Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
Have you ever treated an adult patient who was acting like a child? Has one of your patients thrown a temper tantrum when he or she was under distress? Have you wondered what could have caused such behavior and how it should be managed?
Impact of the Doctor-Patient Relationship
Have you ever wondered what makes the doctor-patient relationship so powerful? Have you ever considered what you could do to strengthen it or to prevent it from crumbling? Have you thought about the consequences of unsatisfactory or adversarial relationships? If you have, then the following case vignettes and discussion should prove useful.
CASE VIGNETTE 1
Mr A, a 43-year-old man with a 20-year history of intravenous drug abuse (complicated by hepatitis C and recurrent abscesses), was admitted to the hospital for treatment of acute bacterial endocarditis. His inpatient medical team consulted the addictions consult/substance abuse team, who evaluated and enrolled him in an outpatient methadone clinic. Mr A noted that prior to this assessment he had never had a “decent” conversation about addiction treatment.
CASE VIGNETTE 2
Ms B, a 75-year-old woman with an alcohol use disorder and gastroesophageal reflux disorder, presented to the oncology clinic following her new (incidental) diagnosis of gastric carcinoma. During the visit, the oncologist explained the importance of assessing the depth of the tumor’s invasion into the gastric wall (ie, to stage the tumor and to decide on treatment options). He noted that if the tumor was confined to the most superficial layer of the stomach, it could be excised during an endoscopy. If the tumor went deeper, Ms B would need radiation and/or chemotherapy or surgery. The oncologist arranged for an immediate visit by the surgeon, who informed her that the cancer would almost certainly be invasive and that he planned to remove a large part of her stomach. He described her surgery as very serious, but necessary, because her cancer was very likely to lead to death. As the surgeon turned to write his note in the electronic medical record, Ms B began to shake her head from side to side and cry.
WHY IS THE DOCTOR-PATIENT RELATIONSHIP SO IMPORTANT?
The doctor-patient relationship involves vulnerability and trust. It is one of the most moving and meaningful experiences shared by human beings. However, this relationship and the encounters that flow from it are not always perfect.
The doctor-patient relationship has been defined as “a consensual relationship in which the patient knowingly seeks the physician’s assistance and in which the physician knowingly accepts the person as a patient.”1(p6) At its core, the doctor-patient relationship represents a fiduciary relationship in which, by entering into the relationship, the physician agrees to respect the patient’s autonomy, maintain confidentiality, explain treatment options, obtain informed consent, provide the highest standard of care, and commit not to abandon the patient without giving him or her adequate time to find a new doctor. However, such a contractual definition fails to portray the immense and profound nature of the doctor-patient relationship. Patients sometimes reveal secrets, worries, and fears to physicians that they have not yet disclosed to friends or family members. Placing trust in a doctor helps them maintain or regain their health and well-being.
This unique relationship encompasses 4 key elements: mutual knowledge, trust, loyalty, and regard.2 Knowledge refers to the doctor’s knowledge of the patient as well as the patient’s knowledge of the doctor. Trust involves the patient’s faith in the doctor’s competence and caring, as well as the doctor’s trust in the patient and his or her beliefs and report of symptoms. Loyalty refers to the patient’s willingness to forgive a doctor for any inconvenience or mistake and the doctor’s commitment not to abandon a patient. Regard implies that the patients feel as though the doctor likes them as individuals and is “on their side.” These 4 elements constitute the foundation of the doctor-patient relationship.
WHAT IS THE STRUCTURE OF THE
DOCTOR-PATIENT RELATIONSHIP?
In their seminal article from 1956, Szasz and Hollender3 outlined 3 basic models of the doctor-patient relationship.
Active-Passive Model
The active-passive model is the oldest of the 3 models. It is based on the physician acting upon the patient, who is treated as an inanimate object. This model may be appropriate during an emergency when the patient may be unconscious or when a delay in treatment may cause irreparable harm. In such situations, consent (and complicated conversations) is waived.
Guidance-Cooperation Model
In the guidance-cooperation model, a doctor is placed in a position of power due to having medical knowledge that the patient lacks. The doctor is expected to decide what is in the patient’s best interest and to make recommendations accordingly. The patient is then expected to comply with these recommendations.
Mutual Participation Model
The mutual participation model is based on an equal partnership between the doctor and the patient. The patient is viewed as an expert in his or her life experiences and goals, making patient involvement essential for designing treatment. The physician’s role is to elicit a patient’s goals and to help achieve these goals. This model requires that both parties have equal power, are mutually interdependent, and engage in activities that are equally satisfying to both parties.
While each of these models may be appropriate in specific situations, over the last several decades there has been increasing support for the mutual participation model whenever it is medically feasible.4
HOW DOES THE NATURE AND QUALITY
OF THE DOCTOR-PATIENT RELATIONSHIP
AFFECT HEALTH OUTCOMES?
Gordon and Beresin5 asserted that poor outcomes (objective measures or standardized subjective metrics that are assessed after an encounter) flow from an impaired doctor-patient relationship (eg, when patients feel unheard, disrespected, or otherwise out of partnership with their physicians6). Thus, there are many different outcome measures. However, these measures can be divided into 3 main domains: physiologic/objective measures, behavioral measures, and subjective measures. Examples of outcome measures for each of these categories are shown in Table 1.
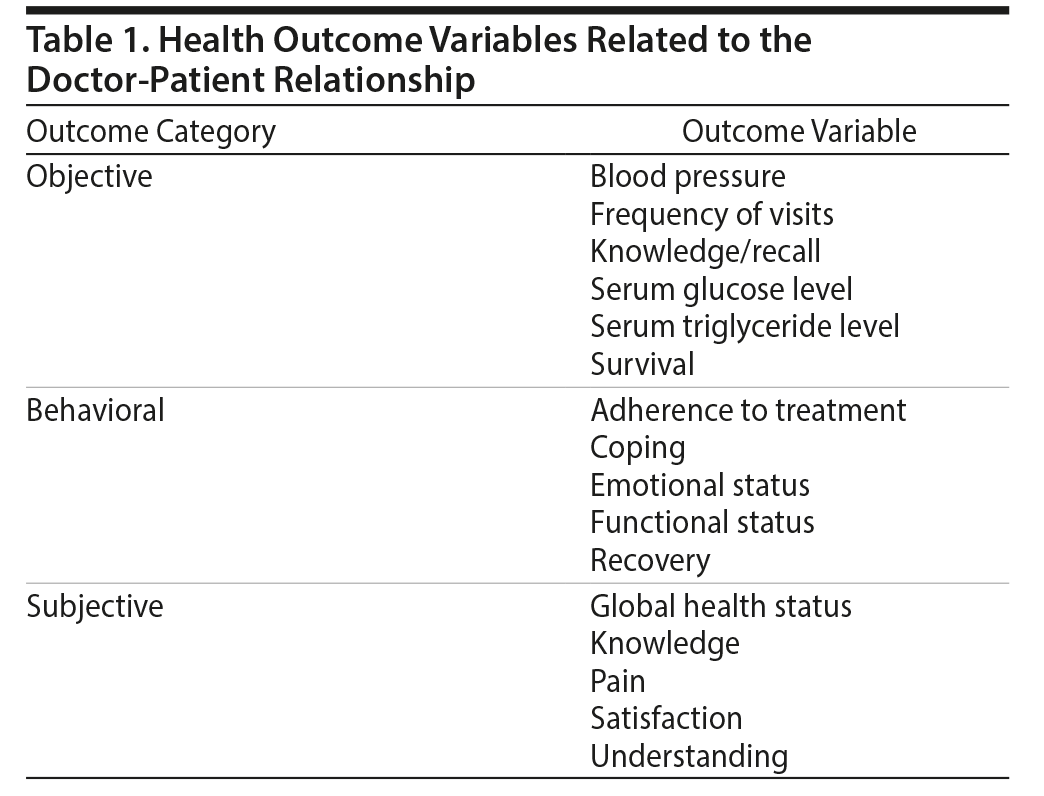
Stewart et al7 noted that the physician’s knowledge of the patient’s ailments and emotional state is associated positively with whether or not those physical ailments resolve. In this instance, the outcome measure is resolution of symptoms (ie, recovery).
In a follow-up meta-analysis of how doctor-patient communication affected outcomes, Stewart8 noted that the quality of communication during history-taking and management also affects outcomes (eg, frequency of visits, emotional health, and symptom resolution) and that such communication extended beyond creation of the “plan.” The manner in which a physician communicates with a patient (even while gathering information) influences how often, and if at all, a patient will return to that same physician.
Furthermore, the quality of communication between doctor and patient involves assessment of the doctor’s willingness to include a patient in the decision-making process, to provide a patient with information programs, and to ask a patient about his or her explanatory model of illness (ie, the perception of the disease as influenced by personal customs and beliefs).9,10
WHAT IS PATIENT SATISFACTION AND HOW IS IT AFFECTED BY THE DOCTOR-PATIENT RELATIONSHIP?
Patient satisfaction is defined as “the degree to which the individual regards the health care service or product or the manner in which it is delivered by the provider as useful, effective, or beneficial.”11 Moreover, all 4 elements of the doctor-patient relationship impact patient satisfaction.
Trust. Bennett et al12 found that, among patients with systemic lupus erythematosus, those who trust and “like” their physician had higher levels of satisfaction. In another study,13 patients’ perceptions of their physician’s trustworthiness were the drivers of patient satisfaction. Knowledge. When doctors discovered patient concerns and addressed patient expectations, patient satisfaction increased as it did when doctors allowed a patient to give information.14,15
Regard. Ratings of a physician’s friendliness, warmth, emotional support, and caring have been associated with patient satisfaction.16–18
Loyalty. Patients feel more satisfied when doctors offer continued support; continuity of care improves patient satisfaction.13,14
WHICH FACTORS CAN ADVERSELY
INFLUENCE THE DOCTOR-PATIENT RELATIONSHIP?
While the attributes and benefits of a favorable doctor-patient relationship have been characterized, few studies have provided solutions for an impaired relationship. Therefore, we propose 4 categories (patient factors, provider factors, patient-provider mismatch factors, and systemic factors) that can interfere with the doctor-patient relationship.
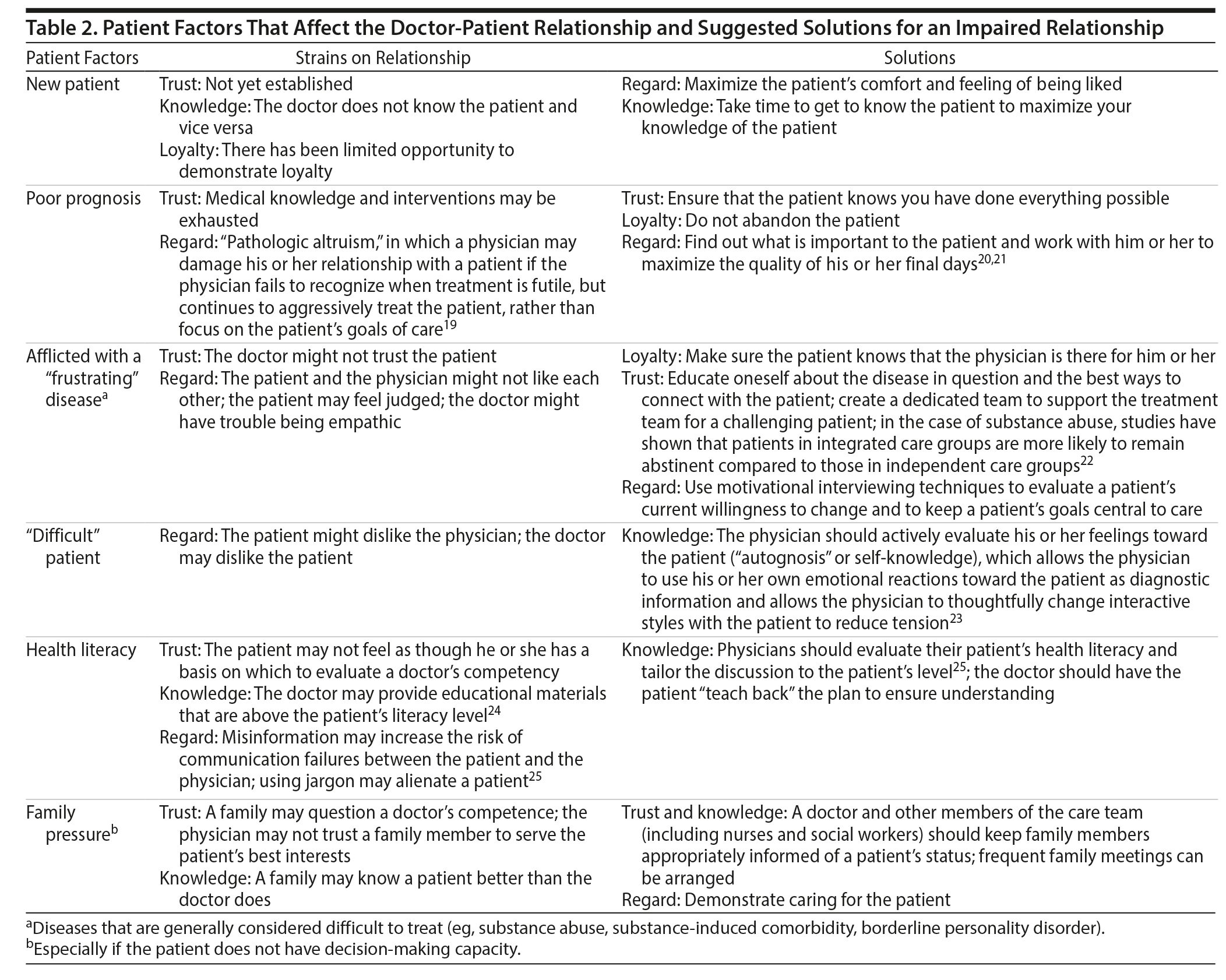
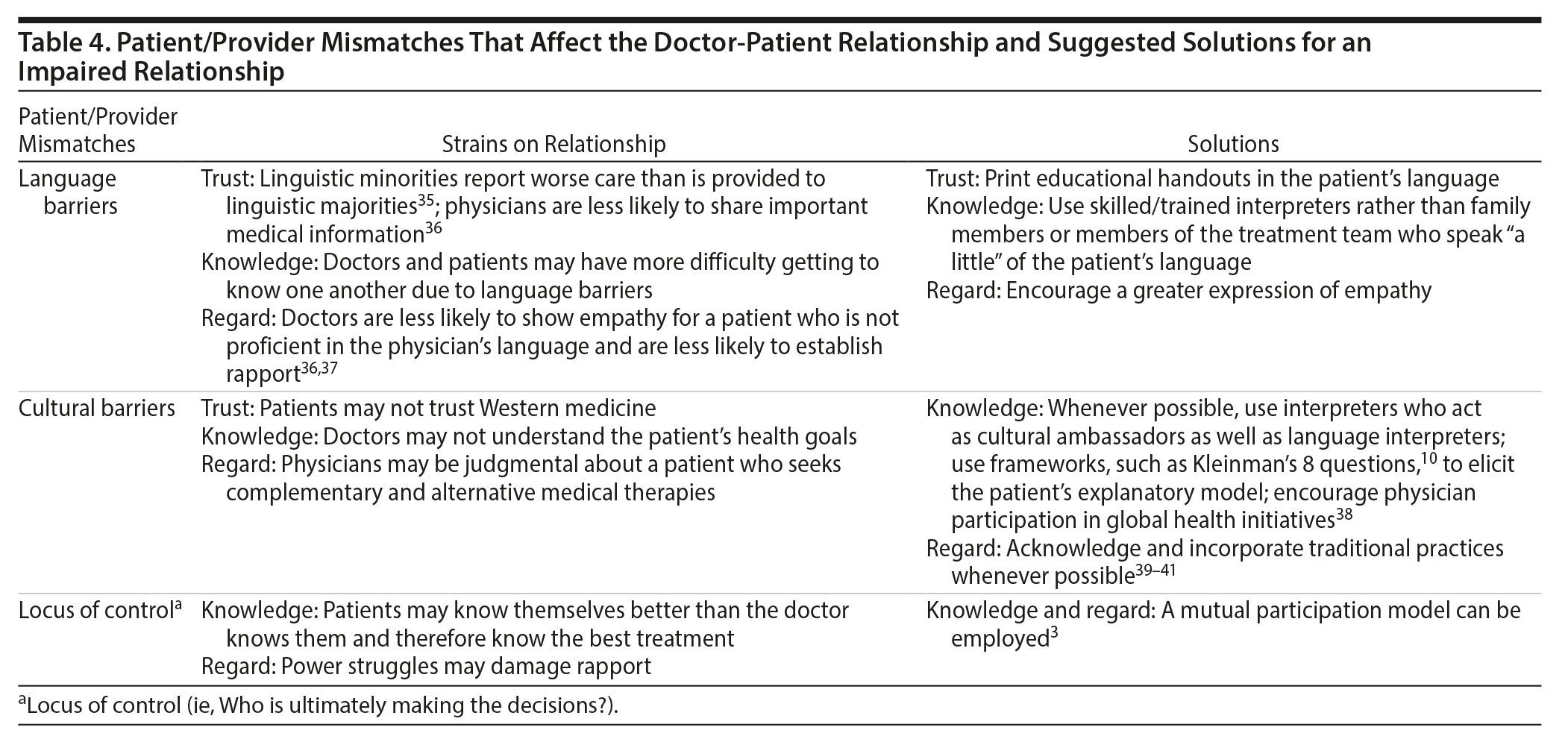
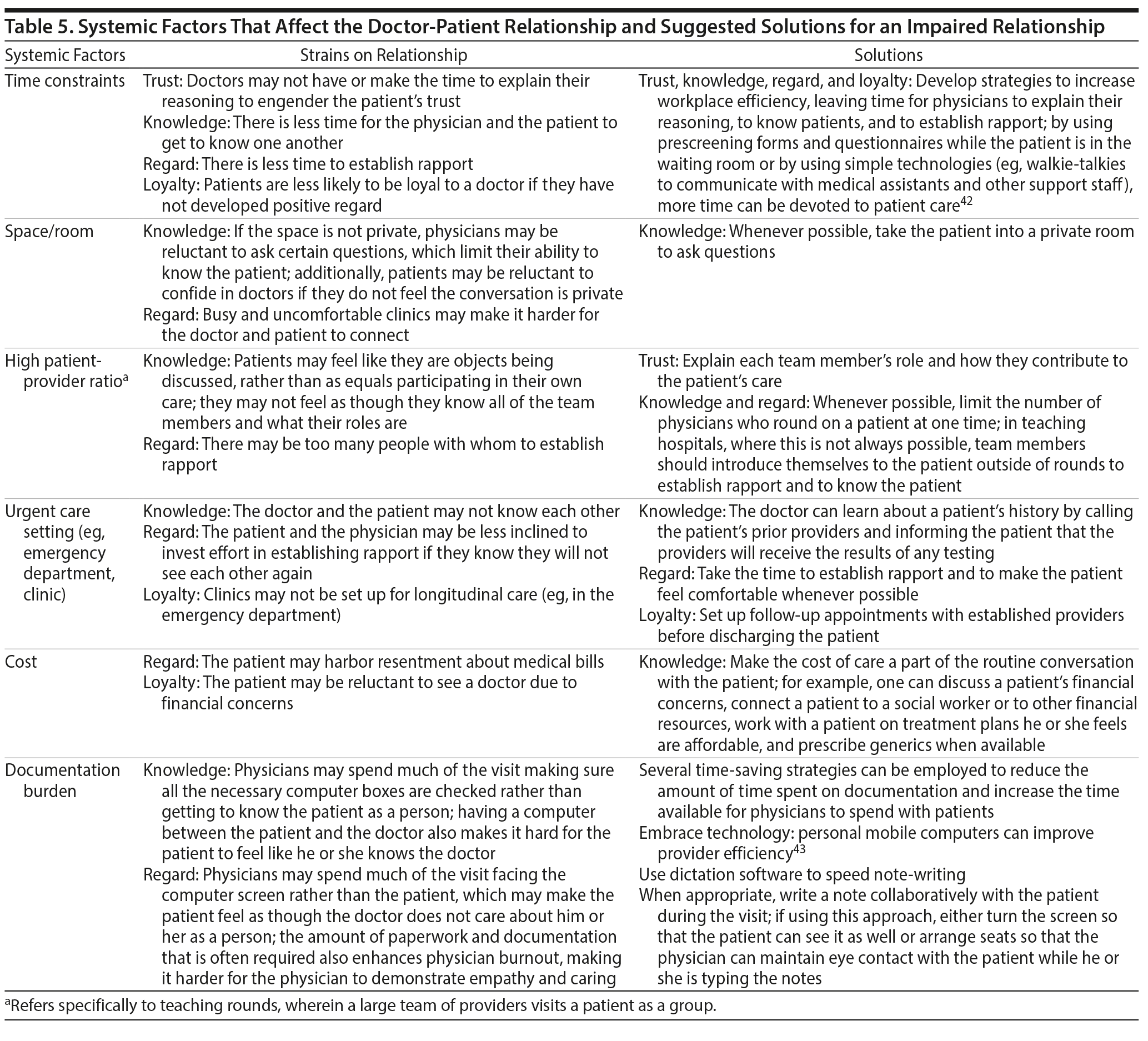
Tables 2–5 summarize the major factors in each of these categories, list elements of the doctor-patient relationship affected by each factor, and propose possible solutions; however, these tables are by no means an exhaustive accounting of the nuances of the doctor-patient relationship.

CASE DISCUSSION
The case of Mr A illustrates an exemplary doctor-patient interaction. He had been hospitalized on multiple occasions with complications (eg, hepatitis C, abscesses, and endocarditis) secondary to his underlying disease (intravenous drug abuse). His medical team made an effort to develop their knowledge of the patient and his disease. Consequently, the team was able to recognize and address his underlying problem. Mr A’s team demonstrated regard for the patient by making him feel that they were “on his side,” and they demonstrated knowledge of his disease, as well of him as a person, resulting in earning his loyalty. Recognizing the gaps in their expertise with regard to addiction management, the medicine team consulted the substance abuse team after Mr A expressed a desire to change his drug use habits in the context of motivational interviewing. Involvement of the substance abuse team is an example of using available resources to overcome the challenge of treating what is generally considered a “frustrating” disease.
Ms B’s case is an example of a failure in the doctor-patient relationship. The oncologist started off well by explaining the upcoming diagnostic steps to the patient. The oncologist built trust by explaining the diagnostic procedures that should be performed to better characterize the nature of the cancer, thus demonstrating her competence and understanding of Ms B’s disease. The oncologist also increased trust by recognizing her own limits by engaging the surgeon’s expertise when needed. However, the interaction between the patient and the surgeon illustrated problems that can arise between the physician and the patient. Since the surgeon had never met the patient before, and the surgeon and the patient had not had a chance to establish trust, neither knew each other and neither had the opportunity to establish loyalty. While it may not be possible for a doctor to develop instant trust and loyalty with a patient (although institutional transference may provide a protective umbrella over the relationship), the doctor in the case of Ms B could have made an effort to demonstrate regard for the patient and to display a desire to know the patient. The surgeon could have started off by asking Ms B open-ended questions about her understanding of her disease, as well as of her fears and expectations regarding her health. This questioning would have allowed the surgeon to create a patient-centered interaction by recognizing and addressing Ms B’s thoughts, concerns, and values. The mutual participation model would have allowed the surgeon to build knowledge of the patient as a person and show regard for her. Ms B’s responses also would have provided the surgeon with information about her level of health literacy, so the surgeon would be better able to target the discussion to her level of understanding.
The surgeon and the oncologist also failed to present a consistent prognosis for Ms B, undermining her trust in the surgeon and the oncologist’s competence and transparency. It is worth acknowledging that sometimes it is difficult to balance the 2 seemingly different roles of a physician: a bearer of bad news that may remove hope versus a healer who cares for and sides with the patient. Neither the surgeon nor the oncologist is necessarily inferior in this context. In fact, the surgeon’s intentions were good. The surgeon was attempting to ensure that Ms B was fully informed of all the different outcomes of the suggested procedure. There are no current screening tests for esophageal/gastric cancer, except in a subpopulation of patients with known Barrett’s esophagus.44 By the time most patients present with symptoms, their disease is well advanced, so the surgeon was right in informing Ms B of the potential severity of her disease. Delivering bad news, especially for a disease with a relatively unfavorable prognosis, will almost always upset any patient. However, the surgeon should have pointed out all the possible outcomes, including that of a superficial malignant lesion, and he should not have sounded so certain about resecting a large portion of Ms B’s stomach, especially prior to endoscopic exploration and disease staging. While the oncologist’s assessment could have been overly optimistic, provision of all the possible outcomes by the oncologist as well as the surgeon would have demonstrated concordance among the physicians, thus allowing Ms B to retain trust in her providers. Additionally, during the initial visit, the surgeon could have simply stated the possibility of the disease’s seriousness, rather than bluntly stating that the disease would most likely be the cause of her demise. The surgeon and oncologist could then reveal more details at subsequent visits when some loyalty had been established and when more information about the extent of her disease was known. Delaying such information until the next visit would not alter staging or management of the disease. The surgeon was right to inform Ms B, but in this context, the manner and the quantity of information divulged ultimately affected the doctor-patient relationship.
Further, distance arose when the surgeon turned away from Ms B at the end of the meeting to complete the visit note. As the documentation burden increases, doctors feel increased pressure to attend to the computer during patient visits, causing face-to-face interaction to suffer. Doctors may unintentionally display a profound lack of empathy by looking at the computer screen instead of at the patient, especially when the patient is experiencing strong emotions. This act of turning away created not only a failure of regard, but also of loyalty. The physician is abandoning the patient to suffer alone despite the physician’s physical presence. In this vignette, the surgeon should have fully addressed Ms B’s emotions before working on the note. In other circumstances, the physician may turn note-writing into a collaborative experience with the patient and encourage the patient to correct or to fill in additional information. If the doctor is writing orders for the patient, it may be useful to explicitly explain to the patient what the physician is doing on the computer so the patient can understand that the physician is using the computer to help to provide better care.
CONCLUSION
As our vignettes intended to illustrate, the doctor-patient relationship is a powerful part of a doctor’s visit and can alter health outcomes for patients. Therefore, it is important for physicians to recognize when the relationship is challenged or failing. If the relationship is challenged or failing, physicians should be able to recognize the causes for the disruption in the relationship and implement solutions to improve care.
REFERENCES
1. QT, Inc v. Mayo Clinic Jacksonville, 2006 US Dist. LEXIS 33668, at *10 (ND Ill May 15, 2006).
2. Ridd M, Shaw A, Lewis G, et al. The patient-doctor relationship: a synthesis of the qualitative literature on patients’ perspectives. Br J Gen Pract. 2009;59(561):e116–e133. doi:10.3399/bjgp09X420248 PubMed
3. Szasz TS, Hollender MH. A contribution to the philosophy of medicine: the basic models of the doctor-patient relationship. AMA Arch Intern Med. 1956;97(5):585–592. doi:10.1001/archinte.1956.00250230079008 PubMed
4. Kaba R, Sooriakumaran P. The evolution of the doctor-patient relationship. Int J Surg. 2007;5(1):57–65. doi:10.1016/j.ijsu.2006.01.005 PubMed
5. Gordon C, Beresin EV. The doctor-patient relationship. In: Stern TA, Fava M, Wilens TE, et al, eds. Massachusetts General Hospital Comprehensive Clinical Psychiatry, 2nd ed. Philadelphia, PA: Elsevier Health Sciences; 2016:1–7.
6. Ong LML, de Haes JCJM, Hoos AM, et al. Doctor-patient communication: a review of the literature. Soc Sci Med. 1995;40(7):903–918. doi:10.1016/0277-9536(94)00155-M PubMed
7. Stewart MA, McWhinney IR, Buck CW. The doctor/patient relationship and its effect upon outcome. J R Coll Gen Pract. 1979;29(199):77–81. PubMed
8. Stewart MA. Effective physician-patient communication and health outcomes: a review. CMAJ. 1995;152(9):1423–1433. PubMed
9. Evans BJ, Kiellerup FD, Stanley RO, et al. A communication skills programme for increasing patients’ satisfaction with general practice consultations. Br J Med Psychol. 1987;60(pt 4):373–378. doi:10.1111/j.2044-8341.1987.tb02756.x PubMed
10. Kleinman A, Eisenberg L, Good B. Culture, illness, and care: clinical lessons from anthropologic and cross-cultural research. Ann Intern Med. 1978;88(2):251–258. doi:10.7326/0003-4819-88-2-251 PubMed
11. Patient satisfaction. Biology online web site. http://www.biology-online.org/dictionary/Patient_satisfaction. Updated October 2, 2005. Accessed April 28, 2015.
12. Bennett JK, Fuertes JN, Keitel M, et al. The role of patient attachment and working alliance on patient adherence, satisfaction, and health-related quality of life in lupus treatment. Patient Educ Couns. 2011;85(1):53–59. doi:10.1016/j.pec.2010.08.005 PubMed
13. Dulewicz V, Van Den Assem B. The GP-patient relationship and patient satisfaction. Br J Healthc Manag. 2013;19(12):596–600. doi:10.12968/bjhc.2013.19.12.596
14. Korsch BM, Negrete VF. Doctor-patient communication. Sci Am. 1972;227(2):66–74. doi:10.1038/scientificamerican0872-66 PubMed
15. Inui TS, Carter WB, Kukull WA, et al. Outcome-based doctor-patient interaction analysis: I. comparison of techniques. Med Care. 1982;20(6):535–549. doi:10.1097/00005650-198206000-00001 PubMed
16. Korsch BM, Freemon B, Negrete VF. Practical implications of doctor-patient interaction analysis for pediatric practice. Am J Dis Child. 1971;121(2):110–114. 10.1001/archpedi.1971.02100130064006 PubMed
17. Gesell SB, Wolosin RJ. Inpatients’ ratings of care in 5 common clinical conditions. Qual Manag Health Care. 2004;13(4):222–227. doi:10.1097/00019514-200410000-00005 PubMed
18. Cousin G, Schmid Mast M, Roter DL, et al. Concordance between physician communication style and patient attitudes predicts patient satisfaction. Patient Educ Couns. 2012;87(2):193–197. doi:10.1016/j.pec.2011.08.004 PubMed
19. Oakley BA. In: Oakley B, Knafo A, Madhavan G, eds. Pathological Altruism. New York, NY: Oxford University Press; 2012.
20. Singer PA, Martin DK, Kelner M. Quality end-of-life care: patients’ perspectives. JAMA. 1999;281(2):163–168. doi:10.1001/jama.281.2.163 PubMed
21. Gawande A. Being Mortal: Medicine and What Matters in the End. New York, NY: Metropolitan Books; 2014.
22. Weisner C, Mertens J, Parthasarathy S, et al. Integrating primary medical care with addiction treatment: a randomized controlled trial. JAMA. 2001;286(14):1715–1723. doi:10.1001/jama.286.14.1715 PubMed
23. Groves JE, Beresin EV. Difficult patients, difficult families. New Horiz-Sci Pract. 1998;6(4):331–343.
24. Wallace LS, Lennon ES. American Academy of Family Physicians patient education materials: can patients read them? Fam Med. 2004;36(8):571–574. PubMed
25. Williams MV, Davis T, Parker RM, et al. The role of health literacy in patient-physician communication. Fam Med. 2002;34(5):383–389. PubMed
26. Ratanawongsa N, Roter D, Beach MC, et al. Physician burnout and patient-physician communication during primary care encounters. J Gen Intern Med. 2008;23(10):1581–1588. doi:10.1007/s11606-008-0702-1 PubMed
27. Halbesleben JRB, Rathert C. Linking physician burnout and patient outcomes: exploring the dyadic relationship between physicians and patients. Health Care Manage Rev. 2008;33(1):29–39. doi:10.1097/01.HMR.0000304493.87898.72 PubMed
28. Irving JA, Dobkin PL, Park J. Cultivating mindfulness in health care professionals: a review of empirical studies of mindfulness-based stress reduction (MBSR). Complement Ther Clin Pract. 2009;15(2):61–66. doi:10.1016/j.ctcp.2009.01.002 PubMed
29. Krasner MS, Epstein RM, Beckman H, et al. Association of an educational program in mindful communication with burnout, empathy, and attitudes among primary care physicians. JAMA. 2009;302(12):1284–1293. doi:10.1001/jama.2009.1384 PubMed
30. Kjeldmand D, Holmström I. Balint groups as a means to increase job satisfaction and prevent burnout among general practitioners. Ann Fam Med. 2008;6(2):138–145. doi:10.1370/afm.813 PubMed
31. Shanafelt T, Dyrbye L. Oncologist burnout: causes, consequences, and responses. J Clin Oncol. 2012;30(11):1235–1241. doi:10.1200/JCO.2011.39.7380 PubMed
32. Kushner RF, Kessler S, McGaghie WC. Using behavior change plans to improve medical student self-care. Acad Med. 2011;86(7):901–906. doi:10.1097/ACM.0b013e31821da193 PubMed
33. O’Leary KJ, Wayne DB, Haviley C, et al. Improving teamwork: impact of structured interdisciplinary rounds on a medical teaching unit. J Gen Intern Med. 2010;25(8):826–832. doi:10.1007/s11606-010-1345-6 PubMed
34. Baker DP, Salas E, King H, et al. The role of teamwork in the professional education of physicians: current status and assessment recommendations. Jt Comm J Qual Patient Saf. 2005;31(4):185–202. PubMed
35. Weech-Maldonado R, Morales LS, Elliott M, et al. Race/ethnicity, language, and patients’ assessments of care in Medicaid managed care. Health Serv Res. 2003;38(3):789–808. doi:10.1111/1475-6773.00147 PubMed
36. Ferguson WJ, Candib LM. Culture, language, and the doctor-patient relationship. Fam Med. 2002;34(5):353–361. PubMed
37. Meeuwesen L, Harmsen JAM, Bernsen RMD, et al. Do Dutch doctors communicate differently with immigrant patients than with Dutch patients? Soc Sci Med. 2006;63(9):2407–2417. doi:10.1016/j.socscimed.2006.06.005 PubMed.
38. Campbell A, Sullivan M, Sherman R, et al. The medical mission and modern cultural competency training. J Am Coll Surg. 2011;212(1):124–129. doi:10.1016/j.jamcollsurg.2010.08.019 PubMed
39. Wang S-M, Caldwell-Andrews AA, Kain ZN. The use of complementary and alternative medicines by surgical patients: a follow-up survey study. Anaesth Analg; 2003;97(4):1010–1015. doi:10.1213/01.ane.0000078578.75597.f3. PubMed.
40. Gordon NP, Sobel DS, Tarazona EZ. Use of and interest in alternative therapies among adult primary care clinicians and adult members in a large health maintenance organization. West J Med. 1998;169(3):153–161. PubMed
41. Astin JA, Marie A, Pelletier KR, et al. A review of the incorporation of complementary and alternative medicine by mainstream physicians. Arch Intern Med. 1998;158(21):2303–2310. doi:10.1001/archinte.158.21.2303 PubMed
42. Kimball B, Joynt J, Cherner D, et al. The quest for new innovative care delivery models. J Nurs Adm. 2007;37(9):392–398. doi:10.1097/01.NNA.0000285142.57118.56 PubMed
43. Patel BK, Chapman CG, Luo N, et al. Impact of mobile tablet computers on internal medicine resident efficiency. Arch Intern Med. 2012;172(5):436–438. doi:10.1001/archinternmed.2012.45 PubMed
44. Hvid-Jensen F, Pedersen L, Drewes AM, et al. Incidence of adenocarcinoma among patients with Barrett’s esophagus. N Engl J Med. 2011;365(15):1375–1383. doi:10.1056/NEJMoa1103042 PubMed
LESSONS LEARNED AT THE INTERFACE OF MEDICINE AND PSYCHIATRY
The Psychiatric Consultation Service at Massachusetts General Hospital (MGH) sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.
Mss Chipidza and Wallwork are fourth-year medical students at Harvard Medical School, Boston, Massachusetts. Dr Stern is chief of the Avery D. Weisman Psychiatry Consultation Service at Massachusetts General Hospital and the Ned H. Cassem professor of psychiatry in the field of psychosomatic medicine/consultation at Harvard Medical School, Boston, Massachusetts.
Dr Stern is an employee of the Academy of Psychosomatic Medicine, has served on the speaker’s board of Reed Elsevier, is a stock shareholder in WiFiMD (Tablet PC), and has received royalties from Mosby/Elsevier and the Massachusetts General Hospital Psychiatry Academy and McGraw Hill. Mss Chipidza and Wallwork report no conflicts of interest related to the subject of this article.
Prim Care Companion CNS Disord 2015;17(5):doi:10.4088/PCC.15f01840
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: May 21, 2015; accepted June 12, 2015.
Published online: October 22, 2015.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Author contributions: Mss Chipidza and Wallwork contributed equally to the manuscript.
Corresponding author: Theodore A. Stern, MD, Harvard Medical School Massachusetts General Hospital, Department of Psychiatry, Massachusetts General Hospital, Fruit St, WRN 605, Boston, MA 02114
([email protected]).
Enjoy this premium PDF as part of your membership benefits!





