Objective: Exercise, yoga, and tai chi are commonly used complementary approaches for health and wellness. This review aims to synthesize the evidence for exercise, yoga, and tai chi in the outpatient treatment of major depressive disorder.
Study Selection: A systematic search of the Ovid MEDLINE, EMBASE, PsycINFO, and Cochrane databases was conducted for randomized controlled trials of exercise, yoga, and tai chi for major depressive disorder.
Data Extraction: Standardized mean differences were calculated and meta-analyzed using a random effects multilevel modeling framework. Heterogeneity and subgroup analysis was conducted.
Results: Twenty-five studies were included for final analysis (exercise: 15, yoga: 7, tai chi: 3). Overall, meta-analysis showed a moderate significant clinical effect. However, when only studies (6 studies) with the lowest risk of bias were included, the overall effect size was reduced to low to moderate efficacy. Overall quality of evidence was low. Heterogeneity and publication bias were high.
Conclusions: The current meta-analysis of outpatient exercise, yoga, and tai chi for treatment of major depressive disorder suggests that adjunctive exercise and yoga may have small additive clinical effects in comparison to control for reducing depressive symptoms. The evidence for tai chi is insufficient to draw conclusions. The concerns with quality of studies, high heterogeneity, and evidence of publication bias preclude making firm conclusions.

Exercise, Yoga, and Tai Chi for Treatment of Major Depressive Disorder in Outpatient Settings:
A Systematic Review and Meta-Analysis
ABSTRACT
Objective: Exercise, yoga, and tai chi are commonly used complementary approaches for health and wellness. This review aims to synthesize the evidence for exercise, yoga, and tai chi in the outpatient treatment of major depressive disorder.
Study Selection: A systematic search of the Ovid MEDLINE, EMBASE, PsycINFO, and Cochrane databases was conducted for randomized controlled trials of exercise, yoga, and tai chi for major depressive disorder.
Data Extraction: Standardized mean differences were calculated and meta-analyzed using a random effects multilevel modeling framework. Heterogeneity and subgroup analysis was conducted.
Results: Twenty-five studies were included for final analysis (exercise: 15, yoga: 7, tai chi: 3). Overall, meta-analysis showed a moderate significant clinical effect. However, when only studies (6 studies) with the lowest risk of bias were included, the overall effect size was reduced to low to moderate efficacy. Overall quality of evidence was low. Heterogeneity and publication bias were high.
Conclusions: The current meta-analysis of outpatient exercise, yoga, and tai chi for treatment of major depressive disorder suggests that adjunctive exercise and yoga may have small additive clinical effects in comparison to control for reducing depressive symptoms. The evidence for tai chi is insufficient to draw conclusions. The concerns with quality of studies, high heterogeneity, and evidence of publication bias preclude making firm conclusions.
Prim Care Companion CNS Disord 2021;23(1):20r02722
To cite: Seshadri A, Adaji A, Orth SS, et al. Exercise, yoga, and tai chi for treatment of major depressive disorder in outpatient settings: a systematic review and meta-analysis. Prim Care Companion CNS Disord. 2021;23(1):20r02722.
To share: https://doi.org/10.4088/PCC.20r02722
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry and Psychology, Mayo Clinic, Rochester, Minnesota
bDepartment of Psychiatry and Psychology, Mayo Clinic Health System, Austin, Minnesota
cSchool of Psychology, Deakin University, Geelong, Australia
dDepartment of Psychiatry, Monash Health-Casey Hospital, Berwick, Australia
eDepartment of Psychiatry, Olmsted Medical Center, Rochester, Minnesota
*Corresponding author: Ashok Seshadri, MD, Department of Psychiatry and Psychology, Mayo Clinic, 1000 First Drive NW, Austin, Minnesota 55912 ([email protected]).
Major depressive disorder (MDD) is a significant health care problem across the globe. MDD has high prevalence and recurrence and is associated with significant morbidity and mortality, loss of work productivity, increased associated health care costs, and high rates of suicide.1,2 Psychopharmacology and psychotherapy are the most commonly used clinical approaches for its treatment. However, although easily available through primary care providers, antidepressants have the disadvantage of a significant side effect burden, leading to poor treatment adherence. Evidence-based psychotherapy approaches are difficult for many people to access and require significant motivational investment and psychological mindedness to be effective. Alternative and complementary therapies are commonly sought after by patients with MDD, as such treatments are perceived to be more congruent with their own values and beliefs toward health and life.3,4
Exercise represents one of the most commonly used complementary approaches for health and wellness. Exercise is defined as any activity that involves planned, structured, and repetitive bodily movement done to improve or maintain physical fitness.5 Common forms of exercise involve aerobic exercise or strength training. Benefits of exercise for depression have been reported for depressive symptoms in previous systematic reviews.6-10 A Cochrane review11 of 35 randomized controlled trials (RCTs) of exercise for depression (diagnosed by any method of any severity) showed overall moderate clinical effect, using a random effects model standardized mean difference of −0.62 (95% CI, −0.81 to −0.42). There was significant heterogeneity in effect sizes (I2 = 63%). However, when only methodologically sound studies were included, the positive effects disappeared.11 A systematic review by Krogh and colleagues,12 however, suggested no benefits of exercise for clinical depression when considering only studies with less risk of bias. Further, it has not been possible to determine what type, duration, or intensity of exercise can be clinically beneficial for those suffering with a major depressive episode.
Other forms of physical activity, particularly forms of mindful movement including yoga and tai chi, have been used increasingly as complementary health approaches.4 Yoga and tai chi are traditional healing practices that come from ancient India and China, respectively. Yoga and tai chi combine the deliberate practice of repetitive movements with emphasis on controlled breathing-induced relaxation and concentration-focused meditation. Hatha yoga, the most commonly practiced yoga approach, combines movement and postures (asanas), breathing (pranayama), and meditation (dhyana). Different types of yoga vary in their emphasis on postures, breathing, and meditation. They include Iyengar yoga (focus on body postures), Vinyasa yoga (integrates postures and breathing—asanas and pranayama), Sudarshan Kriya yoga (predominantly breathing focused), and Sahaj yoga (meditation focused) among others. Tai chi is a Chinese martial art that involves complex, choreographed movements in coordination with breathing.13 Tai chi combines concentration, coordinated body movements, deep rhythmic breathing, and meditation to attain a relaxed state of mind.
A systematic review14 of yoga for treatment of MDD identified a heterogeneous group of studies comparing yoga to multiple interventions, with high risk of bias across studies. The results suggested positive effects in comparison to placebo and comparable effects to evidence-based interventions; however, considering the methodological heterogeneity, the authors14 did not complete a meta-analysis. To our knowledge, there are no systematic reviews of tai chi for adjunctive treatment of MDD.
Why Is This Review Important?
Exercise has long been believed to be effective for the treatment of depression.15 Several systematic reviews and meta-analyses of exercise for the treatment of depressive symptoms suggest a small, but favorable, clinical effect when factoring for quality of studies.6-11,16 However, the most recent review12 raised important questions about the clinical effect of exercise interventions when considering the quality of available evidence. The authors12 concluded that there was no evidence of positive effect when only higher-quality studies were included. However, the studies in this meta-analysis12 included participants with major and minor depression, inpatient and outpatient studies, and a wide range of follow-up duration. Therefore, the current review attempts to reevaluate the scientific evidence, limiting inclusion to studies using standardized diagnostic criteria for diagnosing MDD and having adequate follow-up duration of at least 8 weeks in outpatient settings. We decided to evaluate whether yoga and tai chi confer additional benefits compared to traditional western exercise practices for the treatment of MDD. Since the last systematic review14 of yoga, 5 RCTs of yoga for MDD have been published.

- Adjunctive exercise and yoga combined with usual antidepressant treatment may offer low to moderate additional clinical benefit for depression.
- Two to 3 sessions of yoga per week performed according to patient capacity may be sufficient for clinical benefit.
Therefore, the main objective of this systematic review is to determine the effectiveness of exercise, yoga, and tai chi compared to any intervention for treatment of MDD, meeting current episode criteria, diagnosed using standardized criteria (ICD-10 or DSM-IV/5), treated in clinical settings, and followed for a sufficient period of time.
METHODS
A systematic search of Ovid MEDLINE, EMBASE, PsycINFO, and Cochrane databases from inception to the second week of March 2019 was conducted on March 11, 2019, by a professional librarian with input from 3 study authors (A.S., M.F.T., J.M.). The search was updated on November 4, 2019. We searched database subject headings, title, and abstract with search terms that included exercise, exercise therapy, kinesiotherapy, yoga, and tai chi or taiji for MDD. We restricted our search to RCTs published in the English language and followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines.17
Study Selection
The online systematic review tool Covidence was used for title screening, full-text review, and data extraction.18 Title and abstract screening was done in duplicate by 2 independent reviewers (A.S. and S.O.). Conflicts were resolved by discussion. Our inclusion criteria were RCTs that included adult patients with MDD compared with any control condition, including other treatment interventions or treatment as usual (TAU), in a current episode, diagnosed using standardized diagnostic criteria with at least 8 weeks of follow-up data, in outpatient settings. We included studies of participant samples with MDD with comorbid conditions if MDD was diagnosed using standardized diagnostic criteria or by clinical interview by a specialist and identified as the primary target of treatment intervention. We excluded studies in which individuals reported depressive symptoms but were not formally diagnosed with MDD, studies that included participants with minor depression (symptoms of depression but not meeting diagnostic criteria for MDD), and those that did not provide outcome data for MDD separately. Studies were included if they provided sufficient data for calculation of effect sizes for the meta-analysis. Efforts were made to reach out to study authors in case of missing data or unclear findings. The primary outcome measure was change in depressive symptom severity assessed using standardized rating scales between the beginning and end of the treatment intervention period.
Data Extraction
Full-text review was completed in duplicate from studies meeting inclusion criteria by 2 authors (A.S. and S.S.O.), with any disagreements resolved by discussion and reaching consensus. Risk of bias assessment was completed by 2 independent authors (A.S. and A.A.) using the Cochrane risk of bias tool.19 Data were extracted by 2 independent reviewers (A.S. and A.A.), and any conflicts that arose were resolved through discussion and consensus.
Data Synthesis
We calculated and compared standardized mean differences for each intervention group for each study using pre- and posttreatment mean, standard deviation (SD) or 95% confidence interval, and number of participants. We extracted the effect sizes if they were reported. Standardized mean differences were calculated using Hedges’ g instead of Cohen d, as the latter is known to produce biased effect estimates for smaller samples.20 Three exercise studies21-23 had multiple comparison groups comprised of different exercise interventions measured against controls. We treated each comparison independently for these 3 studies. To prevent double counting of participants, we divided the sample sizes of common comparison groups within studies. One exercise study24 had multiple comparison groups (ie, 5 groups) comprised of different doses (low dose vs public health dose) and duration of exercise (3 days/wk or 5 days/wk) interventions measured against control. We combined the results of the different dose arms to obtain a single comparison to the control group.24
Statistical Analysis
R studio (R version 3.6.1)25 was used to conduct meta-analysis and subgroup analysis. The inverse variance method was used for weighting studies of differing sample sizes. We used a random effects multivariate model framework to compute overall effect sizes for the meta-analysis to account for complex data structures such as multiple comparison groups within studies.
All analyses including exercise studies used the multivariate model framework. We used a random effects model to pool effect sizes using the DerSimonian-Laird estimator when analyzing yoga and tai chi studies separately, as they had single effect estimates.26 All other subgroup analyses were conducted using mixed effects modeling.
Heterogeneity and Subgroup Analysis
Heterogeneity was assessed using the Cochran Q statistic with P < .10 used as a cutoff to attribute heterogeneity between study factors rather than by chance.27 The I2 statistic was used to assess the contribution of between-study heterogeneity to the overall estimate of heterogeneity. We assigned cutoffs of 25%, 50%, and 75% for small, moderate, and large levels of heterogeneity between studies, respectively.27 Sensitivity analysis was conducted after removing outliers and high-risk studies. Subgroup analysis, based on a mixed effects model, was conducted to further investigate heterogeneity between studies by stratifying studies according to types of active intervention, comparator groups (active control or attention control versus treatment-as-usual/inactive control), participant characteristics (clinical setting or volunteers from nonclinical setting), augmentation, or monotherapy.
Publication Bias
Egger regression test and funnel plots, using the trim-and-fill method, were utilized to qualitatively and quantitatively assess publication bias.28,29 We performed random effects meta-analysis using imputed data to account for effects of publication bias.
Risk of Bias Assessment
The Cochrane risk of bias tool19 was used to assess bias in the meta-analysis. This tool contains categories for sequence generation, allocation concealment, blinding of participants and personnel, blinding of outcome assessment, handling of incomplete data, selective reporting, and any other forms of bias. Cochrane guidelines recommend that all key domains be rated low risk to qualify for a global low-risk score. Even a single high or unclear risk domain confers high risk on a global scale.19 Considering the nature of exercise, yoga, and tai chi interventions, blinding of participants and personnel providing interventions is not possible. We thus excluded this item from our risk of bias assessment. For this review, we classified studies as having low bias if they had low risk of bias assessed by sequence generation, allocation concealment, blinding of personnel, blinding of outcome assessment, handling of incomplete data, and selective reporting.
RESULTS
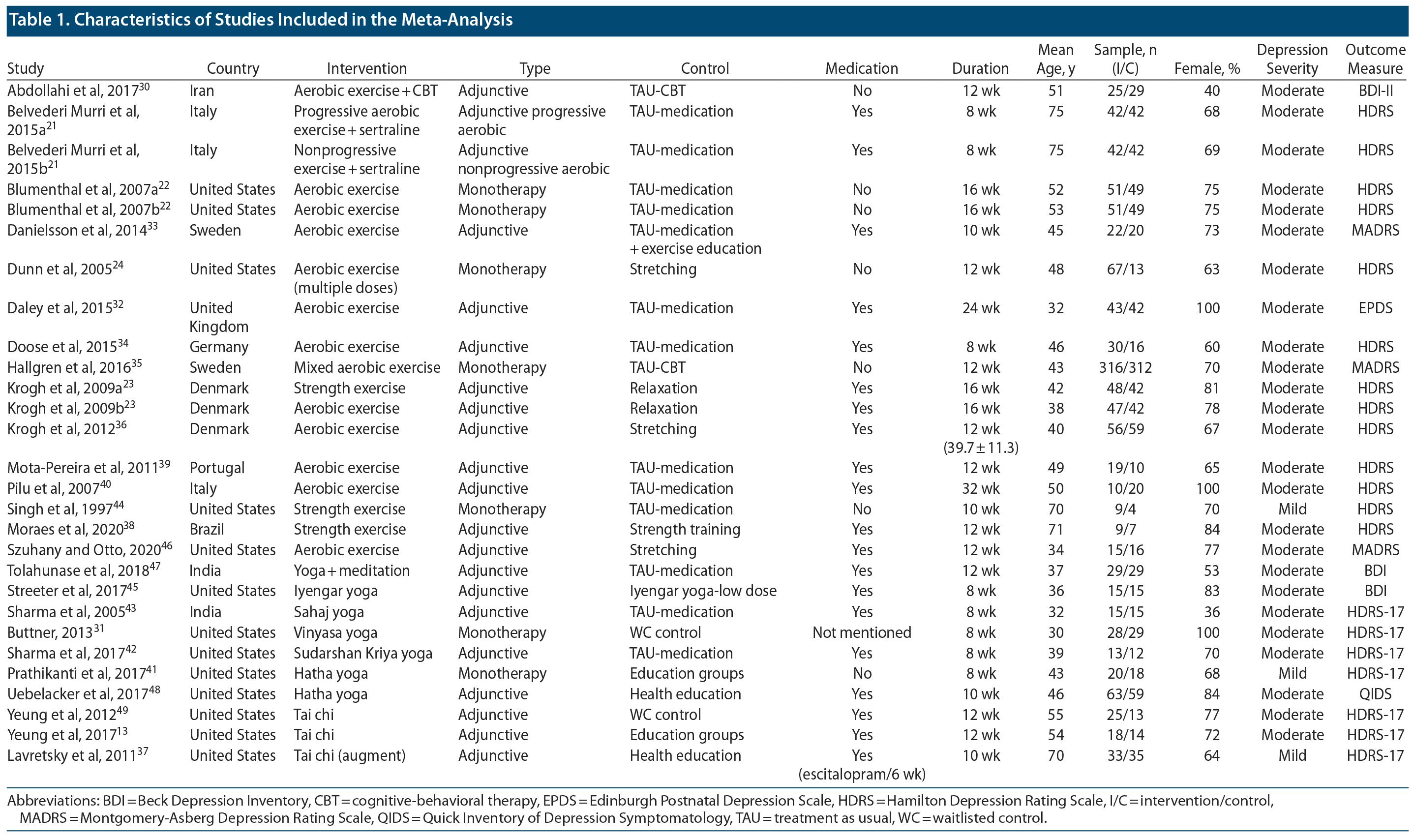
Our search strategy resulted in 1,017 published articles. After deduplication, 689 articles were screened based on title and abstract from which 60 studies were found eligible for full-text review. Twenty-five RCTs13,21-24,30-49 were included in the meta-analysis (Supplementary Figure 1). Across 15 exercise, 7 yoga, and 3 tai chi studies, 1,112 participants were enrolled in the intervention groups, while 971 participants were enrolled in the control groups. The RCTs were conducted in the United States (12),13,22,24,31,37,41,42,44-46,48,49 Brazil (1),38 the United Kingdom (1),32 Sweden (2),33,35 Italy (2), Denmark (2),23,36 Germany (1),34 Portugal (1),39 India (2),43,47 and Iran (1).30
Exercise
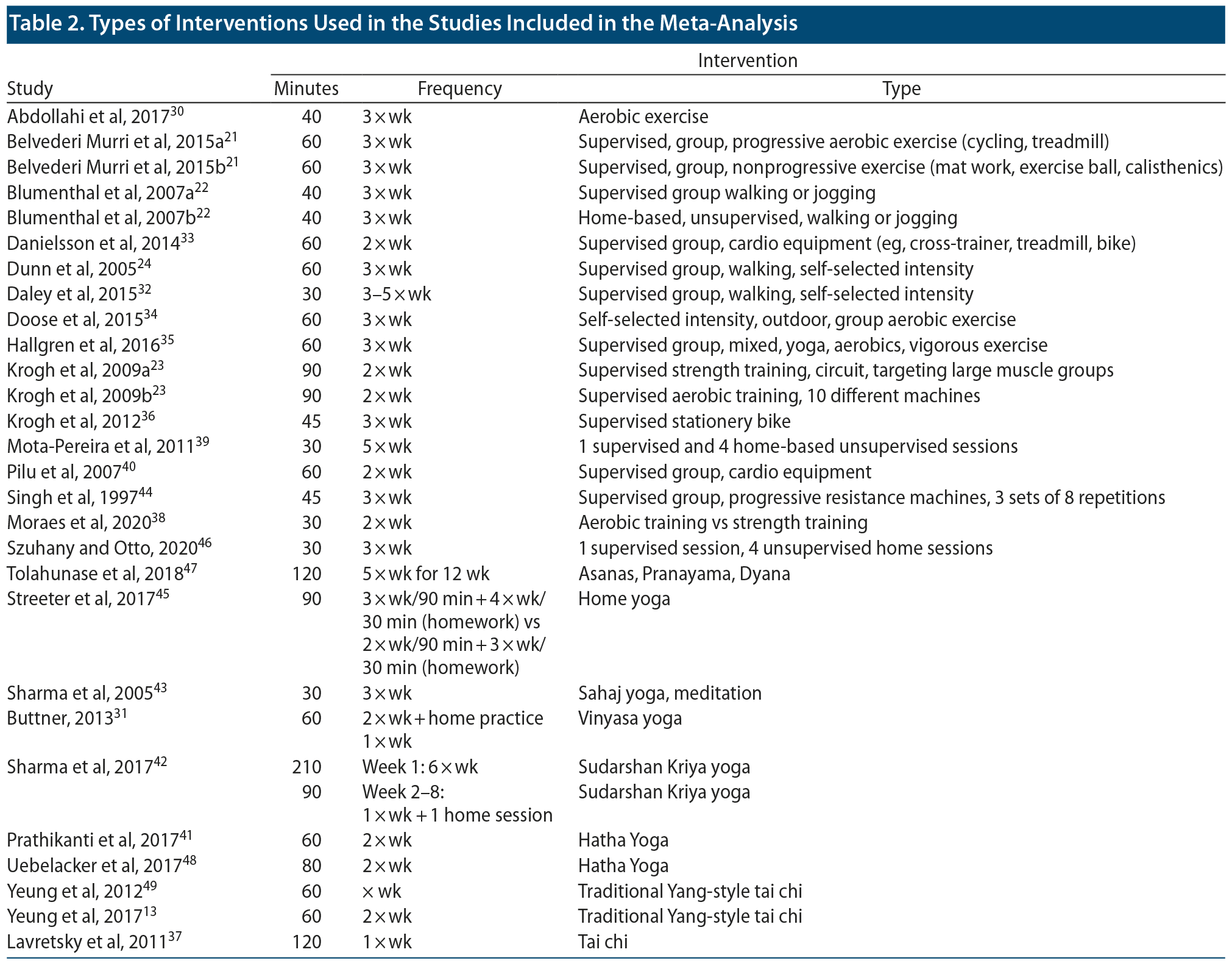
The most common exercise type was aerobic exercise (17 groups from 15 studies21-24,30,32-36,38-40,44,46) including walking, jogging, and aerobic exercise machines such as the treadmill and stationary bike, with strength training used in 3 groups (Table 1). The treatment duration for exercise studies varied between 8 and 32 weeks, with a mean study duration of 15.5 weeks (Table 1). Most of the exercise sessions (15) were group based and conducted with close supervision with other study participants. Three studies22,39,46 used home-based exercise programs. In the exercise studies, there were 15 intervention groups using exercise augmentation to usual therapy and 6 intervention groups using exercise monotherapy (Table 2).
Yoga and Tai Chi
Five yoga studies had treatment duration of 8 weeks, while 2 studies used longer treatment duration periods of 1048 and 1247 weeks. Five yoga studies31,41,45,47,48 used Hatha yoga, while 1 study used Sudarshan Kriya yoga42 and 1 used Sahaj yoga.43 Five yoga studies42,43,45,47,48 used yoga as an augmentation strategy, while 2 studies31,41 used yoga monotherapy. All 3 tai chi studies13,37,49 used 10- to 12-week intervention periods to augment usual treatment for depression compared to control conditions.
Sample Characteristics
All except 3 RCTs had participants diagnosed with moderate depressive episode, while 3 studies37,41,44 recruited participants with mild depression based on baseline outcome measure scores. The Hamilton Depression Rating Scale (15 studies)50 and Beck Depression Inventory (4 studies)51 were the most common outcome measures. One RCT39 recruited a sample with treatment-resistant depression. In terms of control interventions, there were 14 inactive TAU intervention groups, 7 attention-controlled education groups, 3 cognitive-behavioral therapy groups, 1 active control group of low-dose intervention (yoga), 2 active exercise interventions, and 2 active medication controls.
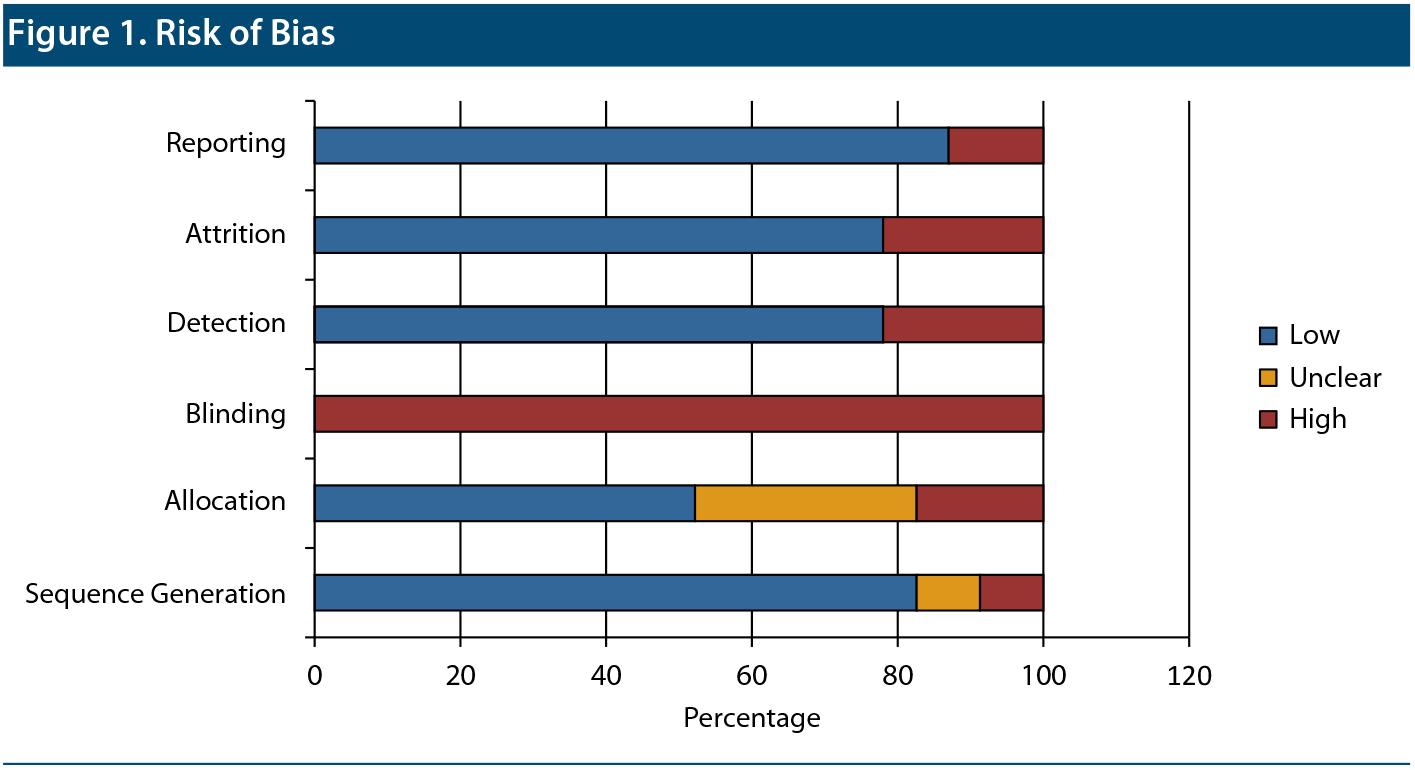
Risk of Bias in Included Studies
The risk of bias was assessed using Cochrane risk of bias criteria (Figure 1). Nineteen RCTs (73% of overall studies) provided details of sequence generation for randomization. However, allocation concealment was reported in only 12 studies13,21,22,24,31-33,37,41,45,47,49 (48%). Overall, 3 studies34,43,46 were rated as having high risk of selection bias, while 10 studies23,24,30,35,37-39,42,44,48 were rated as unclear (combined 52%). The risk of detection bias was rated high or unclear for 6 RCTs13,31,34,40,42,43 (24%). Six studies13,23,30,39,46,49 (24%) did not report intent-to-treat statistical analysis, while 3 studies13,23,39 (12%) showed reporting bias. Given that the interventions were exercise, yoga, and tai chi, blinding of participants and personnel was difficult, making the risk of bias inherently high, particularly when the control intervention was a passive or TAU condition. Overall, 621,22,32,41,45,47 of the 25 studies qualified as a high-quality study across the risk of bias criteria, excluding blinding of participants and personnel criteria.
Effects of Interventions on Depression
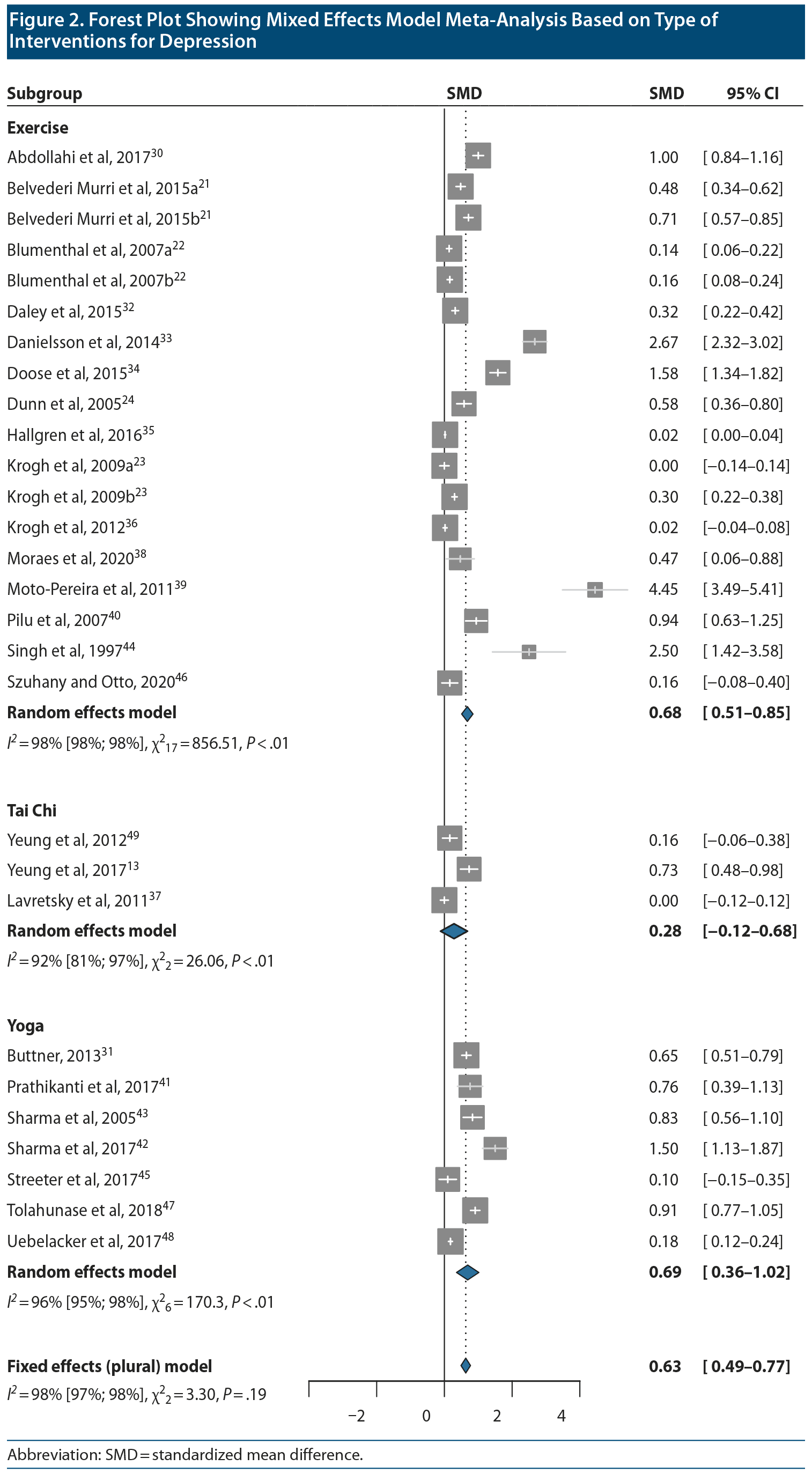
Multivariate model meta-analysis revealed that, taken together, exercise, yoga, and tai chi showed efficacy in reducing depression symptoms with a moderate favorable effect in reducing depression symptoms compared to all control conditions, applying Cohen cutoff criteria (0.2: small, 0.5: moderate, 0.8: large) for effect sizes (k = 28; Hedges’ g = 0.63; 95% CI, 0.50-0.76; P < .001)52 (Figure 2). Cochran Q statistic (1,165, df = 27, P < .001) suggested significant heterogeneity. The I2 statistic indicated that 98% of the variance was accounted for by between-study differences in effect size, with 7 studies30,33,34,39,42,44,47 contributing the most to overall heterogeneity. Influence analysis removing the 7 outlier studies revealed significant influence to the pooled effect sizes. The overall effect was reduced to a small to moderate effect size (k = 21; Hedges’ g = 0.33; 95% CI, 0.23-0.42; P < .001) with a significant Cochran Q statistic (410, df = 20, P < .001). When we included only the 6 studies meeting criteria for the lowest risk of bias (3 exercise studies and 3 yoga studies),21,22,32,41,45,47 the overall effect size showed low to moderate efficacy in reducing depressive symptoms (k = 8; Hedges’ g = 0.41; 95% CI, 0.14-0.66; P = .007).
Subgroup Analysis
Intervention. Exercise. Fifteen RCTs of exercise comprised of 18 groups of exercise compared to controls were included in the meta-analysis. This included 15 groups of aerobic exercise and 3 groups of strength training exercises. Fourteen groups used exercise augmentation to usual therapy, while 4 groups used exercise monotherapy. All studies recruited participants with moderate depression except 1 with mild depression.44 Three studies22,39,46 employed home-based facilitated exercise protocols, the majority being supervised onsite group sessions. The most common exercise frequency was 3 sessions per week, with duration ranging from 30 to 60 minutes. Compared to the control groups, multivariate model random effects meta-analysis showed that exercise-based interventions had an overall moderate effect in improving depressive symptoms at the end of the intervention period (k = 18; Hedges’ g = 0.74; 95% CI, 0.06-1.40; P = .03). There was significant heterogeneity (Q = 113, df = 17, P < .001), with significant variance due to between-study differences in effect size (I2 = 98%). When only the 3 high-quality studies were included,21,22,32 low to moderate effect was observed (Hedges’ g = 0.31; 95% CI, 0.03-0.59; P = .03), with low heterogeneity between studies (Q = 3.9, df = 4, P = .4). Removing 5 outlier studies30,33,34,39,44 from the meta-analysis caused the effect size to decrease (Hedges’ g = 0.23; 95% CI, 0.07-0.38; P = .007), with low heterogeneity between studies (Q = 15, df = 12, P = .21).
Yoga. Random effects meta-analysis of 7 RCTs of yoga with 7 treatment arms showed that yoga improved depression outcomes in comparison to control conditions with moderate effect size (n = 260; Hedges’ g = 0.69; 95% CI, 0.36-1.02; P < .001). There was significant heterogeneity (Q = 170, df6 = 3, P < .001), with significant variance due to between-study differences in effect sizes (I2 = 96%). When only higher-quality studies41,45,47 were included in the meta-analysis, an effect size of Hedges’ g = 0.59; 95% CI, 0.04-1.13; P = .03 was observed. Significant between-study heterogeneity was also observed (I2 = 93%).
Tai Chi. Random effects meta-analysis of 3 RCTs comparing tai chi with controls that included 2 attention control education groups and 1 waitlist control group showed no significant difference in reducing depression symptoms between tai chi and control groups (n = 138; Hedges’ g = 0.28; 95% CI, −0.12-0.68; P = .25), with high heterogeneity (Q = 26, df = 2, P < .001, I2 = 92%).
Type of Control
Exercise, yoga, and tai chi (combined) were significantly superior to the active group (Hedges’ g = 0.45; 95% CI, 0.26-0.63; P < .01) and TAU group (Hedges’ g = 0.81; 95% CI, 0.59-1.30; P < .001). A mixed effects model test for subgroup differences showed significantly larger differences for TAU controls compared to active controls (Q = 6.2, df = 1, P < .02).
Clinical Participants or Volunteers
Exercise, yoga, and tai chi (combined) were significantly superior to control in the clinical group (Hedges’ g = 0.57; 95% CI, 0.41-0.73; P < .01) and volunteer group (Hedges’ g = 0.81; 95% CI, 0.47-1.15; P < .01). A mixed effects model test for subgroup differences showed significantly greater effect in volunteers compared to clinical participants (Q = 4.8, df = 1, P = .02).
Quality of Studies
Exercise, yoga, and tai chi (combined) were significantly superior to control in high-quality studies (Hedges’ g = 0.44; 95% CI, 0.24-0.64; P < .01) and low-quality studies (Hedges’ g = 0.78; 95% CI, 0.49-0.96; P < .01). A mixed effects model test for subgroup differences showed significant differences based on quality of studies (Q = 4.72, df = 1, P = .03), such that efficacy estimates were larger among low-quality studies.
Augmentation or Monotherapy
Exercise, yoga, and tai chi (combined) were significantly superior to control when used as monotherapy (Hedges’ g = 0.40; 95% CI, 0.21-0.60; P < .01) or as augmentation to standard therapy (Hedges’ g = 0.71; 95% CI, 0.53-0.96; P < .01). A mixed effects model test for subgroup differences showed significantly greater effect with augmentation to standard therapy (Q = 5.17, df = 1, P = .02).
Dose or Duration of Intervention
There was no significant difference between duration of intervention sessions of duration of 30 to 45 minutes or session lengths > 60 minutes (Q = 0.09, df = 1, P = .75). Similarly, there were no differences between exercise frequency ≤ 3 sessions per week or ≥ 3 sessions per week. (Q = 1.88, df = 1, P = .38).
Publication Bias
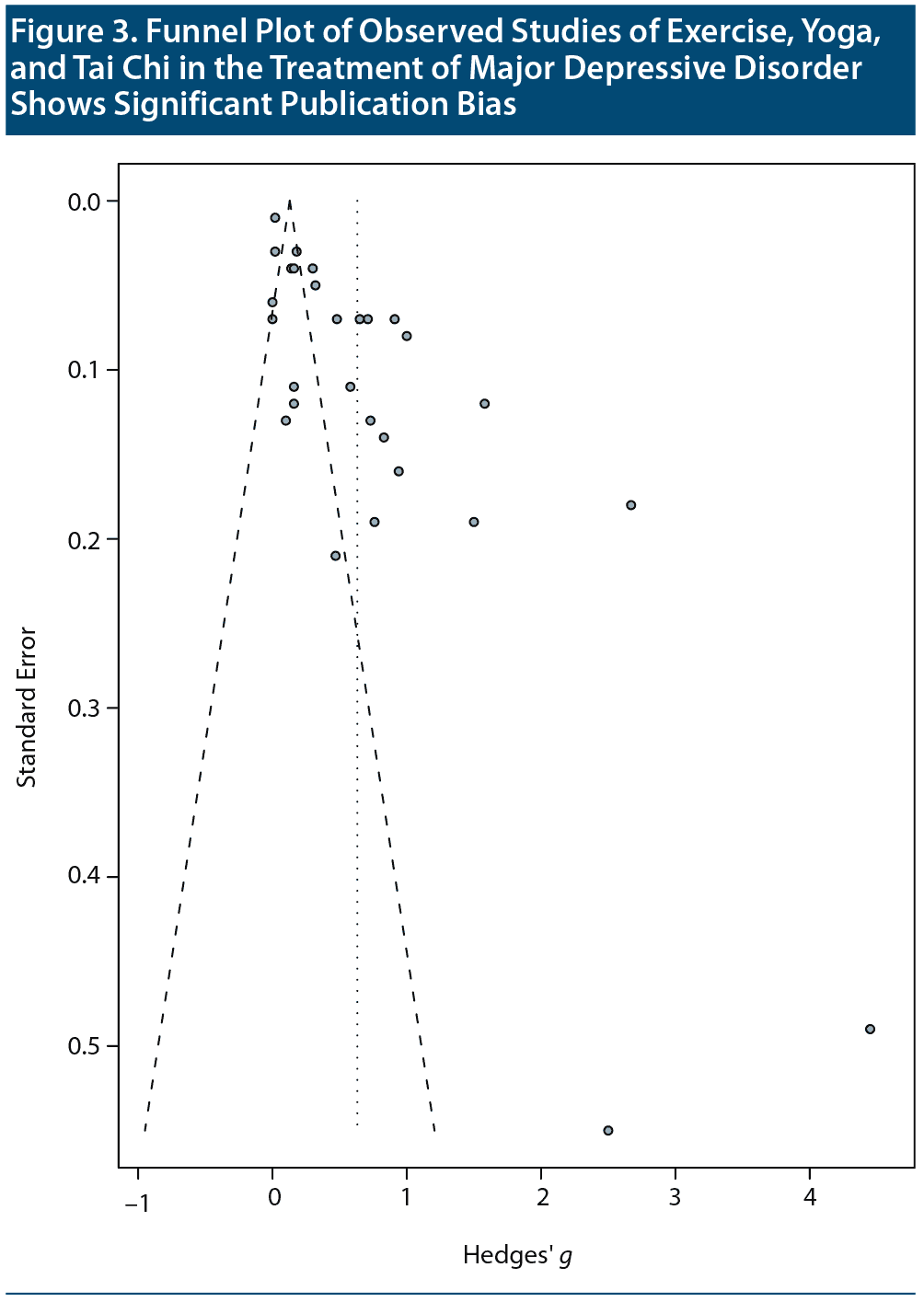
Qualitative and quantitative assessments of publication bias for studies of exercise, yoga, and tai chi using Funnel plot with trim-and-fill method and Egger regression test (intercept = 6.72; 95% CI, 4.6-8.9; t = 6.4; P < .001) showed significant concerns with reporting bias (Figure 3). The trim-and-fill method identified and imputed 14 studies to adjust for funnel plot asymmetry. A random effects meta-analysis including the imputed data estimated the effect size for the interventions to be low (Hedges’ g = 0.11; 95% CI, −0.03-0.26; P = .13). When publication bias for studies of yoga are considered separately, an imputed model suggests a small, nonsignificant positive effect on depression (Hedges’ g = 0.32; 95% CI, −0.005-0.6; Z = 1.93; P = .05). However, considering the low number of yoga studies, this model may lack adequate statistical power to detect publication bias.
DISCUSSION
Summary of Main Results
The current meta-analysis of studies on exercise, yoga, and tai chi yields findings that suggest exercise and yoga may have a small additive clinical benefit as a complementary strategy to other standardized treatment modalities in the treatment of MDD. However, our study confirms the concerns expressed by previous authors11,12 regarding overall quality of the published literature. Our study identified concerns for high publication bias as well. Although the overall pooled effect of exercise and yoga shows moderate clinical effect in reducing depressive symptoms in patients with a current depressive episode, this finding is based on overall low-quality evidence. When factoring in quality, the clinical effect is low in reducing depressive symptoms. When factoring for publication bias, the positive treatment effect disappears.
However, with the currently available evidence, adjunctive exercise and yoga added to usual treatment for depression may be superior to usual treatment alone. Although yoga had a better clinical effect on depression symptoms compared to exercise (after adjusting for quality and publication bias), current knowledge is inadequate to draw conclusions on its relative effect compared to traditional exercise such as aerobic exercise or strength training. Adjunctive tai chi does not appear to be an effective intervention for MDD based on current evidence.
Overall Completeness and Applicability of Evidence
This review systematically searched the published literature in English for RCTs on exercise, yoga, and tai chi in the treatment of a current episode of MDD. We focused our review on adults diagnosed with clinical MDD. Included studies from clinical settings used clinical or standardized assessment criteria to diagnose MDD in participants. Participants in studies drawn from community volunteers were diagnosed using standardized diagnosis criteria. We excluded studies with participants reporting depressive symptoms without a formal diagnosis of MDD. While other reviews for exercise for depression exist, the last review focusing on clinical MDD was published in 2011.16 This is the first review to include other modalities like tai chi and yoga, wherein additional mental processes are involved in addition to physical movements. We have updated the literature of yoga studies for MDD. This review focuses on the acute effects of exercise, yoga, and tai chi for depressive symptoms in MDD with a follow-up duration of at least 8 weeks. This is comparable to similar study designs of pharmacotherapy and psychotherapy interventions. However, this design does not address the longer-term effectiveness of these interventions in the treatment of MDD. We were unable to make any conclusions on optimal dose or frequency of exercise. On the basis of our analysis, we found no difference between groups based on dose or duration of exercise. One study24 found that public health dose of exercise (defined by energy expenditure of 17.5 cal/kg/wk for 3-5 days a week) was no more effective than low-dose exercise (defined by energy expenditure 7 cal/kg/wk for 3 days a week) in reducing depressive symptoms. Most of the RCTs (20 studies) employed trial designs of 2 to 3 supervised sessions a week with exercise performed according to the capacity of the participants.
Quality of the Evidence
Many of the included studies in this meta-analysis showed risk of bias. Allocation concealment bias was judged high or unclear in 48% of the studies. Six studies did not report results using intention-to-treat analysis (24%), while 6 studies showed detection bias (24%). Considering that the intervention was a form of physical activity, compared to control, there was significant risk of participant bias due to difficulty with blinding participants adequately, even when attention controlled designs were used. Overall, 6 studies qualified as high-quality across all criteria, except participant blinding. We found significant publication bias as illustrated by the asymmetric funnel plot, which likely overestimates the overall effect size of the interventions. We searched the published and gray literature and attempted to reach authors when effect size data were not clearly presented in published reports. However, we did not obtain responses to all of our requests for data.
Agreements and Disagreements With Other Studies or Reviews
A 2013 Cochrane review and meta-analysis of exercise for depression by Cooney et al11 reported moderate positive treatment effects for depression in comparison to control interventions. This effect reduced to a smaller effect when only high-quality studies were included. This review was not restricted to clinical populations or diagnosis of MDD using standardized diagnostic criteria.11 The overall effect size was similar to that of the current study. A more recent meta-analysis12 of exercise showed overall similar effect size (SMD = 0.66) to our current study, but also included studies with participants classified as having minor depression and inpatient participant samples. When only high-quality studies were included, no differences between exercise and control interventions were found.12 In contrast, using more strict inclusion criteria of diagnosis, follow-up duration, and settings, we found evidence of a small positive effect size for studies of higher quality in our analysis.
Implications for Practice
Our review suggests high risk of bias with the published literature of exercise, yoga, and tai chi interventions for MDD. Although the overall effect sizes suggest moderate clinical efficacy for exercise as an augmenting strategy in the treatment of MDD, when only the studies of higher quality are included, the effects of exercise are likely to be modest. Our review suggests that yoga may have a low to moderate effect on depression when used as an augmenting strategy. The effect was maintained even when only higher-quality studies were included in the analysis. We do not have enough evidence to make a judgment on effect of tai chi for MDD. Taken together, the evidence suggests that complementary exercise and yoga may offer low to moderate additional clinical benefit when added to a treatment plan for a major depressive episode. In terms of dosing, 2 to 3 sessions per week performed according to the capacity of the participants may be adequate to obtain the clinical benefit.
Implications for Research
The role of behavioral activation in recovery from depression and the relative lack of perceived side effects from exercise have led to continued interest in use of exercise as a treatment option for patients with MDD. Adoption of complementary health practices from other regions of the world like yoga and tai chi has attracted greater interest among researchers in assessing the effects of yoga and tai chi for patients with MDD. This is evident from the multiple research publications in the last 2 years.
Larger, adequately powered studies with more robust methodology are needed to confirm early findings from the current body of studies of yoga and tai chi. Future studies of exercise, yoga, and tai chi should focus on research methodologies that use control groups utilizing evidence-based therapies or active attention-controlled groups. Trials of exercise interventions from outside Europe and North America and yoga/tai chi studies from Europe may answer whether the interventions can be applied across cultures. Additionally, head-to-head trials between exercise, yoga, and tai chi interventions may also address if one type of exercise intervention is more acceptable and feasible for people suffering from MDD. This may allow for better attention-controlled designs of RCTs.
CONCLUSIONS
The current meta-analysis of studies of exercise, yoga, and tai chi for treatment of MDD suggest that complementary and adjunctive exercise and yoga may have a small clinical effect in comparison to treatment as usual for reducing depressive symptoms following an acute course of therapy when factoring for quality of included studies. However, the concerns with quality of studies, high heterogeneity, and evidence of publication bias found in our meta-analysis preclude making firm conclusions on clinical effect. Larger, well-designed trials with robust clinical trial methodologies are needed to further confirm these findings. There is insufficient evidence to make a conclusion on the effectiveness of tai chi for MDD.
Submitted: June 19, 2020; accepted August 31, 2020.
Published online: December 31, 2020.
Author contributions: Study design: Drs Seshadri, Clark, Frye, Fuller-Tyszkiewicz, and McGillivray. Data collection: Drs Seshadri, Orth, and Adaji. Data analysis: Drs Seshadri, Singh, and Fuller-Tyszkiewicz. Drafting of manuscript: Dr Seshadri. Critical review of manuscript: Drs Singh, Clark, Frye, Fuller-Tyszkiewicz, and McGillivray.
Potential conflicts of interest: Dr Clark has received consultant fees from Roche Diabetes Care GmbH. Dr Frye has received grant support from Assurex Health, Mayo Foundation, and Medibio; consultant fees from Actify Neurotherapies, Allergan, Intra-Cellular Therapies, Janssen, Myriad, Neuralstem, Takeda, and Teva; and CME/travel/honoraria from American Physician Institute, CME Outfitters, and Global Academy for Medical Education. Drs Seshadri, Adaji, Orth, Singh, Fuller-Tyszkiewicz, and McGillivray report no conflicts of interest related to the subject of this article.
Funding/support: None.
Acknowledgments: The authors thank librarians Ann Farrell and Larry Prokop (Mayo Clinic, Rochester, New York), who helped with the literature search, and Lori Solmonson and Angie Lam (Mayo Clinic, Rochester, New York), who performed a thorough review of the manuscript in preparation for article submission. The acknowledged individuals report no conflicts of interest related to the subject of this article.
Additional information: The data that support the findings of this study are available on request from Dr Seshadri ([email protected]). The data are not publicly available due to privacy or ethical restrictions.
Supplementary material: See accompanying pages.
REFERENCES
1. Kessler RC. The effects of stressful life events on depression. Annu Rev Psychol. 1997;48(1):191-214. PubMed Crosseref
2. Moussavi S, Chatterji S, Verdes E, et al. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet. 2007;370(9590):851-858. PubMed CrossRef
3. Astin JA. Why patients use alternative medicine: results of a national study. JAMA. 1998;279(19):1548-1553. PubMed CrossRef
4. Clarke TC, Black LI, Stussman BJ, et al. Trends in the use of complementary health approaches among adults: United States, 2002-2012. Natl Health Stat Rep. 2015;(79):1-16. PubMed
5. Roitman J, Herridge M, American College of Sports Medicine. ACSM’s Resource Manual for Guidelines for Exercise Testing and Prescription. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 2001.
6. Lawlor DA, Hopker SW. The effectiveness of exercise as an intervention in the management of depression: systematic review and meta-regression analysis of randomised controlled trials. BMJ. 2001;322(7289):763-767. PubMed CrossRef
7. Mead GE, Morley W, Campbell P, et al. Exercise for depression. Cochrane Database Syst Rev. 2008;(4):CD004366. PubMed
8. Rethorst CD, Wipfli BM, Landers DM. The antidepressive effects of exercise: a meta-analysis of randomized trials. Sports Med. 2009;39(6):491-511. PubMed CrossRef
9. Sjösten N, Kivelפ SL. The effects of physical exercise on depressive symptoms among the aged: a systematic review. Int J Geriatr Psychiatry. 2006;21(5):410-418. PubMed CrossRef
10.Stathopoulou G, Powers M, Berry A, et al. Exercise interventions for mental health: a quantitative and qualitative review. Clin Psychol Sci Pract. 2006;13(2):179-193. CrossRef
11.Cooney GM, Dwan K, Greig CA, et al. Exercise for depression. Cochrane Database Syst Rev. 2013;(9):CD004366. PubMed
12.Krogh J, Hjorth׸j C, Speyer H, et al. Exercise for patients with major depression: a systematic review with meta-analysis and trial sequential analysis. BMJ Open. 2017;7(9):e014820. PubMed CrossRef
13.Yeung AS, Feng R, Kim DJH, et al. A pilot, randomized controlled study of tai chi with passive and active controls in the treatment of depressed Chinese Americans. J Clin Psychiatry. 2017;78(5):e522-e528. PubMed CrossRef
14.Cramer H, Anheyer D, Lauche R, et al. A systematic review of yoga for major depressive disorder. J Affect Disord. 2017;213:70-77. PubMed CrossRef
15.Beesley S, Mutrie N. Exercise is beneficial adjunctive treatment in depression. BMJ. 1997;315(7121):1542-1543. PubMed CrossRef
16.Krogh J, Nordentoft M, Sterne JA, et al. The effect of exercise in clinically depressed adults: systematic review and meta-analysis of randomized controlled trials. J Clin Psychiatry. 2011;72(4):529-538. PubMed CrossRef
17.Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700. PubMed CrossRef
18.Covidence. Covidence systematic review software. Covidence website. www.covidence.org. Published 2019. Accessed December 1, 2020.
19.Higgins JPT, Green SE. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaboration website. http://handbook.cochrane.org. Published 2011. Updated March 2011. Accessed December 1, 2020.
20.Borenstein M, Hedges L, Higgins J, et al. Introduction to Meta-Analysis. Chichester, UK: John Wiley & Sons; 2009.
21.Belvederi Murri M, Amore M, Menchetti M, et al; Safety and Efficacy of Exercise for Depression in Seniors (SEEDS) Study Group. Physical exercise for late-life major depression. Br J Psychiatry. 2015;207(3):235-242. PubMed CrossRef
22.Blumenthal JA, Babyak MA, Doraiswamy PM, et al. Exercise and pharmacotherapy in the treatment of major depressive disorder. Psychosom Med. 2007;69(7):587-596. PubMed CrossRef
23.Krogh J, Saltin B, Gluud C, et al. The DEMO trial: a randomized, parallel-group, observer-blinded clinical trial of strength versus aerobic versus relaxation training for patients with mild to moderate depression. J Clin Psychiatry. 2009;70(6):790-800. PubMed CrossRef
24.Dunn AL, Trivedi MH, Kampert JB, et al. Exercise treatment for depression: efficacy and dose response. Am J Prev Med. 2005;28(1):1-8. PubMed CrossRef
25.RStudio: Integrated Development for R. RStudio website. http://www.rstudio.com/. Published 2015. Accessed July 5, 2019.
26.DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7(3):177-188. PubMed CrossRef
27.Higgins JP, Thompson SG, Deeks JJ, et al. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557-560. PubMed CrossRef
28.Duval S, Tweedie R. Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics. 2000;56(2):455-463. PubMed CrossRef
29.Egger M, Davey Smith G, Schneider M, et al. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315(7109):629-634. PubMed CrossRef
30.Abdollahi A, LeBouthillier DM, Najafi M, et al. Effect of exercise augmentation of cognitive behavioural therapy for the treatment of suicidal ideation and depression. J Affect Disord. 2017;219:58-63. PubMed CrossRef
31.Buttner MM. Efficacy of yoga for depressed postpartum women: A randomized controlled trial [dissertation]. Iowa City, Iowa; University of Iowa: 2013.
32.Daley AJ, Blamey RV, Jolly K, et al. A pragmatic randomized controlled trial to evaluate the effectiveness of a facilitated exercise intervention as a treatment for postnatal depression: the PAM-PeRS trial. Psychol Med. 2015;45(11):2413-2425. PubMed CrossRef
33.Danielsson L, Papoulias I, Petersson EL, et al. Exercise or basic body awareness therapy as add-on treatment for major depression: a controlled study. J Affect Disord. 2014;168:98-106. PubMed CrossRef
34.Doose M, Ziegenbein M, Hoos O, et al. Self-selected intensity exercise in the treatment of major depression: a pragmatic RCT. Int J Psychiatry Clin Pract. 2015;19(4):266-275. PubMed CrossRef
35.Hallgren M, Helgadóttir B, Herring MP, et al. Exercise and internet-based cognitive-behavioural therapy for depression: multicentre randomised controlled trial with 12-month follow-up. Br J Psychiatry. 2016;209(5):414-420. PubMed CrossRef
36.Krogh J, Videbech P, Thomsen C, et al. DEMO-II trial: aerobic exercise versus stretching exercise in patients with major depression—a randomised clinical trial. PLoS One. 2012;7(10):e48316. PubMed CrossRef
37.Lavretsky H, Alstein LL, Olmstead RE, et al. Complementary use of tai chi chih augments escitalopram treatment of geriatric depression: a randomized controlled trial. Am J Geriatr Psychiatry. 2011;19(10):839-850. PubMed CrossRef
38.Moraes HS, Silveira HS, Oliveira NA, et al. Is strength training as effective as aerobic training for depression in older adults? a randomized controlled trial. Neuropsychobiology. 2020;79(2):141-149. PubMed CrossRef
39.Mota-Pereira J, Silverio J, Carvalho S, et al. Moderate exercise improves depression parameters in treatment-resistant patients with major depressive disorder. J Psychiatr Res. 2011;45(8):1005-1011. PubMed CrossRef
40.Pilu A, Sorba M, Hardoy MC, et al. Efficacy of physical activity in the adjunctive treatment of major depressive disorders: preliminary results. Clin Pract Epidemol Ment Health. 2007;3(1):8. PubMed CrossRef
41.Prathikanti S, Rivera R, Cochran A, et al. Treating major depression with yoga: a prospective, randomized, controlled pilot trial. PLoS One. 2017;12(3):e0173869. PubMed CrossRef
42.Sharma A, Barrett MS, Cucchiara AJ, et al. A breathing-based meditation intervention for patients with major depressive disorder following inadequate response to antidepressants: a randomized pilot study. J Clin Psychiatry. 2017;78(1):e59-e63. PubMed CrossRef
43.Sharma VK, Das S, Mondal S, et al. Effect of Sahaj Yoga on depressive disorders. Indian J Physiol Pharmacol. 2005;49(4):462-468. PubMed
44.Singh NA, Clements KM, Fiatarone MA. A randomized controlled trial of progressive resistance training in depressed elders. J Gerontol A Biol Sci Med Sci. 1997;52(1):M27-M35. PubMed CrossRef
45.Streeter CC, Gerbarg PL, Whitfield TH, et al. Treatment of major depressive disorder with iyengar yoga and coherent breathing: a randomized controlled dosing study. J Altern Complement Med. 2017;23(3):201-207. PubMed CrossRef
46.Szuhany KL, Otto MW. Efficacy evaluation of exercise as an augmentation strategy to brief behavioral activation treatment for depression: a randomized pilot trial. Cogn Behav Ther. 2020;49(3):228-241. PubMed CrossRef
47.Tolahunase MR, Sagar R, Faiq M, et al. Yoga- and meditation-based lifestyle intervention increases neuroplasticity and reduces severity of major depressive disorder: a randomized controlled trial. Restor Neurol Neurosci. 2018;36(3):423-442. PubMed
48.Uebelacker LA, Tremont G, Gillette LT, et al. Adjunctive yoga v. health education for persistent major depression: a randomized controlled trial. Psychol Med. 2017;47(12):2130-2142. PubMed CrossRef
49.Yeung A, Lepoutre V, Wayne P, et al. Tai chi treatment for depression in Chinese Americans: a pilot study. Am J Phys Med Rehabil. 2012;91(10):863-870. PubMed CrossRef
50.Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. PubMed CrossRef
51.Beck A, Steer R, Brown G. Manual for the Beck Depression Inventory-II. San Antonio, TX: Psychological Corporation; 1996.
52.Cohen J. A power primer. Psychol Bull. 1992;112(1):155-159. PubMed CrossRef
This PDF is free for all visitors!