The Impact of Body Image on Patient Care
Have you ever wondered how one’s sense of self interacts with disease processes and conditions? Have you thought about how body image, self-esteem, and quality of life impact function? If you have, then the following vignette and discussion may serve as a stimulus to look at the concept of body image and how it impacts the comprehensive care of your patients.
CASE VIGNETTE
As a child, Mr A was a healthy, social, interactive, and playful boy until, at age 5 years, he was hit by a runaway car. The accident led to a hospitalization for a clavicular fracture and facial trauma that resulted in a disfiguring scar on his right cheek.
This scar led to teasing by his kindergarten classmates; he was nicknamed “scarface.” As Mr A progressed through childhood and adolescence, he became quite shy and withdrawn; this prompted school teachers to place him in “special” classes. Although he never saw a mental health professional (eg, a psychologist, social worker, or psychiatrist), it was readily apparent that his shyness was exacerbated by interactions with his peers and that he coped by withdrawing from social situations.
Although his scar became less visible as he aged, his shyness persisted. Even as a young man, he was very uncomfortable having his picture taken or looking at his reflection. When someone stared at him, he felt that he was being ridiculed. However, if the looks and stares were accompanied by flattery, his discomfort would diminish.
As an adult, Mr A was hospitalized for assessment of shortness of breath; there, he was the subject of morning rounds. Having all eyes focused on him made Mr A feel self-conscious and criticized and he became less open in his responses and less willing to volunteer information that may have been helpful to his care. Despite a successful professional and personal life, his body image as an adult reflected his early response to trauma and disfigurement.
WHAT IS BODY IMAGE?
Body image involves perceptions, thoughts, and behaviors related to one’s appearance. For example, Mr A’s body image was dominated by having been a child with a scarred face. When a patient’s world view or body image adversely impacts the provision of health care, primary care physicians should place such views in perspective and adjust care plans. Mr A’s discomfort during rounds (manifest by terse responses) led to a strategy that eased his dysphoria (eg, by commenting positively on his appearance, for example, “You’ re looking good today, how do you feel?”). Such insight and action might have enabled Mr A to be more forthcoming and helpful to his caregivers. In this way, knowledge of body image can affect care.
Body image must be differentiated from “self-esteem” and “quality of life,” as these latter 2 concepts encompass not only appearance but also one’s relationships, religious views, culture, career, and values. However, body image often influences both self-esteem and quality of life. Nonetheless, changes in body image do not always reflect changes in self-esteem and quality of life, and our vignette demonstrates that positive self-esteem and a good quality of life do not necessarily imply a positive body image.1 Despite the fact that Mr A overcame his shyness as an adult, his core identity and body image failed to change over time.
WHEN IS BODY IMAGE ESTABLISHED?
Typically, body image is established before the age of 6 years. By this age, children are aware of their own appearance and of the societal bias against people with certain body types (eg, obesity),2 and children who are overweight tend to internalize this message. During early adolescence, body image continues to develop, especially among girls (when they gain an average of 50 lb, 20%-30% of which is comprised of fat deposited in the hips, thighs, buttocks, and waist).3
In addition to biologic developmental processes, external factors (eg, trauma, cultural influences, exposure to the media, relationships, and life experiences) affect body image. In the case of Mr A, his body image was affected by teasing he experienced following disfigurement. Although during his adolescence and adulthood he was not referred to by his childhood nickname, his body image (of a scarred person) persisted, despite educational and professional successes. Attention paid to body image can affect the delivery of care.
HOW IS BODY IMAGE ASSESSED?
At times, simply asking a person about his or her world view (eg, optimistic, pessimistic, confident, insecure, attractive, or unappealing) will start the dialogue between physician and patient regarding body image. For example, a late-developing teenaged boy may feel like a short person even though by the end of college he has grown to a height of 6 ft 8 in. Or, a chronically overweight child still feels “fat” and unattractive despite development of a sculpted body during high school. Fortunately, a variety of quantifiable measures are available for the assessment of body image in children, adolescents, and adults. Each age group requires a different measure, as each faces different developmental tasks. Table 1 provides a list of measurements related to body image in children.4-9
The most commonly measured attitudinal component of body image is dissatisfaction with body size4; human figure drawings have been particularly helpful for such assessments (especially in those who lack sophisticated language skills). Silhouettes that represent the body (from being very underweight to very overweight) have also been employed. In these tests, individuals are asked to select the figure that represents their current size and the size they would like to be.4
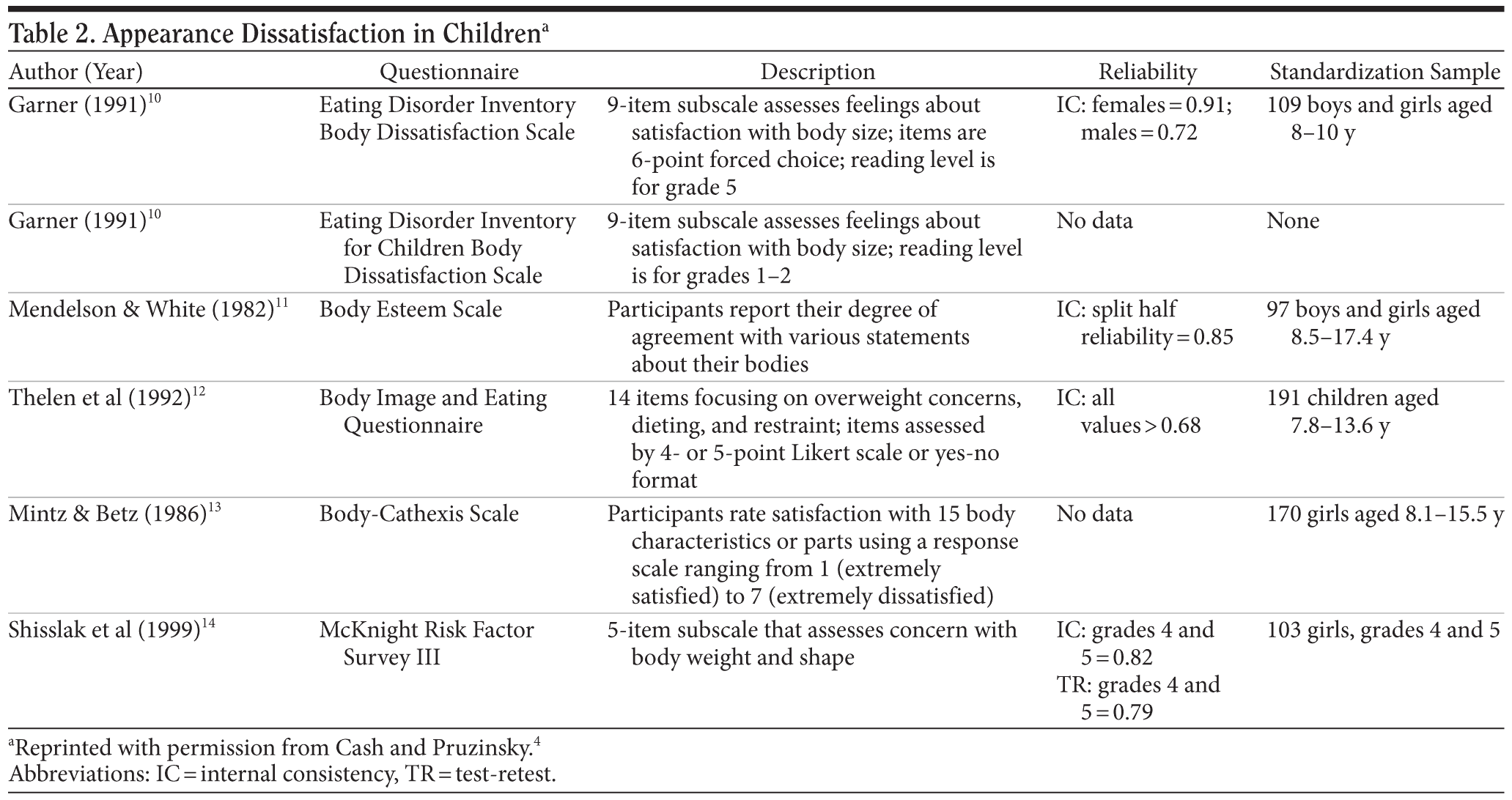
Assessment of attitudes must be contrasted with dissatisfaction with appearance; tools for measurement of these factors are listed in Table 2.4,10-14 Dissatisfaction with appearance reflects values, eg, how much satisfaction or dissatisfaction exists.
Unfortunately, some of the measures listed in Table 2 are global, whereas others are specifically related to dissatisfaction with different parts of the body; optimal assessment of body image should include both global and specific measures. In a medical context, a patient’s affect, behavior, and cognition are often oversimplified; at times, a more thorough assessment of body image is needed.
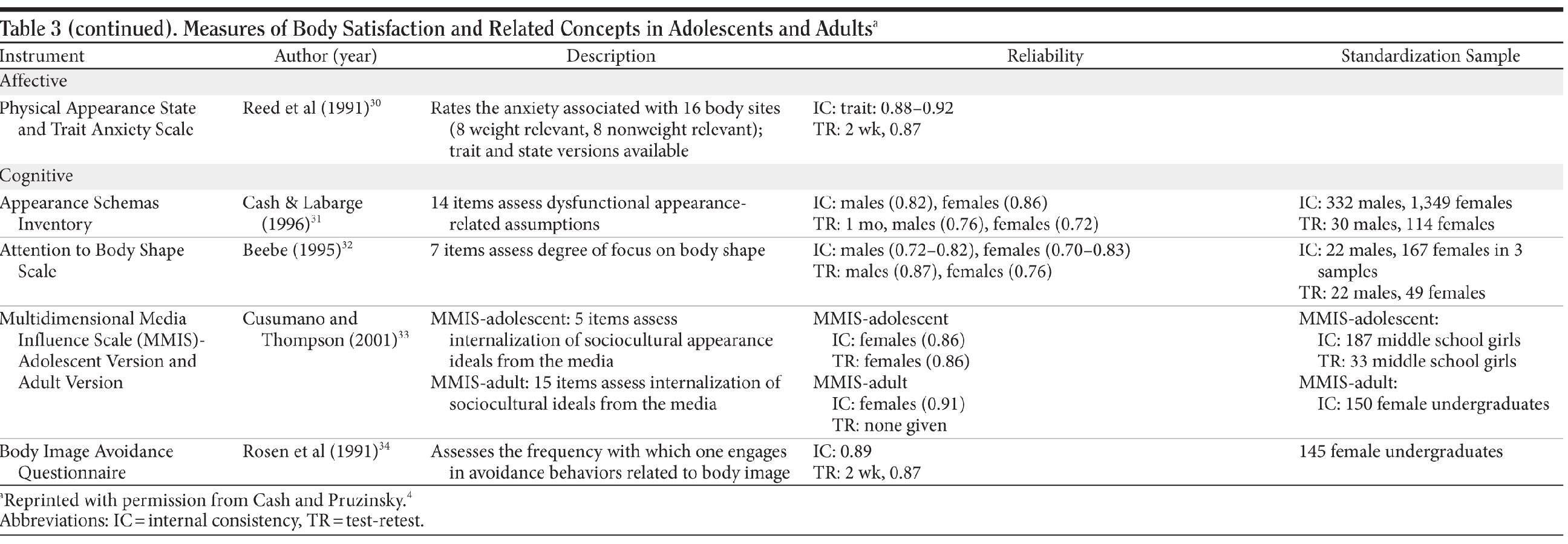
Table 3 provides measures of body satisfaction.4,15-34 Some activities and concerns (eg, sexual activity, peer pressure, and fashion) are more important for adolescents and adults than for children. When social interactions or adherence with care are less than optimal, assessment of body image may improve doctor-patient communications and patient behaviors.
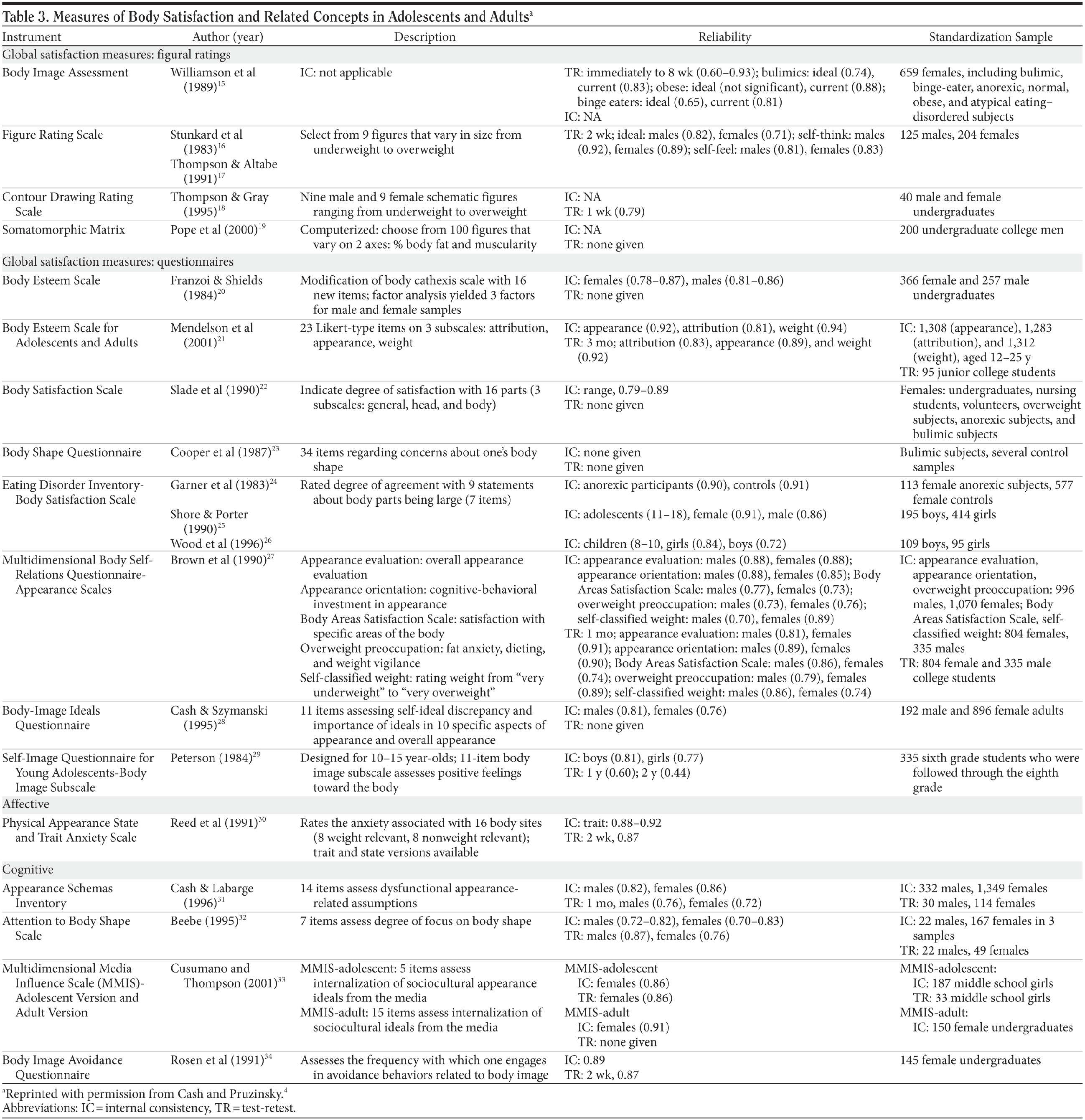
Body image measurement requires that the term satisfaction be further broken down into satisfaction (eg, with weight, shape, and specific body areas) as well as severity (eg, of the body image disturbance); measurement should be multimodal.
WHY IS IT IMPORTANT TO KNOW ABOUT A PATIENT’ S BODY IMAGE?
A patient’s response to illness can be affected by many variables (including how he or she looks, behaves [eg, withdrawn, noncompliant, aggressive, or retaliatory], and thinks). Changes in physical appearance, function, and body integrity are typically central to the experience of illness and to medical treatment. Unfortunately, dissatisfaction with body image has become more prevalent since the early 1970s,4 possibly due to an increase in the influence of the media.
HOW CAN A PHYSICIAN ASSESS AND MANAGE CHANGES IN BODY IMAGE?
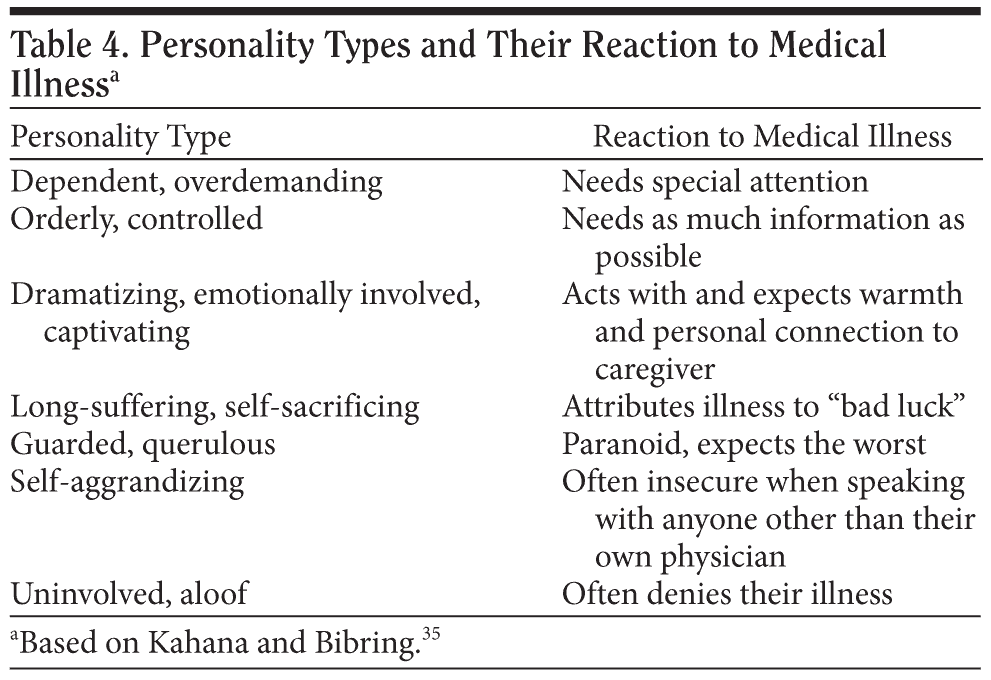
Several decades ago, Kahana and Bibring35 embarked on development of a strategy to help physicians manage patients with different reactions to medical illness (Table 4). They advised that under stress, patients tend to exaggerate the behaviors linked with their personality style; knowledge of prototypical reactions can be used in connection with body image to deliver more comprehensive care.35
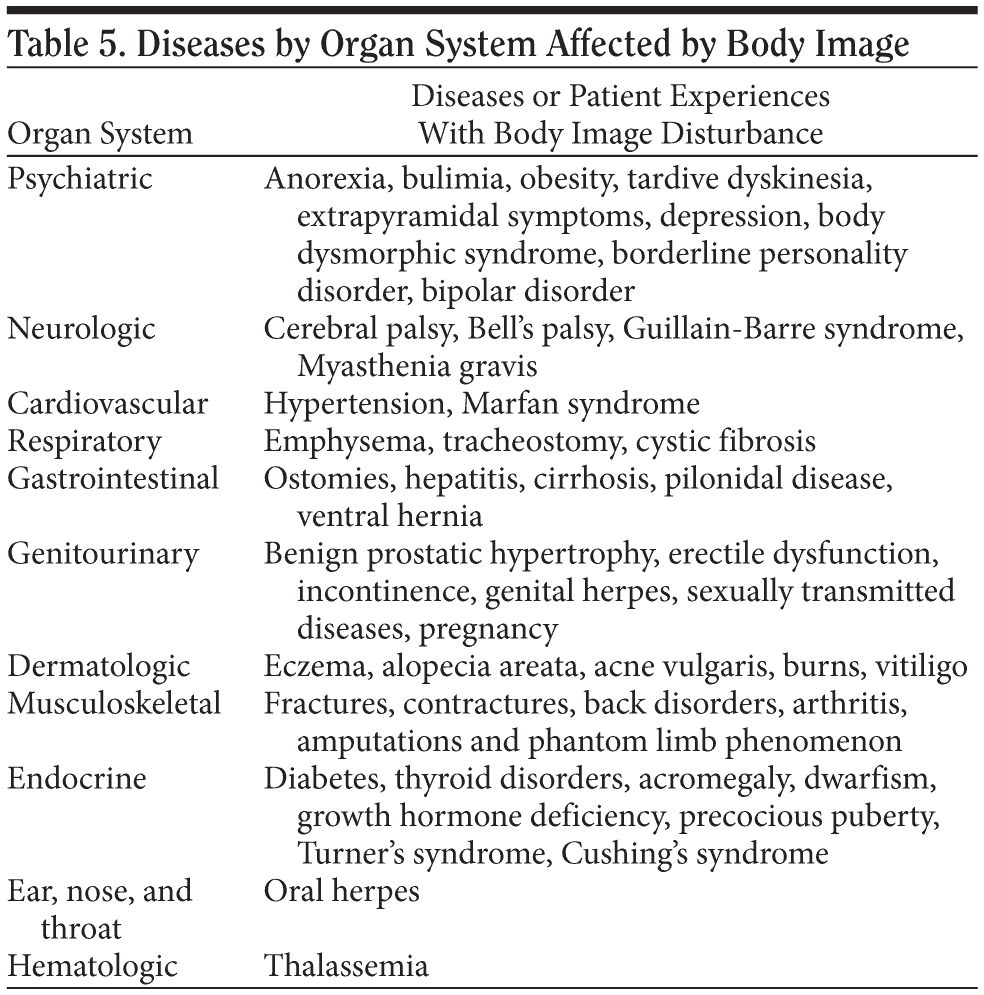
Additional tools, eg, the patient’s health-related quality of life index can be maximized when one distinguishes between a patient who does and does not have a body image concern.4,36,37 Individual differences also play a role, as not all patients with a specific condition manifest the same body image. Table 5 lists categories of diseases (organized by organ system) that commonly produce disturbances in body image.
In addition to the diseases listed in Table 5, other conditions (eg, trauma, cancer, infection, and aging) affect health and body image. Each has the capacity to change appearance and bodily integrity and therefore body image. These changes also affect how others treat the afflicted person, and this is often a significant source of distress.
Appearance-related distress occurs not only because of a change of appearance but also because it is a persistent reminder of the disease (especially when changes in appearance are accompanied by functional changes [eg, loss of function or changes in bowel habits]). The speed with which these changes occur can also be a factor, as it affects accommodation to the change. Some conditions will be accompanied by changes in sensory perceptions (eg, phantom limb sensations and pain).
Conditions that are highly visible to strangers (eg, loss of an eye, loss of a limb, and facial scars) cause more distress than those that are hidden. External devices (eg, ileostomy bags, tracheostomy tubes, and prosthetic devices) can also cause body image distress and affect the patient’s overall feeling about appearance. Drugs (eg, chemotherapy, antipsychotics, and steroids) can also cause changes in appearance that may be more disturbing to a patient than their more commonly known side effects (eg, nausea and fatigue). Therefore, physicians should learn how to identify and manage reactions to these effects. For example, when children with cancer perceive their physical appearance more positively, they tend to be less depressed, to be less socially anxious, and to have higher self-esteem.38
WHAT ARE SOME COMMON DISORDERS CAUSED BY BODY IMAGE DISTURBANCE?
Thus far, we have discussed life experiences, medical conditions, and medications that may lead to body image changes. For example, trauma, endocrine disorders, cancer, steroid treatment, and antidepressants commonly lead to changes in appearance that may lead to body image disturbance. In the previous examples, the body image disturbance is the effect of an antecedent life experience, medical condition, or treatment. However, we would like to also present some common disorders wherein the cause and effect are reversed. That is to say, body image is the cause rather than the effect, and the result is a body image disorder according to the DSM-IV-TR.39 These disorders are anorexia nervosa, bulimia nervosa, and body dysmorphic disorder, also known as dysmorphophobia. While a comprehensive presentation of each disease is beyond the scope of this article, we will focus on those aspects relevant to primary care physicians who may encounter these patients and refer them to mental health professionals. Key considerations will include issues related to assessment, referral, and treatment.
ANOREXIA NERVOSA
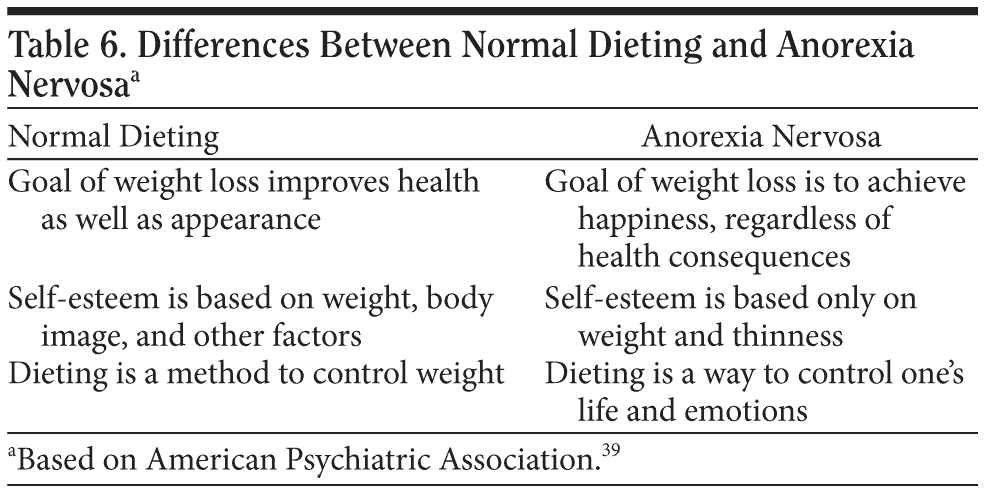
According to the DSM-IV-TR,39 anorexia nervosa is characterized by “an intense fear of gaining weight or becoming fat, even though underweight” and “disturbance in the way in which one’s body weight or shape is experienced, undue influence of body weight or shape on self-evaluation, or denial of the seriousness of current low body weight.”39(p589) The body image disturbance in anorexia is so significant that even after weight restoration, the majority of patients with anorexia nervosa continue to worry excessively about body weight and shape.40 The anorexic patient restricts calories, but there is a significant difference between the normal dieter and the patient with anorexia; the anorexic patient places supreme importance on his or her appearance. Table 6 shows the difference between the characteristics of the normal dieter and the patient with anorexia nervosa.39
The clinician should note that anorexic patients often are emaciated and have electrolyte disturbances, thinning hair, amenorrhea, and dry skin (due to electrolyte disturbances and malnutrition). Therefore, when requesting a psychiatric consultation, it is helpful to consider abnormal laboratory values and whether the patient, if female, is menstruating normally. Treatment of anorexia nervosa involves size estimation feedback and cognitive-behavioral therapy aimed at reinterpreting the body image disturbance, rather than on trying to completely change it. The physician also needs to be aware that patients with anorexia often present with severe electrolyte imbalances; these abnormalities need to be measured and corrected as necessary.
BULIMIA NERVOSA
Similar to the case of anorexia, bulimia nervosa is preceded by a similar body image disturbance and fear of becoming fat; afflicted patients control this fear by purging, by taking laxatives, or by exercising after binge eating. Primary care physicians should be aware that bulimic patients are at increased risk for the development of comorbid conditions (eg, obesity, substance abuse, and major depression).39 Unlike the anorexic patient, the patient with bulimia consumes large amounts of calories, then tries to “undo” the eating by a variety of methods (as mentioned above). The primary care physician should inform his or her patient that purging only eliminates up to 50% of the calories consumed, but usually much less. Laxatives and diuretics are minimally effective due to the fact that the weight loss achieved is mostly water.
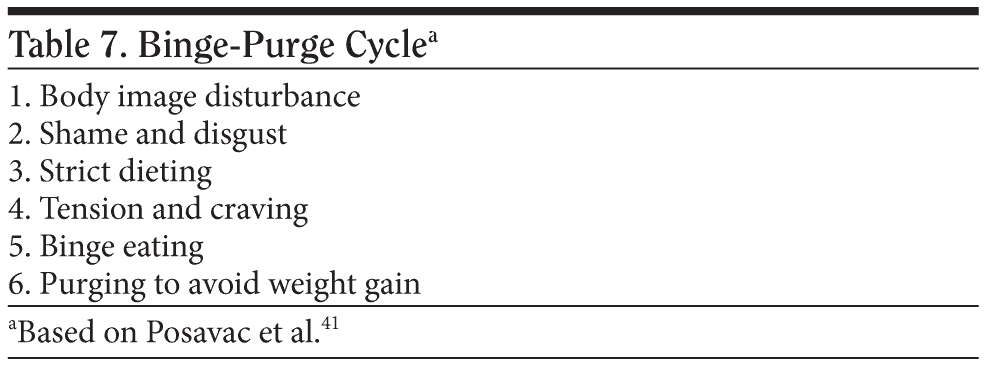
It is helpful to assess for the effects of acidic vomitus on the bulimic’s teeth as a primary sign. Other signs for the physician, friends, and family of the patient include going to the bathroom after meals, using laxatives excessively, using diuretics or enemas, exercising compulsively, or developing scars on the knuckles from putting fingers in the mouth to induce vomiting. When requesting a psychiatric consultation for a bulimic patient, the presence of these comorbidities will be important. Table 7 lists the sequence of the binge-purge cycle that sustains bulimia.41
The treatment of choice for bulimia is cognitive-behavioral therapy aimed at breaking the binge-purge cycle, as well as changing unhealthy thoughts and patterns. Antidepressants are also used in the treatment of bulimia. Posavac and associates41 found that brief interventions helped women become more critical of media messages and reduced the adverse effects of exposure to thin ideal images.
BODY DYSMORPHIC DISORDER
Body dysmorphic disorder involves a preoccupation with an imagined defect in appearance.39 For example, when an objectively slight physical anomaly is present, the patient with body dysmorphic disorder has a markedly excessive concern. The patient’s preoccupation causes clinically significant distress or impairment in social, occupational, or other areas of function not better accounted for by another mental disorder. As in anorexia and bulimia, a body image disturbance precedes the disease. The most common territories of concern for the patient involve the face (more specifically the hair, skin, and nose). Most afflicted patients have low self-esteem, shame, embarrassment, unworthiness, and a fear of rejection. Patients often perform repetitive, time-consuming, and compulsive behaviors to inspect, hide, or fix the perceived defect. Ironically, although the goal of these behaviors is to diminish the anxiety provoked by the body image concerns, these behaviors often increase and maintain the anxiety. Table 8 lists some of the behaviors associated with body dysmorphic disorder.39 These behaviors are abnormal in both a qualitative and quantitative manner.
When requesting a psychiatric consultation for body dysmorphic disorder, it is helpful to know whether the patient has received plastic surgery or dermatologic treatments. In fact, one reason that body dysmorphic disorder has been underdiagnosed is because affected patients seek nonpsychiatric treatment (eg, cosmetic surgery, dermatologic therapy) and are reluctant to reveal concerns about their appearance due to feelings of shame.42 Since body dysmorphic disorder has been omitted from previous versions of the DSM, it has been more difficult for some clinicians to recognize. Treatment of body dysmorphic disorder, like bulimia, involves cognitive-behavioral therapy and antidepressants. Other adjunctive therapies (eg, supportive psychotherapy and insight-oriented psychotherapy) have been tried, but there are little data to support their efficacy.42
Body image changes can result from medical, surgical, or traumatic conditions and may be the cause of others (eg, anorexia, bulimia, and body dysmorphic disorder).
HOW CAN WE MANAGE BODY IMAGE DISTURBANCE?
Disfigurement can be divided into 2 groups: objective (true disfigurement) and subjective (perception of disfigurement); their management may differ. Patients can correct a defect with surgery or learn to hide the defect. However, if a patient believes that he or she is disfigured, but does not have a true disfigurement, it may help to reframe his or her experience (eg, by seeing someone else with a similar defect and learning how he or she copes with it).
In addition to accurate assessment, optimal management of body image may include pharmacologic interventions for anxiety or depression. Behavioral modification can also be used to teach coping skills and relaxation techniques. Physical modification of the body (eg, via plastic surgery, weight gain, weight loss, and muscle building) may also be used. In short, problem solving on many levels (eg, psychological, emotional, medical, physical, spiritual, and cultural) may be required to assist with body image management.
CONCLUSION
When considering body image, it may be helpful to remember the often-used phrases: “beauty is in the eyes of the beholder,” “beauty is only skin deep,” and “never judge a book by its cover.” These expressions take on new meaning when considering body image vis-× -vis its role in the mediation of reactions to physical conditions. Body image develops relatively early in life and can be measured in children, adolescents, and adults with a variety of scales (from both global and body area-specific perspectives). Since many disease processes, medical and surgical interventions, and possibly patient factors contribute to changes in body image, assessment and management of body image facilitate positive patient experiences and outcomes.
REFERENCES
1. Bolton MA, Pruzinsky T, Cash TF, et al. Measuring outcomes in plastic surgery: body image and quality of life in abdominoplasty patients. Plast Reconstr Surg. 2003;112(2):619-625, discussion 626-627.doi:10.1097/01.PRS.0000070972.57000.08 PubMed
2. Smolak L, Levine MP. Body image in children In: Thompson JK, Smolak L, eds. Body Image, Eating Disorders, and Obesity in Youth: Assessment, Prevention, and Treatment. Washington, DC: American Psychological Association; 2001;41-66. doi:10.1037/10404-002
3. Graber JA, Peterson AC, Brooks-Gunn J. Pubertal processes: methods, measures, and models. In: Graber JA, Brooks-Gunn J, Peterson AC, eds. Transitions Through Adolescence: Interpersonal Domains and Context. Mahwah, NJ: Erlbaum; 1996:23-53.
4. Cash TF, Pruzinsky T, eds. Body Image: A Handbook of Theory, Research, and Clinical Practice. New York, NY: Guilford Press; 2004.
5. Collins M. Body figure perceptions and preferences among pre-adolescent children. Int J Eat Disord. 1991;10(2):191-208. doi:10.1002/1098-108X(199103)10:2<199::AID-EAT2260100209>3.0.CO;2-D
6. Childress A, Brewerton T, Hodges E, et al. The Kids’ Eating Disorders Survey (KEDS): a study of middle school students. J Am Acad Child Psy. 1993;32:841-850.
7. Veron-Guidry S, Williamson DA. Development of a body image assessment procedure for children and preadolescents. Int J Eat Disord. 1996;20(3):287-293. doi:10.1002/(SICI)1098-108X(199611)20:3<287::AID-EAT8>3.0.CO;2-K PubMed
8. Sands R, Tricker J, Sherman C, et al. Disordered eating patterns, body image, self-esteem, and physical activity in pre-adolescent school children. Int J Eat Disord. 1997;21:151-166.
9. Tiggemann M, Pennington B. The development of gender differences in body-size dissatisfaction. Australian Psychiatrist. 1990;25:301-311.
10. Garner DM. Eating Disorder Inventory for Children (EDI-C). Odessa, FL: Psychological Assessment Resources; 1991.
11. Mendelson BK, White DR. Relation between body-esteem and self-esteem of obese and normal children. Percept Mot Skills. 1982;54(3):899-905. PubMed
12. Thelen M, Powell A, Lawrence C, et al. Eating and body image concerns among children. J Clin Child Psychol. 1992;21(1):41-46. doi:10.1207/s15374424jccp2101_7
13. Mintz L, Betz N. Sex differences in the nature, realism, and correlates of body image. Sex Roles. 1986;15(3-4):185-195. doi:10.1007/BF00287483
14. Shisslak CM, Renger R, Sharpe T, et al. Development and evaluation of McKnight Risk Factor Survey for assessing potential risk and protective factors for disordered eating in pre-adolescent and adolescent girls. Int J Eat Disord. 1999;25(2):191-214. doi:10.1002/(SICI)1098-108X(199903)25:2<195::AID-EAT9>3.0.CO;2-B
15. Williamson DA, Davis CJ, Bennett SM, et al. Development of a simple procedure for assessing body image disturbances. Behav Assess. 1989;11:433-446.
16. Stunkard AJ, Sorenson TI, Schulsinger F. Use of the Danish Adoption Register for the study of obesity and thinness. In: Kety S, Rowland LP, Sidman RL, et al, eds. The Genetics of Neurological and Psychiatric Disorders. New York, NY: Raven Press; 1983:115-120.
17. Thompson JK, Altabe NM. Psychometric qualities of Figure Rating Scale. Int J Eat Disord. 1991;10(5):615-619. doi:10.1002/1098-108X(199109)10:5<615::AID-EAT2260100514>3.0.CO;2-K
18. Thompson MA, Gray JJ. Development and validation of a new body-image assessment scale. J Pers Assess. 1995;64(2):258-269. doi:10.1207/s15327752jpa6402_6 PubMed
19. Pope HG Jr, Gruber AJ, Mangweth B, et al. Body image perception among men in three countries. Am J Psychiatry. 2000;157(8):1297-1301. doi:10.1176/appi.ajp.157.8.1297 PubMed
20. Franzoi SL, Shields SA. The Body Esteem Scale: multidimensional structure and sex differences in a college population. J Pers Assess. 1984;48(2):173-178. doi:10.1207/s15327752jpa4802_12 PubMed
21. Mendelson BK, Mendelson MJ, White DR. Body-esteem scale for adolescents and adults. J Pers Assess. 2001;76(1):90-106. doi:10.1207/S15327752JPA7601_6 PubMed
22. Slade PD, Dewey ME, Newton T, et al. Development and preliminary validation of the Body Dissatisfaction Scale (BSS). Psychol Health. 1990;4(3):213-220. doi:10.1080/08870449008400391
23. Cooper PJ, Taylor MJ, Cooper Z, et al. The development and validation of the Body Shape Questionnaire. Int J Eat Disord. 1987;6(4):485-494. doi:10.1002/1098-108X(198707)6:4<485::AID-EAT2260060405>3.0.CO;2-O
24. Garner DM, Olmested MP, Polivy J. Development and validation of a multi-dimensional eating disorder inventory for anorexia nervosa and bulimia. In J. Eat Disord. 1983;2(2):15-34. doi:10.1002/1098-108X(198321)2:2<15::AID-EAT2260020203>3.0.CO;2-6
25. Shore RA, Porter JE. Normative and reliability data for 11- to 18-year-olds on the Eating Disorder Inventory. Int J Eat Disord. 1990;9(2):201-207. doi:10.1002/1098-108X(199003)9:2<201::AID-EAT2260090209>3.0.CO;2-9
26. Wood KC, Becker JA, Thompson JK. Body image dissatisfaction in preadolescent children. J Appl Dev Psychol. 1996;17(1):85-100. doi:10.1016/S0193-3973(96)90007-6
27. Brown TA, Cash TF, Mikulka PJ. Attitudinal body-image assessment: factor analysis of the Body-Self Relations Questionnaire. J Pers Assess. 1990;55(1-2):135-144. doi:10.1207/s15327752jpa5501&2_13 PubMed
28. Cash TF, Szymanski ML. The development and validation of the Body-Image Ideals Questionnaire. J Pers Assess. 1995;64(3):466-477. doi:10.1207/s15327752jpa6403_6 PubMed
29. Peterson AC. A Self-Image Questionnaire for Young Adolescents (SIQYA): Reliability and validity studies. J Youth Adolesc. 1984;13(2):93-111. doi:10.1007/BF02089104
30. Reed DL, Thompson JK, Brannick MT, et al. Development and validation of the Physical Appearance State and Trait Anxiety Scale (PASTAS). J Anxiety Disord. 1991;5(4):323-332. doi:10.1016/0887-6185(91)90032-O
31. Cash TF, Labarge AS. Development of the Appearance Schemas Inventory: a new cognitive body-image assessment. Cognit Ther Res. 1996;20(1):37-50. doi:10.1007/BF02229242
32. Beebe DW. The attention to body shape scale: a new measure of body focus. J Pers Assess. 1995;65(3):486-501. doi:10.1207/s15327752jpa6503_8 PubMed
33. Cusumano DL, Thompson JK. Media influence and body image in 8-11-year-old boys and girls: a preliminary report on the multidimensional media influence scale. Int J Eat Disord. 2001;29(1):37-44. doi:10.1002/1098-108X(200101)29:1<37::AID-EAT6>3.0.CO;2-G PubMed
34. Rosen JC, Srebnik D, Saltzberg E, et al. Development of a body image avoidance questionnaire. Psychol Assess. 1991;3(1):32-37. doi:10.1037/1040-3590.3.1.32
35. Kahana RJ, Bibring GL. Personality types in medical management. In: Zinberg NE, ed. Psychiatry and Medical Practice in a General Hospital. New York, NY: International Universities Press; 1964:108-123.
36. Dimsdale JE, Baum A, eds. Quality of Life in Behavioral Medicine Research. Mahwah, NY: Erlbaum; 1995.
37. Harter S. The Construction of the Self: A Developmental Perspective. New York, NY: Guilford Press; 1999.
38. Varni JW, Katz ER, Colegrove R Jr, et al. Perceived physical appearance and adjustment of children with newly diagnosed cancer: a path analytic model. J Behav Med. 1995;18(3):261-278.doi:10.1007/BF01857873 PubMed
39. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
40. Cash TF, Deagle EA 3rd. The nature and extent of body-image disturbances in anorexia nervosa and bulimia nervosa: a meta-analysis. Int J Eat Disord. 1997;22(2):107-125.doi:10.1002/(SICI)1098-108X(199709)22:2<107::AID-EAT1>3.0.CO;2-J PubMed
41. Posavac HD, Posavac SS, Weigel RG. Reducing the impact of media images on women’s body image disturbance: three targeted interventions. J Soc Clin Psychol. 2001;20(3):324-340. doi:10.1521/jscp.20.3.324.22308
42. Phillips KA. Body image and body dysmorphic disorder. In: Fariburn CG, Brownell KD, eds. Eating Disorders and Obesity: A Comprehensive Handbook. 2nd ed. New York, NY: Guilford Press; 2002:113-117.