Objective: To assess whether and how effectively an interactive presentation about lifestyle medicine could impact the knowledge and attitudes of medical students to prepare them for managing chronic conditions in their patients. Chronic diseases are increasingly prevalent and problematic. Although chronic disease management involves lifestyle modification, few physicians are adequately trained in effective motivational interventions.
Methods: We surveyed first- and second-year Harvard Medical School students in October 2015 before and after a presentation on lifestyle medicine and quantified changes in their knowledge, attitudes/confidence, and skills.
Results: Medical students learned the basics of behavioral change after a 1-hour presentation, and their confidence with regard to implementing interventions increased. Median scores of confidence in counseling patients on lifestyle changes improved as did their ability to counsel patients on exercise, nutrition, sleep, stress management, and smoking cessation.
Conclusions: After a brief intervention, medical students can learn principles of behavioral management and how to implement the skills with patients suffering from chronic illnesses.
Increasing Knowledge and Confidence in Behavioral Change:
A Pilot Study

ABSTRACT
Objective: To assess whether and how effectively an interactive presentation about lifestyle medicine could impact the knowledge and attitudes of medical students to prepare them for managing chronic conditions in their patients. Chronic diseases are increasingly prevalent and problematic. Although chronic disease management involves lifestyle modification, few physicians are adequately trained in effective motivational interventions.
Methods: We surveyed first- and second-year Harvard Medical School students in October 2015 before and after a presentation on lifestyle medicine and quantified changes in their knowledge, attitudes/confidence, and skills.
Results: Medical students learned the basics of behavioral change after a 1-hour presentation, and their confidence with regard to implementing interventions increased. Median scores of confidence in counseling patients on lifestyle changes improved as did their ability to counsel patients on exercise, nutrition, sleep, stress management, and smoking cessation.
Conclusions: After a brief intervention, medical students can learn principles of behavioral management and how to implement the skills with patients suffering from chronic illnesses.
Prim Care Companion CNS Disord 2016;18(6):doi:10.4088/PCC.16m01962
© Copyright 2016 Physicians Postgraduate Press, Inc.
aHarvard Medical School, Boston, and Stroke Institute for Research and Recovery, Spaulding Rehabilitation Hospital, Charlestown, Massachusetts
bHarvard Medical School, Beth Israel Deaconess Medical Center, Boston, Massachusetts
cUniversity of Washington School of Medicine, Harvard Extension School, Boston, Massachusetts
dClinical Psychology, Harvard Extension School, Boston, Massachusetts
eMolecular and Cellular Biology, Harvard College, Cambridge, Massachusetts
fAvery D. Weisman Psychiatry Consultation Service and Office for Clinical Careers, Massachusetts General Hospital and Department of Psychiatry, Harvard Medical School, Boston, Massachusetts
*Corresponding author: Theodore A. Stern, MD, Department of Psychiatry, Massachusetts General Hospital, Fruit St, WRN 605, Boston, MA 02114 ([email protected]).
Chronic diseases and conditions (eg, heart disease, diabetes, chronic obstructive pulmonary disease, addictions, and obesity) are prevalent and problematic around the globe. While in 2000, less than 15 million lives were lost to these often preventable chronic diseases (eg, heart disease, stroke, diabetes, cancer, lung disease),1 that number soared to over 35 million lives in 2012.2 Moreover, management of chronic diseases is distinctly different from that of acute conditions, such as myocardial infarction, fractures, infections, and internal bleeding. Care of chronic diseases is often rooted in lifestyle choices (eg, what to eat, how much to eat, whether to exercise, and how to manage stressors of daily life) that influence our physiology and our risks for chronic disease. Research reveals that between 70% and 80% of chronic disease can be prevented by implementation of appropriate lifestyle changes.1 Such lifestyle issues need to be addressed with the patient in a collaborative manner that creates a partnership between the patient and the physician to motivate patients to make healthy choices. Unfortunately, habits take time and effort to develop. Physicians can serve an integral role in fostering an environment conducive to healthy habits and discovering intrinsic motivation for making changes.
More than a decade ago, Mokdad and colleagues3 described the leading causes of death (tobacco use, physical inactivity, and poor diet), which highlights the potential impact of lifestyle interventions on reducing morbidity and mortality. In addition, the Diabetes Prevention Study4 demonstrated that lifestyle interventions that focused on adopting healthy eating patterns, engaging in regular physical activity, and monitoring weight could be more effective than a medication for glucose control in decreasing the rate of conversion to diabetes in a prediabetic patient population. Despite these observations, medical schools have not traditionally educated students about counseling patients on changing behaviors (such as adopting regular physical activity and maintaining a healthy diet).
To address the large number of patients with chronic diseases related to lifestyle choices, physicians of the future will need to know how to motivate their patients and create change, as well as how to feel confident about their behavioral change counseling knowledge and skills. While many programs target the acquisition of knowledge and comprehension, only one-fourth of them target the acquisition of skills in analysis, synthesis, and evaluation.5
Teaching effective communication techniques is now recognized as an essential part of medical education worldwide. Student- and faculty-rated factors associated with being a "good doctor" in Korea cited "communication and collaboration with patients" and "medical knowledge and clinical skills" as most important.6 This collaborative coach approach to counseling is becoming the standard for "good doctoring."
Several studies have investigated approaches to teaching strategies for behavioral change to medical residents. A systematic review7 investigating the training in motivational interviewing during residency demonstrated that motivational interviewing education can be successfully implemented.
Health and wellness coaching has also been used and studied for more than a decade and is rooted in psychological theories (eg, social cognitive theory, goal-setting theory, adult learning theory, self-efficacy, self-determination theory, and positive psychology). This coaching method uses skills and techniques, such as motivational interviewing, appreciative inquiry, and the transtheoretical model of change.8 Randomized controlled studies9-15 have investigated the difference between using the health coaching interventions and usual care in a variety of medical conditions (such as diabetes, cardiovascular disease, asthma, and cancer pain) and have demonstrated improved health outcomes (eg, lower cholesterol levels, lower hemoglobin A1c levels, fewer rehospitalizations for asthma, and better pain control). Most coaching interventions include some form of collaboration, 1-on-1 counseling sessions, goal-setting, education, and accountability.16
Given that few studies have been conducted on interventions intended to improve behavioral change skills and strategies, we sought to answer the question, "Can a 1-hour lecture on behavioral change increase knowledge and confidence in first- and second-year medical students?"

- Chronic disease management involves lifestyle modification.
- Randomized controlled trials have validated the efficacy of health coaching.
- Medical students can learn principles of behavioral management and enhance their confidence levels regarding behavioral change counseling after a 1-hour presentation.
METHODS
We conducted a presurvey and postsurvey of first-year Harvard Medical School students (preselected by their interest in lifestyle medicine) via participation in the Lifestyle Medicine Interest Group in October 2015. The study qualified for institutional review board exempt status.
Twenty students attended a 1-hour lecture on lifestyle medicine by an experienced physician (E.P.F.) with knowledge of lifestyle medicine. Information was provided about what lifestyle medicine is, what research exists on it, what nutrition and physical exercise is essential for health, and what techniques are involved in motivational interviewing. The students were provided with an identical presurvey and postsurvey created to evaluate their comprehension of the content presented as well as their perceived changes in confidence in and attitude toward lifestyle medicine knowledge and techniques. Of the 20 students who attended the lecture, all 20 completed the presurvey, while 15 completed the postsurvey.
The survey (provided as questions in Tables 1, 2, and 3) included multiple-choice questions covering the material presented during the 1-hour lecture as well as numerically scaled confidence questions (ie, 1 is low confidence and 10 is high confidence) regarding how they felt about counseling patients on topics related to lifestyle medicine and their perception of the importance of lifestyle medicine knowledge and skills.
RESULTS
Knowledge
As seen in Table 1, although a large majority of attendees had a rudimentary understanding of the "coach approach" prior to the presentation, at the time of the presurvey, only 75% knew that randomized control trials had validated the efficacy of health coaching. By the time the postsurvey was conducted, 93% of attendees had knowledge of the health coaching research. Although 40% of attendees incorrectly believed that patients needed to be told "as much as possible" in order to manifest behavioral change, no students held this assumption at the time of the postsurvey. In assessing a patient’s stage of change, the percentage of students who answered correctly improved from 25% (pretalk) to 93% (posttalk). Prior to the presentation, 30% of students believed that giving a patient their body mass index (BMI) for review at home or telling a patient that their obesity would most likely kill them were valid approaches to motivating an overweight patient to adopt a healthier lifestyle. At the postsurvey, 93% of students chose a coach approach to behavior motivation, with no students choosing the 2 aforementioned choices. Prior to the presentation, all students understood the importance of educating themselves and their patients about healthy diets, exercise, and stress reduction. All students also knew that one’s own health habits correlate with one’s impact as a clinician (Table 1).
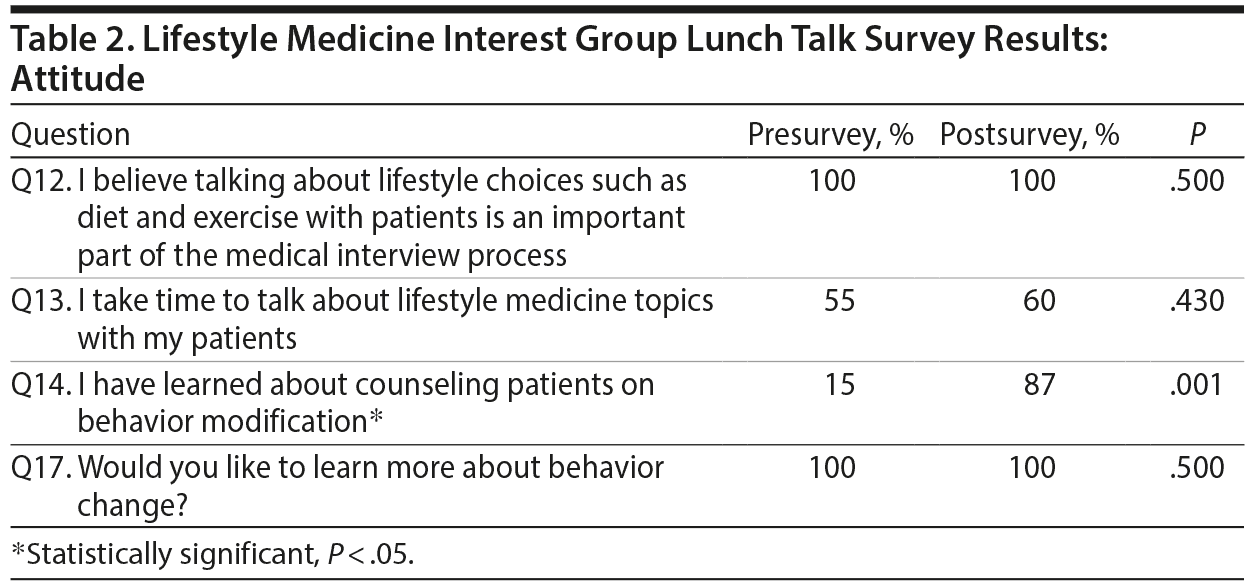
Attitude
Although all students believed in the importance of talking to patients about healthy lifestyles as part of the medical interview, a little more than half of the students admitted to actually talking to patients about healthy lifestyle choices. Although only 15% of students acknowledged learning about behavior modification prior to the presentation, 87% claimed to have learned about counseling during the presentation. All students endorsed wanting to learn more about behavioral change (Table 2).
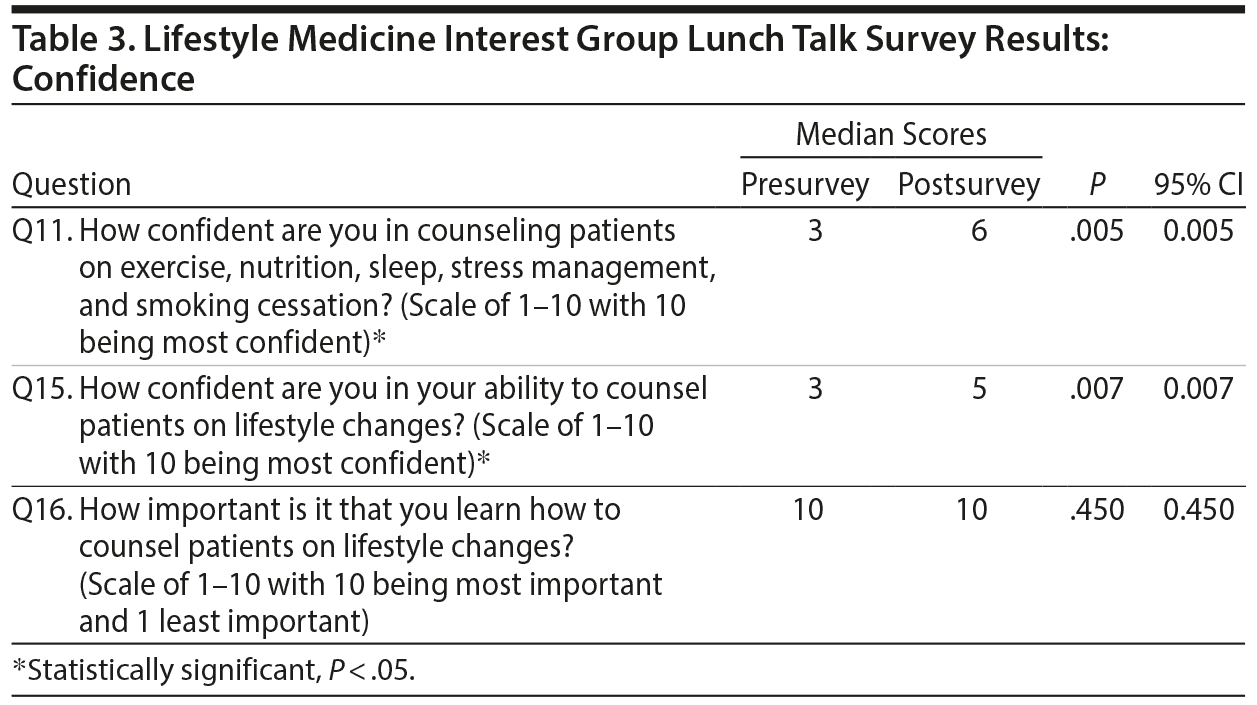
Confidence
Median scores of confidence in counseling patients on lifestyle changes improved from 3 in the presurvey to 5 in the postsurvey (with 1 being not confident and 10 being most confident). Similarly, confidence improved from 3 to 6 in students’ ability to counsel patients on exercise, nutrition, sleep, stress management, and smoking cessation, which provided internal validation for the study. Students believed the ability to counsel patients on lifestyle choices was most important, rating it a 10 (Table 3).
DISCUSSION
Recognizing the Value of Clinical Communication
Given a focus on behavioral change in the medical community (for patients and for physicians), it is important to explore different strategies as to how medical students can learn the theories of behavioral change and increase their confidence in using behavioral change techniques. Emphasizing the patient-practitioner relationship is a key strategy in teaching behavioral change techniques. Adherence to physician advice during counseling sessions is higher when the patient-practitioner relationship is strong. Some medical schools have recognized that doctor-patient communication17 and healthy behaviors are important components of medical school training. More than a decade ago, Kalet and colleagues18 reported that nearly two-thirds (65%) of medical schools taught communication skills in the preclinical years. They described a curriculum designed by faculty at New York University School of Medicine, Case Western Reserve School of Medicine, and University of Massachusetts Medical School, called the Macy Initiative in Health Communication. This curriculum was both useful and effective in increasing the communication skills of third-year medical students.18 Teaching medical students how to coach patients on lifestyle changes may be a way to positively affect patient outcomes. Some medical schools are already piloting the use of medical students as health coaches.19 In Ohio, Krok-Schoen and colleagues18 investigated a medical school pilot coaching program with medical students who were paired with elderly diabetic patients. Their study showed improvements in patients’ stages of change for exercise as well as improvements in patients’ health-related quality of life, providing initial evidence that a coaching program for medical students can have a positive effect on elderly, diabetic patients.
Behavioral Change Counseling Can Be Taught in Brief Educational Interventions
Our 1-hour interactive presentation increased the levels of confidence in medical students about counseling patients on behavioral change. The content introduced students to the coach approach to behavioral change counseling, a form of collaboration and negotiation using many of the motivational interviewing principles put forward by Miller and Rollnick.20 The presentation also included a discussion of the transtheoretical model of change, also known as the stages of change, and clinical cases that described the difference between advising patients and coaching patients.
Students are aware of the importance of lifestyle medicine counseling and behavioral change techniques. In our study, all students reported that the topic was important. Moreover, all of the students expressed interest in learning more about the behavioral change process. They were primed for this information and training. They also knew that if a patient did not follow instructions given at a previous visit, the best path forward was to inquire (nonjudgmentally) about what happened. Prior to the presentation, a quarter of Harvard Medical School students included in our sample were unaware of the randomized controlled studies performed on health coaching and health outcomes. The majority of them were unable to correctly identify the stage of change from the transtheoretical model of change framework. These 2 areas of knowledge increased immediately after the 1-hour presentation. However, what was unexpected was the self-reported change in confidence levels that students experienced after the lecture. The 1-hour presentation was sufficient to increase confidence levels on 2 different but similar questions on the presurvey and postsurvey.
Limitations
Limitations of our study included a lack of a long-term follow-up to assess application of knowledge and confidence gained from the talk. Also, the nature of the presentation self-selected for students already interested in lifestyle medicine.
Future Directions
Increasing knowledge empowers medical students and physicians to counsel patients on lifestyles and behavioral change. Increasing confidence and self-efficacy in behavioral change counseling further facilitates this process. In addition, having the opportunity to practice newly learned skills in a workshop setting and to test competence in these skills (by evaluating students using these behavioral change skills with patients) improves performance.
After presentations and workshops on behavioral change, follow-up inquiries about how often students counsel on behavioral change during their clerkships and clinical rotations will help demonstrate if these efforts in education are translatable to the clinic setting. Medical students also need to learn how to work with community resources to help support patients after they leave the doctor’s office.21
CONCLUSION
Medical students clearly see the value of behavioral change counseling, can learn these basic concepts via a 1-hour presentation, and enhance their confidence level with regard to counseling patients on lifestyle issues. Given the epidemics of obesity and diabetes facing this nation and the world, an emphasis on empowering medical students to counsel patients on lifestyles and behaviors is of paramount importance, and interventions as brief as 1 hour can enhance knowledge and confidence levels.
Submitted: April 12, 2016; accepted October 13, 2016.
Published online: November 24, 2016.
Potential conflicts of interest: Dr Stern is an employee of the Academy of Psychosomatic Medicine, has served on the speaker’s board of Reed Elsevier, is a stock shareholder in WiFiMD (Tablet PC), and has received royalties from Mosby/Elsevier, the Massachusetts General Hospital Psychiatry Academy, and McGraw Hill. Dr Frates, Mr Xiao, and Mss Simeon, McCargo, and Guo report no financial or other affiliation relevant to the subject of this article.
Funding/support: None.
REFERENCES
1. World Health Organization. Widespread misunderstandings about chronic disease—and the reality. 2005. WHO Web site. http://www.who.int/chp/chronic_disease_report/media/Factsheet2.pdf.
2. World Health Organization. Noncommunicable Diseases (NCD) Country Profiles. 2013. WHO Web site. http://www.who.int/nmh/countries/usa_en.pdf
3. Mokdad AH, Marks JS, Stroup DF, et al. Actual causes of death in the United States, 2000. JAMA. 2004;291(10):1238-1245. PubMed doi:10.1001/jama.291.10.1238
4. Knowler WC, Barrett-Connor E, Fowler SE, et al; Diabetes Prevention Program Research Group. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346(6):393-403. PubMed doi:10.1056/NEJMoa012512
5. Légaré F, Freitas A, Thompson-Leduc P, et al. The majority of accredited continuing professional development activities do not target clinical behavior change. Acad Med. 2015;90(2):197-202. PubMed doi:10.1097/ACM.0000000000000543
6. Yoo HH, Lee JK, Kim A. Perceptual comparison of the "good doctor" image between faculty and students in medical school [Korean]. Korean J Med Educ. 2015;27(4):291-300. PubMed
7. Dunhill D, Schmidt S, Klein R. Motivational interviewing interventions in graduate medical education: a systematic review of the evidence. J Grad Med Educ. 2014;6(2):222-236. PubMed doi:10.4300/JGME-D-13-00124.1
8. Prochaska JO, Velicer WF. The transtheoretical model of health behavior change. Am J Health Promot. 1997;Sept-Oct;12(1):38-48. PubMed doi/abs/10.4278/0890-1171-12.1.38
9. Whittemore R, Melkus GD, Sullivan A, et al. A nurse-coaching intervention for women with type 2 diabetes. Diabetes Educ. 2004;30(5):795-804. PubMed doi:10.1177/014572170403000515
10. Sacco WP, Morrison AD, Malone JIA. A brief, regular, proactive telephone "coaching" intervention for diabetes: rationale, description, and preliminary results. J Diabetes Complications. 2004;18(2):113-118. PubMed doi:10.1016/S1056-8727(02)00254-4
11. Koenigsberg MR, Bartlett D, Cramer JS. Facilitating treatment adherence with lifestyle changes in diabetes. Am Fam Physician. 2004;69(2):309-316. PubMed
12. Edelman D, Oddone EZ, Liebowitz RS, et al. A multidimensional integrative medicine intervention to improve cardiovascular risk. J Gen Intern Med. 2006;21(7):728-734. PubMed doi:10.1111/j.1525-1497.2006.00495.x
13. Vale MJ, Jelinek MV, Best JD, et al; COACH Study Group. Coaching patients On Achieving Cardiovascular Health (COACH): a multicenter randomized trial in patients with coronary heart disease. Arch Intern Med. 2003;163(22):2775-2783. PubMed doi:10.1001/archinte.163.22.2775
14. Fisher EB, Strunk RC, Highstein GR, et al. A randomized controlled evaluation of the effect of community health workers on hospitalization for asthma: the asthma coach. Arch Pediatr Adolesc Med. 2009;163(3):225-232. PubMed doi:10.1001/archpediatrics.2008.577
15. Oliver JW, Kravitz RL, Kaplan SH, et al. Individualized patient education and coaching to improve pain control among cancer outpatients. J Clin Oncol. 2001;19(8):2206-2212. PubMed
16. Wolever RQ, Simmons LA, Sforzo GA, et al. A systematic review of the literature on health and wellness coaching: defining a key behavioral intervention in healthcare. Glob Adv Health Med. 2013;2(4):38-57. PubMed doi:10.7453/gahmj.2013.042
17. Chipidza FE, Wallwork RS, Stern TA. Impact of the doctor-patient relationship. Prim Care Companion CNS Disord. 2015;17(5):doi:10.4088/PCC.15m01840. PubMed doi:10.4088/PCC.15m01840
18. Kalet A, Pugnaire MP, Cole-Kelly K, et al. Teaching communication in clinical clerkships: models from the Macy Initiative in Health Communications. Acad Med. 2004;79(6):511-520. PubMed doi:10.1097/00001888-200406000-00005
19. Krok-Schoen JL, Shim R, Nagel R, et al. Outcomes of a health coaching intervention delivered by medical students for older adults with uncontrolled type 2 diabetes. Gerontol Geriatr Educ. 2015:1-17. PubMed doi:10.1080/02701960.2015.1018514
20. Miller WR, Rollnick S. Motivational Interviewing: Preparing People for Change. New York, NY: Guilford; 2002.
21. Campos-Outcalt D, Calonge N. Commentary: adding realism and perspective to behavioral counseling curricula for medical students. Acad Med. 2012;87(7):840-841. PubMed doi:10.1097/ACM.0b013e3182580f56
Enjoy this premium PDF as part of your membership benefits!