Objective: Metabolic syndrome is a common underdiagnosed condition among psychiatric patients exacerbated by second-generation antipsychotics, with the exception of aripiprazole and ziprasidone. This study evaluated the prescribing and treating behavior with regard to antipsychotics and metabolic syndrome of psychiatrists before and after implementation of a mandatory admission order set and electronic notification of results.
Method: Baseline data from 9,100 consecutive psychiatric admissions to a mental health hospital (July 2013-July 2014) were compared to postintervention data (July 2014-January 2015), which included 1,499 consecutive patient records. The intervention initiated standardized admission testing with electronic notification to psychiatrists when patients met metabolic syndrome criteria (according to Axis III of the DSM-IV). Charts were examined for inclusion of this diagnosis at discharge and for treatment changes.
Results: At baseline, only 2.4% of patients (n = 214) were evaluated for metabolic syndrome. Of these, 34.5% (0.8% of the total sample) met metabolic syndrome criteria. Only 15 patients (0.16%) were comprehensively treated. No chart listed metabolic syndrome under Axis III of the DSM-IV. After the intervention, the diagnosis of patients meeting the criteria for metabolic syndrome increased from 0% to 29.3%. Less than 3% of patients were switched to drugs with a more benign metabolic profile. All patients who continued on second-generation antipsychotics had metabolic retesting. Thirty-eight experienced a significant and rapid increase in triglyceride levels after only 3 to 17 days.
Conclusions: Mandatory intake testing increases the number of patients evaluated for metabolic syndrome. Electronic alerts increase the inclusion of metabolic syndrome among discharge diagnoses but rarely affect prescribing practices.
Is Metabolic Syndrome On the Radar?
Improving Real-Time Detection of Metabolic Syndrome
and Physician Response by Computerized Scan of the
Electronic Medical Record
ABSTRACT
Objective: Metabolic syndrome is a common underdiagnosed condition among psychiatric patients exacerbated by second-generation antipsychotics, with the exception of aripiprazole and ziprasidone. This study evaluated the prescribing and treating behavior with regard to antipsychotics and metabolic syndrome of psychiatrists before and after implementation of a mandatory admission order set and electronic notification of results.
Method: Baseline data from 9,100 consecutive psychiatric admissions to a mental health hospital (July 2013–July 2014) were compared to postintervention data (July 2014–January 2015), which included 1,499 consecutive patient records. The intervention initiated standardized admission testing with electronic notification to psychiatrists when patients met metabolic syndrome criteria (according to Axis III of the DSM-IV). Charts were examined for inclusion of this diagnosis at discharge and for treatment changes.
Results: At baseline, only 2.4% of patients (n = 214) were evaluated for metabolic syndrome. Of these, 34.5% (0.8% of the total sample) met metabolic syndrome criteria. Only 15 patients (0.16%) were comprehensively treated. No chart listed metabolic syndrome under Axis III of the DSM-IV. After the intervention, the diagnosis of patients meeting the criteria for metabolic syndrome increased from 0% to 29.3%. Less than 3% of patients were switched to drugs with a more benign metabolic profile. All patients who continued on second-generation antipsychotics had metabolic retesting. Thirty-eight experienced a significant and rapid increase in triglyceride levels after only 3 to 17 days.
Conclusions: Mandatory intake testing increases the number of patients evaluated for metabolic syndrome. Electronic alerts increase the inclusion of metabolic syndrome among discharge diagnoses but rarely affect prescribing practices.
Prim Care Companion CNS Disord 2016;18(1):doi:10.4088/PCC.15m01849
© Copyright 2016 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, bDepartment of Emergency Medicine, cStatistical and Research Consultant, Kaweah Delta Health Care District, Visalia, California
*Corresponding author: Joachim Raese, MD, Department of Psychiatry, Kaweah Delta Health Care District, 400 W Mineral King Ave, Visalia, CA 93291 ([email protected]).
Mental illness is associated with an increased relative risk of mortality of 2.2 or 10 years of life lost.1 This excess mortality is multifactorial including the disorganizing effects of the mental illness, unaddressed side effects of treatment, and concomitant physical illnesses (often inadequately treated). Psychiatric patients have reduced life spans, more medical diseases, and more frequent contact with the health care system than non–mentally ill people. Common but rarely addressed problems among the mentally ill are obesity, hypertension, dyslipidemia, and glucose abnormalities.2 One might expect the mentally ill to receive more regular medical monitoring and treatment.3 Unfortunately, patients with psychiatric disorders receive lower quality medical care.4 Metabolic syndrome contributes heavily to this excess morbidity.
Metabolic syndrome is an energy utilization disorder characterized by increased waist circumference, elevated fasting glucose triglyceride levels, reduced high-density lipoprotein (HDL) levels, and elevated blood pressure. Metabolic syndrome is diagnosed when 3 or more criteria are present.5 Metabolic syndrome itself is associated with cognitive decline in adolescents and adults6 and accelerated decline in the elderly.7 One hypothesized mechanism is arteriosclerotic brain damage from untreated hypertension8; another is the microvascular inflammation caused by excess serum glucose.9
The increased risk of metabolic syndrome in the severely mentally ill is multifactorial.10,11 Obesity is 1.5 to 2 times higher among the mentally ill than the general population.12 Dyslipidemia, hypertension, and diabetes also are common.12 Mental disorders may have a bidirectional relationship with metabolic syndrome.13 Obesity is a risk factor for depression.14 Schizophrenia reduces life expectancy by 20%15,16 and is associated with a 43% prevalence of metabolic syndrome.17 Early onset of metabolic syndrome is associated with first-episode schizophrenia spectrum disorders, suggesting a direct relationship.18 Patients with bipolar disorder have a mean metabolic syndrome prevalence of 37.3%.3 Patients who develop metabolic syndrome double their 10-year cardiovascular disease risk,19 primarily because of an increase in cardiovascular disease.20
Patients treated with second-generation antipsychotics (SGAs) rarely receive complete laboratory workups,21–23 and when such tests are done, the results rarely change therapy.24 Therefore, increased attention to metabolic screening for hospitalized psychiatric patients is a pending quality of care measure .25,26 Unfortunately, treatment for mental illness also may increase metabolic syndrome risk. Although SGAs may have fewer extrapyramidal effects,27 they have a metabolic cost. Clozapine and olanzapine directly impair glucose metabolism and induce insulin resistance compared with risperidone28 and are associated with diabetes.29 Clozapine and olanzapine are associated with significant weight gain. Olanzapine was discontinued due to excessive weight gain twice as often as other antipsychotics in the Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) trial.27 Quetiapine and risperidone have less effect on weight. Aripiprazole and ziprasidone cause the least weight gain.30 The chance of SGA-induced weight gain appears to be polygenetic.31,32
METHOD
Ethics Review
The institutional review board of Kaweah Delta Health Care District (Visalia, California) approved this study. Study participants were inpatients of Kaweah Delta Mental Health Hospital. Because all data were deidentified before analysis and reported in aggregate, the institutional review board determined that no individual consent was required.
Design Summary
This was an observational study of the effects of a natural experiment on the prescribing and treating behavior of psychiatrists before and after implementation of a mandatory admission order set and electronic notification of results.
Criteria for Metabolic Syndrome
- Body mass index (BMI) was used as a criterion for diagnosis of metabolic syndrome until November 2014, when waist circumference was added to the intake procedure. Thereafter, a waist circumference > 88 cm for women and > 102 cm for men was used instead when available.33,34
- Hypertension: systolic blood pressure > 130 mm HG and diastolic blood pressure > 85 mm Hg.
- BMI > 25 kg/m2.
- Fasting glucose > 110 mg/dL.
- Hyperlipidemia with either fasting HDL < 40 mg/dL (< 50 mg/dL in females) or fasting triglycerides > 150 mg/dL.
Population
Electronic medical records (EMRs) of mental health admissions were reviewed. Baseline data from 9,100 consecutive psychiatric admissions (July 2013–July 2014) were compared to postintervention data (July 2014–January 2015), which included 1,499 consecutive patient records.
Interventions
In response to a pending federal quality of care requirement, in July 2014 a mandatory admission order set was changed to include fasting glucose, triglyceride, and HDL levels; BMI; and a complete set of vital signs, which included weight and, later, waist circumference. A computer algorithm that scanned the EMR for metabolic syndrome criteria was implemented. The algorithm sent a secure, personal e-mail within 24 hours of admission to the treating psychiatrist. The e-mail included the supporting data and an advisory to include the diagnosis under Axis III of the DSM-IV in both the progress note and discharge summary and suggested that appropriate interventions for metabolic syndrome might include switching to a different antipsychotic, treatment with a antihypertensive, or treatment with lipid or glucose-lowering drugs. The algorithm also added a new progress note template to the EMR that required the psychiatrist to respond and acknowledge the presence of metabolic syndrome and describe planned interventions. For patients who continued to receive the SGAs clozapine, risperidone, olanzapine, and quetiapine after the diagnosis of metabolic syndrome, a second lipid panel and glucose level were obtained after 3 to 17 days to monitor acute changes in these metabolic indices. Aripiprazole and ziprasidone were not included in the list of SGAs that triggered the additional tests because they do not carry significant increased metabolic risk.31,35,36
Data Collection
The automated algorithm was used to detect criteria of metabolic syndrome in the EMRs. The algorithm extracted patient age, gender, blood pressure, BMI, glucose, HDLs, triglycerides, and waist circumference. Admission diagnoses were extracted and categorized as psychotic disorder, bipolar disorder, depressive disorder, or other diagnoses. Use of the SGAs clozapine, olanzapine, risperidone, and quetiapine was noted. When laboratory and biometric criteria for metabolic syndrome were met, the algorithm searched for metabolic syndrome in the discharge summary. It also searched for changes made to patient therapy.
Calculated Variables
Diagnosis (per DSM-IV criteria) was grouped into 4 categories: psychotic disorders (psychotic disorder not otherwise specified, schizophrenia, and schizoaffective disorder), depressive disorders (major depressive disorder and depressive disorder not otherwise specified), bipolar disorder, and adjustment/mood disorder not otherwise specified.
Patients were stratified by number of metabolic syndrome criteria met (3–5). The triglyceride/HDL ratio was calculated because higher ratios are associated with increased risk of coronary artery disease.36 Completeness of treatment of the components of metabolic syndrome was scored as 1 = no treatment, 2 = partial treatment, and 3 = complete treatment (all components of metabolic syndrome were addressed).
Medications were recorded by category: antihypertensive, lipid-lowering agents, and hypoglycemic agents. Discharge summaries were for metabolic syndrome in Axis III of the DSM-IV.
RESULTS
Baseline
Prior to initiating the enhanced admission order set, 9,100 consecutive charts were evaluated. Most patients (97.6% or 8,886/9,100) did not have the complete recommended admission orders. Of the 214 patients who did, 34.5% (74/214) met metabolic syndrome criteria, consistent with the literature. Only 15 patients (20.0% of patients meeting criteria for metabolic syndrome) were comprehensively treated. Another 50.0% of the 74 patients were partially treated, while 30.0% received no treatment. At baseline, no patient had metabolic syndrome recorded under Axis III of the DSM-IV.
Postintervention
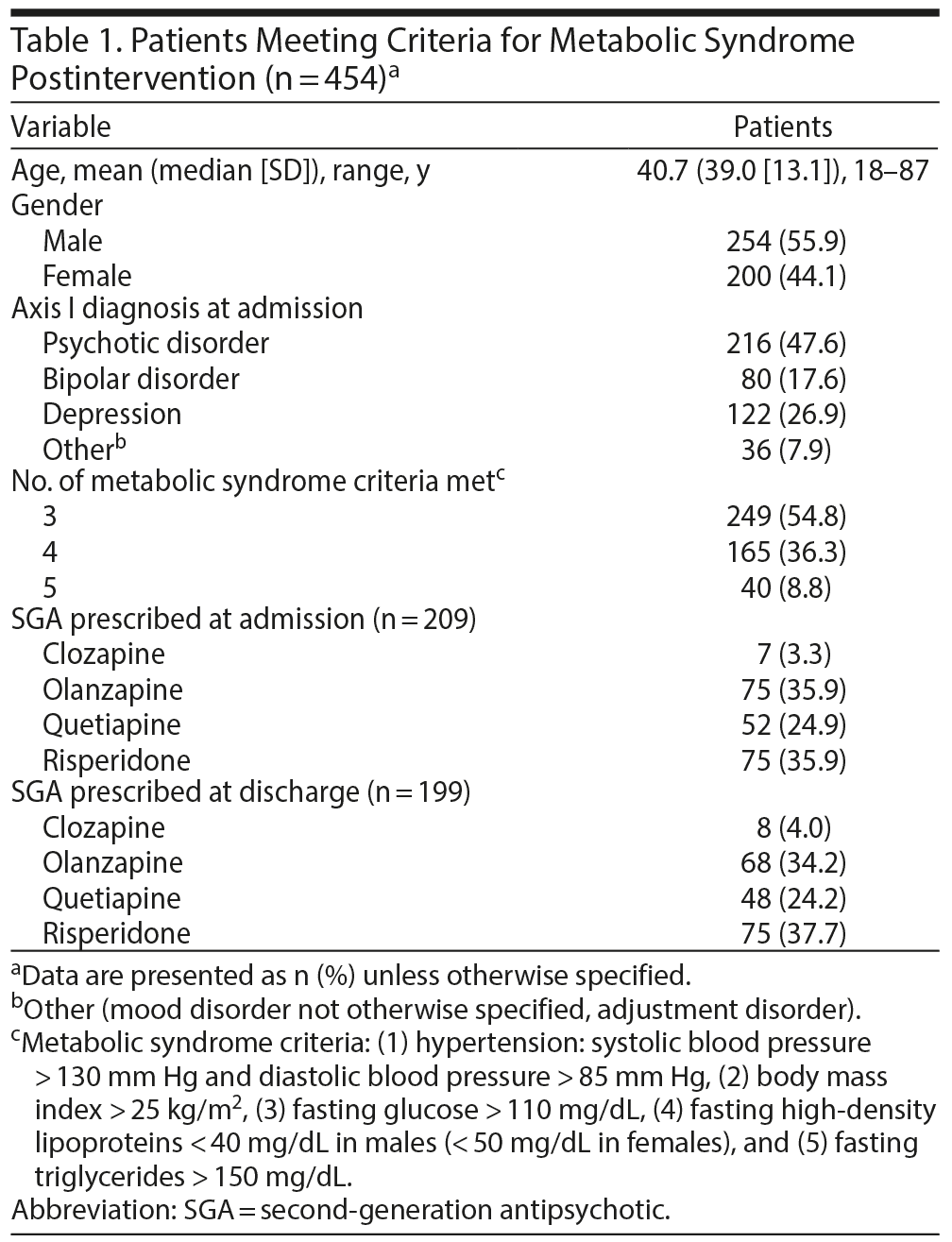
Of 1,499 consecutively admitted patients, 454 were diagnosed with metabolic syndrome (Table 1). Among metabolic syndrome patients, psychotic disorders accounted for the largest group with 47.6% (216/454). Depressive disorder was next with 26.9% (122/454), followed by bipolar disorder with 17.6% (80/454) and adjustment/mood disorder not otherwise specified with 7.9% (36/454). Almost half (54.8%, 249/454) of metabolic syndrome patients met 3 criteria for metabolic syndrome, 36.3% (165/454) met 4 criteria, and 8.8% (40/454) met 5 criteria. This finding is similar to other mental health populations in the literature.
Three measures of intervention effectiveness were used.
- Documentation of metabolic syndrome under Axis III of the DSM-IV discharge summary, which improved significantly from 0% to 29.3%.
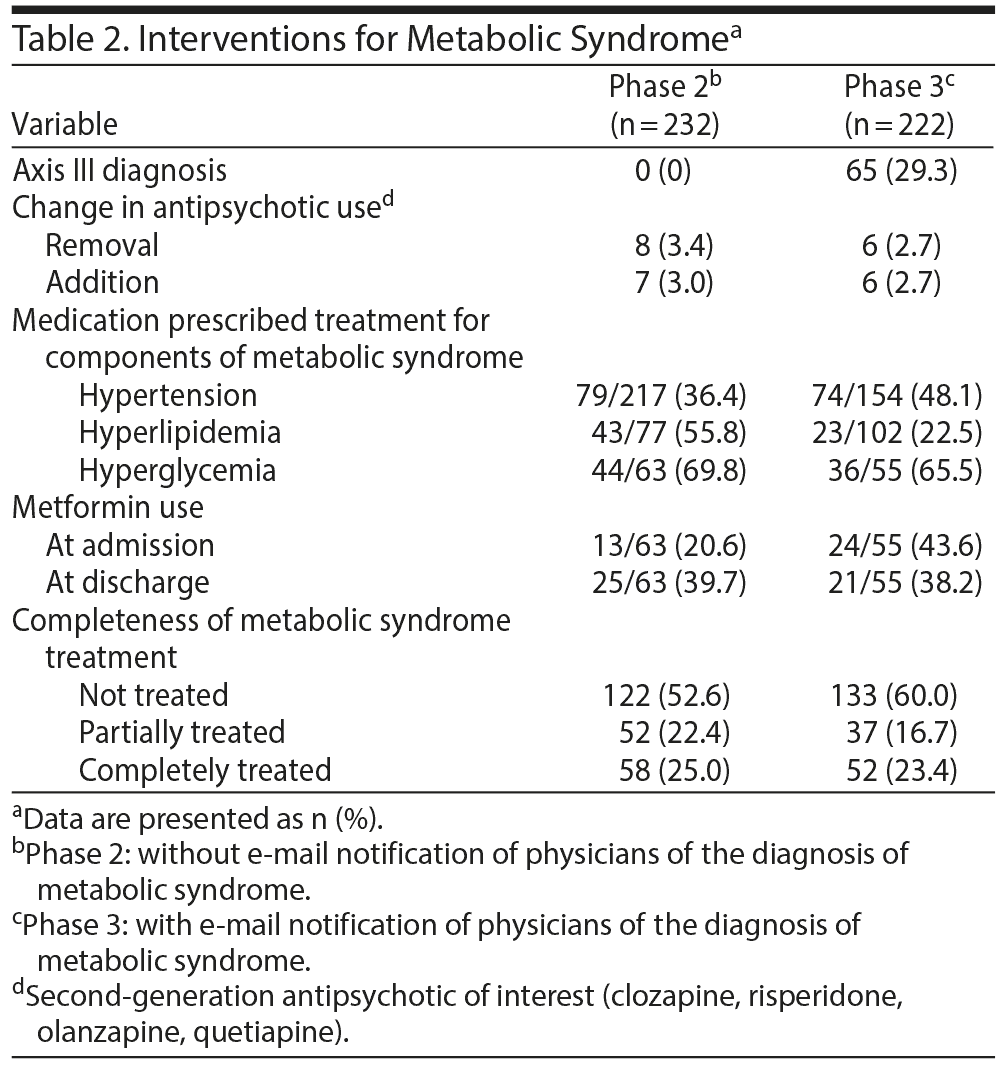
- Prescription of SGAs from admission to discharge, which showed little change (Table 1). At admission, 35.9% of patients were prescribed olanzapine compared to 34.2% at discharge. Risperidone was the initial drug of choice for 35.9% at admission compared to 37.7% at discharge. Quetiapine accounted for 24.9% at admission and 24.2% at discharge. Psychiatrists did not switch patients with metabolic syndrome to drugs with a more benign metabolic profile. Despite e-mail alerts, 2.7% (6/222) of patients received a new prescription for an SGA (Table 2).
- Comprehensiveness of treatment for the components of metabolic syndrome, which failed to improve (Table 2). Most noticeably, the percentage of patients with metabolic syndrome who did not receive any medication treatment did not change (52.6% prior to the use of e-mail notifications and 60.0% after the implementation of e-mail alerts). Prescriptions for metformin did not increase after e-mail notifications to psychiatrists alerting them to the diagnosis of metabolic syndrome (Table 2).
Effects of Continued SGAs on Patients
Fasting lipid and glucose serum levels were automatically reordered for subjects with metabolic syndrome who continued to receive SGAs. Of these, 38 patients experienced a rapid increase in triglycerides after only 3 to 17 days. The magnitude of the triglyceride increase of 3 patients is of particular interest (Figure 1 and Table 3). Two patients prescribed olanzapine at admission exhibited a 3-fold increase in triglycerides, while 1 patient had a nearly 15-fold increase in triglycerides after 9 days of taking olanzapine.
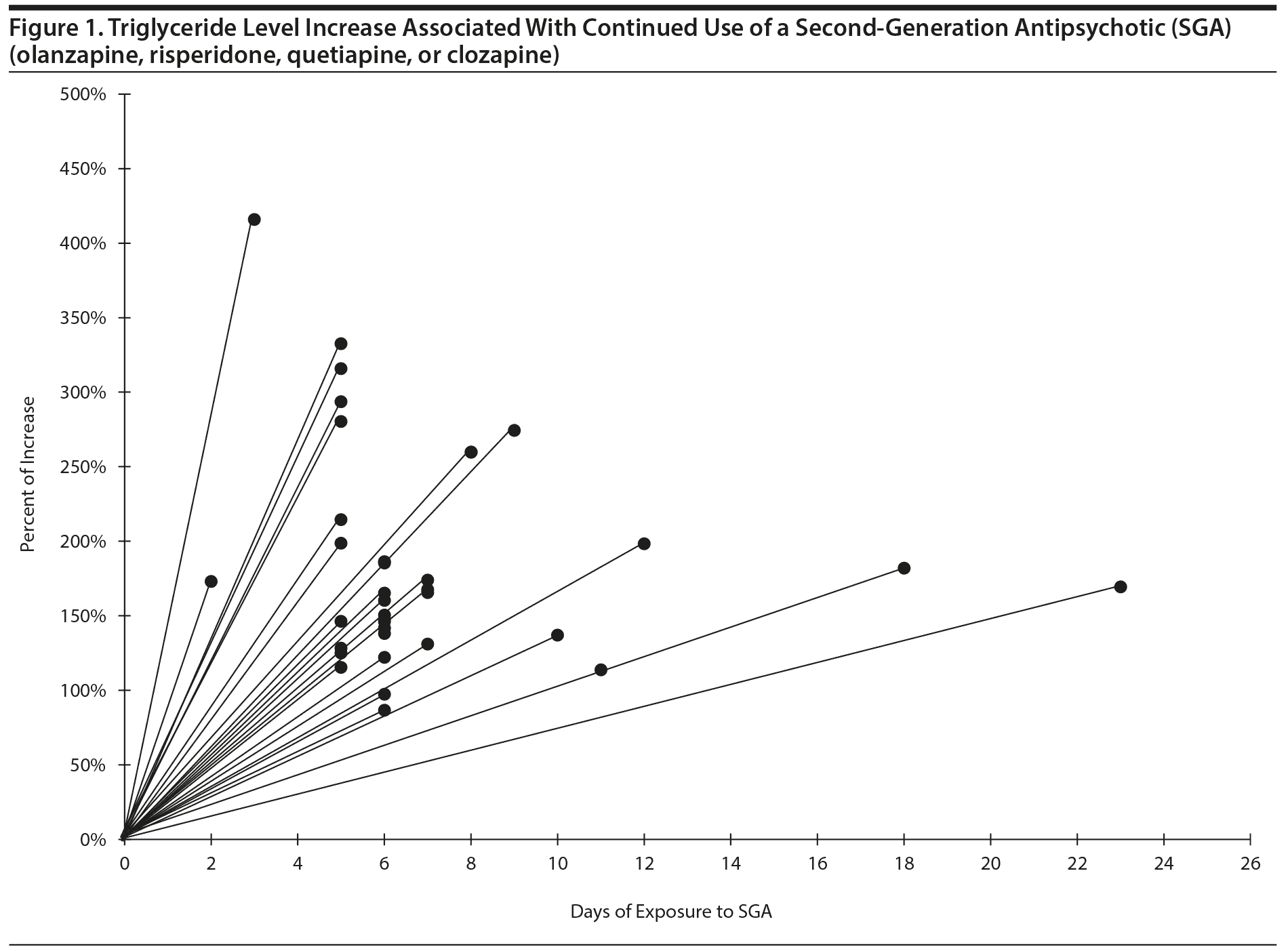
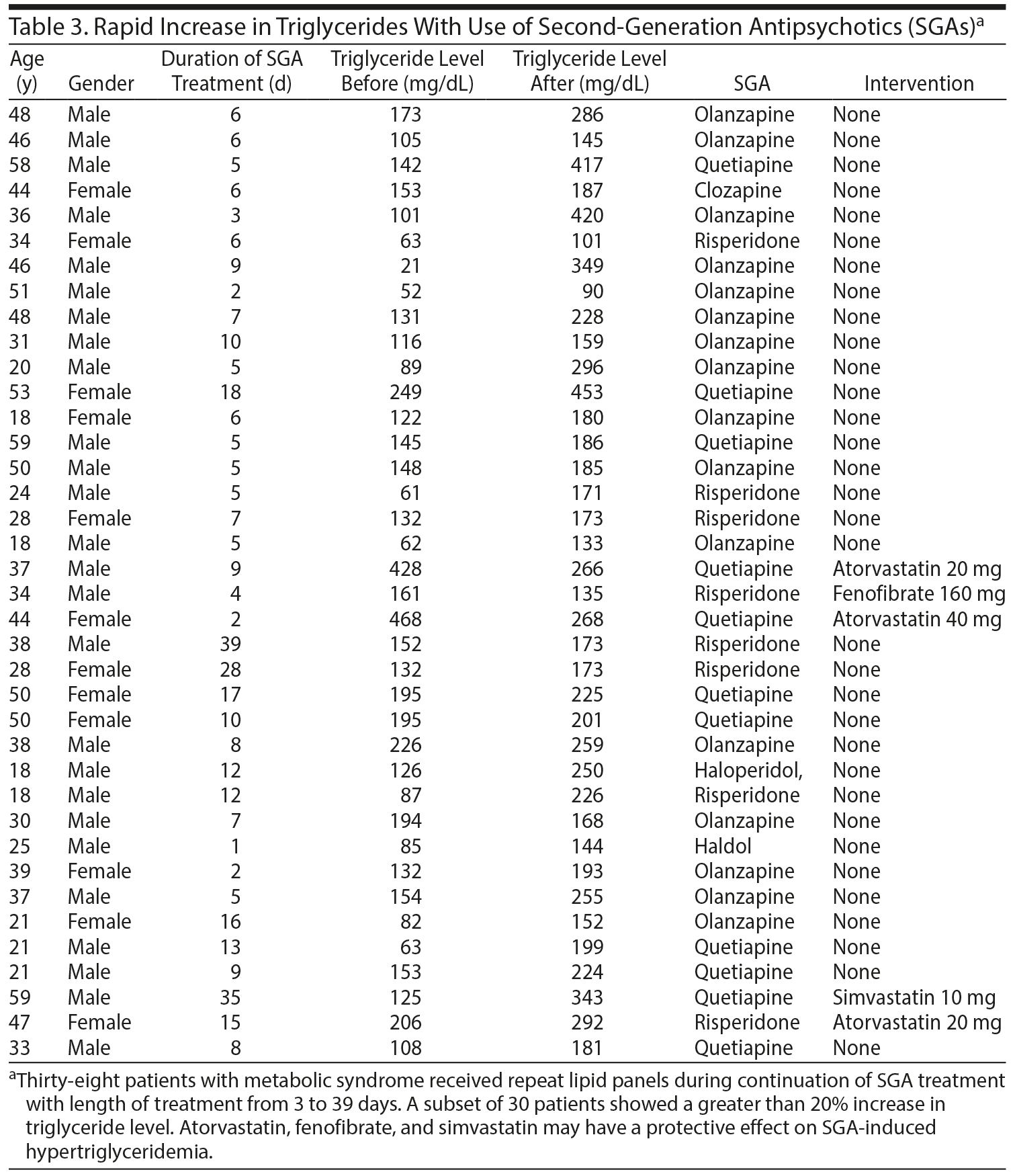
In 2 of these 3 patients, atorvastatin appeared to attenuate this effect. One patient taking olanzapine showed a decrease of triglyceride level from 468 mg/dL to 268 mg/dL after the addition of atorvastatin 40 mg. A second patient who received quetiapine had a decrease in triglyceride level from 428 mg/dL to 266 mg/dL within 9 days after starting atorvastatin 20 mg.
These responses suggest that some patients have an increased vulnerability to the metabolic effects of SGAs. A single nucleotide polymorphism near the melanocortin 4 receptor gene (MC4R) has been linked in a recessive fashion (P = 5.59 × 10–12) to rapid excessive weight gain, increased body fat, and triglyceride levels in pediatric patients undergoing first exposure to SGAs.38
Severity of Metabolic Syndrome by
Psychiatric Diagnosis
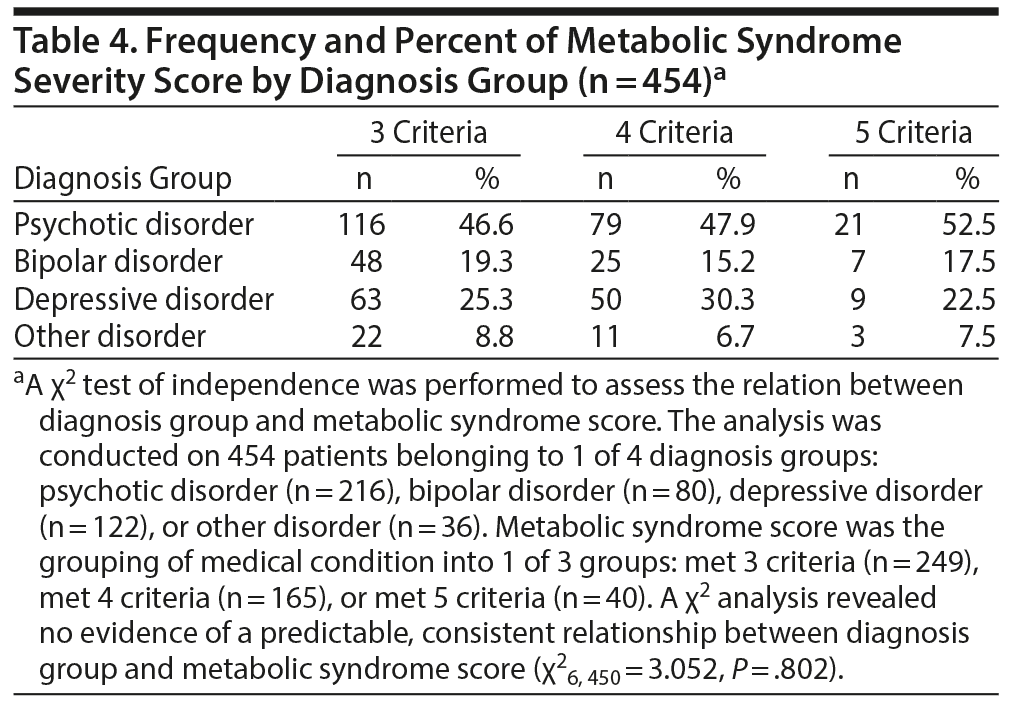
The patients (n = 454) were divided into 4 diagnostic groups: psychotic disorder (n = 216), bipolar disorder (n = 80), depressive disorder (n = 122), or other (n = 36). Number of metabolic syndrome criteria met produced 3 groups: met 3 criteria (n = 249), met 4 criteria (n = 165), or met 5 criteria (n = 40). A χ2 analysis revealed no evidence of a predictable, consistent relationship between diagnosis group and metabolic syndrome score (χ26, 450 = 3.052, P = .802; Table 4).
DISCUSSION
This study suggests that psychiatrists infrequently consider metabolic syndrome. Testing is rarely ordered. When testing becomes automated, the results are rarely examined. When the diagnostic criteria for metabolic syndrome are met, the diagnosis is rarely entered into the psychiatric discharge summary. The component metabolic disorders are rarely addressed or treated in the inpatient psychiatric setting. Potential barriers that may contribute to psychiatrists’ passivity include lack of familiarity, lack of urgency, and lack of agreement. Barriers to change may include lack of knowledge, historical prescribing practices, and cognitive dissonance.
Lack of Familiarity
Studies25,39 indicate that the majority of psychiatrists are aware of the direct relationship between antipsychotic use and obesity and even the relationship to metabolic syndrome. However, their understanding may be superficial. For example, according to Newcomer et al,39 only 22% of the 300 psychiatrists surveyed recognized that dyslipidemia was a metabolic complication of SGA use.
Lack of Urgency
Awareness of metabolic syndrome does not necessarily translate into diagnosis or management. Many psychiatrists are unfamiliar with current guidelines and recommendations for diagnosis and treating the “medical” diseases of hypertension, diabetes, hyperlipidemia, and obesity. They prefer to leave these diseases to their medical colleagues. They may know that metabolic syndrome reduces life expectancy, but since its detrimental effects are not immediate, they may leave treatment to a “later” time that never comes. Psychiatrists are more likely to overlook metabolic syndrome as it is considered a low priority in patient management. They may not believe their monitoring makes a difference. Only 20.6% of the 2,534 psychiatrists in the Japanese Psychiatric Hospitals Association believed that the frequency with which they monitored their patients was sufficient to reduce metabolic risks.40
Lack of Agreement
Treatment guidelines for individual indices of metabolic syndrome such as hypertension, hyperglycemia, and hyperlipidemia have existed for many years. However, there is no standardized guideline for treating metabolic syndrome, which is secondary to antipsychotic use. There is dissent about which patients to monitor, the utility of glucose tolerance testing, and the point at which to consider switching antipsychotics.41 This lack of general agreement might relieve the individual psychiatrist of any impetus to adhere to medical guidelines.42
Barriers to Behavior Change
Passive educational interventions have limited effectiveness. Physicians demonstrate a limited response to US Food and Drug Administration (FDA) warnings and recommendations, such as those for suggested laboratory monitoring for troglitazone, pemoline, or antipsychotics and clinical monitoring for antidepressants. Physician responses are generally incomplete or temporary.43 For example, FDA advisories about potential cardiovascular risks of attention-deficit/hyperactivity disorder medications have had little discernible effect on national prescribing of these medicines.44 Additionally, antipsychotic polypharmacy remains prevalent despite guideline recommendations for monotherapy.45
Lack of Knowledge
Psychiatrists in our hospital, and in the wider psychiatric community, clearly favor SGAs over first-generation antipsychotics (FGAs). At introduction, drug manufacturers’ advertisements claimed the SGAs produced fewer extrapyramidal symptoms. SGAs quickly became the treatment of choice for psychotic disorders.46 Perphenazine (an FGA) has a frequency of movement side effects similar to SGAs.47 SGAs have a number of other side effects, and in the balance, it remains unclear to what extent SGAs are superior to FGAs.
There is little evidence to support SGAs over FGAs in general.48 One double-blind, randomized, controlled trial reported that olanzapine (an SGA) might not result in a superior quality of life compared to haloperidol due to its increased risk of weight gain and higher cost.49 Haloperidol with benztropine may be superior to olanzapine, as the combination can prevent the deleterious metabolic outcomes of SGA use.
The publicly funded CATIE trial also did not support the superiority of SGAs in schizophrenia.27 CATIE is one of the most influential antipsychotic studies to date. In this study, unfortunately, FGAs were underrepresented, and none were included in the second and final phase of the study, which found olanzapine to be superior to other atypical antipsychotics in regard to symptom reduction and duration of treatment adherence. (FGAs were excluded from the second phase of CATIE on the basis of the assumption that they would cause more side effects.) To conclude, according to CATIE, SGAs may not have a substantial advantage over FGAs.
Cognitive Dissonance
SGAs remain popular among psychiatrists at our facility, mirroring prescribing practices across the nation. The percentage of patients treated with SGAs was unchanged before and after e-mail notifications to the psychiatrists that their patients met criteria for metabolic syndrome. This lack of change may be because psychiatrists about to prescribe SGAs are likely to experience some cognitive dissonance when confronted daily with explicit reminders that a substantial number of their patients either present with metabolic syndrome or may develop it early in the course of treatment with SGAs. Yet, through much of their professional lives, they have been in the habit of prescribing SGAs and have been advised that FGAs are “not as good.” Furthermore, although psychiatrists have a general awareness of metabolic syndrome (as evidenced by the reduction in olanzapine prescriptions after the FDA issued a black box warning on the metabolic risks of olanzapine),24 this awareness may not translate into choice of antipsychotic for a specific patient for whom the treating psychiatrist is about to prescribe medication.
Despite the increase in appropriate documentation of metabolic syndrome in the EMR from 0% to 38%, little improvement was observed in the treatment of hyperlipidemia, hypertension, or hyperglycemia. More than half (53.5%) of patients did not receive treatment targeted to the components of metabolic syndrome before psychiatrists were notified by e-mail that their patient met criteria for metabolic syndrome. After e-mail notification was instituted, this percentage remained at 52.8%. This lack of attention is in stark contrast to the finding that amelioration of metabolic syndrome–associated problems can be obtained with metformin, a well-established and well-tolerated drug that reduces weight and hemoglobin A1c as well as triglycerides in antipsychotic-treated patients.50–54
Role of Computer Algorithms in Detection
and Treatment of Metabolic Syndrome
Active interventions, such as letters or phone calls to physicians, can decrease the use of antipsychotic polypharmacy but may produce a “big-brother”–like atmosphere.55 EMRs are powerful tools for changing physician behavior and improving clinical performance in drug dosing and preventive care,56 resulting in substantial reduction in health care costs.57 Their potential is not yet fully explored. In our study, an EMR admission order set was instrumental in increasing the detection of metabolic syndrome. Unfortunately, mere detection is insufficient. Placing a metabolic syndrome alert in the EMR, coupled with individual notification of the psychiatrist, resulted in only 38% of qualifying patients actually having the diagnosis listed in the psychiatric discharge summary.
EMRs can be designed to incorporate forcing functions. An example of a forcing function is the requirement to enter a creatinine level in the EMR in order to request a contrast-enhanced radiography. A forcing function, which could potentially be incorporated into an EMR, might present physicians with an order set that changes its options depending on whether the patient meets criteria for metabolic syndrome or not. Ultimately, patient management will improve with elimination of human errors in diagnosis.
CONCLUSION
Diagnosing and treating metabolic syndrome is of critical importance in psychiatric patients. This study shows that metabolic syndrome is often underdiagnosed and even when diagnosed is rarely completely treated. Switching antipsychotic medications from SGAs to FGAs will decrease the prevalence of metabolic syndrome, yet psychiatrists seem reluctant to use this strategy. More troubling is the reluctance of psychiatrists to acknowledge and document the diagnosis of metabolic syndrome. More intensive education of both psychiatrists and consulting internists may be helpful in changing prescribing behavior, but incorporating forcing functions into the EMR is more likely to have an immediate effect.
In addition, future quality measures such as the Hospital Based Inpatient Psychiatric Services (Specification Manual for National Quality Core Measures version 2015A)58 may require psychiatrists to document metabolic syndrome. These measures may incentivize physicians to change their prescribing choices.
Submitted: June 17, 2015; accepted November 19, 2015.
Published online: January 28, 2016.
Drug names: aripiprazole (Abilify), atorvastatin (Lipitor and others), clozapine (Clozaril, FazaClo, and others), fenofibrate (Antara), olanzapine (Zyprexa and others), quetiapine (Seroquel and others), risperidone (Risperdal and others), simvastatin (Zocor), ziprasidone (Geodon and others).
Author contributions: Drs Lui and Randhawa collected the data and performed the analysis. Dr Totten assisted in writing and editing the manuscript. Dr Smith consulted on the statistical analysis. Dr Raese conceived the research question and oversaw the project.
Potential conflicts of interest: None reported.
Funding/support: This work was supported by an institutional grant from the Kaweah Healthcare District Foundation, Visalia, California.
Role of the sponsor: The funding organization had no role in the design and conduct of the study; collection, management, and analysis of the data; or preparation, review, and approval of the manuscript.
Previous presentation: Some results of this work were accepted as a poster presentation at the 168th annual meeting of the American Psychiatric Association; May 16–20, 2015; Toronto, Ontario, Canada.
REFERENCES
1. Walker ER, McGee RE, Druss BG. Mortality in mental disorders and global disease burden implications: a systematic review and meta-analysis. JAMA Psychiatry. 2015;72(4):334–341. doi:10.1001/jamapsychiatry.2014.2502 PubMed
2. Correll CU, Druss BG, Lombardo I, et al. Findings of a US national cardiometabolic screening program among 10,084 psychiatric outpatients. Psychiatr Serv. 2010;61(9):892–898. doi:10.1176/ps.2010.61.9.892 PubMed
3. Vancampfort D, Vansteelandt K, Correll CU, et al. Metabolic syndrome and metabolic abnormalities in bipolar disorder: a meta-analysis of prevalence rates and moderators. Am J Psychiatry. 2013;170(3):265–274. doi:10.1176/appi.ajp.2012.12050620 PubMed
4. Björkenstam E, Ljung R, Burström B, et al. Quality of medical care and excess mortality in psychiatric patients: a nationwide register-based study in Sweden. BMJ Open. 2012;2(1):e000778. doi:10.1136/bmjopen-2011-000778 PubMed
5. Grundy SM, Brewer HB Jr, Cleeman JI, et al. National Heart, Lung, and Blood Institute. Definition of metabolic syndrome: report of the National Heart, Lung, and Blood Institute/American Heart Association conference on scientific issues related to definition. Circulation. 2004;109(3):433–438. doi:10.1161/01.CIR.0000111245.75752.C6 PubMed
6. Yates KF, Sweat V, Yau PL, et al. Impact of metabolic syndrome on cognition and brain: a selected review of the literature. Arterioscler Thromb Vasc Biol. 2012;32(9):2060–2067. doi:10.1161/ATVBAHA.112.252759 PubMed
7. Dregan A, Stewart R, Gulliford M. Cardiovascular risk factors and cognitive decline in adults aged 50 and over: a population-based cohort study. Age Ageing. 2012;0:1–8 Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults Executive Summary of the Third Report of the National Cholesterol Education Program [NCEP]. PubMed
8. Friedman JI, Wallenstein S, Moshier E, et al. The effects of hypertension and body mass index on cognition in schizophrenia. Am J Psychiatry. 2010;167(10):1232–1239. doi:10.1176/appi.ajp.2010.09091328 PubMed
9. Yaffe K, Falvey C, Hamilton N, et al. Diabetes, glucose control, and 9-year cognitive decline among older adults without dementia. Arch Neurol. 2012;69(9):1170–1175. PubMed
10. Osborn DP, Wright CA, Levy G, et al. Relative risk of diabetes, dyslipidemia, hypertension and the metabolic syndrome in people with severe mental illnesses: systematic review and meta-analysis. BMC Psychiatry. 2008;8(1):84. doi:10.1186/1471-244X-8-84 PubMed
11. Mitchell AJ, Vancampfort D, Sweers K, et al. Prevalence of metabolic syndrome and metabolic abnormalities in schizophrenia and related disorders: a systematic review and meta-analysis. Schizophr Bull. 2013;39(2):306–318. doi:10.1093/schbul/sbr148 PubMed
12. Newcomer JW. Second-generation (atypical) antipsychotics and metabolic effects: a comprehensive literature review. CNS Drugs. 2005;19(suppl 1):1–93. doi:10.2165/00023210-200519001-00001 PubMed
13. Luppino FS, de Wit LM, Bouvy PF, et al. Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. Arch Gen Psychiatry. 2010;67(3):220–229. doi:10.1001/archgenpsychiatry.2010.2 PubMed
14. Jokela M, Hamer M, Singh-Manoux A, et al. Association of metabolically healthy obesity with depressive symptoms: pooled analysis of eight studies. Mol Psychiatry. 2014;19(8):910–914. doi:10.1038/mp.2013.162 PubMed
15. Brown S. Excess mortality of schizophrenia: a meta-analysis. Br J Psychiatry. 1997;171(6):502–508. doi:10.1192/bjp.171.6.502 PubMed
16. Brown S, Kim M, Mitchell C, et al. Twenty-five year mortality of a community cohort with schizophrenia. Br J Psychiatry. 2010;196(2):116–121. doi:10.1192/bjp.bp.109.067512 PubMed
17. McEvoy JP, Meyer JM, Goff DC, et al. Prevalence of the metabolic syndrome in patients with schizophrenia: baseline results from the Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) schizophrenia trial and prevalence of the metabolic syndrome in patients with schizophrenia: baseline results from the clinical comparisons with estimates from NHANES III. Schizophr Res. 2005;80:19–32. doi:10.1016/j.schres.2005.07.014 PubMed
18. Correll CU, Robinson DG, Schooler NR, et al. Cardiometabolic risk in patients with first-episode schizophrenia spectrum disorders: baseline results from the RAISE-ETP study. JAMA Psychiatry. 2014;71(12):1350–1363. PubMed
19. Correll CU, Frederickson AM, Kane JM, et al. Metabolic syndrome and the risk of coronary heart disease in 367 patients treated with second-generation antipsychotic drugs. J Clin Psychiatry. 2006;67(4):575–583. doi:10.4088/JCP.v67n0408 PubMed
20. Newcomer JW. Metabolic considerations in the use of antipsychotic medications: a review of recent evidence. J Clin Psychiatry. 2007;68
(suppl 1):20–27. PubMed
21. De Hert M, Detraux J, van Winkel R, et al. Metabolic and cardiovascular adverse effects associated with antipsychotic drugs. Nat Rev Endocrinol. 2012;8(2):114–126. doi:10.1038/nrendo.2011.156 PubMed
22. Barnes TR, Paton C, Cavanagh MR, et al. UK Prescribing Observatory for Mental Health. A UK audit of screening for the metabolic side effects of antipsychotics in community patients. Schizophr Bull. 2007;33(6):1397–1403. doi:10.1093/schbul/sbm038 PubMed
23. Barnett M, VonMuenster S, Wehring H, et al. Assessment of monitoring for glucose and lipid dysregulation in adult Medi-Cal patients newly started on antipsychotics. Ann Clin Psychiatry. 2010;22(1):9–18. PubMed
24. Morrato EH, Druss B, Hartung DM, et al. Metabolic testing rates in 3 state Medicaid programs after FDA warnings and ADA/APA recommendations for second-generation antipsychotic drugs. Arch Gen Psychiatry. 2010;67(1):17–24. doi:10.1001/archgenpsychiatry.2009.179 PubMed
25. Centers for Medicare and Medicaid Services. Final FY 2016 Medicare Payment and Policy Changes for Inpatient Psychiatric Facilities. https://www.cms.gov/Newsroom/MediaReleaseDatabase/Fact-sheets/2015-Fact-sheets-items/2015-07-31.html. Accessed January 7, 2016.
26. Quality Reporting Center. Inpatient Psychiatric Facility Quality Reporting (IPFQR) Program Measures for Fiscal Year (FY) 2017 and FY 2018. http://www.qualityreportingcenter.com/wp-content/uploads/2014/10/IPF_FY2017-2018_MeasuresTablesPopSampFY17_Tool_20151023_FINAL_508.pdf. Accessed January 7, 2016.
27. Lieberman JA, Stroup TS, McEvoy JP, et al. Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) Investigators. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med. 2005;353(12):1209–1223. doi:10.1056/NEJMoa051688 PubMed
28. Henderson DC, Cagliero E, Copeland PM, et al. Glucose metabolism in patients with schizophrenia treated with atypical antipsychotic agents: a frequently sampled intravenous glucose tolerance test and minimal model analysis. Arch Gen Psychiatry. 2005;62(1):19–28. doi:10.1001/archpsyc.62.1.19 PubMed
29. Leslie DL, Rosenheck RA. Incidence of newly diagnosed diabetes attributable to atypical antipsychotic medications. Am J Psychiatry. 2004;161(9):1709–1711. doi:10.1176/appi.ajp.161.9.1709 PubMed
30. Allison DB, Mentore JL, Heo M, et al. Antipsychotic-induced weight gain: a comprehensive research synthesis. Am J Psychiatry. 1999;156(11):1686–1696. PubMed
31. Lett TA, Wallace TJM, Chowdhury NI, et al. Pharmacogenetics of antipsychotic-induced weight gain: review and clinical implications. Mol Psychiatry. 2012;17(3):242–266. doi:10.1038/mp.2011.109 PubMed
32. Reynolds GP. Pharmacogenetic aspects of antipsychotic drug–induced weight gain: a critical review. Clin Psychopharmacol Neurosci. 2012;10(2):71–77. doi:10.9758/cpn.2012.10.2.71 PubMed
33. Huang PL. A comprehensive definition for metabolic syndrome. Dis Model Mech. 2009;2(5–6):231–237. doi:10.1242/dmm.001180 PubMed
34. National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Third report of the National Cholesterol Education Program (NCEP) Expert Panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III) final report. Circulation. 2002;106(25):3143–3421. PubMed
35. L’Italien GJ, Casey DE, Kan HJ, et al. Comparison of metabolic syndrome incidence among schizophrenia patients treated with aripiprazole versus olanzapine or placebo. J Clin Psychiatry. 2007;68(10):1510–1516. doi:10.4088/JCP.v68n1006 PubMed
36. Meyer JM, Davis VG, Goff DC, et al. Change in metabolic syndrome parameters with antipsychotic treatment in the CATIE schizophrenia trial: prospective data from phase 1. Schizophr Res. 2008;101(1–3):273–286. doi:10.1016/j.schres.2007.12.487 PubMed
37. da Luz PL, Favarato D, Faria-Neto JR Jr, et al. High ratio of triglycerides to HDL cholesterol predicts extensive coronary disease. Clinics (Sao Paulo). 2008;63(4):427–432. 10.1590/S1807-59322008000400003 PubMed
38. Malhotra AK, Correll CU, Chowdhury NI, et al. Association between common variants near the melanocortin 4 receptor gene and severe antipsychotic drug-induced weight gain. Arch Gen Psychiatry. 2012;69(9):904–912. doi:10.1001/archgenpsychiatry.2012.191 PubMed
39. Newcomer JW, Nasrallah HA, Loebel AD. The atypical antipsychotic therapy and metabolic issues national survey: practice patterns and knowledge of psychiatrists. J Clin Psychopharmacol. 2004;24(suppl 1):S1–S6. doi:10.1097/01.jcp.0000142281.85207.d5 PubMed
40. Sugawara N, Yasui-Furukori N, Yamazaki M, et al. Psychiatrists’ attitudes toward metabolic adverse events in patients with schizophrenia. PLoS ONE. 2014;9(1):e86826. doi:10.1371/journal.pone.0086826 PubMed
41. Cohn TA, Sernyak MJ. Metabolic monitoring for patients treated with antipsychotic medications. Can J Psychiatry. 2006;51(8):492–501. PubMed
42. Cabana MD, Rand CS, Powe NR, et al. Why don’t physicians follow clinical practice guidelines? a framework for improvement. JAMA. 1999;282(15):1458–1465. doi:10.1001/jama.282.15.1458 PubMed
43. Dusetzina SB, Higashi AS, Dorsey ER, et al. Impact of FDA drug risk communications on health care utilization and health behaviors: a systematic review. Med Care. 2012;50(6):466–478. doi:10.1097/MLR.0b013e318245a160 PubMed
44. Kornfield R, Watson S, Higashi AS, et al. Effects of FDA advisories on the pharmacologic treatment of ADHD, 2004–2008. Psychiatr Serv. 2013;64(4):339–346. doi:10.1176/appi.ps.201200147 PubMed
45. Gilmer TP, Dolder CR, Folsom DP, et al. Antipsychotic polypharmacy trends among Medicaid beneficiaries with schizophrenia in San Diego County, 1999–2004. Psychiatr Serv. 2007;58(7):1007–1010. doi:10.1176/ps.2007.58.7.1007 PubMed
46. Kerwin RW. The new atypical antipsychotics: a lack of extrapyramidal side effects and new routes in schizophrenia research. Br J Psychiatry. 1994;164(2):141–148. doi:10.1192/bjp.164.2.141 PubMed
47. Stroup TS, McEvoy JP, Swartz MS, et al. The National Institute of Mental Health Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) project: schizophrenia trial design and protocol development. Schizophr Bull. 2003;29(1):15–31. doi:10.1093/oxfordjournals.schbul.a006986 PubMed
48. Carpenter WT, Buchanan RW. Lessons to take home from CATIE. Psychiatr Serv. 2008;59(5):523–525. doi:10.1176/ps.2008.59.5.523 PubMed
49. Rosenheck R, Perlick D, Bingham S, et al. Department of Veterans Affairs Cooperative Study Group on the Cost-Effectiveness of Olanzapine. Effectiveness and cost of olanzapine and haloperidol in the treatment of schizophrenia: a randomized controlled trial. JAMA. 2003;290(20):2693–2702. doi:10.1001/jama.290.20.2693 PubMed
50. Jarskog LF, Hamer RM, Catellier DJ, et al. METS Investigators. Metformin for weight loss and metabolic control in overweight outpatients with schizophrenia and schizoaffective disorder. Am J Psychiatry. 2013;170(9):1032–1040. doi:10.1176/appi.ajp.2013.12010127 PubMed
51. Baptista T, Martínez J, Lacruz A, et al. Metformin for prevention of weight gain and insulin resistance with olanzapine: a double-blind placebo-controlled trial. Can J Psychiatry. 2006;51(3):192–196. PubMed
52. Baptista T, Rangel N, Fernández V, et al. Metformin as an adjunctive treatment to control body weight and metabolic dysfunction during olanzapine administration: a multicentric, double-blind, placebo-controlled trial. Schizophr Res. 2007;93(1–3):99–108. doi:10.1016/j.schres.2007.03.029 PubMed
53. Carrizo E, Fernández V, Connell L, et al. Extended release metformin for metabolic control assistance during prolonged clozapine administration: a 14-week, double-blind, parallel group, placebo-controlled study. Schizophr Res. 2009;113(1):19–26. doi:10.1016/j.schres.2009.05.007 PubMed
54. Klein DJ, Cottingham EM, Sorter M, et al. A randomized, double-blind, placebo-controlled trial of metformin treatment of weight gain associated with initiation of atypical antipsychotic therapy in children and adolescents. Am J Psychiatry. 2006;163(12):2072–2079. doi:10.1176/ajp.2006.163.12.2072 PubMed
55. Fleischhacker WW, Uchida H. Critical review of antipsychotic polypharmacy in the treatment of schizophrenia. Int J Neuropsychopharmacol. 2014;17(7):1083–1093. doi:10.1017/S1461145712000399 PubMed
56. Hunt DL, Haynes RB, Hanna SE, et al. Effects of computer-based clinical decision support systems on physician performance and patient outcomes: a systematic review. JAMA. 1998;280(15):1339–1346. doi:10.1001/jama.280.15.1339 PubMed
57. Hillestad R, Bigelow J, Bower A, et al. Can electronic medical record systems transform health care? potential health benefits, savings, and costs. Health Aff (Millwood). 2005;24(5):1103–1117. doi:10.1377/hlthaff.24.5.1103 PubMed
58. The Joint Commission. Specifications Manual for Joint Commission National Quality Measures (v2015A1). Hospital Based Inpatient Psychiatric Services (HBIPS). https://manual.jointcommission.org/releases/TJC2015A1/HospitalBasedInpatientPsychiatricServices.html. Accessed January 7, 2016.
Enjoy this premium PDF as part of your membership benefits!


