Objective: To evaluate which body parts preoccupy adolescents with body dysmorphic disorder (BDD).
Methods: Patients admitted to an inpatient psychiatric hospital who agreed to take part in the study completed the Body Dysmorphic Disorder Questionnaire (child and adolescent version) and Body Dysmorphic Disorder Diagnostic Module. Patients also completed a questionnaire that addressed age at onset, coping strategies, history of sexual abuse, amount of time patients spent thinking about their perceived defects, and the area of the body that the participants were preoccupied with and the specific coping strategy used. All patients met DSM-5 criteria for BDD. The study was conducted from January 17, 2014, to September 29, 2014.
Results: Patients with BDD (N = 17) were preoccupied with the face: 6 (35.2%), skin: 3 (17.6%), lips: 5 (29.4%), nose: 3 (17.6%), teeth: 3 (17.6%), ears: 1 (5.8%), and eyes: 1 (5.8%), while gender-specific parts included breasts: 5 (50%) and penis: 4 (57.1%). The mean age at onset of BDD was 10.5 years, and the time spent thinking about the imagined defect averaged 3.5 hours per day.
Conclusions: Patients with BDD are more preoccupied with exposed facial body parts such as skin, lips, nose, teeth, ears, and eyes and body parts with sexual connotations such as breasts in females and the penis in males.
Evaluation of the Body Parts That Preoccupy Adolescents With Body Dysmorphic Disorder

ABSTRACT
Objective: To evaluate which body parts preoccupy adolescents with body dysmorphic disorder (BDD).
Methods: Patients admitted to an inpatient psychiatric hospital who agreed to take part in the study completed the Body Dysmorphic Disorder Questionnaire (child and adolescent version) and Body Dysmorphic Disorder Diagnostic Module. Patients also completed a questionnaire that addressed age at onset, coping strategies, history of sexual abuse, amount of time patients spent thinking about their perceived defects, and the area of the body that the participants were preoccupied with and the specific coping strategy used. All patients met DSM-5 criteria for BDD. The study was conducted from January 17, 2014, to September 29, 2014.
Results: Patients with BDD (N = 17) were preoccupied with the face: 6 (35.2%), skin: 3 (17.6%), lips: 5 (29.4%), nose: 3 (17.6%), teeth: 3 (17.6%), ears: 1 (5.8%), and eyes: 1 (5.8%), while gender-specific parts included breasts: 5 (50%) and penis: 4 (57.1%). The mean age at onset of BDD was 10.5 years, and the time spent thinking about the imagined defect averaged 3.5 hours per day.
Conclusions: Patients with BDD are more preoccupied with exposed facial body parts such as skin, lips, nose, teeth, ears, and eyes and body parts with sexual connotations such as breasts in females and the penis in males.
Prim Care Companion CNS Disord 2017;19(5):17m02154
https://doi.org/10.4088/PCC.17m02154
© Copyright 2017 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Central Michigan University College of Medicine, Saginaw, Michigan
*Corresponding author: Mohammad Jafferany MD, Department of Psychiatry, Central Michigan University College of Medicine, 1000 Houghton Ave, Saginaw, MI 48602 ([email protected]).
Patients with body dysmorphic disorder (BDD) are obsessed with perceived body defects and have associated difficulty in social functioning.1 These patients dislike parts of their body such as the nose, hair, chest, and stomach, with some patients camouflaging their perceived defect and others seeking surgical interventions due to the distress that accompanies the disorder.2 Some patients with BDD are isolated at home and fear being around people because of their perceived body defects.3 Repetitive and excessive preoccupation with grooming, touching, or fiddling with perceived body defects has been reported.2 Similarities between BDD and obsessive-compulsive spectrum disorder with suggestion that they might share similar pathogenic pathways have been reported.4 Although the exact life stage when BDD is most prevalent is subject to debate, most studies5 suggest that the symptoms tend to begin during adolescence, with symptoms oscillating between increased and decreased intensity. Few published studies have focused on the body parts that preoccupy adolescent BDD patients. Thus, the purpose of this study was to identify and evaluate the body parts of most concern to these patients.
METHODS
After ethical review committee approval was obtained, we enrolled 18 males and 27 females admitted for inpatient hospitalization who agreed to participate in the study. Participants were aged 8-18 years, were able to be interviewed, understood the wording of the questionnaires, and had no thought disorder. All patients met DSM-5 criteria for BDD. The study was conducted from January 17, 2014, to September 29, 2014.
Assessments
Study participants were asked to complete the Body Dysmorphic Disorder Questionnaire (child and adolescent version)6 and the Body Dysmorphic Disorder Diagnostic Module.6 Patients who screened positive for BDD were then given a questionnaire to address the age at onset of symptoms, coping strategies, history of sexual abuse, and the amount of time spent thinking about their perceived defects. The questionnaire also screened for the area of the body that the participants were most preoccupied with in addition to the specific coping strategy used. The criteria for BDD, which includes appearance concerns unobservable to others, performance of repetitive behaviors, comparison of appearance with others in response to appearance concerns, and significant distress or impairment in social functions due to the preoccupation, were based on the DSM-5.7

- Patients with body dysmorphic disorder (BDD) are obsessed with perceived body defects and have associated difficulty in social functioning.
- Patients with BDD are most preoccupied with exposed facial body parts such as skin, lips, nose, teeth, ears, and eyes and gender-specific body parts with a sexual connotation such as breasts in women and the penis in men.
- These data will help clinicians better understand these patients and assist in their management.
RESULTS
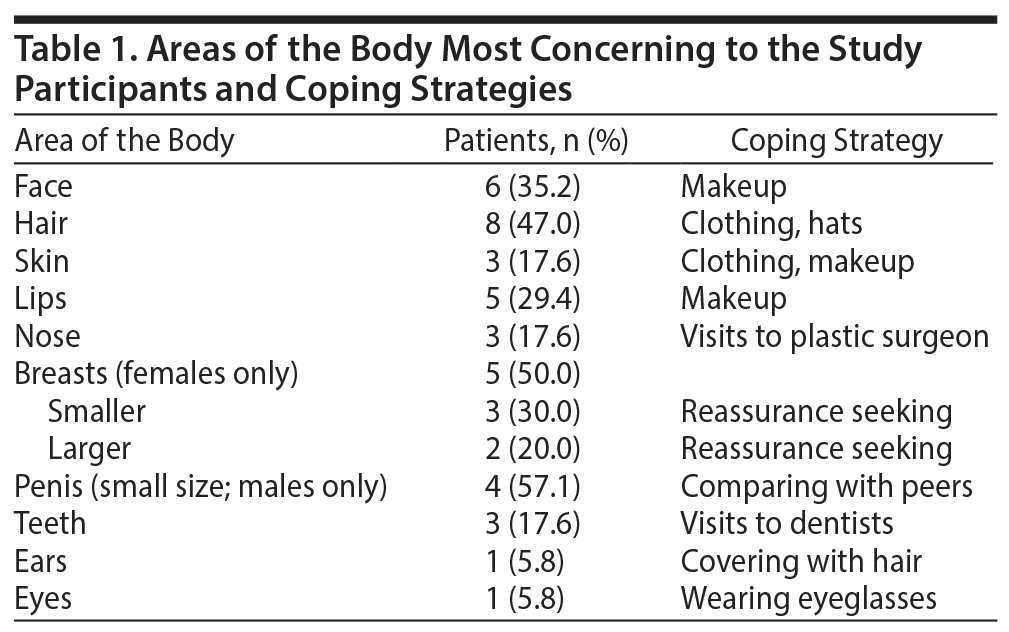
Seventeen patients (10 females and 7 males) had BDD. The mean age at onset of BDD was 10.5 years, and the time spent thinking about the imagined defect averaged 3.5 hours per day. In terms of the body parts of most concern, 6 (35.2%) reported face (coping strategy: makeup), 8 (47.0%) reported hair (coping strategy: hats), 3 (17.6%) reported skin (coping strategy: clothing and makeup), 5 (29.4%) reported lips (coping strategy: makeup), 3 (17.6%) reported nose (coping strategy: visit to plastic surgeon), 3 (17.6%) reported teeth (coping strategy: visits to the dentist), 1 (5.8%) reported ears (coping strategy: covering with hair), and 1 (5.8%) reported eyes (coping strategy: eyeglasses) (Table 1).
With regard to gender-specific body parts, female participants were most concerned with breasts (n = 5, 50%) and utilized reassurance as a coping strategy. Three (30%) had perceived smaller breasts and 2 (20%) had perceived larger breasts. Male participants reported perceived smaller penis as most concerning (n = 4, 57.1%) and utilized comparison with peers as a coping strategy.
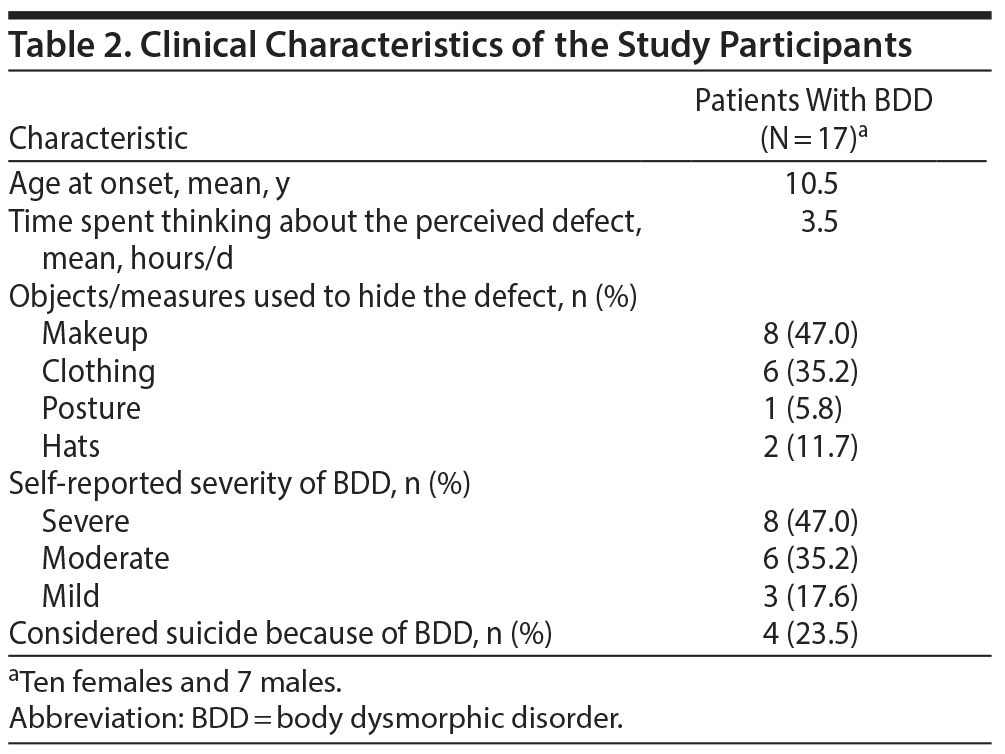
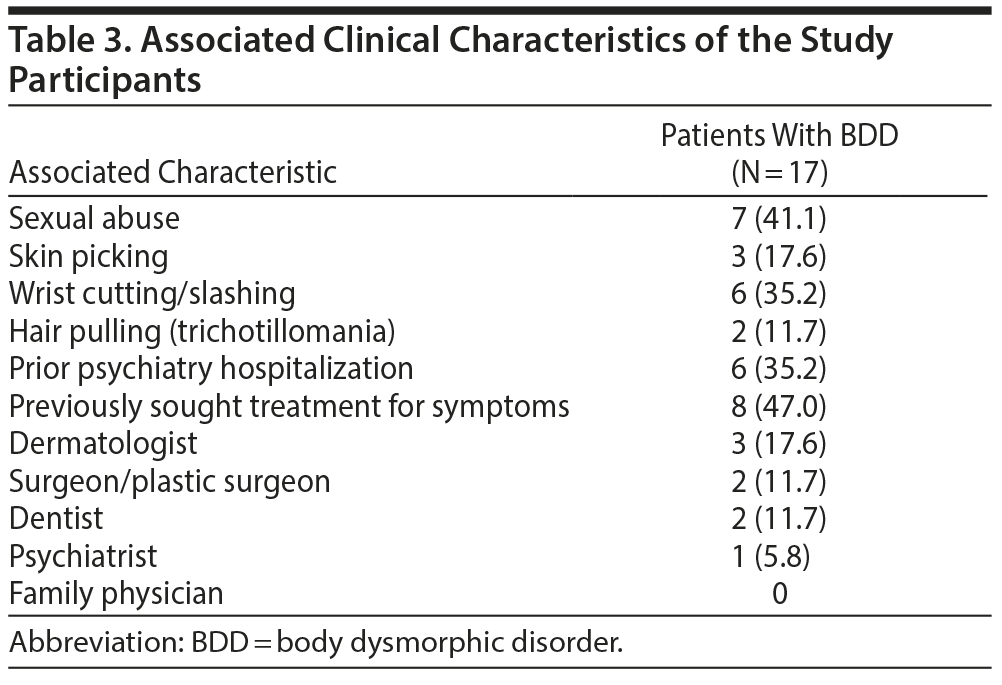
Patients reported hiding the perceived defects with makeup: 8 (47.0%), clothing: 6 (35.2%), posture: 1 (5.8%), and hats: 2 (11.7%) (Table 2). Eight patients (47.0%) rated their BDD as severe, 6 (35.2%) as moderate, and 3 (17.6%) as mild, while 4 (23.5%) considered suicide because of BDD (see Table 2). Seven (41.1%) reported sexual abuse, 3 (17.6%) skin picking, 6 (35.2%) wrist cutting, and 2 (11.7%) trichotillomania. Six (35.2%) had a prior psychiatric hospitalization, and 8 (47.0%) had sought treatment with other providers. Of the patients, 3 (17.6%) had seen a dermatologist, 2 (11.7%) had seen a surgeon or plastic surgeon, 2 (11.7%) had seen a dentist, and 1 (5.8%) had seen psychiatrists for their perceived defect, while none reported seeing a family physician (Table 3).
DISCUSSION
The study was designed to determine which body parts most concern adolescent BDD patients. The study revealed that among both sexes the most concerning body parts were hair (47.0%), face (35.2%), and lips (29.4%), while gender-specific parts included breasts (50.0% in all females) and penis (57.1% in all males). Other commonly affected parts were nose, teeth, and ears. These findings are similar to other reports8 that suggested that body regions involved in BDD include hair, breasts, and genitalia, with a variant in males that includes the desire to have increased muscle mass. Most patients with BDD classified their BDD as a severe problem (47%), 35.2% rated it as moderate, and only 17.6% rated it as mild, which underscores the importance of diagnosis.9 Only a very small percentage of the BDD patient population sought help from a psychiatrist (5.8%). Other specialties contacted for help with this matter were dermatologists, surgeons, and dentists. Surprisingly, none of the patients in the BDD group contacted a family physician for help. Previous studies10 also showed that a majority of patients present to a surgeon or specifically to a plastic surgeon.
Limitations include that this study was conducted among patients recruited within an inpatient setting and that the data presented are mostly self-reported, thus making the generalizability of our results within the general population uncertain.
This study shows that BDD can occur among patients admitted to an inpatient psychiatric hospital. BDD patients’ preoccupation is more with exposed facial body parts such as skin, lips, nose, teeth, ears, and eyes and body parts with historical sexual connotation such as breasts in women and the penis in men.
Submitted: April 27, 2017; accepted July 28, 2017.
Published online: October 26, 2017.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. Sadock BJ, Sadock VA, Ruiz P. Kaplan and Sadock’s Synopsis of Psychiatry: Behavioral sciences/Clinical Psychiatry. Philadelphia, PA: Lippincott Williams & Wilkins (LWW), Wolter Kluwer Health,2015;11.
2. Phillips KA, Menard W, Fay C, et al. Demographic characteristics, phenomenology, comorbidity, and family history in 200 individuals with body dysmorphic disorder. Psychosomatics. 2005;46(4):317-325. PubMed CrossRef
3. Phillips KA, McElroy SL, Keck PE, et al. Body dysmorphic disorder: 30 cases of imagined ugliness. Am J Psychiatry. 1993;150(2):302-308. PubMed CrossRef
4. Chosak A, Marques L, Greenberg JL, et al. Body dysmorphic disorder and obsessive-compulsive disorder: similarities, differences and the classification debate. Expert Rev Neurother. 2008;8(8):1209-1218. PubMed CrossRef
5. Phillips KA. Body dysmorphic disorder. In: Hudak R, Dougherty DD, eds. Clinical Obsessive-Compulsive Disorders in Adults and Children. New York, NY: Cambridge University Press; 2011.
6. Danesh M, Beroukhim K, Nguyen C. et al. Body dysmorphic screening tools for the dermatologist: a systematic review. Practical Dermatol. 2015; 3:44-49.
7. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
8. Conrado LA, Hounie AG, Diniz JB, et al. Body dysmorphic disorder among dermatologic patients: prevalence and clinical features. J Am Acad Dermatol. 2010;63(2):235-243. PubMed CrossRef
9. Belli H, Belli S, Ural C, et al. Psychopathology and psychiatric co-morbidities in patients seeking rhinoplasty for cosmetic reasons. West Indian Med J. 2013;62(5):481-486. PubMed
10. Phillips KA, Coles ME, Menard W, et al. Suicidal ideation and suicide attempts in body dysmorphic disorder. J Clin Psychiatry. 2005;66(6):717-725. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!