ABSTRACT
Background: This study surveyed adults with attention-deficit/hyperactivity disorder (ADHD) to understand the impact of the COVID-19 pandemic on aspects of their disorder, quality of life, and treatment experience.
Methods: A cross-sectional survey of US-resident members of PatientsLikeMe (PLM) was conducted through the PLM health tracking platform between March 10 and April 2, 2021. Adult participants with self-reported ADHD currently taking prescription medication (treated) and those not taking medication (untreated) were enrolled.
Results: The study included 93 adults, of whom 48 patients were taking medication for ADHD. Most of the 45 untreated patients were not taking medication for reasons unrelated to the pandemic. Of the 47 treated patients who also completed the survey, 22 patients had ≥ 1 switch in ADHD medication type, and nearly half had a dosage change during the pandemic. Further, 29 treated patients reported a negative impact of the pandemic on their daily ADHD medication routine, primarily due to a “lack of schedule” and “changes to structured routine,” and 16 patients reported “increased difficulty” adhering to prescribed ADHD medication during the pandemic compared with before the pandemic. Of the total study population, 52 patients reported having a telehealth visit during the pandemic, and 38 patients had an ADHD management goal. All but 1 patient with an ADHD management goal reported a negative impact of the pandemic on progress toward their goal. More treated patients than untreated adults reported having control over bothersome ADHD symptoms.
Conclusions: Adults with ADHD reported increased difficulty in managing their symptoms during the COVID-19 pandemic.
Prim Care Companion CNS Disord 2023;25(4):22m03474
Author affiliations are listed at the end of this article.
Attention-deficit/hyperactivity disorder (ADHD) is a neurodevelopmental disorder characterized by inattention, hyperactivity, and impulsivity.1 ADHD often begins in childhood, but it persists into adulthood for many individuals.1,2 The prevalence of ADHD in adults was estimated to be 4.4% in a US national survey.3
The core symptoms of ADHD (inattention, hyperactivity, and impulsivity) tend to endure throughout life, but their clinical presentation may change over time.4–6 In adults, inattention can be expressed through difficulties organizing and prioritizing work, lack of concentration, and trouble completing tasks.5,6 Hyperactivity can be characterized by feelings of restlessness or agitation, excessive talking, and the inability to rest, relax, or sleep.6,7 Impulsivity can manifest as frequent job changes, interrupting, acting without forethought, and blurting out thoughts that can cause distress to others.5,6 Adults with ADHD are also more likely to engage in sensation-seeking behavior, risk taking, and unhealthy practices such as smoking or alcohol or drug misuse.6,7
ADHD has a negative impact on long-term outcomes (including educational attainment and employability) among adults, as well as on their self-esteem and social functioning.8–10 A recent (2019) cross-sectional study by Quintero et al11 found that, compared with control populations, adults with ADHD reported significantly lower (ie, worse) total scores and scores on all subscales of life outlook, relationships, psychological health, and life productivity on the Adult ADHD Quality of Life rating scale. Long-term ADHD can result in a variety of burdensome socioeconomic costs such as loss of work productivity, increased health care expenditures, and higher spending on social services.9,12,13 Other impacts are more difficult to quantify, such as high emotional burden, impaired goal attainment, and poor quality of life for both the individual with ADHD and other family members.9
PatientsLikeMe (PLM) is an online, integrated community that offers health management and a real-world data platform through which patients with diverse medical conditions support one another and share personal information about their health, symptoms, and treatments.14 The PLM platform provides real-world data on a wide range of conditions and their management by tracking symptoms, quality of life, and other important health data. As of early 2020, the PLM community consisted of approximately 830,000 members, sharing their experiences managing over 2,800 conditions, including ADHD.
The ongoing COVID-19 pandemic has resulted in widespread shifts in social interactions and access to effective treatment since early 2020. School and workplace closures leading to impaired social interactions and financial uncertainties, telehealth services without in-person support and interaction, and other pandemic-related stressors may be especially challenging for patients with psychiatric and neurodevelopmental disorders, including adults with ADHD.15,16 These changes have the potential to worsen ADHD symptoms and increase the burden of disease. The UNCOVER study (Understanding the patient experience during the COVID-19 pandemic, effects on real world quality of life, symptom management and clinical outcomes in patients treated and untreated for ADHD) surveyed adult patients with ADHD in the US who are members of PLM to better understand the impact of the COVID-19 pandemic on aspects of their disorder and quality of life.
METHODS
Study Design
In the UNCOVER study, a 36-question cross-sectional survey was conducted between March 10 and April 2, 2021, via the PLM health tracking platform. The study included adult patients (aged ≥ 18 years) with ADHD in the US who were taking prescribed medication for ADHD (treated) or were not taking any ADHD management drugs (untreated). Study participants were PLM members with self-reported ADHD who provided written informed consent. No additional exclusion criteria were applied. The UNCOVER study protocol was approved by the WIRB-Copernicus Group Institutional Review Board on February 23, 2021. Questions that captured the experience with ADHD are listed in Supplementary Appendix 1.
Data and Statistical Analyses
The survey collected data related to the impact on treatment, access to medical care, symptoms, and ADHD management goals. Descriptive statistics were calculated for demographics and individual survey items. Summary statistics for continuous variables included the number of respondents and mean value. Categorical variables were reported as frequencies and proportions. Categorical variables were compared using the χ2 test, and continuous variables were compared between groups using 2-sample t tests.
RESULTS
Study Participants and Impact of the COVID-19 Pandemic on Employment and Insurance
The 39-question survey was completed by 93 adults (Table 1). The majority of respondents were female and aged ≥ 40 years. Of the 93 participants, 32 individuals (34%) reported a change in employment status during the COVID-19 pandemic, and 8 of them had lost their jobs and were still unemployed at the time of this study. Twenty participants (22%) had a change in their medical insurance during the pandemic, including 6 individuals who reported loss of medical insurance coverage during the study period.
Impact of the COVID-19 Pandemic on Medication Management for ADHD
Of the entire study population, 45 patients (48%) were not taking prescription drugs for the treatment of ADHD at the time of the study, and the remaining 48 patients (52%) were taking prescribed medication for ADHD. Of the 45 patients not on any prescribed ADHD medication at the time of the study, 4 patients reported that they were regularly taking prescribed medication for ADHD prior to the pandemic. Only 3 (7%) of the 45 patients in this group reported difficulties accessing treatment (due to loss of employment or insurance coverage) during the pandemic as their reason for not taking ADHD medication. Most patients in this group (27/45, 60%) stated their reason for not taking prescribed ADHD medication was unrelated to the pandemic, and 7 patients (16%) reported they were not taking ADHD medication due to side effects.
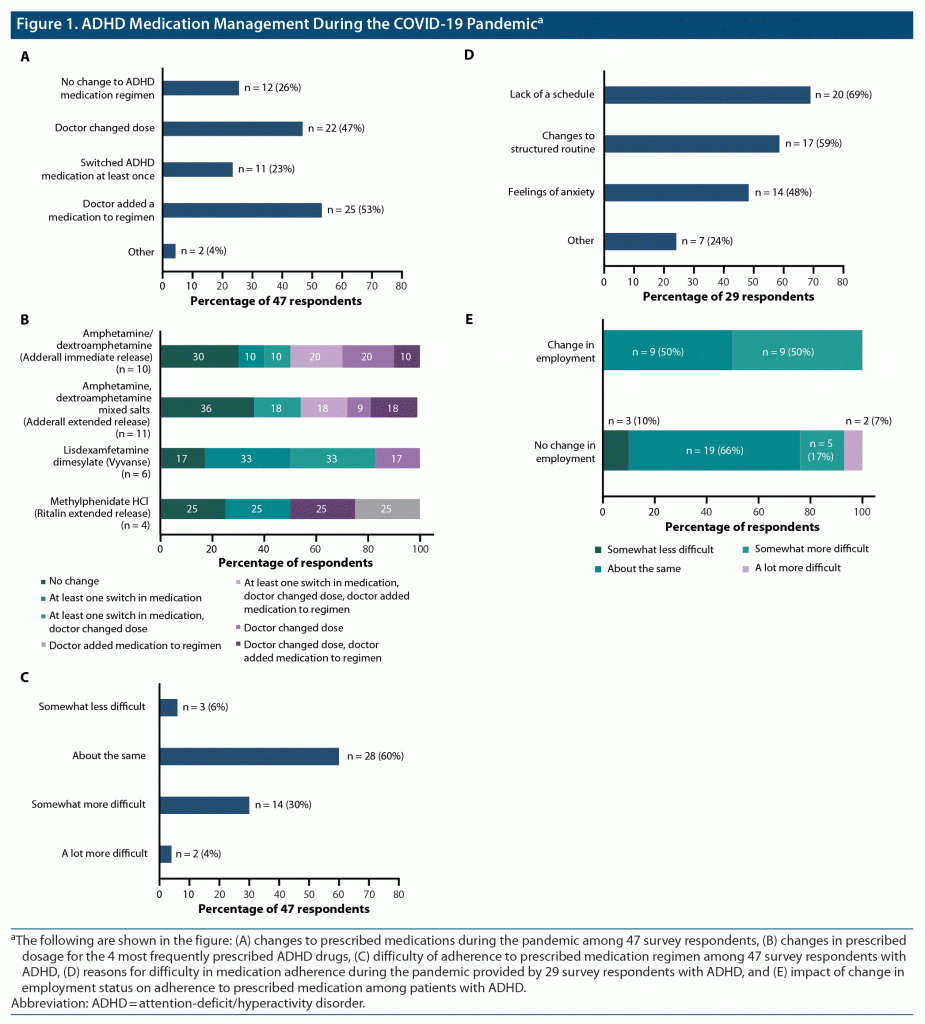
Of the 48 participants who were taking prescription drugs for ADHD (such as amphetamine, lisdexamfetamine dimesylate, and methylphenidate) at the time of the study, 1 respondent did not complete additional follow-up questions on ADHD management. Of the 47 patients who completed the survey, one-quarter (23%) had at least 1 switch in their prescribed medication, and nearly half of the patients (47%) had their medication dosage changed by their physicians since the beginning of the COVID-19 pandemic (Figures 1A and B). In addition, one-third of the patients in this group (34%) reported greater difficulty in adhering to their ADHD medication during the pandemic than before (Figure 1C). Nearly two-thirds of treated patients reported that pandemic-related difficulties negatively impacted their daily medication routine, primarily due to “lack of schedule” (n = 20) and “changes to routine structure” (n = 17, Figure 1D). Fewer patients without a change in employment status reported difficulty adhering to their medication regimen, compared with those who had a change in employment, although this difference was not statistically significant (P = .08) (Figure 1E).
Management of ADHD Symptoms and Treatment Goals During the COVID-19 Pandemic
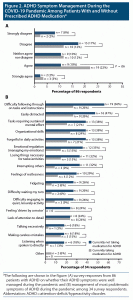
Of the 93 survey participants, 86 patients (44 patients taking medication for ADHD and 42 untreated patients) further described the management of their ADHD symptoms and treatment goals during the COVID-19 pandemic. Of these 86 patients, 34 patients (39%) either “disagreed” or “strongly disagreed” that their symptoms were well managed during the pandemic, citing “difficulty following through on tasks and instructions” (n = 28), “easily distracted” (n = 25), and lack of “organizational skills” (n = 21) as the most difficult symptoms to manage (Figures 2A and 2B). Most patients who “agreed” or “strongly agreed” that their symptoms were well managed during the pandemic (22/33, 67%) were taking prescribed medications (Figure 2A). Patients receiving medication for ADHD also appeared to have better control in managing the most problematic symptoms of ADHD than those not taking any medication for ADHD, although this comparison was not statistically significant (P = .056, Figure 2A).
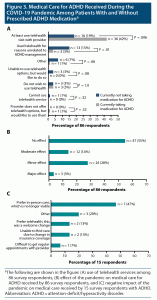
More than half of the patients (52/86, 60%) reported having at least 1 telehealth visit related to ADHD (Figure 3A). While 47 of 86 patients said that the pandemic did not affect the medical care they received for ADHD at all (Figure 3B), 15 others reported a pandemic-related negative impact on their level of medical care, including 7 patients who stated a preference for in-person care that was not easily available during the pandemic (Figure 3C).
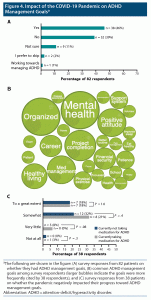
Regardless of treatment status, 38 patients had goals for managing their ADHD during the pandemic, including management of mental health, organization, and a positive attitude (Figures 4A and 4B). However, 37 of those 38 patients reported a negative impact of the pandemic on progress toward their goal (Figure 4C).
DISCUSSION
ADHD is a pervasive disorder that can affect multiple areas of life, including employment and work productivity, as well as social and family relationships. While the current COVID-19 pandemic has created unprecedented challenges at every level of society, many clinicians have recognized that individuals with ADHD may be especially vulnerable to stresses caused by the pandemic.15 In the UNCOVER study, we aimed to understand the impact of the pandemic on patients with ADHD with respect to their quality of life, symptom management, and goal attainment and to determine the role played by their treatment status and health care interactions on that impact.
The main finding of this study was that patients with ADHD reported greater difficulty in managing their symptoms during the COVID-19 pandemic than before. Patients with ADHD experienced a wide range of behavioral symptoms that were self-reported as bothersome during the pandemic, including “difficulty following through on tasks and instructions” and being “easily distracted.” Fewer patients who were taking prescription medications for ADHD reported difficulties with symptom management than those who were not being treated with medication, suggesting that everyday functioning associated with ADHD was better managed in patients treated with medication.
Many patients treated with an ADHD medication reported a change in medication, dosage, or medication routine during the pandemic. In this study, 23% of treated adult patients reported a switch in prescribed medication, and 47% had a change of dose, including those taking amphetamine, lisdexamfetamine dimesylate, and methylphenidate. In this study, we do not know how long patients were on their current/previous treatment. By comparison, in a study conducted primarily in the pre-pandemic period (January 2015−October 2020),17 24% of treatment-naive patients switched medication within 2 months after treatment initiation, and 25% required a formulation change or another medication for anxiety or depression. The European ADHD Guidance Group15 highlights that individuals with ADHD may be more susceptible to stresses caused by the pandemic. Pandemic-associated stress may underlie the relatively high rates of ADHD medication regimen changes reported by our survey respondents. Further, many patients in our study found it difficult to adhere to their ADHD medication during the pandemic, attributing this to pandemic-related disruptions to daily medication routine structure. Half of the patients who had a change in employment status found it difficult to adhere to their ADHD medication, compared with only a quarter who had no change in employment during the pandemic, suggesting that change in employment status is an added stressor affecting patients with ADHD. These observations reiterated the impact of the unique circumstances of the pandemic on adult patients with ADHD.
The reduced availability of face-to-face consultations, coupled with state- and federal-level policy changes, has led to a dramatic increase in the availability of telehealth services in the United States.16,18 In this study, 60% of respondents had at least 1 telehealth visit. The proportion of patients who had a telehealth visit was higher among those receiving ADHD medication than in untreated patients. The widespread availability of telehealth visits may partially account for the finding that over half of patients reported that the pandemic did not negatively impact the medical care received for ADHD. Nonetheless, 7 of 15 survey respondents who indicated that their ADHD-related treatment was affected by the pandemic expressed a preference for in-person care. Many respondents reported working toward a goal as a self-care strategy to better manage their ADHD. The ADHD goals of these patients were diverse, but improvement in mental health, lifestyle, and home and work environments was important. This suggests that consistent support—that is tailored to the individual needs of patients and that facilitates achievement of treatment goals—is warranted.
The current pandemic has increased the demand for health care services, which has tested the resources and resilience of health care systems.18 Pandemic-associated stress factors, such as social isolation, financial anxieties, and health concerns, can worsen mental health issues and increase the need for clinical services.16 Our data suggest this is especially true of patients with ADHD, who thrive under consistency and structured routines.19 Behavioral issues of patients with ADHD can be effectively managed with medication, access to health care services tailored to individual preferences, and consistent peer support. Enhanced training to improve virtual patient-clinician interactions, design of adapted digital tools for patients with ADHD, and creation of virtual peer support groups such as PLM may compensate for the lack of face-to-face interaction and increase support for patients with ADHD using telehealth services.16 Goal attainment training and digital tools to help track symptoms, set goals, and monitor progress (like PLM) could be helpful to further support patients in their care journey.20
This study is limited by the selection of participants who, as members and contributors to the PLM platform, may be particularly invested in trying to understand and manage their condition. This limits the generalizability of the findings to the overall population of patients with ADHD. In general, the PLM population is also more biased toward middle-aged women. As such, the participants in this study were also more likely to be female and aged ≥ 40 years. The small sample size restricts interpretation of the data. The cross-sectional design of the study did not capture changes in patient experiences over the course of the pandemic; for example, whether symptoms improved or deteriorated. Comparisons of patient experiences with the pre-pandemic period were not possible. The results presented in this study were merely descriptive and are not causal.
Results of this survey show that the COVID-19 pandemic potentially had deleterious effects on adults with ADHD. Patients with ADHD reported more difficulties in managing their ADHD during the COVID-19 era than before the start of the pandemic. The proportion of patients reporting a negative impact of COVID-19 on ADHD symptom and treatment management was higher among patients not taking any ADHD medication compared with those who were taking prescription drugs for ADHD; however, these findings were not significant. More patients taking prescribed medication for ADHD reported having control over the most bothersome symptoms of ADHD than those not taking any medication for ADHD.
Article Information
Published Online: July 13, 2023. https://doi.org/10.4088/PCC.22m03474
© 2023 Physicians Postgraduate Press, Inc.
Submitted: December 20, 2022; accepted March 28, 2023.
To Cite: Raveendran S, Burke MC, Klahn K, et al. The experience of adults with attention-deficit/hyperactivity disorder in 2021 during the COVID-19 pandemic: the UNCOVER Study. Prim Care Companion CNS Disord. 2023;25(4):22m03474.
Author Affiliations: PatientsLikeMe LLC, Boston, Massachusetts (Raveendran, Burke); Takeda Pharmaceuticals USA, Inc, Lexington, Massachusetts (Klahn, McCue, Roy, Martin, Sarkey).
Corresponding Author: Subhara Raveendran, PhD, PatientsLikeMe LLC, 6 Liberty Square, Suite 2602, Boston, MA 02109 ([email protected]).
Relevant Financial Relationships: At the time of the study, Drs Raveendran and Burke were employees of PatientsLikeMe, LLC, Boston, MA. Drs Klahn, McCue, Roy, Martin, and Sarkey are employees of Takeda Pharmaceuticals USA, Inc, Lexington, MA. PatientsLikeMe, LLC, and Takeda Pharmaceuticals USA, Inc, collaborated to perform this study. The funding was provided by Takeda Pharmaceuticals USA, Inc, Lexington, MA.
Funding/Support: PatientsLikeMe and Takeda Pharmaceuticals, Inc, collaborated on this study. This research and the journal’s publication fees were supported by Takeda Pharmaceuticals USA, Inc, Lexington, MA. Under the direction of the authors, editorial support was provided by Oishika Panda, PhD (Oxford PharmaGenesis, Inc, Newtown, PA) and funded by Takeda Pharmaceuticals USA, Inc (Lexington, MA).
Role of the Sponsor: The sponsor (PatientsLikeMe, LLC) was involved in the study design and conduct, the analysis of the results, the generation of the manuscript, and the approval to submit the manuscript for publication.
Previous Presentation: Psych Congress; October 29‒November 1, 2021; San Antonio, TX.
Acknowledgments: The authors thank the survey respondents who participated in this study.
Supplementary Material: See accompanying pages.
Clinical Points
- Adult patients with attention-deficit/hyperactivity disorder (ADHD) found it more difficult to manage their symptoms during the COVID-19 pandemic than before.
- The COVID-19 pandemic led to disruptions in daily routine, fewer in-person interactions with health care providers and peers, and employment-related stress, all of which caused issues with adherence to ADHD treatment regimens among patients.
- As patients with ADHD have diverse treatment and disease management goals, health care providers should aim to provide support tailored to the individual needs of every patient to facilitate achievement of these goals.
References (20)

- Feldman HM, Reiff MI. Clinical practice: attention deficit-hyperactivity disorder in children and adolescents. N Engl J Med. 2014;370(9):838–846. PubMed CrossRef
- Faraone SV, Asherson P, Banaschewski T, et al. Attention-deficit/hyperactivity disorder. Nat Rev Dis Primers. 2015;1(1):15020. PubMed CrossRef
- Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716–723. PubMed CrossRef
- Adler LA, Faraone SV, Spencer TJ, et al. The structure of adult ADHD. Int J Methods Psychiatr Res. 2017;26(1):e1555. PubMed CrossRef
- Goodman DW, Thase ME. Recognizing ADHD in adults with comorbid mood disorders: implications for identification and management. Postgrad Med. 2009;121(5):20–30. PubMed CrossRef
- Kooij JJS, Bijlenga D, Salerno L, et al. Updated European Consensus Statement on diagnosis and treatment of adult ADHD. Eur Psychiatry. 2019;56(1):14–34. PubMed CrossRef
- Giupponi G, Innamorati M, Rogante E, et al. The characteristics of mood polarity, temperament, and suicide risk in adult ADHD. Int J Environ Res Public Health. 2020;17(8):2871. PubMed CrossRef
- Biederman J, Petty C, Fried R, et al. Impact of psychometrically defined deficits of executive functioning in adults with attention deficit hyperactivity disorder. Am J Psychiatry. 2006;163(10):1730–1738. PubMed CrossRef
- Bernfort L, Nordfeldt S, Persson J. ADHD from a socio-economic perspective. Acta Paediatr. 2008;97(2):239–245. PubMed CrossRef
- Fredriksen M, Dahl AA, Martinsen EW, et al. Childhood and persistent ADHD symptoms associated with educational failure and long-term occupational disability in adult ADHD. Atten Defic Hyperact Disord. 2014;6(2):87–99. PubMed CrossRef
- Quintero J, Morales I, Vera R, et al. The impact of adult ADHD in the quality of life profile. J Atten Disord. 2019;23(9):1007–1016. PubMed CrossRef
- Brod M, Pohlman B, Lasser R, et al. Comparison of the burden of illness for adults with ADHD across seven countries: a qualitative study. Health Qual Life Outcomes. 2012;10(1):47. PubMed CrossRef
- Jennum P, Hastrup LH, Ibsen R, et al. Welfare consequences for people diagnosed with attention deficit hyperactivity disorder (ADHD): a matched nationwide study in Denmark. Eur Neuropsychopharmacol. 2020;37:29–38. PubMed CrossRef
- PatientsLikeMe. Empowering patients through community. PatientsLikeMe website. Published 2005. Accessed April 2022. https://www.patientslikeme.com/about
- Cortese S, Asherson P, Sonuga-Barke E, et al; European ADHD Guidelines Group. ADHD management during the COVID-19 pandemic: guidance from the European ADHD Guidelines Group. Lancet Child Adolesc Health. 2020;4(6):412–414. PubMed CrossRef
- Torous J, Wykes T. Opportunities from the coronavirus disease 2019 pandemic for transforming psychiatric care with telehealth. JAMA Psychiatry. 2020;77(12):1205–1206. PubMed CrossRef
- Biederman J, DiSalvo M, Green A, et al. Rates of switching stimulants in consecutively referred medication naïve adults with ADHD. Acta Psychiatr Scand. 2021;144(6):626–634. PubMed CrossRef
- Tarricone R, Rognoni C. What can health systems learn from COVID-19? Eur Heart J suppl. 2020;22(suppl P):P4–P8. PubMed CrossRef
- Ginapp CM, Macdonald-Gagnon G, Angarita GA, et al. The lived experiences of adults with attention-deficit/hyperactivity disorder: a rapid review of qualitative evidence. Front Psychiatry. 2022;13:949321. PubMed CrossRef
- Jensen DA, Halmøy A, Stubberud J, et al. An exploratory investigation of goal management training in adults with ADHD: improvements in inhibition and everyday functioning. Front Psychol. 2021;12:659480. PubMed CrossRef
This PDF is free for all visitors!