Prim Care Companion CNS Disord 2022;24(5):21cr03170
To cite: Fana M, Werner L, Williams J, et al. Multiple strokes in a patient with systemic lupus erythematosus in the absence of common underlying syndromes. Prim Care Companion CNS Disord. 2022;24(5):21cr03170.
To share: https://doi.org/10.4088/PCC.21cr03170
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Neurology, Henry Ford Health System, Detroit, Michigan
bWayne State University, School of Medicine, Detroit, Michigan
cDepartment of Infectious Disease, Henry Ford Health System, Detroit, Michigan
*Corresponding author: Michael Fana, MD, MSc, 2799 E Grand Blvd, Detroit, MI 48202 ([email protected]).
Systemic lupus erythematosus (SLE) is an autoimmune disease with manifestations in nearly every organ system with a predilection for Black females.1 Neuropsychiatric SLE (NPSLE) is a commonly reported neurocognitive presentation in patients with SLE; up to 50% of patients with SLE will develop NPSLE within 3–5 years of SLE diagnosis.2 The most serious manifestation of NPSLE is ischemic stroke, which affects 3%–20% of patients with SLE.1 To date, the etiology of ischemic strokes in patients with SLE is known to be due to (1) a hypercoagulable state secondary to antiphospholipid antibody syndrome (APS) or atherosclerosis, (2) cerebral vasculitis (ie, cerebritis), or (3) marantic cardioembolism.1 Approximately 20%–30% of patients with SLE are found to have APS; meanwhile, cerebral vasculitis in SLE is rare, and its incidence in postmortem studies has been documented in 7% to 10% of cases.3 Currently, there are no reports, to our knowledge, on patients with SLE presenting with multiple strokes in the absence of such aforementioned etiology.
Case Report
The patient was a 32-year-old Black woman with a known medical history of SLE who presented to the hospital with acute onset of fevers to 40.9°C (105.6°F), recurring falls, confusion, diffuse joint pain, and a chronic reticular erythematous rash prominent on the hands and feet. She had recently completed a 3-week prednisone taper for a prior lupus flareup 1 week prior to presentation. Her home medication regimen included daily hydroxychloroquine. She endorsed subjective fevers and generalized malaise.
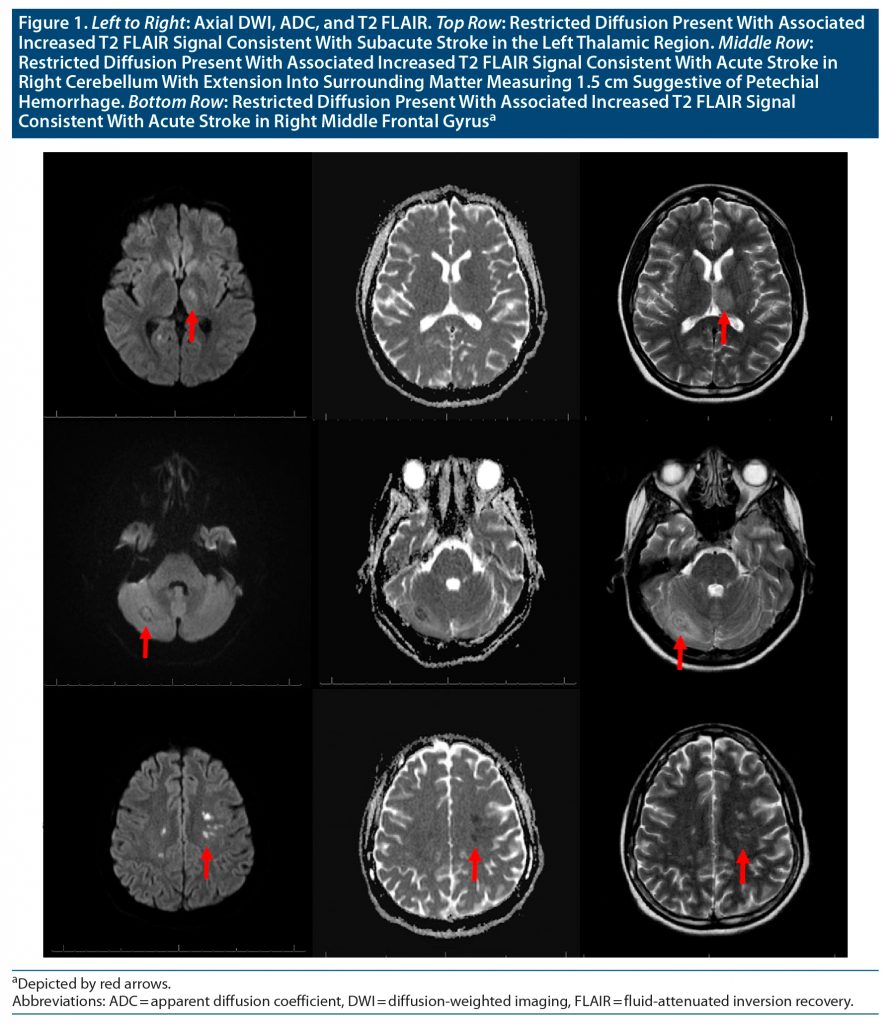
Extensive workup completed to assess for infectious etiology versus acute lupus flareup found unremarkable evidence for bacteremia, fungemia, or bacterial, fungal, mycobacterial, or viral meningitis. The virology panel was negative, and there was no urine or cerebrospinal culture growth. The neurologic examination showed intact cranial nerves with reflexes 2/4, distal to proximal sensory gradient seen in bilateral feet, motor strength 4/5 in bilateral upper and lower extremities, intention tremor on finger-to-nose testing, and dysdiadochokinesia on rapid alternating finger tap test. A computed tomography (CT) head scan without contrast demonstrated an area of focal hypodensity within the right cerebellar hemisphere. CT angiography demonstrated no significant stenosis or occlusion of intracranial or extracranial arteries. Follow-up magnetic resonance imaging (MRI) and magnetic resonance angiography of the head with and without contrast confirmed petechial hemorrhage of the right cerebellum with nonsignificant narrowing of the A2 and A3 segments of the anterior cerebral artery and acute-subacute infarctions of the right middle frontal gyrus and left thalamus (Figure 1).
Of note, the patient had previous negative noncontrast CT head findings in 2017 for an episode of distal extremity paresthesia. Lipid panel studies were unremarkable for hypercholesterolemia or hyperlipidemia. Cardiolipin antibody panel demonstrated elevated IgG and IgM levels to 21.6 and 32.6 GPL U/mL, respectively, and unremarkable β-2 glycoprotein antibody levels. Transthoracic echocardiogram and transesophageal echocardiogram were unremarkable for cardiac thrombi, and carotid Doppler ultrasound was unremarkable for stenosis or atherosclerosis. Finally, liver biopsy demonstrated mild portal and chronic inflammation with mild sinusoidal congestion without significant fibrosis.
Discussion
Through extensive workup, we discovered no evidence of cerebral vasculitis, antiphospholipid antibody syndrome, or cardioembolic source of stroke in our patient. This suggests our patient’s source of acute and subacute strokes was secondary to an idiopathic chronic inflammatory disease state. MRI of the head and CT angiogram findings were unremarkable for vasculitis, which was further substantiated by the liver biopsy results. We were less convinced of antiphospholipid syndrome, as the patient met only 1 clinical criteria of the Sapporo criterion: evidence of arterial thrombosis.4 No evidence of thrombi or emboli were found on diagnostic studies, and her calculated atherosclerotic cardiovascular disease risk factor was 8%. Of note, our patient’s persistent fever and intention tremor resolved with a 3-day course of methylprednisolone with significant improvement in her dysdiadochokinesia. In addition to her home hydroxychloroquine regimen, our patient was instructed to begin an anticoagulation regimen with warfarin 5 mg/d.
Published online: September 8, 2022.
Relevant financial relationships: None.
Funding/support: None.
Previous presentation: Presented at the Mayo Clinic 13th Annual Stroke and Cerebrovascular Disease Review 2021; October 13–16, 2021; Amelia Island, Florida.
Patient consent: Consent was received from the patient to publish the report, and information has been de-identified to protect anonymity.
References (4)

- Shaban A, Leira EC. Neurological complications in patients with systemic lupus erythematosus. Curr Neurol Neurosci Rep. 2019;19(12):97. PubMed CrossRef
- Govoni M, Bortoluzzi A, Padovan M, et al. The diagnosis and clinical management of the neuropsychiatric manifestations of lupus. J Autoimmun. 2016;74:41–72. PubMed CrossRef
- Barile-Fabris L, Hernández-Cabrera MF, Barragan-Garfias JA. Vasculitis in systemic lupus erythematosus. Curr Rheumatol Rep. 2014;16(9):440. PubMed CrossRef
- Wilson WA, Gharavi AE, Koike T, et al. International consensus statement on preliminary classification criteria for definite antiphospholipid syndrome: report of an international workshop. Arthritis Rheum. 1999;42(7):1309–1311. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!