Chronic skin disease has a devastating effect on a person’s physical and psychological well-being. Skin disease significantly impacts all aspects of a patient’s life including school, relationships, career choices, social and leisure activities, and sexual life. The physical, psychological, and social consequences affect not only the patients, but also caregivers and family members as well. Common psychological problems associated with skin disease include, but are not limited to, feelings of stress, anxiety, anger, depression, shame, social isolation, low self-esteem, and embarrassment. Besides psychopharmacology, multiple psychotherapeutic techniques have proved to be helpful in addressing the psychological sequelae of skin disease.

ABSTRACT
Chronic skin disease has a devastating effect on a person’s physical and psychological well-being. Skin disease significantly impacts all aspects of a patient’s life including school, relationships, career choices, social and leisure activities, and sexual life. The physical, psychological, and social consequences affect not only the patients, but also caregivers and family members as well. Common psychological problems associated with skin disease include, but are not limited to, feelings of stress, anxiety, anger, depression, shame, social isolation, low self-esteem, and embarrassment. Besides psychopharmacology, multiple psychotherapeutic techniques have proved to be helpful in addressing the psychological sequelae of skin disease.
Prim Care Companion CNS Disord 2018;20(2):17nr02247
To cite: Jafferany M, Pastolero P. Psychiatric and psychological impact of chronic skin disease. Prim Care Companion CNS Disord. 2018;20(2):17nr02247.
To share: https://doi.org/10.4088/PCC.17nr02247
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Central Michigan University, Saginaw, Michigan
*Corresponding author: Mohammad Jafferany, MD, FAPA, Department of Psychiatry, Central Michigan University, Saginaw, MI 48603 ([email protected]).
Chronic skin disease has a devastating effect on a person’s physical and psychological well-being and impacts all aspects of life—from schooling, relationships, and career choices to social activities, sexual life, and leisure activities. The physical, psychological, and social consequences affect not only the patients, but also caregivers and family members as well. Common psychological problems associated with skin disease include, but are not limited to, feelings of stress, anxiety, anger, depression, shame, social isolation, low self-esteem, and embarrassment. Besides psychopharmacology, multiple psychotherapeutic techniques have proved to be helpful in addressing the psychological sequelae of skin disease.
The association between psychological stress and manifestation or exacerbation of different skin diseases is well established.1 In a cross-sectional web-based survey2 in a university sample of 422 participants, heightened stress levels associated with pruritus, alopecia, seborrhea, hyperhidrosis, and trichotillomania were reported. The indifference of those not directly affected is often exacerbated by the misplaced assumption that skin diseases are contagious or caused by poor hygiene, leading to feelings of isolation and depression among those struggling with skin issues. Furthermore, many studies3 have shown a direct correlation between skin disease and a higher risk of substance abuse. Even more concerning is the reported increased incidence of suicidal ideation and intent in those with skin disease.4
The most common skin conditions associated with higher levels of distress are eczema, psoriasis, alopecia, and acne. Other conditions that contribute to psychosocial stress to varying degrees include vitiligo, urticaria, rosacea, herpes simplex and zoster, viral warts, and some tumors.5
PSYCHOSOCIAL IMPACT OF SKIN DISEASE
The psychological and social impact of skin disease depends heavily on the sites affected and distribution of symptoms, the attitude of the individual, and the prevailing culture toward skin disease. A patient’s social support, consisting of family and interpersonal relationships, and the patient’s coping skills and belief system all play an important role in the management of psychological sequelae. Social stigma can adversely affect and exacerbate the patient’s mental distress. In a study6 involving 510 acne patients, participants reported high levels of psychological and emotional problems that were comparable with other chronic medical conditions such as asthma, seizure disorder, diabetes, chronic back pain, and arthritis.
Patients with a chronic skin condition will seek diagnostic evaluation and treatment to improve multiple facets of their day-to-day life, including their psychological health, social functioning, professional life, sleep quality, and overall disposition. These holistic qualities combined define quality of life—how individuals perceive their position in life in the context of the cultural value system in which they live and in relation to their goals, expectations, standards, and concerns. Skin disease can significantly affect a person’s ability to socialize and interact with other people. Thus, making and maintaining personal and intimate relationships may be difficult for this population. In a survey7 conducted by the British Skin Foundation, 29% of those surveyed felt that their skin condition was an active barrier in finding a partner, 20% felt it was a major factor in a breakup, and 56% reported low self-confidence, difficulty making friends, and weak sexual performance.

- The social and psychological impact of skin disease affects patients and their caregivers and family members.
- Due to various cultural perspectives regarding skin disease, a physician should be culturally competent to appropriately diagnosis, manage, and educate patients and their families.
- Psychosocial intervention improves disease severity and enhances quality of life.
Social isolation is often a product of chronic skin disease and leads to impairment in the overall psychological well-being of patients.8 Those with severe acne and scarring actively try to avoid social situations and present with feelings of low self-confidence and self-esteem. Patients with vitiligo frequently report a negative impact in sexual relationships and a high level of embarrassment. Patients with vulvodynia report persistent unexplained pain that prevents them from enjoying an active sexual lifestyle.8
Physical and leisure activities are other social spheres that are affected by chronic skin diseases. Physical impairment is common in many chronic skin conditions. Patients with severe psoriatic arthritis often experience decreased mobility, which leads to psychological stress due to their inability to attend social gatherings.9 Extended periods of immobility contribute to feelings of loneliness and depression. Post-herpetic neuralgia and chronic leg ulcers have similar repercussions.10
Many studies11 have shown that children with visible skin disease are subjects of bullying. Bullying leads to withdrawal, isolation, low self-esteem, absenteeism, and consequent academic decline in these patients. It is important to realize that it is not just the patient who suffers, but also the family and friends who bear the brunt of the psychosocial repercussions of chronic skin disease. Parents caring for a child with chronic eczema may feel distressed about their child’s emotional health and their inability to help. Parents also experience feelings of guilt, hopelessness, helplessness, and depression.12
Sleep disturbance is common in patients with chronic skin disease. In 1 study,13 sleep disturbances and impaired quality of sleep were noted in 60% of children with eczema. During an exacerbation, this percentage increased to 83%. The decreased quality of sleep was associated with behavioral deficits that affected social and academic development, leading to psychosocial stress for the child and family.13 As a result, both parents and siblings of these patients often have a decline in academic and work performance.
Cultural awareness plays a more prominent role in psychosomatic medicine compared to other fields. Given that the world is a global village and the rise of multicultural societies in various countries, it is becoming increasingly important for providers to familiarize themselves with a patient’s social and psychological needs. In the context of psychodermatology, myths and beliefs about skin diseases by different ethnic and cultural groups may have a profound effect on the patient’s ability to cope with the distress associated with his or her skin condition. Vitiligo is commonly associated with stigma, which is particularly more relevant among darker-skinned patients.14 The increased visibility in these patients has led to higher levels of psychological distress. In some cultures and ethnic groups, skin color is regarded as a parameter of beauty in women. In other cultures, due to its presentation, there is a stigmatization of vitiligo similar to that of leprosy.14 Culturally, the loss of skin pigmentation may threaten ethnic identity, adding another dimension to the psychological distress experienced by these patients.15 Difficulties in finding life partners for marriage may also result.15 Often, an empathetic interpreter is needed to translate the patient’s language and convey his or her psychological feelings to the physician.
Hair and skin share a similar weight in importance with regard to cultural identity. Hair has a religious importance in various religious groups such as Sikhs and Rastafarians. Across cultures throughout history, hair has often reflected one’s society and virility.16 Ornate hairstyles in Europe during the 1700s reflected the economic standing of the individual, as they were expensive to maintain.17 Multimillion dollar industries are built on maintaining the perception of excellent hair including the use of wigs, hair transplants, and concealing powders and sprays. With the high prevalence of comorbid psychiatric illnesses with conditions such as alopecia,18 physicians and patients should be made aware of the options available to increase patient self-esteem and overall quality of life.
EVALUATING AND MANAGING PSYCHOLOGICAL SEQUELAE OF CHRONIC SKIN DISEASE
It is critical for health care professionals to be knowledgeable and sympathetic toward patients’ physical and mental needs. Patients should be able to feel comfortable enough to convey their concerns and confident that what is expressed is said in a safe, private, and nonjudgmental environment. Besides creams, ointments, and medications used to treat skin conditions, patients could benefit from psychotherapeutic techniques to relieve their anxiety, depression, and other psychological distress. Psychological intervention has been shown to be beneficial in numerous studies.19 In a meta-analysis19 involving 22 studies, psychological intervention was shown to have a medium-to-large-sized effect on the severity of skin conditions, psychosocial outcomes, and itch and scratch reaction.
Health-related quality of life is an important aspect of care for chronic skin conditions. Patients have the opportunity to express their opinions about the value they place on health and how their condition and its treatment affect their quality of life. It is important to assess health-related quality of life during the course of treatment to measure the physical and psychological successes and failures of interventions.
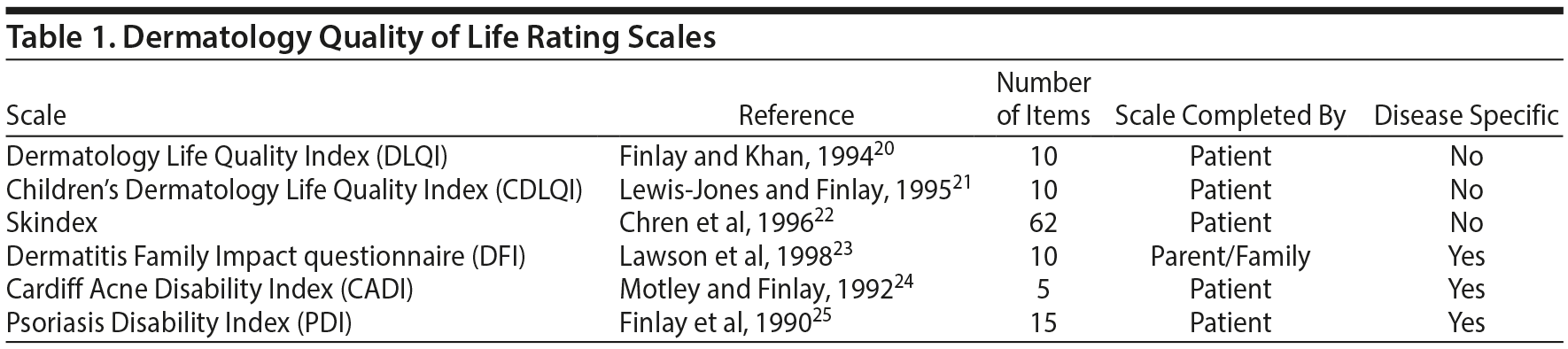
General standardized questionnaires are one example of the many tools used to measure health-related quality of life. Some are scorable, while others allow more variable responses. The design of questionnaires can vary. Some are meant to be used across all disease states, while others are more specific for a limited range of skin diseases (Table 1). Questionnaires are also available for specific skin diseases.
The most widely used dermatology-specific measurement tools employed are the Dermatology Life Quality Index (DLQI)20 and the Skindex.22 The Children’s Dermatology Life Quality Index (CDLQI)21 is a general dermatology measure specifically for children. The DLQI and CDLQI are useful tools in assessing the psychosocial impact of skin disorders. The DLQI, developed in 1994 and available in over 90 languages, contains 10 questions covering a wide range of areas of the body affected by skin disease. The questionnaire addresses symptoms; level of embarrassment; interference with shopping or housework; choice of clothing; participation in social and leisure activities; participation in athletic, academic, and professional activities; sexual relationships; and the effects of treatment. The responses range from “not at all” to “very much.”
The Skindex was developed as a method to allow patients the opportunity to convey the unseen problems they may experience in association with their skin disease. Patients who present with a relatively small skin lesion may be significantly more distressed than a patient with a larger physical deformity. The Skindex is a 62-item self-administered survey with 8 scales measuring the cognitive, social, and emotional aspects of chronic skin diseases. There are more abbreviated forms of the Skindex, such as the Skindex-29 and Skindex-16, which have 29 and 16 items, respectively.
The Dermatitis Family Impact questionnaire (DFI)23 is a 10-question survey completed by a family member (typically the caregiver) of the affected child. This questionnaire differs from the Skindex and the DLQI in that it is directed to the family and not the patient. The DFI analyzes various aspects of life such as shopping, leisure activities, food preparation, and emotional distress that may be present in the family member due to the child’s having dermatitis. The responses range from “not at all” to “very much.” These surveys have been widely used to assess the degree of psychosocial stress and the success of interventions.
ATOPIC DERMATITIS
Atopic dermatitis is an inflammatory skin condition characterized by pruritus, redness, and cracked dry skin. Atopic dermatitis is seen in 15%-20% of children.26 Sleep is integral in the development and well-being of children. A common problem with atopic dermatitis is its negative effect on sleep. Children with intense pruritus often have difficulty falling asleep, which leads to issues with learning and day-to-day functioning due to increased fatigue. This psychosocial problem stemming from atopic dermatitis extends further than the dermatologic field. Sleep is a key factor in the overall well-being of a patient. Barilla et al27 indicated that sleep-targeted therapies for those with atopic dermatitis are important, as they allow for greater satisfaction with treatment.
In infants with atopic dermatitis, skin sensation may be altered due to chronic inflammatory changes.28 Emotional development may be impaired because skin performs a major role in the development of communication and sensory perception.28 Children and their parents develop a stronger bond through touch, fostering feelings of well-being and self-esteem.29 Furthermore, using the CDLQI, Beattie and Lewis-Jones30 illustrated that parents observed their children to have impairment in quality of life comparable to that of children with cystic fibrosis and renal disease.
Parents should be cautious with regard to interventions for their children. Due to the chronic nature of atopic dermatitis, parents often encourage physicians to prescribe medications, provide referrals, and initiate unnecessary testing. Schmitt et al31 found that compared to healthy controls, children on chronic antihistamine therapy had an increase in attention-deficit/hyperactivity disorder symptoms, warranting further investigation. Physicians should make time to empathize, understand, and address any concerns the patients and their families may have and prescribe appropriate treatments with side effects in mind.
In adult populations, loss of productivity at work due to poor sleep and chronic stress can result from atopic dermatitis. Furthermore, loss of income can occur due to taking sick leave and making expenditures on specialized clothing, emollients, creams, and treatments. In the social setting, patients often have concerns with their attractiveness, which affects their work prospects and ability to develop personal relationships. Kiebert et al32 found that adult patients with atopic dermatitis had lower mental health component scores than patients with diabetes or hypertension. Patients may be unaware of how many aspects of their life are affected by their skin conditions and require a thorough evaluation by their physician to address all of their concerns.
ACNE
Acne is a common skin condition often accepted as a general problem that people must cope with. It is estimated that 93.3% of adolescents aged 16-18 years experience acne.33 Thus, this condition is often underappreciated by both laypeople and medical staff. In reality, the psychosocial and emotional problems stemming from acne are comparable to those of diabetes, epilepsy, asthma, and arthritis.34
Depression and anxiety have been associated with acne.35 Self-image and self-esteem are greatly affected, and forming interpersonal relationships with others becomes increasingly more difficult, especially in adolescent populations. Social phobia was found to affect 45.7% of high school patients with acne compared to 18.4% of patients in the control group.36 Further exacerbating the problems associated with acne is the increased incidence of bullying. Bullying was found to be experienced significantly more in teenagers with acne compared to those without.37 When treating acne, it is important to manage the cosmetic aspect of health and the patient’s overall psychosocial well-being. Isotretinoin has been shown to be efficacious in decreasing anxiety and depression scores using the Hospital Anxiety and Depression Scale.38
Acne can have a significant effect on a patient’s quality of life.40 DLQI responses analyzed by Tasoula et al39 showed that approximately 21% of the patients surveyed reported that their schoolwork and personal activities were negatively affected, and 19.2% admitted that acne affected their personal lives. In regard to social withdrawal and isolation, 14% of those surveyed admitted to avoiding physical activities such as swimming to prevent embarrassment.39 Patients with postinflammatory hyperpigmentation also suffer from a decreased quality of life. In a study by Darji et al,40 subjects with post-inflammatory hyperpigmentation reported statistically significant poor mean scores on the Acne-QoL survey compared to subjects with acne only, indicating that patients with post-inflammatory hyperpigmentation and acne had negatively impacted self-perceptions and social functioning.
PSORIASIS
Psoriasis is an autoimmune inflammatory condition that results in hyperproliferation that presents as red or silver scaly skin, atrophic nail changes, and plaques. Systemic therapy is often required to manage the symptoms. Approximately 1.4%-2.0% of the population is affected by psoriasis.26 Along with the cosmetic symptoms, psoriasis also can cause severe pain in the form of arthritis. One study41 found that both physical and mental functioning were reduced in patients with psoriasis, similar to that in arthritis, depression, cancer, and coronary vascular disease.
There are numerous neuropsychiatric comorbidities among psoriatic patients. In an adolescent population, Galili et al42 demonstrated that patients had a higher frequency of headaches, anxiety disorders, and impaired social adjustment skills compared to healthy controls. Furthermore, patients with psoriasis often report depression.43 Although psoriasis is not fatal, patients are at an increased risk of suicide.43 The degree of severity of pruritus associated with plaque psoriasis has been correlated to the severity of depression.44 Patients report embarrassment due to the appearance of psoriasis and the difficulty in masking it. Social isolation often results, and activities such as swimming and other recreational activities are often avoided. Ginsburg and Link45 reported that 19% of patients with moderate to severe psoriasis had experienced social rejection, such as being asked to leave the pool or gym. Female patients were more likely to report a decrease in quality of life than men, although the impact of the disease decreased with increasing age.46
Management of psoriasis requires a knowledgeable physician to efficiently diagnose and manage the condition and provide the appropriate resources and referrals when necessary. Disease-modifying antirheumatic drugs are indicated for the management of psoriasis.47 These medications can affect patient quality of life due to toxic side effects and immunosuppression that may result from their use. Stress-reduction techniques have been shown to complement pharmacologic management.47
VITILIGO
Vitiligo is characterized by the lack of pigmentation of the skin that is well-circumscribed. Its distribution can range from small localized areas of skin to a large area of depigmentation. Vitiligo has a worldwide prevalence of 0.5%-2%.48 Although the disorder is not associated with pruritus or other acute skin pathology, it has a significant impact on the well-being of those afflicted. Patients often view vitiligo as a disfigurement and a reason to be ashamed. Cultural identity in terms of skin color and conformity contribute to the increased stress and feelings of isolation, stigmatization, and inadequacy.14 Patients are often burdened by the need to cover up the disorder with clothing or makeup.15 Due to the increased stress and pressures from society, patients with vitiligo often experience severe psychological problems including anxiety, depression, social withdrawal, and suicidal ideation.
Parents and families of children with vitiligo also experience psychosocial stress. In a survey49 of Chinese families, parents of children with vitiligo tended to be affected in terms of psychosocial health. According to results of the DFI, aspects such as shopping, leisure activities, and housework were significantly more affected in families of vitiligo patients compared to those in the control group.49 Families that follow more traditional societal norms place a great emphasis on marriage. Vitiligo was found to be a barrier to marriage in a study15 in Saudi Arabia. Over half of 898 men and women surveyed stated they would not marry an individual with vitiligo. Even when married, quality of life is affected due to the skin condition. In an Indian study,50 married female patients with vitiligo had higher DLQI scores compared to males. This discrepancy attributed to discrimination and social conflict with in-law relatives.50
Depression is a common disorder present in this population. In a study50 of Indian patients, 59% of vitiligo patients sampled were found to have depression. In the same study,50 vitiligo patients displayed higher overall DLQI scores compared to the control group. This incidence of depression was also evident in an Italian study51 wherein 31% of those evaluated responded that they were depressed “often” or “all the time” using the Skindex. Females were found to be more affected by depression than males.51 Of concern is the suicidal ideation that has been documented in patients who suffer significant psychosocial stress and lack appropriate coping skills.42
ALOPECIA
Alopecia is a common inflammatory condition defined by hair loss. The regions affected can be small and well-circumscribed (alopecia areata) or may involve a universal loss of body hair (alopecia universalis). Alopecia affects both sexes equally across all age ranges and has a prevalence in the United States of approximately 0.1%-0.2%.52 The risk of alopecia areata compared to alopecia totalis and universalis is approximately 5%.52 As this disease is autoimmune in nature, autoimmune conditions such as thyroid disorders, inflammatory bowel disease, and anemias frequently occur in those affected by alopecia. There are no definitive treatments for alopecia.
Given the increasing pressure on physical appearance, those with alopecia are often subject to feelings of embarrassment and shame. Patients often attempt to cover up their hair loss with wigs and hats or resort to cutting off all their hair. Although some relief is provided by these methods, anxiety associated with concealing hair loss is significant.53 Alopecia areata is often misdiagnosed as tinea capitis, a fungal infection of the scalp. Concerns that alopecia is contagious also negatively contribute to patients’ feelings of self-worth. Left unaddressed, the psychological stressors may manifest into more severe psychiatric pathology.
Depression and anxiety are commonly seen in patients with alopecia. In a survey53 performed in the United Kingdom of 338 participants aged ≥ 13 years, clinically significant levels of anxiety and depression were reported in patients with alopecia. Of concern was that almost half of those surveyed were found to have social anxiety.53 Using the Beck Depression Inventory and the Eysenck Personality Questionnaire, Aghaei et al18 found that depression, stress, and neuroses were significantly present in patients with alopecia compared to a control group. They further concluded that size and placement of the lesions contribute to different psychological reactions.18
Quality of life has been shown in various studies54,55 to be significantly affected by alopecia. Among pediatric populations, the emotional impact of the disease is evident. Children of all ages with alopecia have experienced bullying, with males experiencing increased physical bullying.54 Using the DLQI, Williamson and colleagues55 found that quality of life was significantly impacted by hair loss due to alopecia, with 40% of the patients surveyed reporting dissatisfaction with the way their doctor interacted with them. Various treatments are available for alopecia, but relapse rates continue to be high.56 It is important for physicians to provide realistic management expectations and refer patients to appropriate counseling services to better manage the psychological aspect of the condition.
GENERAL PRINCIPLES OF MANAGEMENT
As discussed previously, psychosocial intervention has been shown to have a significant impact on not just the psychosocial pathology but also on the severity of skin disease itself.19 The physician’s approach to the patient, education provided, and interventions initiated all play an important role in managing chronic skin disease.
Dermatologic conditions are common in the primary care setting. A retrospective study57 from the University of Miami over a 2-year period found that 36.5% of patients presented with at least 1 dermatologic problem. In a survey58 of 12,000 patients in the Netherlands, 65.1% of patients reported contacting only their primary care physician for management of dermatologic conditions. Patients typically present first to primary care for evaluation and treatment of skin disorders; thus, primary care providers have the opportunity to address the psychiatric and psychological pathology that accompanies the physical malady by involving behavioral health staff. Collocated behavioral and primary health staff facilitate this collaboration and have been shown to decrease no-show rates.59 Behavioral staff, in turn, should also begin to familiarize themselves with the field of psychodermatology to fully understand the medical limitations and risks that medication and therapy plans may have for the patient. The following therapeutic modalities have proved helpful in the management of patients experiencing the psychological effects of chronic skin disease:
- Empathy
- Acknowledge and validate the patient’s concerns
- Spend extra time during exacerbation of disease and at the time of initial diagnosis
- Ask about psychosocial and economic effects of skin disease
- Education
- Provide education to the patient and answer questions about the natural history, medical management, prognosis, and likely social complication of skin disease
- Dispel common misconceptions about contagiousness
- Discuss possible pharmacologic treatment-related side effects
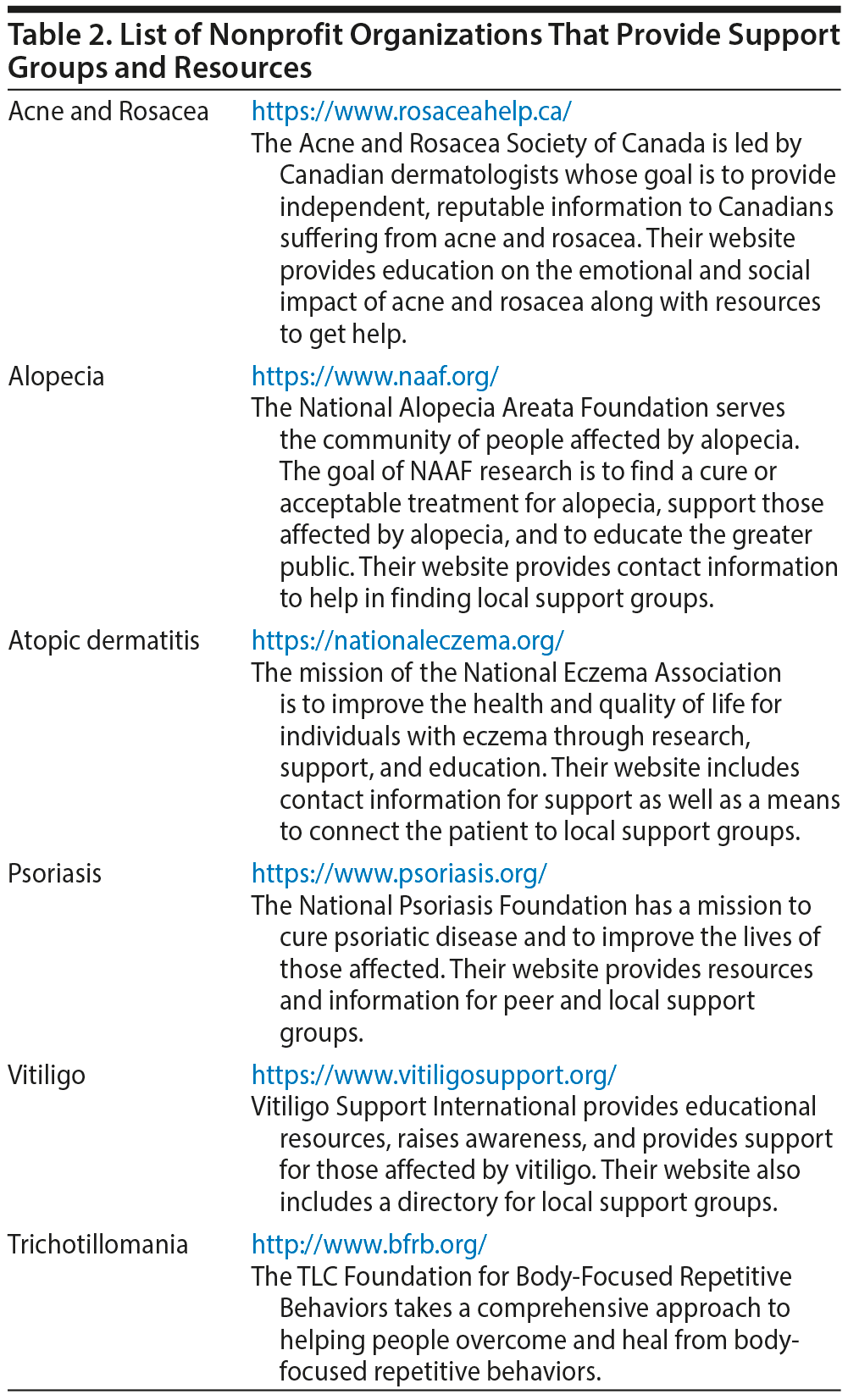
- Provide resources such as handouts or referral to support groups and websites (Table 2)
- Medical management
- Use of emollients, creams, and oral medications for management of skin pathology
- Use of psychotropic medications to address comorbid psychiatric illnesses
- Use of psychotropic medications to treat primary psychiatric illness related to skin pathology, such as skin picking, trichotillomania, or delusions of parasitosis
- Stress management
- Inform the patient about the role of stress in the causation and exacerbation of skin disease
- Provide techniques and resources to better manage stress to control disease exacerbations
- Psychotherapy
- Cognitive-behavioral therapy (CBT): The primary focus of CBT is to address dysfunctional thought patterns and behaviors. A patient’s dysfunctional thoughts and feelings are addressed by altering the underlying cognition and behavior. CBT has been shown to be efficacious in the management of both pruritic and nonpruritic dermatoses60 as well as in patients with chronic pain.61
- Acceptance and commitment therapy (ACT): ACT focuses on strengthening of psychological flexibility.62 Although ACT has been shown to decrease the severity of symptoms in patients with pain, depression, and personality disorders,63 its fundamental purpose is to change the relationship of the patient with his/her symptoms through the use of mindfulness skill development.
- Mindfulness-based stress reduction (MBSR): MBSR includes practices such as meditation, exercise, and yoga. The goal of mindfulness is to maintain awareness of the present and disengage oneself from strong attachment to beliefs or emotions, leading to emotional balance and well-being.64 MBSR has been effective in treating chronic pain and has been shown to be efficacious in the management of moderate to severe psoriasis.65
- Habit reversal therapy (HRT): HRT aims to replace or alter dysfunctional behaviors and replace them with neutral actions. It consists of 3 major components: awareness training, replacing dysfunctional behaviors with a competing response, and motivational techniques such as social support or behavioral reward systems.66 HRT has been found to be beneficial in the management of self-inflicted lesions such as skin picking.67
- Family and child interventions: Education regarding the impact of various psychocutaneous disorders on the family and child interactions and disruption of bonding between the mother and child, for example, in cases of severe atopic eczema and other chronic skin diseases, should be prioritized before considering various therapeutic options.
CONCLUSION
The scope of effects from chronic skin conditions extends beyond that of dermatology alone. Neuropsychiatric pathologies ranging from depression and anxiety to familial stressors and cultural identity have been identified and analyzed by numerous studies. Atopic dermatitis, acne, alopecia, psoriasis, and vitiligo all have a strong impact on a patient’s overall physical and mental well-being. They affect patients’ self-esteem as well as their ability to relate to others and develop and pursue a full life on the basis of their cultural definition. Identification of the other issues related to the skin disorder (eg, psychiatric) is the first step to addressing, destigmatizing, and treating these patients holistically and to improving their overall quality of life. The role of a physician as a healer is to treat the visible and invisible aspects of disease.
Submitted: November 10, 2017; accepted January 18, 2018.
Published online: April 26, 2018.
Financial disclosure: Drs Jafferany and Pastolero have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: None.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, isotretinoin is not approved by the US Food and Drug Administration for the treatment of anxiety or depression.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Rodriquez-Vallecio E, Woodbury-Farina MA. Dermatological manifestation of stress in normal and psychiatric population. Psychiatr Clin North Am. 2014;37(4):625-651. PubMed CrossRef
2. Schut C, Mollanazar NK, Sethi M, et al. Psychological stress and skin symptoms in college students: results of a cross-sectional web-based questionnaire study. Acta Derm Venereol. 2016;96(4):550-551. PubMed CrossRef
3. Ferreira BR, Pio-Abreu JL, Reis JP, et al. Analysis of the Prevalence of Mental Disorders in Psoriasis: The Relevance of Psychiatric Assessment in Dermatology. Psychiatr Danub. 2017;29(4):401-406. PubMed CrossRef
4. Picardi A, Lega I, Tarolla E. Suicide Risk in skin disorders. Clin Dermatol. 2013;31(1):47-56. PubMed CrossRef
5. Shenefelt PD. Psychological interventions in the management of common skin conditions. Psychol Res Behav Manag. 2010;3:51-63. PubMed CrossRef
6. Ismail KH, Mohammaed-Ali KB. Quality of life in patients with acne in Erbil city. Health Qual Life Outcomes. 2012;10(1):60. PubMed CrossRef
7. Smithard A, Glazebrook C, Williams H. Acne prevalence, knowledge about acne and psychological morbidity in mid-adolescence: a community-based study. Br J Dermatol. 2001;145(2):274-279. PubMed CrossRef
8. Narang T. Garima, Singh, SM. Psychosexual disorders and dermatologists. Indian Dermatol Online J. 2016;7(3):149-158. PubMed CrossRef
9. Hong J, Koo B, Koo J. The psychosocial and occupational impact of chronic skin disease. Dermatol Ther (Heidelb). 2008;21(1):54-59. PubMed CrossRef
10. Johnson RW, Bouhassira D, Kassianos G, et al. The impact of herpes zoster and post-herpetic neuralgia on quality-of-life. BMC Med. 2010;8(1):37. PubMed CrossRef
11. Chernyshov PV. Stimagtization and self-perception in children with atopic dermatitis. Clin Cosmet Investig Dermatol. 2016;9:159-166. PubMed CrossRef
12. Pauli-Pott U, Darui A, Beckmann D. Infants with atopic dermatitis: maternal hopelessness, child-rearing attitudes and perceived infant temperament. Psychother Psychosom. 1999;68(1):39-45. PubMed CrossRef
13. Cafferman D, Kennedy JD, Gold M, et al. Eczema, sleep, and behavior in children. J Clin Sleep Med. 2010;6(6):581-588. PubMed
14. Alghamdi KM, Moussa NA, Mandil A, et al. Public perceptions and attitudes toward vitiligo. J Cutan Med Surg. 2012;16(5):334-340. PubMed CrossRef
15. Thompson AR, Clarke SA, Newell RJ, et al; Appearance Research Collaboration. Vitiligo linked to stigmatization in British South Asian women: a qualitative study of the experiences of living with vitiligo. Br J Dermatol. 2010;163(3):481-486. PubMed CrossRef
16. Muscarella F, Cunningham MR. The evolutionary significance and social perception of male pattern baldness and facial hair. Ethol Sociobiol. 1996;2(2):99-117. CrossRef
17. Saed S, Ibrahim O, Bergfeld WF. Hair camouflage: a comprehensive review. Int J Womens Dermatol. 2016;2(4):122-127. PubMed CrossRef
18. Aghaei S, Saki N, Daneshmand E, et al. Prevalence of psychological disorders in patients with alopecia areata in comparison with normal subjects. ISRN Dermatol. 2014:304370. PubMed CrossRef
19. Lavda AC, Webb T, Thompson AR. A meta-analysis of the effectiveness of psychological interventions for adults with skin conditions. Br J Dermatol. 2012;167(5):970-979. PubMed CrossRef
20. Finlay AY, Khan GK. Dermatology Life Quality Index (DLQI)—a simple practical measure for routine clinical use. Clin Exp Dermatol. 1994;19(3):210-216. PubMed CrossRef
21. Lewis-Jones MS, Finlay AY. The Children’s Dermatology Life Quality Index (CDLQI): initial validation and practical use. Br J Dermatol. 1995;132(6):942-949. PubMed CrossRef
22. Chren MM, Lasek RJ, Quinn LM, et al. Skindex, a quality-of-life measure for patients with skin disease: reliability, validity, and responsiveness. J Invest Dermatol. 1996;107(5):707-713. PubMed CrossRef
23. Lawson V, Lewis-Jones MS, Finlay AY, et al. The family impact of childhood atopic dermatitis: the Dermatitis Family Impact Questionnaire. Br J Dermatol. 1998;138(1):107-113. PubMed CrossRef
24. Motley RJ, Finlay AY. Practical use of a disability index in the routine management of acne. Clin Exp Dermatol. 1992;17(1):1-3. PubMed CrossRef
25. Finlay AY, Khan GK, Luscombe DK, et al. Validation of Sickness Impact Profile and Psoriasis Disability Index in psoriasis. Br J Dermatol. 1990;123(6):751-756. PubMed CrossRef
26. Julian CG. Dermatology in general practice. Br J Dermatol. 1999;141(3):518-520. PubMed CrossRef
27. Barilla S, Felix K, Jorizzo JL. Stressors in atopic dermatitis. Adv Exp Med Biol. 2017;1027:71-77. PubMed CrossRef
28. Nadelson T. A person’s boundaries: a meaning of skin disease. Cutis. 1978;21(1):90-93. PubMed
29. Koblenzer PJ. Parental issues in the treatment of chronic infantile eczema. Dermatol Clin. 1996;14(3):423-427. PubMed CrossRef
30. Beattie PE, Lewis-Jones MS. A comparative study of impairment of quality of life in children with skin disease and children with other chronic childhood diseases. Br J Dermatol. 2006;155(1):145-151. PubMed CrossRef
31. Schmitt J, Buske-Kirschbaum A, Tesch F, et al. Increased attention-deficit/hyperactivity symptoms in atopic dermatitis are associated with a history of antihistamine use. Allergy. 2018;73(3):615-626. PubMed CrossRef
32. Kiebert G, Sorensen SV, Revicki D, et al. Atopic dermatitis is associated with a decrement in health-related quality of life. Int J Dermatol. 2002;41(3):151-158. PubMed CrossRef
33. Bagatin E, Timpano DL, Ramos dos Sandos Guadanhim L. Acne vulgaris: prevalence and clinical forms in adolescents from Sao Paulo, Brazil. An Bras Dermatol. 2014;89(3):428-435. PubMed CrossRef
34. Mallon E, Newton JN, Klassen A, et al. The quality of life in acne: a comparison with general medical conditions using generic questionnaires. Br J Dermatol. 1999;140(4):672-676. PubMed CrossRef
35. Halvorsen JA, Stern RS, Dalgard F, et al. Suicidal Ideation, mental health problems, and social impairment are increased in adolescent with acne: A Population-based study. J Invest Dermatol. 2011;131(2):363-370. PubMed CrossRef
36. Bez Y, Tesilova Y, Kaya MC, et al. High social phobia frequency and related disability in patients with acne vulgaris. Eur J Dermatol. 2011;21(5):756-760. PubMed
37. Ritvo E, Del Ross JQ, Stillman MA, et al. Psychosocial judgments and perceptions of adolescents with acne vulgaris: a blinded, controlled comparison of adult and peer evaluations. Biopsychosoc Med. 2011;5(1):11. PubMed CrossRef
38. Marron SE, Tomas-Aragones L, Boira S. Anxiety, depression, quality of life and patient satisfaction in acne patients treated with oral isotretinoin. Acta Derm Venereol. 2013;93(6):701-706. PubMed CrossRef
39. Tasoula E, Gregoriou S, Chalikias J, et al. The impact of acne vulgaris on quality of life and psychic health in young adolescents in Greece: results of a population survey. An Bras Dermatol. 2012;87(6):862-869. PubMed CrossRef
40. Darji K, Varade R, West D, et al. Psychosocial impact of postinflammatory hyperpigmentation in patients with acne vulgaris. J Clin Aesthet Dermatol. 2017;10(5):18-23. PubMed
41. Gupta MA, Gupta AK. Depression and suicidal ideation in dermatology patients with acne, alopecia areata, atopic dermatitis and psoriasis. Br J Dermatol. 1998;139(5):846-850. PubMed CrossRef
42. Galili E, Barzilai A, Shreberk-Hassidim R, et al. Neuropsychiatric comorbidity among adolescents with psoriasis [published online ahead of print October 8, 2017]. Br J Dermatol. PubMed CrossRef
43. Gupta MA, Gupta AK, Schork NJ, et al. Depression modulates pruritus perception: a study of pruritus in psoriasis, atopic dermatitis, and chronic idiopathic urticaria. Psychosom Med. 1994;56(1):36-40. PubMed CrossRef
44. Rapp SR, Feldman SR, Exum ML, et al. Psoriasis causes as much disability as other major medical diseases. J Am Acad Dermatol. 1999;41(3):401-407. PubMed CrossRef
45. Ginsburg IH, Link BG. Feelings of stigmatization in patients with psoriasis. J Am Acad Dermatol. 1989;20(1):53-63. PubMed CrossRef
46. McKenna KE, Stern RS. The impact of psoriasis on the quality of life of patients from the 16-center PUVA follow-up cohort. J Am Acad Dermatol. 1997;36(3):388-394. PubMed CrossRef
47. Ben-Arye E, Ziv M, Frenkel M, et al. Complementary medicine and psoriasis: linking the patient’s outlook with evidence-based medicine. Dermatology. 2003;207(3):302-307. PubMed CrossRef
48. Kr×¼ger C, Schallreuter KU. A review of the worldwide prevalence of vitiligo in children/adolescents and adults. Int J Dermatol. 2012;51(10):1206-1212. PubMed CrossRef
49. Amer AA, Mchepange UO, Gao XH, et al. Hidden victims of childhood vitiligo: impact on parents’ mental health and quality of life. Acta Derm Venereol. 2015;95(3):322-325. PubMed CrossRef
50. Sangma LN, Nath J, Bhagabati D. Quality of life and psychological morbidity in vitiligo patients: a study in a teaching hospital from north-east India. Indian J Dermatol. 2015;60(2):142-146. PubMed CrossRef
51. Sampogna F, Tabolli S, Abeni D. Impact of different skin conditions on quality of life. G Ital Dermatol Venereol. 2013;148(3):255-261. PubMed
52. Safavi K. Prevalence of alopecia areata in the first National Health and Nutrition Examination Survey. Arch Dermatol. 1992;128(5):702. PubMed CrossRef
53. Montgomery K, White C, Thompson A. A mixed methods survey of social anxiety, anxiety, depression, and wig use in alopecia. BMJ Open. 2017;7(4):e015468. PubMed CrossRef
54. Christensen T, Yang JS, Castelo-Soccio L. Bullying and quality of life in pediatric alopecia areata. Skin Appendage Disord. 2017;3(3):115-118. PubMed CrossRef
55. Williamson D, Gonzalez M, Finlay AY. The effect of hair loss on quality of life. J Eur Acad Dermatol Venereol. 2001;15(2):137-139. PubMed CrossRef
56. Gupta AK, Carviel J, Abramovits W. Treating Alopecia Areata: Current Practices Versus New Directions. Am J Clin Dermatol. 2017;18(1):67-75. PubMed CrossRef
57. Lowell BA, Froelich CW, Federman DG, et al. Dermatology in primary care: prevalence and patient disposition. J Am Acad Dermatol. 2001;45(2):250-255. PubMed CrossRef
58. Verhoeven EWM, Kraaimaat FW, van Weel C, et al. Skin diseases in family medicine: prevalence and health care use. Ann Fam Med. 2008;6(4):349-354. PubMed CrossRef
59. Guck TP, Guck A, Badurak-Brack A, et al. No-show rates in partially integrated models of behavioral health care in a primary care setting. Fam Syst Health. 2007;25(2):137-146. CrossRef
60. Shenefelt PD. Biofeedback, cognitive behavioral methods and hypnosis in dermatology: is it all in your mind? Dermatol Ther. 2003;16(2):114-122. PubMed CrossRef
61. Veehof MM, Oskam MJ, Schreurs KM, et al. Acceptance-based interventions for the treatment of chronic pain: a systematic review and meta analysis. Pain. 2011;152(3):533-542. PubMed CrossRef
62. Hayes SC, Luoma JB, Bond FW, et al. Acceptance and commitment therapy: model, processes and outcomes. Behav Res Ther. 2006;44(1):1-25. PubMed CrossRef
63. Powers MB, Zum Vorde Sive Vording MB, Emmelkamp PM. Acceptance and commitment therapy: a meta-analytic review. Psychother Psychosom. 2009;78(2):73-80. PubMed CrossRef
64. Ludwig DS, Kabat-Zinn J. Mindfulness in medicine. JAMA. 2008;300(11):1350-1352. PubMed CrossRef
65. Kabat-Zinn J, Wheeler E, Light T, et al. Influence of mindfulness meditation-based stress reduction interventions on rates of skin clearing in patients with moderate to severe psoriasis undergoing phototherapy (UVB) and photochemotherapy (PUVA). Psychosom Med. 1998;60(5):625-632. PubMed CrossRef
66. Conelea CA, Klein-Tasman BP. Habit reversal therapy for body-focused repetitive behavior in Williams’s syndrome; a case study. J Dev Phys Disabil. 2013;25(6):597-611. PubMed CrossRef
67. Tomas-Aragones L, Consoli SM, Consoli SG, et al. Self-inflicted lesions in dermatology: a management and therapeutic approach—a position paper from the European Society for Dermatology and Psychiatry. Acta Derm Venereol. 2017;97(2):159-172. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!