Objective: To describe outpatient prescription treatment for active-duty military members with posttraumatic stress disorder (PTSD). Medical records were screened for drug-drug interactions with PTSD-related medications and for adverse drug events.
Method: A retrospective chart review was conducted of the medical records of active-duty service members aged 18 to 65 years who had a diagnosis of PTSD (ICD-9 criteria) and received psychiatric treatment at Naval Hospital Camp Pendleton, Camp Pendleton, California, between October 1, 2010, and October 31, 2010. Prescription medication treatment over a 6-month period (October 1, 2010, through March 31, 2011) was reviewed.
Results: Among 275 patients, 243 (88.4%) had at least 1 prescription dispensed and 219 (79.6%) had at least 1 PTSD-related medication dispensed. More than 1 PTSD-related medication was dispensed to 153 (55.6%) patients. The most common medication classes dispensed were selective serotonin reuptake inhibitors (SSRIs) and serotonin-norepinephrine reuptake inhibitors (SNRIs) (35.1%), novel antidepressants (15.6%), and anticonvulsants (15.0%). The most frequently dispensed PTSD-related medications were zolpidem: 149 (9.8%), sertraline: 147 (9.7%), gabapentin: 134 (8.8%), prazosin: 111 (7.3%), and trazodone: 110 (7.2%). In the subgroup of 219 patients who received PTSD-related medications, overlapping periods of treatment between an SSRI and another PTSD-related medication occurred in 58 (26.5%) patients. Potential drug-drug interactions with this combination involved 44 (20.1%) patients; no adverse drug events were reported. Among these 44 patients, 55 different potential drug-drug interactions were identified.
Conclusions: Patients receiving medications for PTSD are frequently treated with SSRIs or SNRIs and are likely to be prescribed more than 1 PTSD-related medication.
Pharmacologic Therapy for Posttraumatic Stress Disorder:
Review of Prescriptions and Potential
Drug-Drug Interactions in a Military Cohort
ABSTRACT
Objective: To describe outpatient prescription treatment for active-duty military members with posttraumatic stress disorder (PTSD). Medical records were screened for drug-drug interactions with PTSD-related medications and for adverse drug events.
Method: A retrospective chart review was conducted of the medical records of active-duty service members aged 18 to 65 years who had a diagnosis of PTSD (ICD-9 criteria) and received psychiatric treatment at Naval Hospital Camp Pendleton, Camp Pendleton, California, between October 1, 2010, and October 31, 2010. Prescription medication treatment over a 6-month period (October 1, 2010, through March 31, 2011) was reviewed.
Results: Among 275 patients, 243 (88.4%) had at least 1 prescription dispensed and 219 (79.6%) had at least 1 PTSD-related medication dispensed. More than 1 PTSD-related medication was dispensed to 153 (55.6%) patients. The most common medication classes dispensed were selective serotonin reuptake inhibitors (SSRIs) and serotonin-norepinephrine reuptake inhibitors (SNRIs) (35.1%), novel antidepressants (15.6%), and anticonvulsants (15.0%). The most frequently dispensed PTSD-related medications were zolpidem: 149 (9.8%), sertraline: 147 (9.7%), gabapentin: 134 (8.8%), prazosin: 111 (7.3%), and trazodone: 110 (7.2%). In the subgroup of 219 patients who received PTSD-related medications, overlapping periods of treatment between an SSRI and another PTSD-related medication occurred in 58 (26.5%) patients. Potential drug-drug interactions with this combination involved 44 (20.1%) patients; no adverse drug events were reported. Among these 44 patients, 55 different potential drug-drug interactions were identified.
Conclusions: Patients receiving medications for PTSD are frequently treated with SSRIs or SNRIs and are likely to be prescribed more than 1 PTSD-related medication.
Prim Care Companion CNS Disord 2015;17(6):doi:10.4088/PCC.15m01843
© Copyright 2015 Physicians Postgraduate Press, Inc.
aDepartment of Pharmacy, Naval Hospital Camp Pendleton, Camp Pendleton, California
bClinical Investigations Department, Naval Hospital Camp Pendleton, Camp Pendleton, California
cCDR, USPHS; Treatment Programs Department, Naval Hospital Camp Pendleton, Camp Pendleton, California
dCDR, MSC, USN; Department of Pharmacy, Naval Hospital Camp Pendleton, Camp Pendleton, California
*Corresponding author: Kara L. Jablonski, PharmD, Naval Hospital Camp Pendleton, Department of Pharmacy, Box 555191, Camp Pendleton, CA 92055 ([email protected]).
Posttraumatic stress disorder (PTSD) has been a rising concern in military health centers across America since recognition as a disorder in the DSM-III in the 1980s.1,2 Currently, the US Food and Drug Administration (FDA) has approved only 2 medications for the treatment of PTSD symptoms: sertraline and paroxetine.3 However, the 2010 Veterans Affairs/Department of Defense Clinical Practice Guideline for Management of Posttraumatic Stress (CPG)4 supports the off-label use of other psychotropic medications for the treatment of PTSD symptoms.
Selective serotonin reuptake inhibitors (SSRIs) and the serotonin-norepinephrine reuptake inhibitor (SNRI) venlafaxine are the preferred first-line pharmacologic treatments for PTSD, as recommended by the CPG.4 SSRIs and SNRIs treat the core symptoms of PTSD in addition to comorbid conditions such as depression, panic disorder, and anxiety.3 Second-line monotherapy agents that are less well-studied classes of medications include mirtazapine, nefazodone, tricyclic antidepressants, and monoamine oxidase inhibitors.5,6 Unmentioned in the CPG, the SNRI duloxetine has also been studied in the monotherapy treatment of PTSD symptoms with positive results, warranting further research.7,8 Prazosin as adjunct therapy has shown consistent efficacy in improving sleep and reducing nightmares.9 Additional adjunct therapies may include atypical antipsychotics, typical antipsychotics, nonbenzodiazepine hypnotics, buspirone, bupropion, trazodone, gabapentin, lamotrigine, propranolol, and clonidine.
Recently, benzodiazepines have been scrutinized as being potentially harmful when used in patients with PTSD. Benzodiazepines show a lack of efficacy evidence in PTSD treatment, are associated with significant withdrawal symptoms,10 and have a high potential for dependence. Furthermore, daily use of benzodiazepines has been shown to interfere with the extinction of fear in prolonged exposure therapy.11 The National Center for PTSD12 recommends reducing or eliminating prescribing of benzodiazepines for those with PTSD. The Army Surgeon General’s Policy13 also addresses increasing concerns regarding “off-label” use of atypical antipsychotics and benzodiazepines due to adverse metabolic effects, high abuse potential, and clinical results demonstrating limited efficacy for PTSD symptom treatment.
With regard to pharmacotherapy, the CPG recommends monotherapy as the preferred course of treatment in addition to psychotherapy and behavioral interventions for patients with PTSD.4 However, the severity and complexity of symptom profiles of service members may require combination therapy in order to adequately treat patient symptoms.4 Hoffman et al14 describe combination therapy as more than 2 medications for 1 indication or prescription of 2 or more medications with identical or similar mechanisms of action in 1 individual. For PTSD, combination therapy may be used for treating comorbid disorders and supplementing the effect of the primary medication.15 Federal funding has not provided for systematic studies on polypharmacy usage.15 The current literature describes data obtained from passive surveillance, surveys, and record reviews.
With multiple medications available for both labeled and off-label use in PTSD, the opportunity for drug-drug interactions and potential for adverse side effects are concerns. The CPG4 lists serotonin syndrome as a possible adverse drug event with the use of SSRIs, SNRIs, and other serotonin-augmenting medications. Serotonin syndrome is described as a triad of mental status changes, autonomic hyperactivity, and neuromuscular abnormalities with varying degrees of severity.16 SSRI overdose has a 10%–14% incidence of serotonin syndrome, with sertraline, paroxetine, and fluvoxamine the most contributory SSRI medications.17 In 2004, the Toxic Exposure Surveillance System18 identified 48,204 exposures to SSRIs that resulted in moderate or major outcomes in 8,187 patients and death in 103 patients; the vast majority of these fatalities were associated with coingestants. No clear guidance regarding patients using multiple pharmacologic agents and risk for serotonin syndrome is provided.4
The objective of the current analysis was to review the prescription medication experience among an active-duty cohort diagnosed with PTSD and describe their medication use. Secondary endpoints included screening medication profiles for potential drug-drug interactions involving SSRIs, SNRIs, and other PTSD-related medications, as well as any documented adverse drug event in the outpatient medical record.
METHOD
Participants
This study was reviewed and approved by the local institutional review board (NHCP.2010.0175). Clinicians obtained data for 275 active-duty service members through a systematic review of outpatient care records. The target population was patients aged 18 to 65 years who had a diagnosis of PTSD (ICD-9 criteria19) and received psychiatric treatment at Naval Hospital Camp Pendleton, Camp Pendleton, California, between October 1, 2010, and October 31, 2010.
Research Design
Study clinicians conducted a retrospective chart review of electronic outpatient medical records in the Armed Forces Health Longitudinal Technology Application and Composite Health Care System. These records are maintained by the United States Navy Bureau of Medicine and Surgery in Falls Church, Virginia. Study clinicians reviewed the prescription medication experience among an active-duty cohort with PTSD at Naval Hospital Camp Pendleton over a 6-month period (October 1, 2010, through March 31, 2011), described the use of both PTSD-related and non–PTSD-related medications, identified frequency and classes of PTSD-related medication use, and screened medication profiles for potential drug-drug interaction involving only PTSD-related medications.
Measures
Demographic information and data regarding use of tobacco and history of alcohol misuse were collected. All medications that were prescribed and dispensed between October 1, 2010, and March 31, 2011, were recorded in a Microsoft Access Database. Data were collected on medications having potential use in PTSD treatment (both monotherapy and adjunct use), which are listed in Table 1-9 of the CPG (Table 2).4 We classified medications from the CPG as PTSD-related, with the addition of duloxetine, temazepam, clonidine, guanfacine, desvenlafaxine, and milnacipran, to include most medications within the CPG-specified classes.4 All other medications collected from the patients’ profiles were classified as non–PTSD treatment-related medications. The duration of medication treatment was defined as the intended therapeutic days’ supply as written by the prescriber and dispensed by the pharmacy. Total days of prescription coverage were censored at October 1, 2010, and March 31, 2011, in order to define prescription coverage days within this 182-day period. A therapeutic overlap was defined as being greater than 1 day of medication overlap by any 2 or more drugs.
Potential drug-drug interactions were identified using Lexi-Comp Database.20 The Lexi-Comp Database categorizes drug-drug interactions as follows: category A (no interaction), category B (no action needed), category C (monitor therapy), category D (modify regimen), or category X (avoid combination).20 Due to clinical relevance, drug-drug interactions were analyzed between specific PTSD-related medications with category D and X ratings in this study. Data also were collected regarding whether an adverse drug event occurred as documented by the provider from outpatient electronic medical records.
Data Analysis
Descriptive analyses included the number of patients who received prescription medications among the PTSD patients defined by inclusion criteria. Analyses also described the prescription days covered among all the patient days available in the 182-day observation period.
RESULTS
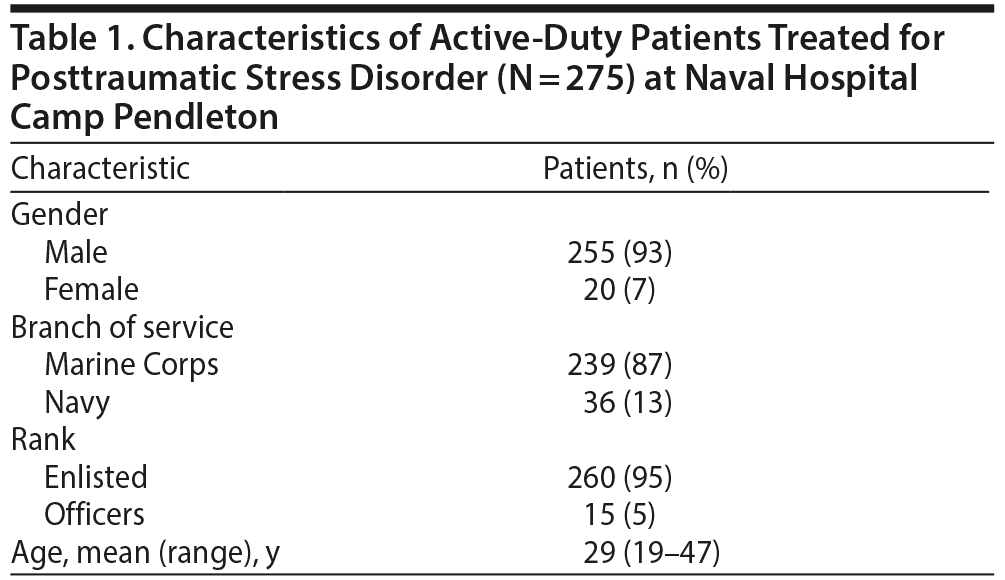
Demographic data were collected for 275 patients (Table 1) treated for PTSD at this institution, as defined by inclusion criteria. All 275 patients were active duty; most were male, enlisted, Marine Corps members with an average age of 29 years (Table 1). Data regarding social and health behavior indicated that 48% of patients were tobacco users during the 6-month study period, and 27% had a diagnosis of alcohol abuse or dependence before or during the 6-month time period. The mean number of patient encounter notes written by any health care provider during this 6-month study was 48, with a range of 1 to 326 encounter notes.
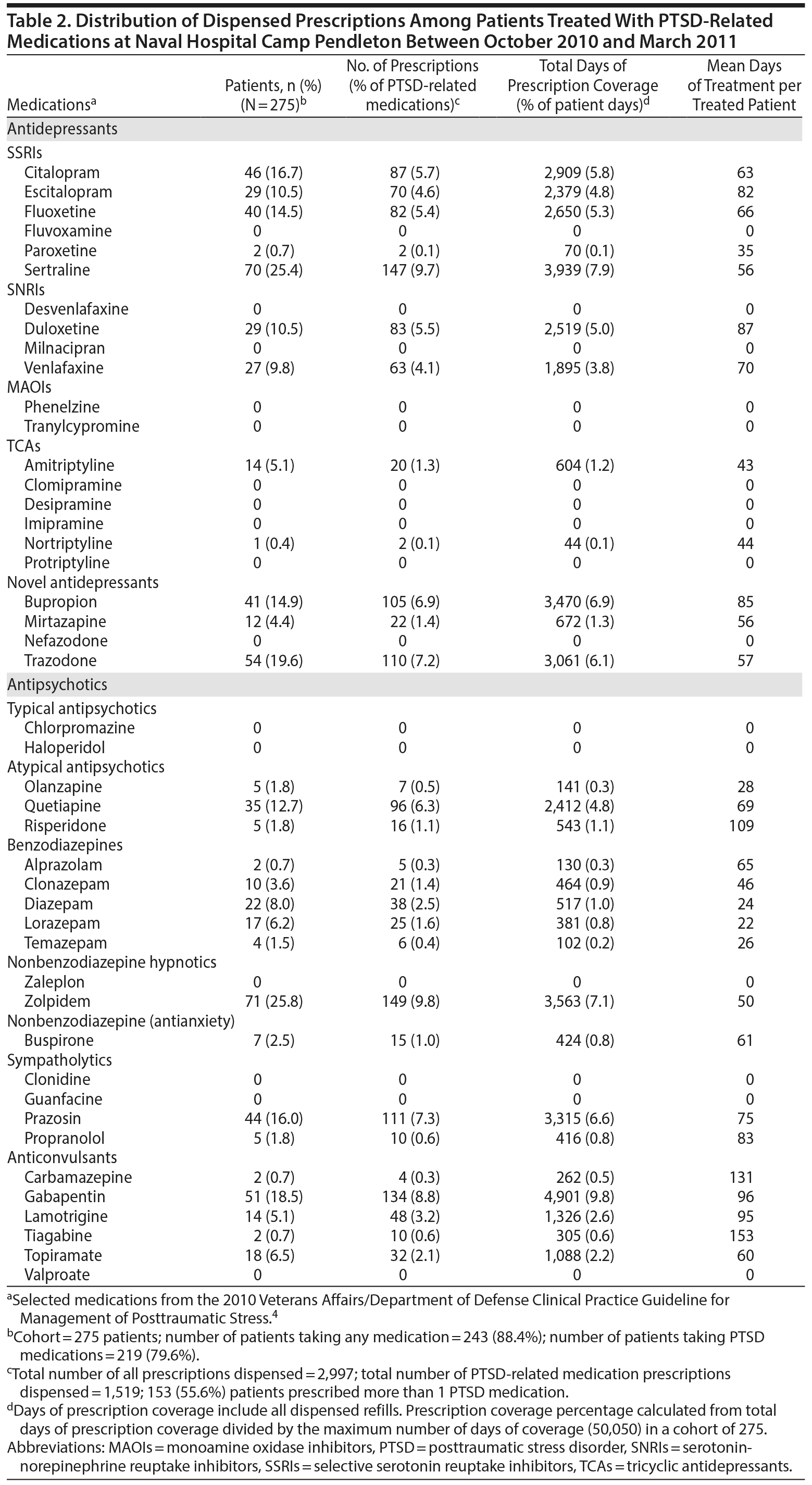
Most patients (243 [88.4%]) had at least 1 medication dispensed during the 6-month time period, and 219 (79.6%) had at least 1 PTSD-related medication dispensed (Table 2). The most frequently dispensed PTSD-related medications were zolpidem: 149 (9.8%), sertraline: 147 (9.7%), gabapentin: 134 (8.8%), prazosin: 111 (7.3%), and trazodone: 110 (7.2%). The medications with the most days of prescription coverage were gabapentin (4,901 patient days), sertraline (3,939 patient days), bupropion (3,470 patient days), trazodone (3,061 patient days), and fluoxetine (2,650 patient days). However, the medications with the longest mean days of treatment per patient were tiagabine (153 days/patient), carbamazepine (131 days/patient), risperidone (109 days/patient), gabapentin (96 days/patient), and lamotrigine (95 days/patient). There were 153 (55.6%) patients prescribed > 1 PTSD-related medication.
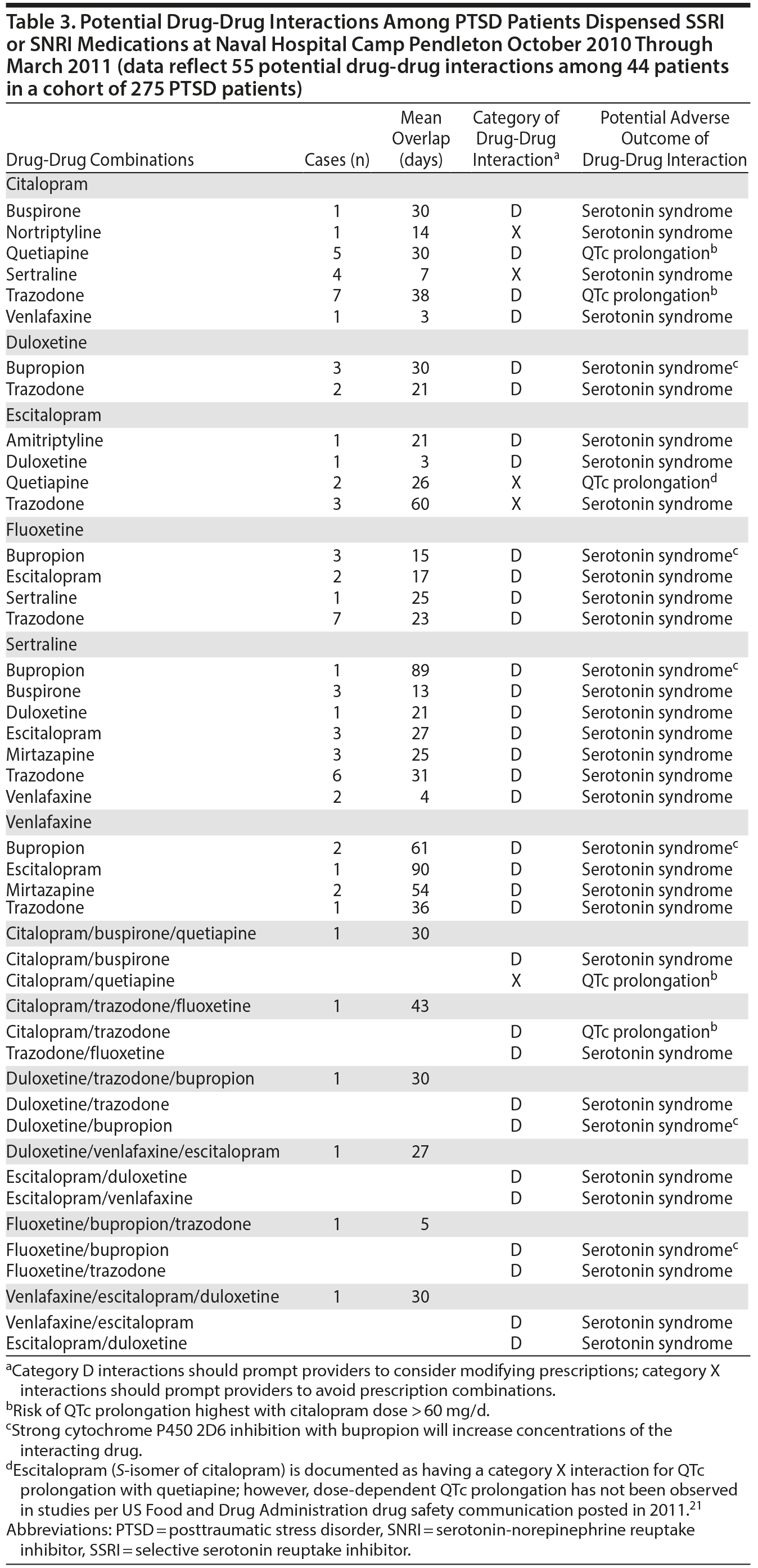
Of the 219 patients with at least 1 prescribed PTSD-related medication, the most common medication classes dispensed were SSRIs (25.5%), novel antidepressants (15.6%), anticonvulsants (15.0%), nonbenzodiazepine hypnotics (9.8%), and SNRIs (9.6%). With respect to this subgroup receiving PTSD-related medications, 58 (26.5%) patients had overlapping periods of treatment between an SSRI or SNRI and another PTSD-related medication (Table 3). Potential drug-drug interactions with SSRIs or SNRIs were identified in 75 cases, most creating risk for serotonin syndrome. Potential drug-drug interactions involving an SSRI or SNRI and another PTSD-related medication involved 44 (20.1%) patients in this subgroup. Among these 44 patients, a total of 55 different potential drug-drug interactions were identified, the most common was between an SSRI and trazodone (24 cases identified). There were no reports or observations of serotonin syndrome or cases of cardiac dysrhythmias related to QTc prolongation.
DISCUSSION
Patients with PTSD may be prescribed more than 1 medication to treat associated complex symptom profiles. As our study demonstrates, SSRIs and SNRIs are commonly prescribed medications for PTSD treatment, and, therefore, serotonin syndrome is of particular concern. Of our sample of military members with a PTSD diagnosis, 80% were prescribed at least 1 PTSD-related medication, and 55.6% were prescribed > 1 PTSD-related medication (Tables 2 and 3). The most frequently dispensed medications were as follows: zolpidem, sertraline, gabapentin, prazosin, and trazodone; the SSRIs and SNRIs were the most common medication classes dispensed.
The number of dispensed prescriptions for duloxetine was greater than venlafaxine, which is of interest due to strong monotherapy recommendations for venlafaxine use.4 This practice pattern may be due to additional comorbidities in this cohort, such as neuropathic pain, but those data were not available in this review. The high prevalence of zolpidem use is notable, as hypnotics are reserved for second-line insomnia treatment after trazodone and are recommended to be used only for short periods of time.4 The addition of zolpidem to the Veterans Affairs national formulary in 200822 may account for the increased prescribing pattern observed in this study as well as in previous studies near this time period.12 Overall, the PTSD-related prescriptions dispensed to our cohort were in accordance with the CPG and first-line treatment for global PTSD symptoms.4
In addition to the number of prescriptions dispensed, we calculated days’ coverage of medication per patient. The majority of SSRI/SNRI prescriptions were dispensed on average for greater than 30 days per patient (including dispensed refills) (range, 22–153 days/patient). This finding indicates that SSRI/SNRI trial periods extended beyond 4 weeks, which is generally considered the minimum time of therapy for onset of action. The medications dispensed with the longest mean days of prescription coverage included risperidone and several anticonvulsants. Of significant interest is the use of atypical antipsychotics in this patient population. Although length of coverage averaged more than 3 months per patient, risperidone was not dispensed to many individual patients. Infrequent use is consistent with the low risk/benefit ratio associated with atypical antipsychotics. A randomized clinical trial23 of veterans with PTSD found risperidone ineffective at PTSD symptom reduction when used as an adjunct to other medication therapy. Atypical antipsychotics are reserved as last-line treatment due to potential risks, such as metabolic abnormalities, as outlined by the Army Surgeon General’s Policy of 2012.13 The CPG does not support the use of atypical antipsychotics as adjunct PTSD therapy due to unknown benefit but does specifically recommend against risperidone use.4 The CPG also discourages the use of antipsychotics as monotherapy treatment and use of benzodiazepines as any part of pharmacologic PTSD treatment.4 Aligning with this recommendation, we found that there were a relatively small number of prescriptions dispensed for benzodiazepines.
Currently, there is no literature that quantifies the degree of risk created by combining multiple medications used for treatment of service members with PTSD. Of the patients in our cohort who were dispensed PTSD-related medications, one-half were dispensed more than 1. On the basis of the large number of SSRIs and SNRIs dispensed, we chose to review the potential drug-drug interactions involving these medication classes within the subset of patients who received PTSD-related medications. Potential for drug-drug interactions increased when patients had overlapping time periods covered by SSRIs and SNRIs and any other of our designated PTSD-related medications. Of the 219 people who received PTSD-related medications, 194 patients (88.6%) received SSRIs and/or SNRIs, creating a risk for category D or X drug-drug interactions of 25.1%. The most frequent combinations involved a potential drug-drug interaction with trazodone. Other medication combinations were identified with potential for inducing cytochrome P450 involvement or QTc prolongation as shown in Table 3. However, we found serotonin syndrome to be the most concerning risk.
Serotonin syndrome can be precipitated by the use of ≥ 2 medications that increase serotonin levels, such as SSRI or SNRIs, tricyclic antidepressants, monoamine oxidase inhibitors, bupropion, serotonin modulators (nefazodone, trazodone), valproate, carbamazepine, and buspirone, all of which are included in the CPG for PTSD treatment with varying recommendations for use.4,16 Serotonin syndrome may occur with therapeutic medication combinations, with intentional overdose, or through unintentional drug reactions.16 Most reported cases of serotonin syndrome are in patients taking multiple serotonergic agents or those who have considerable exposure to a single serotonin-augmenting drug.24
Although no adverse drug events were reported in our cohort, our study shows that there was a risk for serotonin syndrome. There are several factors that may explain the absence of observed adverse drug events. The incidence of serotonin syndrome is difficult to assess in clinical practice for several reasons, including underdiagnosis. According to Boyer and Shannon,16 more than 85% of physicians do not recognize serotonin syndrome as a clinical diagnosis. Symptoms also may be attributed to other medical or psychiatric illness.24 A diagnosis of serotonin syndrome is mostly determined by exclusion and inference from a patient’s current medications.24
The probability of such events may be relatively low in this cohort, even when multiple drug-drug overlaps exist. Additionally, our data document all dispensed medications, but patients may not have taken all medications as prescribed. Poor medication adherence, including overuse and underuse of medication,25 is common in those with challenging conditions such as PTSD.26 The observed potential drug-drug interactions reflected in our data would be less likely to occur if patients were noncompliant with medications. Nonetheless, the potential for serious drug-drug interactions in patients taking PTSD-related medications merits concern and extra vigilance on the part of providers to minimize risks. In 6 of these patients, the risk was increased by overlaps of 3 serotonin-affecting medications. Some of these overlaps were duplications of therapy, meaning 2 medications with the same mechanism of action were covering the same time period. Providers may have advised patients to discontinue taking 1 medication when another was prescribed in these situations, but our chart review did not reflect this kind of provider counseling.
This novel exploration of combination medication use in a well-defined cohort highlights the risk of serotonin syndrome in patients receiving treatment for PTSD. The study’s limitations, however, must be addressed in future work. A retrospective chart review provided detailed information about the medications dispensed to each patient with complete medication profiles, but could not verify that patients used the medication as directed. Also, we could not ascertain providers’ reasoning for multiple medication prescriptions from the medical records. The small number of providers for this population during this time period may have introduced provider-specific medication selection bias.
Our methodology was not designed specifically for the detection of serotonin syndrome, and while no adverse events were reported, this does not mean that none occurred. The literature indicates that both patients and providers have difficulty recognizing these symptoms or may not attribute mild symptoms to medication use.16,27 Our data were obtained during the year that the CPG was published.4 Providers may not have fully implemented these guidelines into practice for our cohort. In addition, the cohort was not restricted to those with exclusive diagnoses of PTSD. The CPG notes that 50% to 80% of patients with PTSD have ≥ 1 comorbid mental health disorders.4 Comorbid conditions and their respective treatments may limit inference about our findings as they relate specifically to PTSD.
Future analyses of these and other data should expand beyond the SSRI and SNRI classes and include all other PTSD medication classes and potential drug-drug interactions. In addition, the non-PTSD medication data collected warrant further exploration, with special focus on pain and sleep medications, which are frequently prescribed. Continued evaluation of prescription practices over time is important in this critically important population.
Submitted: May 26, 2015; accepted June 23, 2015.
Published online: December 3, 2015.
Drug names: alprazolam (Xanax, Niravam, and others), bupropion (Wellbutrin and others), carbamazepine (Tegretol, Epitol, and others), citalopram (Celexa and others), clomipramine (Anafranil and others), clonazepam (Klonopin and others), clonidine (Catapres and others), desipramine (Norpramin and others), desvenlafaxine (Pristiq, Khedezla, and others), diazepam (Valium and others), duloxetine (Cymbalta), escitalopram (Lexapro and others), fluoxetine (Prozac and others), fluvoxamine (Luvox and others), gabapentin (Neurontin, Gralise, and others), guanfacine (Tenex and others), haloperidol (Haldol), imipramine (Tofranil and others), lamotrigine (Lamictal and others), lorazepam (Ativan and others), milnacipran (Savella), mirtazapine (Remeron and others), nortriptyline (Pamelor, Aventyl, and others), olanzapine (Zyprexa and others), paroxetine (Paxil, Pexeva, and others), phenelzine (Nardil and others), prazosin (Minipress and others), propranolol (Inderal and others), protriptyline (Vivactil and others), quetiapine (Seroquel and others), risperidone (Risperdal and others), sertraline (Zoloft and others), temazepam (Restoril and others), tiagabine (Gabitril and others), topiramate (Topamax and others), tranylcypromine (Parnate and others), trazodone (Oleptro), venlafaxine (Effexor and others), zaleplon (Sonata and others), zolpidem (Ambien, Edluar, and others).
Author contributions: This work was prepared as part of the authors’ official duties. Title 17 USC 105 provides that “Copyright protection under this title is not available for any work of the United States government.” Title 17 USC 101 defines a United States Government work as a work prepared by a military service member or employee of the United States Government as part of that person’s official duties.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Disclaimer: The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.
Acknowledgment: The authors appreciate the support of the staff at Naval Hospital Camp Pendleton.
REFERENCES
1. Scott WJ. PTSD in DSM-III: a case in the politics of diagnosis and disease. Soc Probl. 1990;37(3):294–310. doi:10.2307/800744
2. Wilson JF. Posttraumatic stress disorder needs to be recognized in primary care. Ann Intern Med. 2007;146(8):617–620. doi:10.7326/0003-4819-146-8-200704170-00025 PubMed
3. Jeffreys M, Capehart B, Friedman MJ. Pharmacotherapy for posttraumatic stress disorder: review with clinical applications. J Rehabil Res Dev. 2012;49(5):703–715. doi:10.1682/JRRD.2011.09.0183 PubMed
4. VA/DoD Clinical Practice Guideline for Management of Posttraumatic Stress. October 2010. Departments of Veterans Affairs and Defense Web site. http://www.healthquality.va.gov/PTSD-Full-2010c.pdf. Accessed October 15, 2014.
5. Chung MY, Min KH, Jun YJ, et al. Efficacy and tolerability of mirtazapine and sertraline in Korean veterans with posttraumatic stress disorder: a randomized open label trial. Hum Psychopharmacol. 2004;19(7):489–494. doi:10.1002/hup.615 PubMed
6. Kosten TR, Frank JB, Dan E, et al. Pharmacotherapy for posttraumatic stress disorder using phenelzine or imipramine. J Nerv Ment Dis. 1991;179(6):366–370. doi:10.1097/00005053-199106000-00011 PubMed
7. Villarreal G, Cañive JM, Calais LA, et al. Duloxetine in military posttraumatic stress disorder. Psychopharmacol Bull. 2010;43(3):26–34. PubMed
8. Aikins DE, Jackson ED, Christensen A, et al. Differential conditioned fear response predicts duloxetine treatment outcome in male veterans with PTSD: a pilot study. Psychiatry Res. 2011;188(3):453–455. doi:10.1016/j.psychres.2011.05.009 PubMed
9. Raskind MA, Peterson K, Williams T, et al. A trial of prazosin for combat trauma PTSD with nightmares in active-duty soldiers returned from Iraq and Afghanistan. Am J Psychiatry. 2013;170(9):1003–1010. doi:10.1176/appi.ajp.2013.12081133 PubMed
10. Kosten TR, Fontana A, Sernyak MJ, et al. Benzodiazepine use in posttraumatic stress disorder among veterans with substance abuse. J Nerv Ment Dis. 2000;188(7):454–459. doi:10.1097/00005053-200007000-00010 PubMed
11. van Minnen A, Arntz A, Keijsers GP. Prolonged exposure in patients with chronic PTSD: predictors of treatment outcome and dropout. Behav Res Ther. 2002;40(4):439–457. doi:10.1016/S0005-7967(01)00024-9 PubMed
12. Bernardy NC, Lund BC, Alexander B, et al. Prescribing trends in veterans with posttraumatic stress disorder. J Clin Psychiatry. 2012;73(3):297–303. doi:10.4088/JCP.11m07311 PubMed
13. Coley HA. Policy Guidance on the Assessment and Treatment of Posttraumatic Stress Disorder (PTSD). Fort Sam Houston, TX: Department of the Army, Headquarters, US Army Medical Command, Office of the Surgeon General; 2012.
14. Hoffman DA, Schiller M, Greenblatt JM, et al. Polypharmacy or medication washout: an old tool revisited. Neuropsychiatr Dis Treat. 2011;7:639–648. doi:10.2147/NDT.S24375 PubMed
15. Preskorn SH, Lacey RL. Polypharmacy: when is it rational? J Psychiatr Pract. 2007;13(2):97–105. doi:10.1097/01.pra.0000265766.25495.3b PubMed
16. Boyer EW, Shannon M. The serotonin syndrome. N Engl J Med. 2005;352(11):1112–1120. doi:10.1056/NEJMra041867 PubMed
17. Nelson LS, Erdman AR, Booze LL, et al. Selective serotonin reuptake inhibitor poisoning: an evidence-based consensus guideline for out-of-hospital management. Clin Toxicol (Phila). 2007;45(4):315–332. doi:10.1080/15563650701285289 PubMed
18. Watson WA, Litovitz TL, Rodgers GC Jr, et al. 2004 Annual report of the American Association of Poison Control Centers Toxic Exposure Surveillance System. Am J Emerg Med. 2005;23(5):589–666. doi:10.1016/j.ajem.2005.05.001 PubMed
19. International Statistical Classification of Diseases and Health-related Problems. 2004. World Health Organization Web site. http://www.cdc.gov/nchs/icd/icd9.htm. Updated September 1, 2009. Accessed October 14, 2014.
20. Lexi-Comp Online [computer program]. Hudson, OH: Lexi-Comp, Inc, Wolters Kluwer Health; January 29, 2011.
21. FDA drug safety communication: revised recommendations for Celexa (citalopram hydrobromide) related to a potential risk of abnormal heart rhythms with high doses. Published August 24, 2011. Food and Drug Administration Web site. http://www.fda.gov/drugs/drugsafety/ucm297391.htm. Updated February 15, 2013. Accessed February 28, 2014.
22. Changes to the VA National Formulary–October 1998 to October 2015. http://www.pbm.va.gov/nationalformulary.asp. Accessed November 9, 2015.
23. Krystal JH, Rosenheck RA, Cramer JA, et al; Veterans Affairs Cooperative Study No. 504 Group. Adjunctive risperidone treatment for antidepressant-resistant symptoms of chronic military service-related PTSD: a randomized trial. JAMA. 2011;306(5):493–502. doi:10.1001/jama.2011.1080 PubMed
24. Nelson EM, Philbrick AM. Avoiding serotonin syndrome: the nature of the interaction between tramadol and selective serotonin reuptake inhibitors. Ann Pharmacother. 2012;46(12):1712–1716. doi:10.1345/aph.1Q748 PubMed
25. Spoont M, Sayer N, Nelson DB. PTSD and treatment adherence: the role of health beliefs. J Nerv Ment Dis. 2005;193(8):515–522. doi:10.1097/01.nmd.0000172474.86877.2b PubMed
26. Huggins JM, Brown JN, Capehart B, et al. Medication adherence in combat veterans with traumatic brain injury. Am J Health Syst Pharm. 2011;68(3):254–258. doi:10.2146/ajhp090629 PubMed
27. Ener RA, Meglathery SB, Van Decker WA, et al. Serotonin syndrome and other serotonergic disorders. Pain Med. 2003;4(1):63–74. PubMed
Enjoy this premium PDF as part of your membership benefits!

