Prim Care Companion CNS Disord 2022;24(4):22cr03253
To cite: Evenson S, Burgess J, Rustad JK. COVID-associated exacerbation of acute psychosis in a patient with schizoaffective disorder. Prim Care Companion CNS Disord. 2022;24(4):22cr03253.
To share: https://doi.org/10.4088/PCC.22cr03253
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Robert Larner, M.D. College of Medicine at the University of Vermont, Burlington, Vermont
bVermont Psychiatric Care Hospital, Montpelier, Vermont
cUniversity of Vermont Medical Center, Burlington, Vermont
dDepartment of Psychiatry, Geisel School of Medicine at Dartmouth, Lebanon, New Hampshire
eDepartment of Mental Health and Behavioral Sciences, White River Junction VA Medical Center, White River Junction, Vermont
fBurlington Lakeside VA Community-Based Outpatient Clinic, Burlington, Vermont
‡Co-first authors.
*Corresponding author: James K. Rustad, MD, Department of Psychiatry, Geisel School of Medicine at Dartmouth, Dartmouth-Hitchcock Medical Center, 1 Medical Center Dr, Lebanon, NH 03766 ([email protected]).
The case presented here, to the best of our knowledge, represents a first in published literature, in which a patient with preexisting schizoaffective disorder experienced an acute worsening of psychosis temporally related to coronavirus disease 2019 (COVID-19) infection.
Case Report
Mr A, a 36-year-old White man with a history of schizoaffective disorder (bipolar type), was admitted to the psychiatric hospital in August 2021 from a residential facility due to exacerbation of psychosis and mania in the setting of medication nonadherence. His symptoms had previously stabilized on clozapine 400 mg by mouth at night and haloperidol 10 mg by mouth at night. During hospitalization, haloperidol was titrated to 20 mg by mouth daily and 10 mg at night, but he declined to take clozapine due to the delusional belief that blood draws would kill him. While he continued experiencing auditory hallucinations and delusional ideation (eg, that he is an Italian vampire whose blood will not regenerate), he remained in good behavioral control, requiring no emergency involuntary procedures and typically scoring “small risk” (0) and always “moderate risk” or less (≤ 2) on the twice-daily Brøset Violence Checklist1 from September 24 to December 8, 2021. This lack of violence was consistent with his 15-year history since diagnosis of schizoaffective disorder.
On December 6, he received the first dose of the Janssen COVID-19 vaccine and, coincidentally, also tested positive for COVID-19 and was transferred to the COVID-19 unit. COVID-19 symptoms were mild and included cough, myalgias, and fevers/chills. He refused vitals. These symptoms peaked on December 9. On December 9, his behavior acutely changed. Without provocation, he threw objects at staff and assaulted staff, requiring manual, mechanical, and pharmacologic restraints. Shortly after being released from restraints, he assaulted a staff member by chokehold, again requiring restraints. That night, he received a total of haloperidol 30 mg, diphenhydramine 100 mg, and lorazepam 4 mg by mouth. His escalated behavior continued the next day, during which he assaulted staff on 3 different occasions, including punching a staff member in the head with force, biting and breaking a staff member’s finger, and spraining another staff member’s wrist. His mental status examination showed intense eye contact, poverty of speech, thought blocking, and command auditory hallucinations telling him that he needed to hurt others to be calm and on the path of God.
In addition to his scheduled haloperidol 20 mg daily, over the course of 9 hours, the patient required high doses of emergency antipsychotics, including olanzapine 25 mg, chlorpromazine 300 mg, lorazepam 6 mg, and diphenhydramine 50 mg by mouth. By night, he engaged in a cooperative discussion about safety and was released from 4-point restraints. He demonstrated a marked improvement in psychotic symptoms and behaviors over the next week while starting clozapine titration. His COVID-19 symptoms resolved by December 13.
Discussion
Evidence that infection may be an incipient factor in acute and chronic psychosis dates to when Menninger2 published on 100 cases of psychosis and other neuropsychiatric sequelae during the 1918 influenza pandemic. Since that time, it has become well established that infections, such as toxoplasmosis, syphilis, and HIV may be a causative factor in psychosis,3,4 and the number of types of infection associated with psychosis continues to expand to include influenza, Ebola, severe acute respiratory syndrome (SARS), Middle East respiratory syndrome, dengue, and Zika.5–9 Population-wide incidence of psychosis during respiratory epidemics and pandemics has been estimated to be 60-fold higher than median baseline incidence of psychosis.6 In a 6-month retrospective cohort evaluating psychiatric outcomes of 236,379 COVID-19 survivors, 1.4% developed a psychotic disorder. Interestingly, COVID-19–associated psychosis was more than 2-fold higher than influenza-associated psychosis and more than 1.6-fold higher for any respiratory infection–associated psychosis.10 This may be due to the extraordinary inflammatory and cytokine storm of COVID-19, which dysregulates neurotransmission.11
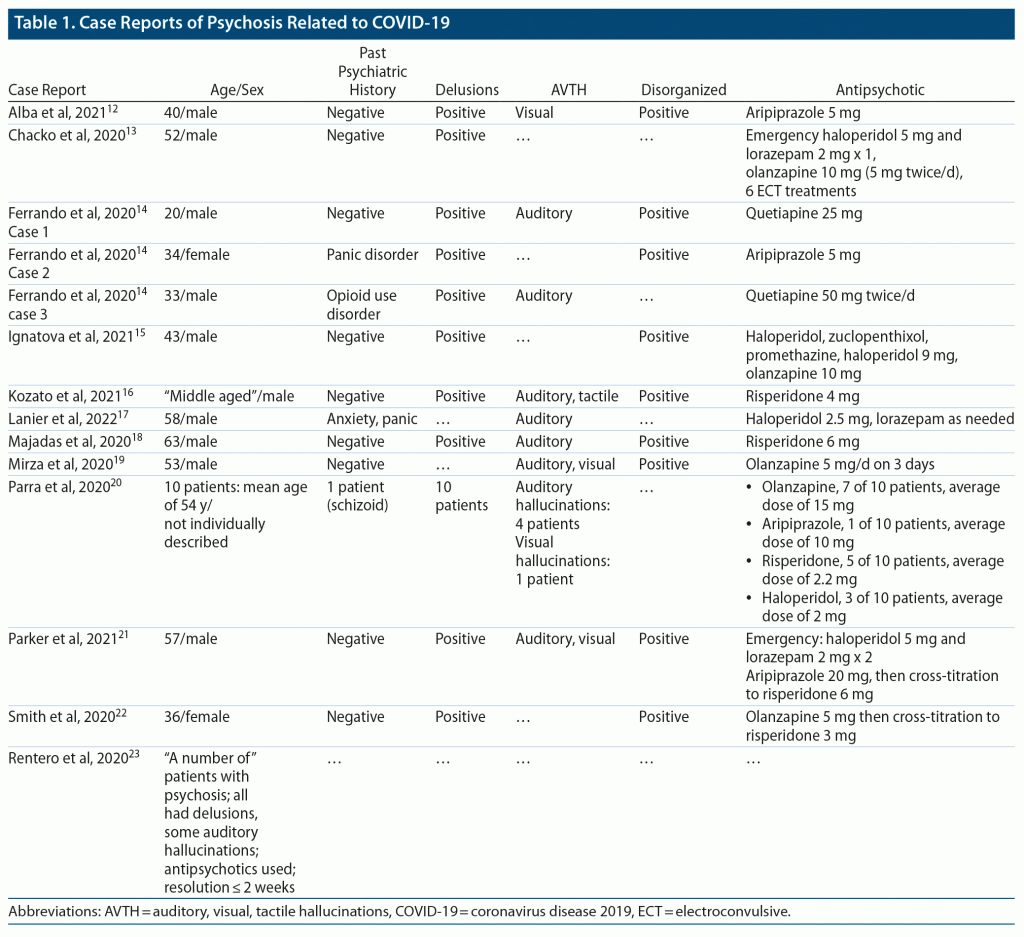
To date, there have been at least 14 case reports covering at least 23 cases of psychosis associated with COVID-19 (Table 1).12–23 Importantly, no cases of COVID-associated psychosis published to date have required COVID-specific treatment for psychosis. This contrasts with other forms of psychosis secondary to a medical condition, wherein treating the underlying condition is often necessary for resolution of psychosis.3 This may be because COVID is often a self-limiting virus, provided an individual survives the infection. Interestingly, antipsychotics, such as haloperidol, chlorpromazine, and the experimental 5-HT2A blocker cinanserin have demonstrated efficacy in treating SARS coronavirus in vitro and in vivo, and it may be possible that treatment with antipsychotics during COVID-associated psychosis also aids in the COVID resolution.24–26
The current case presents a patient with preexisting schizoaffective disorder who experienced acute worsening of psychosis temporally related to COVID-19 infection. Although it is possible that the presentation could have occurred during the natural course of his psychotic illness, the dramatic worsening of psychosis during his acute infection was notable. In particular, the patient’s level of violence due to command auditory hallucinations has never occurred in the patient’s 15-year history of schizoaffective disorder. The actionable lesson from this case is that COVID-19 may cause worsening of psychosis in patients with preexisting psychotic disorders and that the most likely treatment avenue remains dopamine-blocking agents.
Submitted: January 29, 2022.
Published online: June 28, 2022.
Relevant financial relationships: None.
Funding/support: None.
Patient consent: Informed consent was received from the patient to publish this report, and patient information was de-identified to protect anonymity.
References (26)

- Almvik R, Woods P, Rasmussen K. The Brøset Violence Checklist: sensitivity, specificity, and interrater reliability. J Interpers Violence. 2000;15(12):1284–1296. CrossRef
- Menninger KA. Psychosis associated with Influenza: I. general data: statistical analysis. JAMA. 1919;72(4):235–241. CrossRef
- Keshavan MS, Kaneko Y. Secondary psychoses: an update. World Psychiatry. 2013;12(1):4–15. PubMed CrossRef
- Yolken RH, Torrey EF. Are some cases of psychosis caused by microbial agents? a review of the evidence. Mol Psychiatry. 2008;13(5):470–479. PubMed CrossRef
- Srikanth S, Ravi V, Poornima KS, et al. Viral antibodies in recent onset, nonorganic psychoses: correspondence with symptomatic severity. Biol Psychiatry. 1994;36(8):517–521. PubMed CrossRef
- Brown E, Gray R, Lo Monaco S, et al. The potential impact of COVID-19 on psychosis: a rapid review of contemporary epidemic and pandemic research. Schizophr Res. 2020;222:79–87. PubMed CrossRef
- Cheng SKW, Tsang JSK, Ku KH, et al. Psychiatric complications in patients with severe acute respiratory syndrome (SARS) during the acute treatment phase: a series of 10 cases. Br J Psychiatry. 2004;184(4):359–360. PubMed CrossRef
- Chavez ME, Rojas M, Fortea A. Post dengue psychosis: report of 4 cases. Eur Neuropsychopharmacol. 2016;26:S574–S575. CrossRef
- Corrêa-Oliveira GE, do Amaral JL, da Fonseca BAL, et al. Zika virus infection followed by a first episode of psychosis: another flavivirus leading to pure psychiatric symptomatology. Br J Psychiatry. 2017;39(4):381–382. PubMed CrossRef
- Taquet M, Geddes JR, Husain M, et al. 6-month neurological and psychiatric outcomes in 236,379 survivors of COVID-19: a retrospective cohort study using electronic health records. Lancet Psychiatry. 2021;8(5):416–427. PubMed CrossRef
- Boldrini M, Canoll PD, Klein RS. How COVID-19 affects the brain. JAMA Psychiatry. 2021;78(6):682–683. PubMed CrossRef
- Alba L, Coll C, Sáez S, et al. New-onset psychosis: a case report of brief psychosis related to COVID-19 infection. Psychiatry Res. 2021;301:113975. PubMed CrossRef
- Chacko M, Job A, Caston F 3rd, et al. COVID-19-induced psychosis and suicidal behavior: case report. SN Compr Clin Med. 2020;2(11):2391–2395. PubMed CrossRef
- Ferrando SJ, Klepacz L, Lynch S, et al. COVID-19 psychosis: a potential new neuropsychiatric condition triggered by novel coronavirus infection and the inflammatory response? Psychosomatics. 2020;61(5):551–555. PubMed CrossRef
- Ignatova D, Krasteva K, Akabalieva K, et al. Post-COVID-19 psychosis: Cotard’s syndrome and potentially high risk of harm and self-harm in a first-onset acute and transient psychotic disorder after resolution of COVID-19 pneumonia. Early Interv Psychiatry. 2021;eip.13254. PubMed CrossRef
- Kozato N, Mishra M, Firdosi M. New-onset psychosis due to COVID-19. BMJ Case Rep. 2021;14(4):e242538. PubMed CrossRef
- Lanier CG, Lewis SA, Patel PD, et al. An unusual case of COVID-19 presenting as acute psychosis. J Pharm Pract. 2022;35(3):488–491. PubMed CrossRef
- Majadas S, Pérez J, Casado-Espada NM, et al. Case with psychotic disorder as a clinical presentation of COVID-19. Psychiatry Clin Neurosci. 2020;74(10):551–552. PubMed CrossRef
- Mirza J, Ganguly A, Ostrovskaya A, et al. Command suicidal hallucination as initial presentation of coronavirus disease 2019 (COVID-19): a case report. Psychosomatics. 2020;61(5):561–564. PubMed CrossRef
- Parra A, Juanes A, Losada CP, et al. Psychotic symptoms in COVID-19 patients: a retrospective descriptive study. Psychiatry Res. 2020;291:113254. PubMed CrossRef
- Parker C, Slan A, Shalev D, et al. Abrupt late-onset psychosis as a presentation of coronavirus 2019 disease (COVID-19): a longitudinal case report. J Psychiatr Pract. 2021;27(2):131–136. PubMed CrossRef
- Smith CM, Komisar JR, Mourad A, et al. COVID-19-associated brief psychotic disorder. BMJ Case Rep. 2020;13(8):e236940. PubMed CrossRef
- Rentero D, Juanes A, Losada CP, et al. New-onset psychosis in COVID-19 pandemic: a case series in Madrid. Psychiatry Res. 2020;290:113097. PubMed CrossRef
- Gordon DE, Jang GM, Bouhaddou M, et al. A SARS-CoV-2 protein interaction map reveals targets for drug repurposing. Nature. 2020;583(7816):459–468. PubMed CrossRef
- Weston S, Coleman CM, Haupt R, et al. Broad anti-coronavirus activity of Food and Drug Administration–approved drugs against SARS-CoV-2 in vitro and SARS-CoV in vivo. J Virol. 2020;94(21):e01218-20. PubMed CrossRef
- Chen L, Gui C, Luo X, et al. Cinanserin is an inhibitor of the 3C-like proteinase of severe acute respiratory syndrome coronavirus and strongly reduces virus replication in vitro. J Virol. 2005;79(11):7095–7103. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!