Diagnosing and Managing Violence
Available categorization systems for violence encountered in medical practice do not constitute optimal tools to guide management. In this article, 4 common patterns of violence across psychiatric diagnoses are described (defensive, dominance-defining, impulsive, and calculated) and management implications are considered. The phenomenologic and neurobiological rationale for a clinical classification system of violence is also presented.
Prim Care Companion CNS Disord 2011;13(5):doi:10.4088/PCC.11br01144
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: January 19, 2011; accepted March 16, 2011.
Published online: October 6, 2011.
Corresponding author: Jeffrey C. Fetter, MD, Concord Hospital, 250 Pleasant St, Concord, NH 03301 ([email protected]).
Violence against other individuals is a common indication for emergency psychiatric evaluation. Medical and psychiatric training provides physicians with skills to assess and treat violence in the context of specific psychiatric disorders but does not generally present a comprehensive, practical approach to assessing and managing violence itself. The medical literature presents no consensus on defining types of violence.1-3
Medical and psychiatric physicians provide care for patients in hospitals, prisons, emergency rooms, group homes, schools, and other facilities where violence occurs. This article will describe common patterns of violence across psychiatric diagnoses and consider management implications.
TYPES OF VIOLENCE
Defensive Violence
Description. Defensive violence occurs when a person perceives a real or imagined threat and acts to defend self or others, perhaps preemptively.4 The person often describes a sense of inability to escape or of being outnumbered. Defensive violence involves gross motor movements in a state of elevated sympathetic tone, and accompanying verbalizations tend to be more accusatory than derisive. Attempts to ward off the threat may involve not only punching and kicking but also defensive behaviors not commonly associated with other types of violence such as scratching, biting, and screaming. The subject’s goal is survival, so the risk of assault remits as the perceived threat subsides.4 Defensive violence has 4 key features: (1) stimulates sympathetic activation, (2) lacks cortical involvement, (3) can be displaced to other targets, and (4) is designed to reduce environmental threat.5 Defensive behavior is associated specifically with the medial hypothalamus or the dorsolateral periaqueductal gray.5
Psychosis may trigger or worsen a defensively violent situation by impairing patients’ ability to accurately judge the level of threat to themselves or the motivations of people around them. Such situations often occur in response to staff members’ attempts to induce these patients to conform to rules of the facility or to take unwanted prescribed medications. Delusions of persecution, a history of having taken concrete steps of preparing to defend oneself on the basis of a delusion, command hallucinations, previous history of violence, and high ward turmoil are particularly indicative of the risk for violence in psychotic inpatients.6
The acute defensive behavior described here does not refer to a psychotic patient engaged in well-planned and precisely targeted preemptive violence, such as that of a delusional patient plotting to murder the object of his/her paranoia. A planned preemptive assault may be better described by the information presented here in the section on calculated violence, although this type of assault is based on delusional beliefs.
Management. The clinical management of acute defensive violence consists of reducing the perceived level of threat. Removal of an actual threat (eg, separating 2 contentious patients physically) may be necessary. Giving the patient the sense that he or she has an ally is another crucial intervention, often best accomplished by establishing some shared goal with the patient, emphasizing that the staff will work toward it, and planning for a follow-up meeting with the patient as to whether it could be accomplished.
Pharmacologic management of acute defensive violence often includes antipsychotic medications.7-10 The use of benzodiazepines, selective serotonin reuptake inhibitors, and tricyclic antidepressants for defensive aggression shows mixed results.11-15 Long-term violence risk in psychotically violent patients is associated with medication nonadherence, substance abuse, and residual symptoms.16 Long-acting depot antipsychotics and clozapine may be considered in these patients.17
Dominance-Defining Violence
Description. Dominance-defining violence occurs most often within members of a self-identified group (eg, prison inmates or sports teams) but can occur whenever aggressive individuals are in competition for status within a hierarchy.
As described in male prison inmates, confrontations precipitated by dominance-defining violence often follow a distinctive pattern:
(1) Derisive comments and threats
(2) Closing the distance between individuals
(3) Light contact (finger or light push)
(4) Right cross punch
(5) Wrestling.
The goal is to dominate or control the challenger in order to establish or maintain a power relationship, thus the participants do not attempt to leave or escape until one loses the encounter.18
Gang membership is a risk factor for dominance violence. Members may attack patients or prisoners of rival gangs or if members of their own gang are present may attack otherwise unaffiliated individuals to garnish their reputation.18 It is useful for physicians to observe for tattoos, clothing, or other local gang signifiers.
Management. While it is difficult for the participants to abort, a person familiar with the dominance-defining pattern can choose to act in a fashion incongruous to it and effectively avoid the onset of violence. For example, if a patient begins the pattern by verbal derision and then starts to close the distance between individuals, the clinician must avoid progressing to light touch and assume a comfortable distance from the patient while standing at an angle to derail the close contact stage.
Dominance behaviors may be managed by minimizing the audience and by responding to challenges to staff authority calmly, with good eye contact and simple concrete redirection. Confident body language is needed to convey that the staff’s authority is not in any doubt.18 The vasopressin system has been implicated in dominance behavior,19 and it may be responsive to fluoxetine.12
Impulsive Violence
Description. Impulsive violence consists of rapid strikes with a minimal period of preceding agitation in the context of frustration or physical discomfort that the patient may not be able to describe verbally. These episodes usually involve punching and are more likely associated with destruction of property than other types of violence. Unlike dominance-defining violence, after these episodes the aggressor does not evince a sense that the relationship with the victim has significantly changed. Impulsive violence is associated with mania, personality disorders, and psychosis.20
Impulsive violence is associated with the convergence of 2 deficits: amygdala hyperreactivity20,21 and a loss of prefrontal inhibition in conjunction with serotonin deficiency.20,22-29
Management. Nonverbal patients may engage in violent or self-injurious behavior to communicate distress due to general medical conditions such as gastroesophageal reflux or dental problems. A thorough search for correctible discomfort is warranted.
Behavioral plans with an emphasis on positive reinforcement of adaptive behavior and extinguishing self-defeating or dangerous behavior may be useful, especially for patients with mental retardation and autism. Direct care staff may also use principles of the collaborative problem-solving approach to prevent impulsive violence, in both children and adults, regardless of psychiatric diagnosis.30
There are a number of pharmacologic strategies to address impulsive violence. Impulsivity arising primarily from amygdala hyperreactivity may respond to mood stabilizers that modulate the γ-aminobutyric acid/glutamate system, particularly in patients with borderline personality disorder.31 Frontal lobe inhibition deficits may respond to selective serotonin reuptake inhibitors,20 stimulants, or atomoxetine.32 Second-generation antipsychotic trials for treatment of impulsive violence have yielded mixed results.33,34
Calculated Violence
Description. Calculated violence consists of premeditated aggressive acts designed to obtain a resource.18 The specific behaviors rely largely on cortical mechanisms and as such are varied and goal-directed. For example, a prisoner intimidating another to obtain cigarettes uses force for a rational goal. This type of violence may be associated with antisocial personality disorder. Although sometimes termed instrumental violence, the term calculated may be preferred because it excludes acute defensive violence more clearly and emphasizes its cortical origin.
People may engage in calculated violence to maintain a social position,35 but its reasoned application distinguishes it from dominance-defining violence. Individuals engaged in calculated violence, in contrast to other forms of violence, become more proficient over time and may use weapons fabricated or obtained in advance. Further distinguishing it from impulsive violence, calculated violence is associated with decreased amygdala activity,36 and pharmacologic agents are less effective.37 Some individuals may engage in calculated violence to obtain the pleasure of the violence itself rather than any concrete resources.
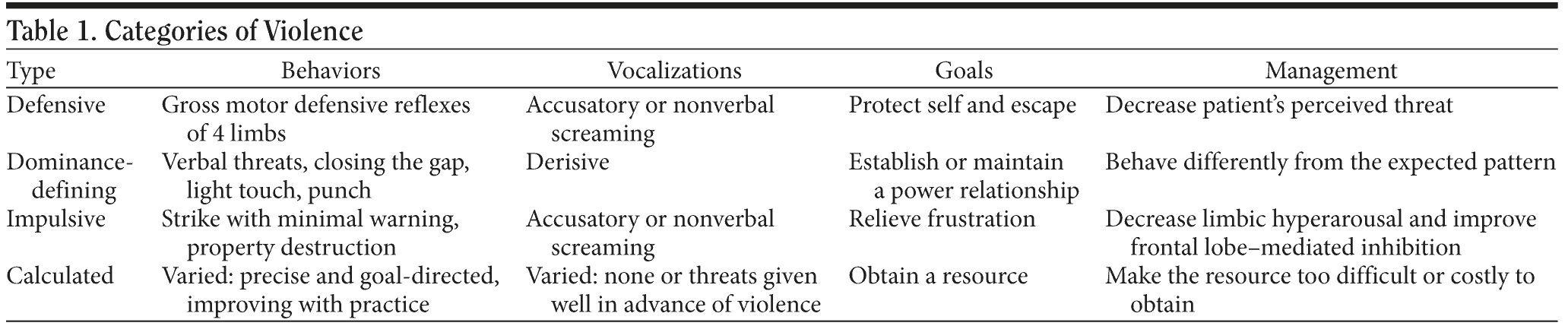
Management. To decrease the risk of calculated violence, it is necessary to make the resource too costly or difficult to acquire. Imposing a penalty (eg, invoking a plan to call the police if a behavior recurs) or increasing the effort required (eg, increasing the supervision of a perpetrator or the distance to the victim) may decrease these behaviors. While physical punishment tends to increase calculated violent behavior, making a socially appropriate substitute by acquiring available resources may decrease it.38 Table 1 provides a description of the categories of violence presented here.
Vignette 1
Mr A, a 23-year-old man with bipolar disorder (DSM-IV criteria), was admitted to the emergency department for threatening his mother by brandishing a golf club. He attempted to punch police officers in the emergency room, making grandiose statements about how people with bipolar disorder are more evolved than regular humans. Mr A arrived on the unit in restraints and upon release assaulted 2 nursing aides, severely injuring one.
He appeared frightened of staff and peers and was started on olanzapine and lithium, which improved his psychosis and grandiosity significantly. Once therapeutic doses of olanzapine were reached, Mr A no longer threatened staff without provocation. However, he continued to impulsively verbally challenge staff and posture aggressively when unit rules were enforced, later apologizing for his behavior. Valproic acid was started, and Mr A’s impulsive agitation reduced quickly upon reaching therapeutic levels. The defensive and impulsive aspects of his presentation responded to different medications.
Vignette 2
Mr B, a 30-year-old man with bipolar disorder and narcissistic personality disorder (DSM-IV criteria), was admitted by his guardian for bizarre behavior and medication noncompliance in violation of a court order. He engaged in aggressive exercise in other peers’ rooms and public areas of the unit and often bumped into staff, feigning that he did not notice them. Mr B was very muscular, and other patients feared him. His impulsiveness took the form of running around the unit and hitting walls without provocation.
To address the dominance behaviors, staff members were coached to meet Mr B’s gaze, deliver simple instructions in a neutral tone, and minimize the audience of behavioral disturbances. The psychiatrist underwent a period of rapport building by honoring a request for access to educational materials, as well as allowing Mr B some input into his medication regimen, with an aim of decreasing his defensive fear of staff. Mr B was prescribed valproic acid, which, above a level of 90 mg/dL, was effective in reducing his hyperkinetic behaviors. Mr B’s dominance-defining violence responded to staff training, while his impulsiveness required therapeutic valproic acid levels.
CONCLUSIONS
Clinicians may avoid common pitfalls in the management of violence by using the nosology described here. Behavior plans and psychopharmacology are the most common means of managing all types of violent behavior, but are less likely to be successful for patients displaying defensive violence. Hospitalization for impulsive violence may prompt treatment for Axis I or II disorders without specifically addressing the amygdala activity and prefrontal dyscontrol that leads to the most problematic behaviors. Defensive and impulsive episodes may prompt staff to gather in large numbers around a patient in a way that feeds a sense of being outnumbered or converts a brief impulsive episode into a prolonged defensive event. Any of the types of violence described may be inappropriately managed primarily by punitive measures best applied to calculated violence, perhaps as a result of staff countertransference.
Moreover, medical directors may find that identification of these categories of violence has implications for staffing and organizing inpatient services. For example, patients who display frequent impulsive violence may be better served on a unit that is structured for use of behavior plans. Patients displaying defensive violence may particularly benefit from a unit with “quiet rooms” to which to escape from the milieu.
These violence types cut across psychiatric diagnoses, such that many units that specialize in a single disorder, such as schizophrenia, may find a variety of these types of violence represented. Some institutions may find it useful to identify patients with dominance behaviors and keep them separated on different units.
It is important to recognize that this typology is limited by the fact that interpersonal violence is a complex phenomenon. Any individual’s pattern of violence and the cause of any specific act of aggression are likely to draw to some extent from more than 1 of the 4 types of violence presented here. For example, a patient who carefully plans the murder of an individual that he/she believes is plotting against him/her may be acting in a calculated way based on delusional beliefs of the need for defense.
This article does not present an exhaustive account of warfare, rape, predatory paraphilia, or many other varieties of violence. However, as the vignettes demonstrate, the 4 types of violence presented may serve as a framework for treatment planning in settings wherein physicians commonly manage violent patients.
Recognition of different patterns of violence has implications for management of both individual patients and the milieu. Careful observation of behavior around aggressive episodes can lead to improvements in management that may decrease staff and patient injuries, decrease length of stay, or permit progression to less restrictive settings.
Drug names: atomoxetine (Strattera), clozapine (Clozaril, FazaClo, and others), fluoxetine (Prozac and others), lithium (Lithobid and others), olanzapine (Zyprexa), valproic acid (Depakene, Stavzor, and others).
Author affiliations: Concord Hospital and Riverbend Community Mental Health Inc, Concord, New Hampshire.
Potential conflicts of interest: Dr Fetter has received honoraria from Eli Lily, Janssen, and Ortho-McNeil.
Funding/support: None reported.
REFERENCES
1. Reid WH, Thorne SA. Personality disorders. In: Simon RI, Tardiff K, eds. Textbook of Violence Assessment and Management. Arlington, VA: American Psychiatric Publishing; 2008:161-183.
2. World Health Organization. World Report on Violence and Health. Violence: a Global Public Health Problem. http://www.who.int/violence_injury_prevention/violence/world_report/en/chap1.pdf. Accessed August 4, 2011.
3. Moyer KE. Kinds of aggression and their physiological basis. Com Behav Biol. 1968:2(2):65-87.
4. Wall PM, Blanchard C, Blanchard RJ. Behavioral and neuropharmacological differentiation of offensive and defensive aggression in experimental and seminaturalistic models. In: Mattson M, ed. Neurobiology of Aggression: Understanding and Preventing Violence. Totowa, NJ: Humana; 2003:73-92.
5. Siegel A, Victoroff J. Understanding human aggression: new insights from neuroscience. Int J Law Psychiatry. 2009;32(4):209-215. PubMed doi:10.1016/j.ijlp.2009.06.001
6. Hamrin V, Iennaco J, Olsen D. A review of ecological factors affecting inpatient psychiatric unit violence: implications for relational and unit cultural improvements. Issues Ment Health Nurs. 2009;30(4):214-226. PubMed doi:10.1080/01612840802701083
7. Marder SR. A review of agitation in mental illness: treatment guidelines and current therapies. J Clin Psychiatry. 2006;67(suppl 10):13-21. PubMed
8. Lesem MD, Zajecka JM, Swift RH, et al. Intramuscular ziprasidone, 2 mg versus 10 mg, in the short-term management of agitated psychotic patients. J Clin Psychiatry. 2001;62(1):12-18. PubMed doi:10.4088/JCP.v62n0104
9. Meehan K, Zhang F, David S, et al. A double-blind, randomized comparison of the efficacy and safety of intramuscular injections of olanzapine, lorazepam, or placebo in treating acutely agitated patients diagnosed with bipolar mania. J Clin Psychopharmacol. 2001;21(4):389-397. PubMed doi:10.1097/00004714-20010800006
10. Zimbroff DL, Marcus RN, Manos G, et al. Management of acute agitation in patients with bipolar disorder: efficacy and safety of intramuscular aripiprazole. J Clin Psychopharmacol. 2007;27(2):171-176. PubMed doi:10.1097/JCP.0b13e318033bd5e
11. Palanza P, Rodgers RJ, Ferrari PF, et al. Effects of chlordiazepoxide on maternal aggression in mice depend on experience of resident and sex of intruder. Pharmacol Biochem Behav. 1996;54(1):175-182. PubMed doi:10.1016/0091-3057(95)02109-4
12. Ferris CF, Melloni RH Jr, Koppel G, et al. Vasopressin/serotonin interactions in the anterior hypothalamus control aggressive behavior in golden hamsters. J Neurosci. 1997;17(11):4331-4340. PubMed
13. Ho HP, Olsson M, Westberg L, et al. The serotonin reuptake inhibitor fluoxetine reduces sex steroid-related aggression in female rats: an animal model of premenstrual irritability? Neuropsychopharmacology. 2001;24(5):502-510. PubMed doi:10.1016/S0893-133X(00)00219-0
14. Villalba C, Boyle PA, Caliguri EJ, et al. Effects of the selective serotonin reuptake inhibitor fluoxetine on social behaviors in male and female prairie voles (Microtus ochrogaster). Horm Behav. 1997;32(3):184-191. PubMed doi:10.1006/hbeh.1997.1420
15. Griebel G, Blanchard DC, Agnes RS, et al. Differential modulation of antipredator defensive behavior in Swiss-Webster mice following acute or chronic administration of imipramine and fluoxetine. Psychopharmacology (Berl). 1995;120(1):57-66. PubMed doi:10.1007/BF02246145
16. Torrey EF, Stanley J, Monahan J, et al; MacArthur Study Group. The MacArthur Violence Risk Assessment Study revisited: two views ten years after its initial publication. Psychiatr Serv. 2008;59(2):147-152. PubMed doi:10.1176/appi.ps.59.2.147
17. Topiwala A, Fazel S. The pharmacological management of violence in schizophrenia: a structured review. Expert Rev Neurother. 2011;11(1):53-63. PubMed doi:10.1586/ern.10.180
18. Miller R. Meditations on Violence: A Comparison of Martial Arts Training and Real World Violence. Wolfboro, NH: YMAA Publication Center; 2008:42-47.
19. Stanley B, Siever LJ. The interpersonal dimension of borderline personality disorder: toward a neuropeptide model. Am J Psychiatry. 2010;167(1):24-39. PubMed doi:10.1176/appi.ajp.2009.09050744
20. Siever LJ. Neurobiology of aggression and violence. Am J Psychiatry. 2008;165(4):429-442. PubMed doi:10.1176/appi.ajp.2008.07111774
21. Hazlett EA, Speiser LJ, Goodman M, et al. Exaggerated affect-modulated startle during unpleasant stimuli in borderline personality disorder. Biol Psychiatry. 2007;62(3):250-255. PubMed doi:10.1016/j.biopsych.2006.10.028
22. New AS, Gelernter J, Yovell Y, et al. Tryptophan hydroxylase genotype is associated with impulsive-aggression measures: a preliminary study. Am J Med Genet. 1998;81(1):13-17. PubMed doi:10.1002/(SICI)1096-8628(19980207)81:1<13::AID-AJMG3>3.0.CO;2-O
23. Nielsen DA, Goldman D, Virkkunen M, et al. Suicidality and 5-hydroxyindoleacetic acid concentration associated with a tryptophan hydroxylase polymorphism. Arch Gen Psychiatry. 1994;51(1):34-38. PubMed
24. Hallikainen T, Saito T, Lachman HM, et al. Association between low activity serotonin transporter promoter genotype and early onset alcoholism with habitual impulsive violent behavior. Mol Psychiatry. 1999;4:385-388. PubMed doi:10.1038/sj.mp.4000526
25. Lappalainen J, Long JC, Eggert M, et al. Linkage of antisocial alcoholism to the serotonin 5-HT1B receptor gene in 2 populations. Arch Gen Psychiatry. 1998;55(11):989-994. PubMed doi:10.1001/archpsyc.55.11.989
26. Raine A, Meloy JR, Bihrle S, et al. Reduced prefrontal and increased subcortical brain functioning assessed using positron emission tomography in predatory and affective murderers. Behav Sci Law. 1998;16(3):319-332. PubMed doi:10.1002/(SICI)1099-0798(199822)16:3<319::AID-BSL311>3.0.CO;2-G
27. Gerra G, Zaimovic A, Avanzini P, et al. Neurotransmitter-neuroendocrine responses to experimentally induced aggression in humans: influence of personality variable. Psychiatry Res. 1997;66(1):33-43. PubMed doi:10.1016/S0165-1781(96)02965-4
28. Strous RD, Bark N, Parsia SS, et al. Analysis of a functional catechol-O-methyltransferase gene polymorphism in schizophrenia: evidence for association with aggressive and antisocial behavior. Psychiatry Res. 1997;69(2-3):71-77. PubMed doi:10.1016/S0165-1781(96)03111-3
29. Haspel T. Beta-blockers and the treatment of aggression. Harv Rev Psychiatry. 1995;2(5):274-281. PubMed doi:10.3109/10673229509017146
30. Green RW, Albon JS. Treating Explosive Kids: The Collaborative Problem-Solving Approach. New York, NY: Guilford; 2006.
31. Hollander E, Tracy KA, Swann AC, et al. Divalproex in the treatment of impulsive aggression: efficacy in cluster B personality disorders. Neuropsychopharmacology. 2003;28(6):1186-1197. PubMed
32. Dopheide JA, Pliszka SR. Attention-deficit-hyperactivity disorder: an update. Pharmacotherapy. 2009;29(6):656-679. PubMed doi:10.1592/phco.29.6.656
33. Amitai N, Markou A. Increased impulsivity and disrupted attention induced by repeated phencyclidine are not attenuated by chronic quetiapine treatment. Pharmacol Biochem Behav. 2009;93(3):248-257. PubMed doi:10.1016/j.pbb.2008.08.025
34. Amitai N, Semenova S, Markou A. Clozapine attenuates disruptions in response inhibition and task efficiency induced by repeated phencyclidine administration in the intracranial self-stimulation procedure. Eur J Pharmacol. 2009;602(1):78-84. PubMed doi:10.1016/j.ejphar.2008.11.001
35. Canada G. Fist Stick Knife Gun. Boston, MA: Beacon Press: 1995;49-50.
36. Kiehl KA, Smith AM, Hare RD, et al. Limbic abnormalities in affective processing by criminal psychopaths as revealed by functional magnetic resonance imaging. Biol Psychiatry. 2001;50(9):677-684. PubMed doi:10.1016/S0006-3223(01)01222-7
37. Connor DF, Carlson GA, Chang KD, et al; Stanford/Howard/AACAP Workgroup on Juvenile Impulsivity and Aggression. Juvenile maladaptive aggression: a review of prevention, treatment, and service configuration and a proposed research agenda. J Clin Psychiatry. 2006;67(5):808-820. PubMed doi:10.4088/JCP.v67n0516
38. Rachlin H. The behavioral economics of violence. Ann N Y Acad Sci. 2004;1036(1):325-335. PubMed doi:10.1196/annals.1330.020