paid adequate attention to the news of the virus and related tasks and that they were able to actively cope instead of being overwhelmed by panic.
We consider it interesting that we measured higher levels of anxiety in the psychiatrists/psychologists group. It is possible that this higher anxiety level is related to their more realistic attitudes (eg, COVID-19 is not just another influenza virus) toward the virus and is associated with their increased interest in reading the news. Facing the reality of the virus situation may overburden coping abilities, resulting in higher levels of anxiety.
Nurses/other professionals tended to feel more hopeful. Possibly, those who tend to avoid valid information about the virus can preserve positive feelings. Further examination could reveal whether more positive feelings (eg, hope) are related to using stronger defense mechanisms (eg, denial, banalization).
When investigating willingness to work, we found that 58% of psychiatric workers would choose to continue working if the pandemic situation became more serious, which seemed to be lower than the findings of a study12 (77.17%) among Chinese medical workers. These differences may be interpreted as higher concern toward family members (97.5%) among Hungarian workers. But, it might also be the case that people from collective cultures (eg, China) are more able to suppress their personal concerns on behalf of society. If more data from individual cultures are available, more adequate comparisons will be made.
The answers to the open-ended questions further nuance the picture: that we basically react with emotions to a crisis situation such as the COVID-19 epidemic. Emotional reactions can subside over time and coping reactions take place. A coping reaction might be self-focused (eg, self-care reactions) or professional/work focused (eg, work-related reactions). It is important to note that denial was present in a large number of responses.
Denial and banalization—as a self-protective mechanism—could help to alleviate anxiety in the short term, as they provide preparation time to cope with the events. In the long run, however, denial can be at the expense of caution at work and the mobilization of effective coping strategies. Our research provides insight into the emotional reactions and coping capacity of psychiatric workers and draws attention to the importance of examining these issues.
Finally, this study had several limitations. First, this study was conducted only in some psychiatric hospitals in Budapest with a limited number of participants. Second, the results are based on a self-reported questionnaire, which might not represent actual practice. And, finally, the questionnaire was filled in within 1–3 days after the declaration of the emergency situation in Hungary, so attitudes might have significantly changed since then. Therefore, more research is needed to confirm the findings of this study. A follow-up study of the participants now that a year has passed would be of great interest. Several research groups in Hungary are also examining the level of stress experienced by health care workers in the past year and possible psychiatric symptoms and the impact on working performance. The strength of our research is that it was a study of early, first reactions to the COVID-19 crisis.
Submitted: November 21, 2020; accepted February 18, 2021.
Published online: April 29, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Clinical Points
- An unexpected crisis situation such as a pandemic increases anxiety among health care workers.
- Psychiatrists/psychologists and nurses responded to the news of COVID-19 with different attitudes and coping mechanisms.
- A special self-protective mechanism—denial—could help to alleviate anxiety in the short term, but in the long run, it is necessary to help health care workers develop more mature coping forms.
References (13)

- Portfolio. How many health workers have been diagnosed with coronavirus in Hungary. Accessed March 30, 2021. https://www.portfolio.hu/gazdasag/20200531/kiderult-hany-egeszsegugyi-dolgozo-lett-koronavirusos-magyarorszagon-434812
- Bai Y, Lin CC, Lin CY, et al. Survey of stress reactions among health care workers involved with the SARS outbreak. Psychiatr Serv. 2004;55(9):1055–1057. PubMed CrossRef
- Xiang YT, Yang Y, Li W, et al. Timely mental health care for the 2019 novel coronavirus outbreak is urgently needed. Lancet Psychiatry. 2020;7(3):228–229. PubMed
- Chua SE, Cheung V, Cheung C, et al. Psychological effects of the SARS outbreak in Hong Kong on high-risk health care workers. Can J Psychiatry. 2004;49(6):391–393. PubMed CrossRef
- Ma X, He Z, Wang Y, et al; China Critical Care Clinical Trial Group (CCCCTG). Knowledge and attitudes of healthcare workers in Chinese intensive care units regarding 2009 H1N1 influenza pandemic. BMC Infect Dis. 2011;11(1):24. PubMed CrossRef
- Tan BYQ, Chew NWS, Lee GKH, et al. Psychological impact of the COVID-19 pandemic on health care workers in Singapore. Ann Intern Med. 2020;173(4):317–320. PubMed
- Shanafelt T, Ripp J, Trockel M. Understanding and addressing sources of anxiety among health care professionals during the COVID-19 pandemic. JAMA. 2020;323(21):2133–2134. PubMed CrossRef
- Abdel Wahed WY, Hefzy EM, Ahmed MI, et al. Assessment of knowledge, attitudes, and perception of health care workers regarding COVID-19: a cross-sectional study from Egypt. J Community Health. 2020;45(6):1242–1251. PubMed
- Saqlain M, Munir MM, Rehman SU, et al. Knowledge, attitude, practice and perceived barriers among healthcare workers regarding COVID-19: a cross-sectional survey from Pakistan. J Hosp Infect. 2020;105(3):419–423. PubMed CrossRef
- Asemahagn MA. Factors determining the knowledge and prevention practice of healthcare workers towards COVID-19 in Amhara region, Ethiopia: a cross-sectional survey. Trop Med Health. 2020;48(1):72. PubMed CrossRef
- Limbu DK, Piryani RM, Sunny AK. Healthcare workers’ knowledge, attitude and practices during the COVID-19 pandemic response in a tertiary care hospital of Nepal. PLoS One. 2020;15(11):e0242126. PubMed CrossRef
- Shi Y, Wang J, Yang Y, et al. Knowledge and attitudes of medical staff in Chinese psychiatric hospitals regarding COVID-19. Brain Behav Immun Health. 2020;4:100064. PubMed CrossRef
- Xiang YT, Zhao YJ, Liu ZH, et al. The COVID-19 outbreak and psychiatric hospitals in China: managing challenges through mental health service reform. Int J Biol Sci. 2020;16(10):1741–1744. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!