ABSTRACT
Objective: To compare the health anxiety and healthy lifestyle behavior experienced by psychiatric patients due to the coronavirus disease 2019 (COVID-19) pandemic with that of a control group.
Methods: The study included 120 outpatients (aged 18–65 years) diagnosed with a psychiatric illness (DSM-5 criteria) who presented to a psychiatry outpatient clinic between June and August 2020. The control group included 120 healthy individuals with a similar age and sex distribution as the patient group. Data were collected with a questionnaire developed by the authors to determine the participants’ adherence to COVID-19 hygiene rules and associated behavioral norms. The Health Anxiety Scale–Short Form, Health Perception Scale, and Health-Promoting Lifestyle Profile were completed by all participants.
Results: The mean Health Anxiety Scale score was significantly lower in the patient group compared to the control group (P < .01). Health anxiety was high in 8% of the patients and 32% of the controls. Also, the mean Health-Promoting Lifestyle Profile score was statistically significantly lower in the patient group compared to the control group (P < .01). There was no significant difference between the groups based on health perception scores and adherence to hygiene rules.
Conclusions: As expected, the healthy lifestyle behavior of individuals without psychiatric illness was higher compared to those with mental disorders. However, health anxiety about COVID-19 was higher among healthy individuals compared to those with a psychiatric disorder. Thus, it could be suggested that individuals without a psychiatric illness prior to the pandemic could need psychiatric assistance after the pandemic.
Prim Care Companion CNS Disord 2022;24(2):21m03197
To cite: Korkmaz S, Atescelik M, Balcı HN, et al. Health anxiety, health perception, and healthy lifestyle behavior among psychiatric patients during the COVID-19 pandemic. Prim Care Companion CNS Disord. 2022;24(2):21m03197.
To share: https://doi.org/10.4088/PCC.21m03197
© Copyright 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Faculty of Medicine, Fırat University, Elazıg, Turkey
bDepartment of Emergency Medicine, Faculty of Medicine, Fırat University, Elazıg, Turkey
cNamık Kemal İlköğretim Okulu, Elazıg, Turkey
dDepartment of Cardiology, Faculty of Medicine, Fırat University, Elazıg, Turkey
*Corresponding author: Sevda Korkmaz, MD, Department of Psychiatry, Faculty of Medicine, Fırat University, 23119, Elazıg, Turkey ([email protected]).
The coronavirus disease 2019 (COVID-19) pandemic has had global effects on all nations, leading to physical and psychological problems in individuals. Both the neuropsychiatric presentations due to the infection and the negative effects of the pandemic on general mental health have led to serious social anxiety.1 Feeling a loss of control, uncertainties associated with the disease, and concerns related to personal health or that of relatives could exponentially increase fear and anxiety.2 It was reported that when fear of the pandemic reaches unattainable levels, outcomes that could threaten psychological health are observed.3 It is known that epidemics could lead to trauma in individuals, increasing stress and anxiety levels.4 However, in pandemics, certain groups are further affected by the negative consequences of the disease. Several recent studies5–7 discussed the possible adverse effects of the COVID-19 pandemic on psychiatric patients, a significantly vulnerable population. Based on our clinical observations, the pandemic has led to negative presentations such as the exacerbation of primary disease and disease symptoms, increased disease symptoms, and discontinuation of treatment in patients with a chronic mental illness. However, studies on the experiences of individuals with chronic mental illness during the pandemic, the impact of the pandemic on these individuals, and their psychological concerns are limited in the literature. A review of the literature revealed no study wherein individuals with psychological illnesses were compared with healthy individuals based on perceptions about COVID-19 infection risk, necrophobia, or the fear of losing relatives. Thus, the present study aimed to assess the intensity of negative emotions such as fear and anxiety and healthy lifestyle behavior experienced by healthy individuals and those with chronic mental illness during the COVID-19 pandemic.
METHODS
The present study was conducted within 3 months of ethics committee approval. The study included 120 outpatients (aged 18–65 years) who presented to Fırat University, Faculty of Medicine, Psychiatry Outpatient Clinic between June and August 2020, were diagnosed with a psychiatric illness based on DSM-5 criteria, met the inclusion criteria, and agreed to participate in the study. For the patients, a physical or mental illness that may prevent them from responding to the questionnaires and scales was accepted as the exclusion criterion. The control group included 120 healthy individuals with a similar age and sex distribution as the patient group. A semistructured sociodemographic data form developed by the authors was completed by all participants. Also, a questionnaire developed by the authors to determine whether the participants adhered to COVID-19 hygiene rules was administered. The Health Anxiety Scale–Short Form,8 Health Perception Scale,9 and Health-Promoting Lifestyle Profile10 were administered to both the patient and control groups.
Scales
Health Anxiety Scale–Short Form. The scale, developed by Salkovskis et al,8 includes 64 items. The short form of the scale includes 18 items. The main 14 items are 4-point Likert-type questions about the emotions and perceptions associated with the individual’s health. The 4 remaining 4-point Likert-type items ask the individual to elaborate about the case when they perceive that they could be seriously ill. Each item is scored between 0 and 3 points. The highest possible scale score is 54. A high scale score indicates high health anxiety. A score ≥ 18 is considered high health anxiety.
Health Perception Scale. The scale developed by Diamond et al9 is a 5-point Likert-type scale that includes 15 items and 4 factors. The scale includes both positive and negative items, and negative items are reverse scored. The lowest possible score is 15, and the highest possible score is 75. A high score indicates a positive perception about health. The scale includes 4 subdimensions: the control center (self-confidence in maintaining good health), self-awareness (belief in self-control on health), certainty (knowledge on the necessary precautions to maintain and improve health), and the significance of health. In the present study, only the total scale score was included in the analysis.
Health-Promoting Lifestyle Profile. Healthy behavior data were collected with this scale developed and revised by Walker et al.10 The 4-point Likert-type scale includes 52 items and 6 subdimensions that measure healthy lifestyle behavior. Subdimensions include spiritual development, health responsibility, physical activity, nutrition, interpersonal relations, and stress management. The total score reflects healthy lifestyle behavior. The minimum score is 52, and the maximum score is 208.
Cleanliness, social distancing, and hygiene rules. This questionnaire was developed by the authors and includes 8 questions to determine adherence to cleanliness and hygiene rules. Each question has 3 possible responses: never (1 point), sometimes (2 points), and always (3 points). The total personal score is the sum of the scores for the 8 questions.
Statistical Analysis
SPSS version 22 software was used in the statistical analyses. The study data are presented as mean ± SD, the intergroup comparison data with normal distribution were analyzed with the student t test, and the data that did not exhibit normal distribution were analyzed with the Mann-Whitney U test. A P value < .05 was considered statistically significant. Participant demographics are presented with descriptive analysis, frequencies, percentages, and mean ± SD. The continuous variable data are presented as mean ± SD, and categorical variable data are presented as n (%).
RESULTS
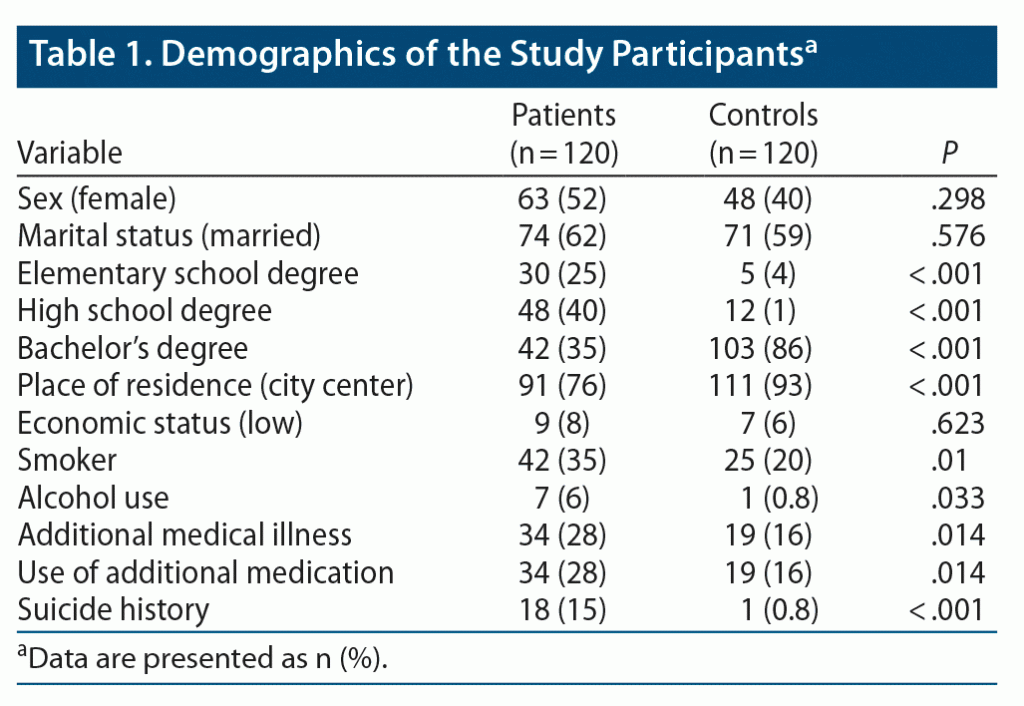
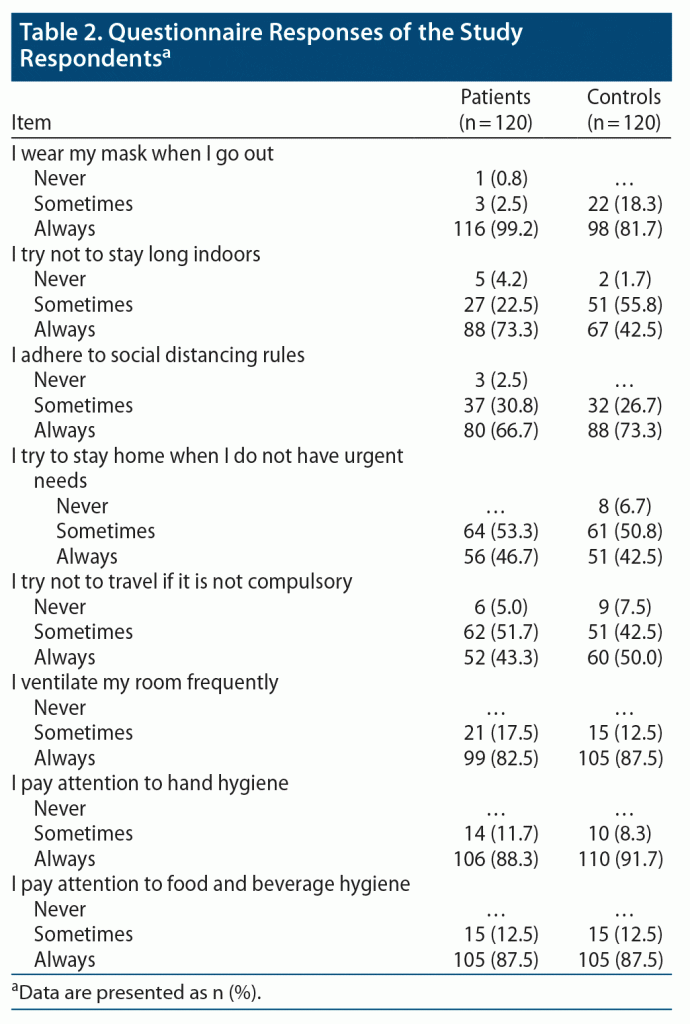
The patient group included 63 female and 57 male participants, and the control group included 48 women and 72 men. The mean ± SD patient age was 37.8 ± 12.8 years, and the mean control group age was 39.03 ± 12.5 years. Patient and control group demographics are presented in Table 1. Responses of patients and healthy controls to questions on hygiene rules are presented in Table 2.
In the patient group, 66 patients had anxiety disorder, 26 had depressive disorder, 23 had adaptation disorder, and 5 were diagnosed with obsessive-compulsive disorder. Alcohol use increased in 1 patient and 2 controls during the pandemic. Smoking increased in 6 patients and 6 controls during the pandemic. High health anxiety was identified in 10 patients (6%) and 38 individuals in the control group (32%) (≥ 18 points). Forty patients and 10 healthy controls had a history of psychiatric disease in the family.
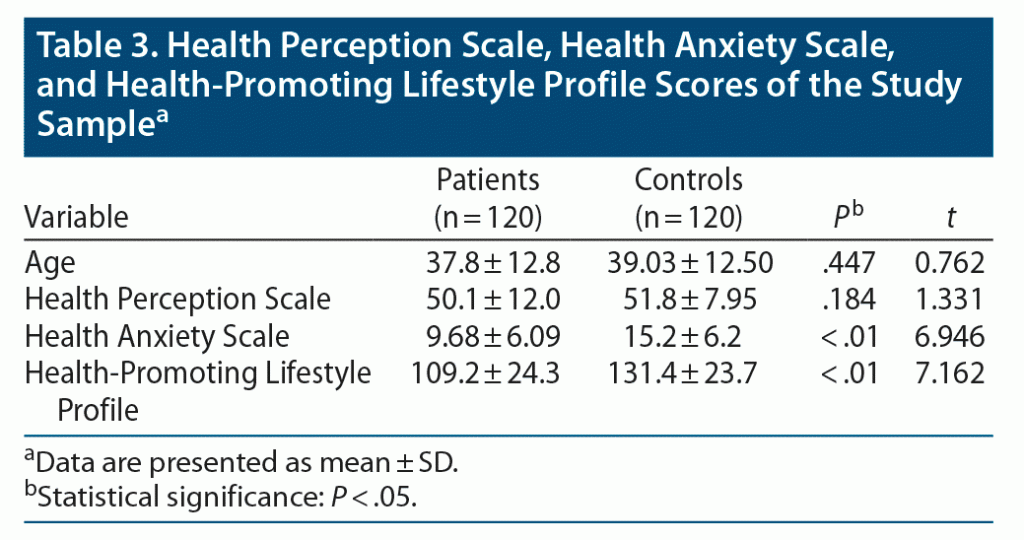
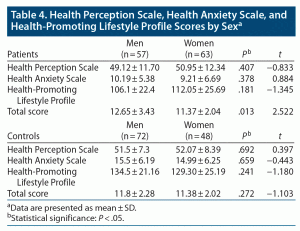
The comparison of the patient and control group scale scores demonstrated that the mean ± SD patient Health Anxiety Scale score (9.68 ± 6.09) was significantly lower compared to the mean control group score (15.2 ± 6.2) (P < .01) (Table 3). Furthermore, the mean ± SD patient Health-Promoting Lifestyle Profile score (109.2 ± 24.3) was statistically significantly lower compared to the control group score (131.4 ± 23.7) (P < .01) (Table 3). There was no significant difference between the Health Perception Scale scores of the groups. Also, there was no statistically significant difference between the scale scores of female and male participants in the patient and control groups (Table 4).
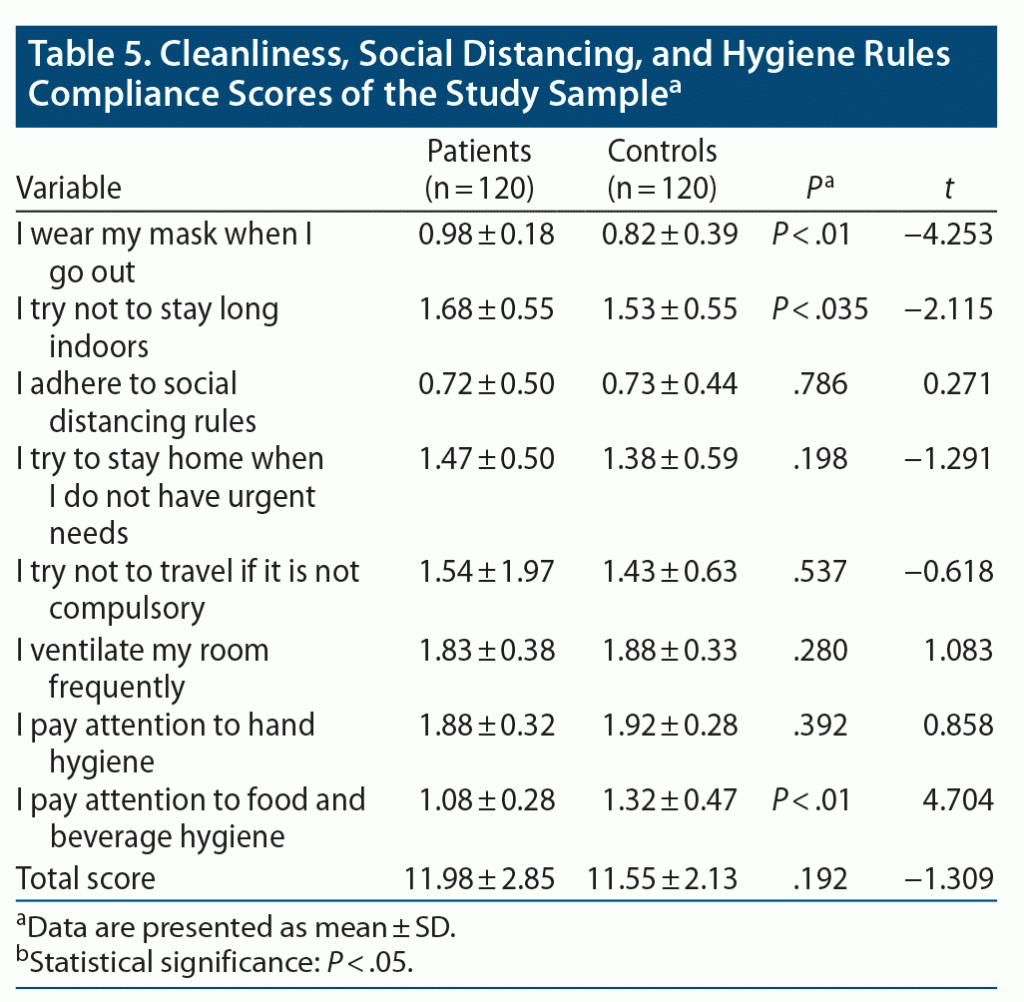
There was no statistically significant difference between the total cleanliness, social distancing, and hygiene scores of the groups. The highest adherence scores in the patient and control groups were for hand hygiene, ventilation of the room, and avoidance of indoor spaces. The COVID-related rule least adhered to in both groups was social distancing. The mask-wearing scores for the patient group were higher compared to the control group, while food and beverage hygiene scores were higher in the control group (Table 5). Based on the cleanliness, social distancing, and hygiene questionnaire scores, there was no difference in the control group based on sex, while the scores of women in the patient group were higher and they adhered to the rules more than the men (P = .013).
DISCUSSION
In this study, it was determined that the health anxiety experienced due to the COVID-19 pandemic was higher in healthy individuals compared to those with psychiatric disorders. Furthermore, it was determined that 8% of the patients and 32% of the individuals in the control group had high health anxiety when the Health Anxiety Scale cutoff score was 18. However, Health-Promoting Lifestyle Profile scores were lower in psychiatric patients compared to healthy individuals as expected.
Disease anxiety disorder (previously hypochondriasis) is characterized by anxiety about the presence of a serious disease or the concern that certain minor existing symptoms indicated a serious disease in the DSM-5.11 Although there is no organic pathology, the individual experiences significant health anxiety due to the misinterpretation of physical sensations. Thus, the individual experiences intense anxiety due to the perceived stimuli and frequently requires medical assistance.12 Health anxiety symptoms exacerbate due to the ideation that they constitute a threat to the individual’s health. Safety-seeking behaviors such as avoidance, control, information search, and assurance could lead to the deterioration of personal functions.
The individual’s personality, genetic traits, experiences, repetitive hospitalizations, or factors such as preexisting diseases and symptoms of these diseases could also affect health anxiety.13,14 Barsky and Klerman15 reported in 1983 that health anxiety is aggravated in cases wherein the individual is under stress, suffers a serious disease, experiences loss of a family member, or perceives that the lives of relatives are in danger.
It has been reported that health anxiety levels increased significantly in society in general due to the global impact of the COVID-19 pandemic.16–18 Epidemic diseases could have a traumatic impact on individuals and may lead to an increase in stress and anxiety levels even after the epidemic. In the present study, consistent with the literature, it was determined that 24% of all participants experienced health anxiety.
Emotions of fear, unhappiness, despair, and desperation experienced due to uncertainties and concerns about the disease during epidemics could lead to significant challenges for individuals.19 Thus, fear or anxiety experienced during crises such as a pandemic could be accepted to a certain degree. Furthermore, the emotions of fear and anxiety could also ensure the implementation of necessary survival precautions. However, when levels of fear and anxiety related to the epidemic are that which are expected, individual functions could be affected, medical assistance needs increase, and significant psychological problems may be observed.20 In the present study, it was determined that the Health Anxiety Scale scores of the healthy group were higher compared to individuals with psychiatric disorders, and 32% of this group experienced health anxiety.
Acceptable anxiety should lead to increased protective behavior in the individual. It is expected that those with high anxiety will take precautions to prevent infection and adhere to hygiene and social distancing recommendations. However, in the present study, there was a statistically significant difference between the total cleanliness, social distancing, and hygiene scores of the groups despite the higher health anxiety level in the control group. This finding is important, since it was demonstrated that the increase in the level of anxiety reduced its protective and motivating properties and could disrupt individual functions. It is known that certain individuals are more vulnerable to health anxiety during an epidemic.18 In a study conducted by Özdin et al19 in Turkey in 2020, it was reported that individuals with a psychological disorder or organic disease exhibited higher levels of stress during the COVID-19 pandemic compared to the general population. In contrast, the present study findings revealed that the health anxiety levels of the individuals with a psychiatric disorder were lower compared to that of healthy individuals. Individuals with psychiatric disease previously faced illnesses, hospital visits, and treatment protocols several times and experienced anxiety associated with a potential disorder. This experience could have facilitated their coping mechanisms with the pandemic, as they are more familiar with health anxiety, and thus reduced the distress induced by a new disease. Our findings are also important since it now could be predicted that individuals with no prior psychiatric disorders may need psychiatric assistance after the pandemic.
In this study, it was determined that mean healthy lifestyle behavior scores of the patients were lower compared to that of the control group. Healthy lifestyle behavior includes sufficient and regular exercise, balanced nutrition, nonsmoking, health responsibility, stress management, and hygiene measures.7 It is known that the physical health presentation is negative not only in those with schizophrenia but also in most individuals with chronic mental illness. In a study conducted by Byeon,20 it was reported that individuals with depression and anxiety smoked more and had higher nicotine dependence than those without depression and anxiety. In another study,21 it was reported that about half of the patients with depression, anxiety, and phobia were obese, and 61% lived a sedentary lifestyle. Furthermore, the same study21 found alcohol abuse in more than 80% of these patients. Thus, the employment of inadequate and negative coping mechanisms such as sedentary lifestyle, poor nutrition and sleep hygiene, smoking, and alcohol use is more common among psychiatric patients compared to healthy individuals. In the present study, healthy lifestyle behavior scores of patients with psychiatric illness were low, which is consistent with the literature.
CONCLUSION
The subacute and chronic effects of COVID-19, observed to cause certain psychiatric symptoms in the acute stage, are not yet known. Studies22,23 conducted after the severe acute respiratory syndrome epidemic demonstrated that the psychological impacts were not always observed in the short term and could lead to severe and permanent psychological problems. A similar outcome could be expected after the COVID-19 pandemic—the neuropsychological consequences of which could be serious. Thus, it is important to protect individuals’ psychological health, to take precautions, and to implement the required psychosocial measures during the acute stage.
In addition to individual factors such as exaggeration of the threat and susceptibility to anxiety, other factors that could exacerbate health anxiety such as the approach of the media to the pandemic have been reported.24–26 In a study18 conducted with 1,046 participants in Turkey, it was determined that the news reports about the pandemic and the time spent on social media could increase health anxiety. Thus, each social group has certain responsibilities to implement certain measures to protect not only the individual but also society.
The present study has certain limitations. Although the number of patients included in the study was adequate, the sample size was not large enough to interpret the health anxiety levels in various psychiatric diseases. Thus, studies conducted with larger sample sizes are required for illness classification.
Submitted: November 22, 2021; accepted February 8, 2022.
Published online: April 5, 2022.
Relevant financial relationships: None.
Funding/support: None.
Clinical Points
- The subacute and chronic effects of COVID-19 infection, observed to cause certain psychiatric symptoms in the acute stage, are not yet known.
- In pandemics, certain groups are more affected by the negative consequences of the disease compared to others.
- It could be predicted that individuals with no prior psychiatric disorder could need psychiatric assistance after the COVID-19 pandemic.
References (26)

- Vindegaard N, Benros ME. COVID-19 pandemic and mental health consequences: systematic review of the current evidence. Brain Behav Immun. 2020;89:531–542. PubMed CrossRef
- Wu P, Fang Y, Guan Z, et al. The psychological impact of the SARS epidemic on hospital employees in China: exposure, risk perception, and altruistic acceptance of risk. Can J Psychiatry. 2009;54(5):302–311. PubMed CrossRef
- Kobayashi T, Jung SM, Linton NM, et al. Communicating the risk of death from novel coronavirus disease (COVID-19). J Clin Med. 2020;9(2):580. PubMed CrossRef
- Joos A. Psychosomatic medicine and COVID-19 pandemic. Psychother Psychosom. 2020;89(4):263–264. PubMed CrossRef
- Muruganandam P, Neelamegam S, Menon V, et al. COVID-19 and severe mental illness: impact on patients and its relation with their awareness about COVID-19. Psychiatry Res. 2020;291:113265. PubMed CrossRef
- Li S, Zhang Y. Mental healthcare for psychiatric inpatients during the COVID-19 epidemic. Gen Psychiatr. 2020;33(2):e100216. PubMed CrossRef
- Hao F, Tan W, Jiang L, et al. Do psychiatric patients experience more psychiatric symptoms during COVID-19 pandemic and lockdown? a case-control study with service and research implications for immunopsychiatry. Brain Behav Immun. 2020;87:100–106. PubMed CrossRef
- Salkovskis PM, Rimes KA, Warwick HM, et al. The Health Anxiety Inventory: development and validation of scales for the measurement of health anxiety and hypochondriasis. Psychol Med. 2002;32(5):843–853. PubMed CrossRef
- Diamond JJ, Becker JA, Arenson CA, et al. Development of a scale to measure adults’ perceptions of health: preliminary findings. J Community Psychol. 2007;35(5):557–561. CrossRef
- Walker SN, Sechrist KR, Pender NJ. The Health-Promoting Lifestyle Profile: development and psychometric characteristics. Nurs Res. 1987;36(2):76–81. PubMed CrossRef
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders DSM-5. Fifth Edition. Köroğlu E (trans.). Ankara: Hekimler Yayın Birliği; 2014.
- Abramowitz JS, Olatunji BO, Deacon BJ. Health anxiety, hypochondriasis, and the anxiety disorders. Behav Ther. 2007;38(1):86–94. PubMed CrossRef
- Rask CU, Munkholm A, Clemmensen L, et al. Health anxiety in preadolescence–associated health problems, healthcare expenditure, and continuity in childhood. J Abnorm Child Psychol. 2016;44(4):823–832.
- Starcevic V, Noyes R. Hypochondriasis and Health Anxiety: A Guide for Clinicians. New York: Oxford University Press; 2014.
- Barsky AJ, Klerman GL. Overview: hypochondriasis, bodily complaints, and somatic styles. Am J Psychiatry. 1983;140(3):273–283. PubMed CrossRef
- Kulu M, Özsoy F. Anxiety and health anxiety levels in non-healthcare community sampling. Kocaeli Med J. 2021;10(50):112–117. CrossRef
- Canlı D, Karaşar B. Health anxiety and emotion regulation during the period of COVID-19 outbreak in Turkey. Psychiatr Danub. 2020;32(3-4):513–520. PubMed CrossRef
- Kazan Kızılkurt O, Yılmaz A, Noyan CO, et al. Health anxiety during the early phases of COVID-19 pandemic in Turkey and its relationship with postpandemic attitudes, hopelessness, and psychological resilience. Perspect Psychiatr Care. 2021;57(1):399–407. PubMed CrossRef
- Özdin S, Bayrak Özdin Ş. Levels and predictors of anxiety, depression and health anxiety during COVID-19 pandemic in Turkish society: the importance of gender. Int J Soc Psychiatry. 2020;66(5):504–511. PubMed
- Byeon H. Association among smoking, depression, and anxiety: findings from a representative sample of Korean adolescents. PeerJ. 2015;3:e1288. PubMed CrossRef
- Melo MC, de Bruin VM, das Chagas Medeiros F, et al. Health of psychiatry residents: nutritional status, physical activity, and mental health. Acad Psychiatry. 2016;40(1):81–84. PubMed CrossRef
- Taylor S. The Psychology of Pandemics: Preparing for the Next Global Outbreak of Infectious Disease. Newcastle upon Tyne: Cambridge Scholars Publishing; 2019.
- Gardner PJ, Moallef P. Psychological impact on SARS survivors: critical review of the English language literature. Can Psychol. 2015;56(1):123–135. CrossRef
- Bish A, Michie S. Demographic and attitudinal determinants of protective behaviours during a pandemic: a review. Br J Health Psychol. 2010;15(Pt 4):797–824. PubMed CrossRef
- Blakey SM, Reuman L, Jacoby RJ, et al. Tracing “fearbola”: psychological predictors of anxious responding to the threat of ebola. Cognit Ther Res. 2015;39(6):816–825. PubMed CrossRef
- Waqas M, Hania A, Hongbo L. Psychological predictors of anxious responses to the COVID-19 pandemic: evidence from Pakistan. Psychiatry Investig. 2020;17(11):1096–1104. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!