Objective: After the earthquakes that occurred in Lorca, Spain, on May 11, 2011, the regional mental health management employed 2 clinical psychologists for 6 months to provide care to people referred by primary care physicians. The objective was to address the expected increased demand for treatment of mental disorders, notably posttraumatic stress disorder (PTSD) and adjustment disorders.
Method: Referred individuals were evaluated and treated according to a clinical protocol designed ad hoc from June 12, 2011, to November 30, 2011. The protocol provided a stepped intervention guided by clinical and psychometric assessment using “normalization” for those with no psychiatric diagnosis, brief group treatment for mild to moderate PTSD or adjustment disorders, individual treatment for more severe PTSD, and referral to the local mental health center for other mental health disorders. Standard adult and child scales to assess posttraumatic, depression, and anxiety symptoms and resilience were used at initial assessment to guide treatment allocation and repeated to assess outcome status. Psychologists also provided a clinical assessment of symptom resolution at the end of the study.
Results: Rates of symptom resolution and improvements on all scales (PTSD, depression, anxiety, and resilience) demonstrated clinically and statistically significant improvement in all treatment groups (P = .000). Dropout was low. Medications were prescribed frequently to adults; no child received medication as a result of the earthquakes. No case of mental disorder related to the earthquakes was referred to the local mental health center during the 6 months of psychologist intervention.
Conclusion:The structured intervention resulted in a high resolution of cases and low dropout, allowing treatment of a larger number of people with optimal frequency (weekly), devoting more time to the most severe cases and less to those moderately or mildly affected.
Psychological Intervention in Primary Care
After Earthquakes in Lorca, Spain
ABSTRACT
Objective: After the earthquakes that occurred in Lorca, Spain, on May 11, 2011, the regional mental health management employed 2 clinical psychologists for 6 months to provide care to people referred by primary care physicians. The objective was to address the expected increased demand for treatment of mental disorders, notably posttraumatic stress disorder (PTSD) and adjustment disorders.
Method: Referred individuals were evaluated and treated according to a clinical protocol designed ad hoc from June 12, 2011, to November 30, 2011. The protocol provided a stepped intervention guided by clinical and psychometric assessment using “normalization” for those with no psychiatric diagnosis, brief group treatment for mild to moderate PTSD or adjustment disorders, individual treatment for more severe PTSD, and referral to the local mental health center for other mental health disorders. Standard adult and child scales to assess posttraumatic, depression, and anxiety symptoms and resilience were used at initial assessment to guide treatment allocation and repeated to assess outcome status. Psychologists also provided a clinical assessment of symptom resolution at the end of the study.
Results: Rates of symptom resolution and improvements on all scales (PTSD, depression, anxiety, and resilience) demonstrated clinically and statistically significant improvement in all treatment groups (P = .000). Dropout was low. Medications were prescribed frequently to adults; no child received medication as a result of the earthquakes. No case of mental disorder related to the earthquakes was referred to the local mental health center during the 6 months of psychologist intervention.
Conclusion:The structured intervention resulted in a high resolution of cases and low dropout, allowing treatment of a larger number of people with optimal frequency (weekly), devoting more time to the most severe cases and less to those moderately or mildly affected.
Prim Care Companion CNS Disord 2015;17(1):doi:10.4088/PCC.14m01691
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: June 14, 2014; accepted September 25, 2014.
Published online: February 26, 2015.
Corresponding author: Servicio Murciano de Salud, Mental Health Subdirection Hospital Psiquiátrico Roman Alberca Lorca s/nEl Palmar, Murcia 30120 Spain ([email protected]).
Natural disasters increase the demand for mental health services.1–3 Posttraumatic stress disorder (PTSD) is the most prevalent mental disorder resulting from natural disasters such as earthquakes, hurricanes, and floods according to most reviews.3,4 Prevalence of PTSD varies from 5% to 60% in the first and second year after a disaster, with most studies reporting prevalence < 30%.5
The loss of the house where one lived, the death of family members, the threat to life, injury, and behavior during the disaster are considered “psychological toxins,” the effect of which are greater the closer the proximity to the event.3 The worst outcomes occur in communities with high levels of destruction and the highest number of casualties. However, natural disasters produce fewer mental health problems than disasters caused by man, and such consequences are usually fewer in developed countries than in developing ones.3,6 According to prior studies, individuals most at risk of developing mental disorders following an earthquake are women, older persons, those with low educational levels, and those with higher levels of exposure to the earthquake’s effects.7,8
There are many descriptive studies on the impact of natural disasters on the affected populations at different points in time (eg, 1 month, 6 months, a year), but there are fewer articles on the effectiveness of structured intervention procedures, especially during the first months after a natural disaster.9 Three clinical trials of brief cognitive-behavioral therapy (CBT) after earthquakes in Turkey and China were carried out 13 months and 2 years after those disasters and therefore addressed chronic or delayed disorders.10 A clinical trial with accident survivors who developed PTSD in the initial months following the events demonstrated that CBT is superior to either repeated measures (a clinician explained in a 20-minute session that symptoms may decline with time and that it was unknown if immediate or delayed treatment was more effective) or a self-help book.11 Treatment with CBT was also demonstrated to be superior to placement on a waiting list in a second trial with terrorism victims.12 Finally, Shooshtary and colleagues13 showed the superiority of brief CBT over waiting list control conditions in the treatment of adolescents (11 to 20 years old) 4 months after an earthquake in Bam, Iran.
Our objective was to evaluate a psychological intervention conducted after the earthquakes in Lorca, Spain, using a protocol designed to integrate 2 clinical psychologists into primary care practices. These professionals worked in 3 health care centers in Lorca and intervened with patients referred by general practitioners also located at the centers. One psychologist worked full time in “La Viña” health care center (the most affected by the earthquakes) and the other divided her time between “San Diego” and “Lorca Centro.” The aim was to provide care to as many people as soon as possible, avoiding the expected excess of demand on the mental health center in Lorca. This is the first experience of total integration of clinical psychologists in health care centers in the region of Murcia, except for the training of residents in clinical psychology.14,15
Lorca is a city in the autonomous community of Murcia in southeastern Spain and has 85,000 inhabitants. On May 11, 2011, Lorca experienced 2 earthquakes during a brief interval that caused significant localized damage and panic among inhabitants and displaced many from their homes. Three people were killed by falling cornice. A total of 9 earthquake-related deaths were confirmed, while approximately 300 were injured. Over 1,000 homes were demolished, and 80% of buildings were damaged. A field hospital was set up by the regional civil defense unit to provide care to the wounded and displaced. Besides medical care, volunteer psychologists provided counseling for early intervention. In this field hospital, 5,000 people sought shelter. Little by little, people returned to their homes if they were livable or moved to relatives’ homes.
The mental health center in Lorca treated 27 people affected during the first month after the earthquake, 16 of them were former patients of the center.16,17 Given the expected increase in demand, mental health management employed 2 clinical psychologists to provide care to patients referred by family physicians. This model is known as the “replacement model” (the primary care physician refers the patient to the psychologist, who assumes responsibility for providing a distinct treatment).18 The aim is to assess the degree of impairment and provide brief treatment for mild to moderate cases, allowing the mental health center to treat severe cases. A specific protocol for evaluation and treatment was developed.
A semistructured interview was developed to assist in determining the degree of impact of the traumatic event depending on a number of variables including direct relationship with fatalities, injuries, and loss of home, business, or both. Diagnostic evaluation was complemented by the use of scales to measure the severity of PTSD, depression, and anxiety and resilience in children and adults.14
For the treatment of PTSD, the relevant Cochrane meta-analysis19 and several high-quality clinical practice guidelines20,21 recommend using a trauma-focused psychotherapy (level of evidence A). Therefore, we adapted Foa and Rothbaum’s22 PTSD treatment protocol for individuals for use with groups. We also recommended brief CBT for anxiety and depressive adjustment disorders.
Our objective was to manage the increasing demand for treatment of mental disorders by using available resources as efficiently as possible, while applying evidence-based treatment for those requiring it.
METHOD
One month after the earthquakes (June 11–14, 2011), the assessment and treatment protocol was presented to primary care physicians working at the health centers, including criteria for referral to the psychologists: people with depressive or anxiety disorders directly related to the earthquake experience. Severe mental disorders (eg, schizophrenia) or reactivated prior mental disorders would be referred to the local mental health center as usual. Family physicians were able to discuss cases directly with the clinical psychologists located at the community health centers and receive continuous feedback from them.
Patients referred by family physicians were interviewed by the clinical psychologists using the semistructured interview. During the first session, the patients (adults or children) completed age-appropriate scales. For adults, these measures were as follows:
- Davidson Trauma Scale23 (DTS), Spanish validated version.24 Designed to assess the frequency and severity of symptoms of PTSD, ranging from 0 to 136 points. A score of 40 was used as the cutoff to indicate that further evaluation for PTSD was needed.
- State/Trait Anxiety Inventory (STAI).25 Designed to assess the current level of anxiety, as well as the willingness to respond to stress.
- Beck Depression Inventory (BDI).26 Designed to classify the intensity of depression in adolescents and adults: low (0–9), mild (10–16), moderate (17–30), and high (> 30).
- Resilience Scale, Spanish version27 (total score ranges from 25 to 175). Values > 146 indicate increased resilience, values between 121 and 146 indicate moderate resilience, and values < 121 indicate low resilience.
For children, these measures were as follows:
- Screen for Child Anxiety Related Emotional Disorders–Revised.28 Cutoff of 42 indicates that further evaluation for PTSD is needed.
- State/Trait Anxiety Inventory for Children.29
- Children’s Depression Inventory. Designed to classify the intensity of depression in children: no depression (0–6), mild (7–12), moderate (13–18), and high (> 18).30
- Escala de Resiliencia Escolar.31 School Resilience Scale for children between ages 9 and 14 years.
With the information obtained from the interview and the scores of the scales, the diagnosis and the severity of symptoms were determined, and patients were assigned to 1 of the following intervention groups:
- Normalization: For those with mild reactions that did not quite constitute a disorder; psychologist intervention to help patients normalize their situations and view symptoms as a normal reaction to a traumatic event that are most likely to disappear with time. A follow-up appointment was made in a month, if necessary.
- Brief group treatment: For mild to moderate disorders (eg, partial PTSD or adjustment disorder with anxiety or depressed mood). The aim was to provide brief therapy involving 5 sessions at an optimal frequency (weekly).
- Individual treatment: In the case of PTSD or severe adjustment disorders, a brief individual intervention of longer duration (up to 10 sessions) adapted to the patient needs was offered.
- Referral to the mental health center for prior mental disorder, reactivated after the experience of the earthquake, or any severe mental disorder.
Some patients, because of illiteracy or lack of time, did not complete any scale (11.7%). In such cases, the psychologists made treatment group allocation decisions on the basis of their clinical assessment alone. At the end of individual or group therapy, the same scales were applied, and the clinical psychologist determined resolution (yes/no), defined as the disappearance of the symptoms that led to consultation.
Analysis
To assess whether there was a statistically significant difference between the patients’ mean prescore and postscore, we used t tests for paired samples. To control medication, we wrote down the dosages prescribed by primary care physicians before referring the patient (pre) and at the end of psychological treatment (post), obtaining the percentage of patients with higher, lower, or equal dose.
In those assigned to the treatment group, 32 (19.8%) did not complete the scales at the end of treatment. We performed an intention-to-treat analysis carrying forward baseline scores for those with no outcome scale data, and the results (not shown) were also statistically significant (P = .000).
RESULTS
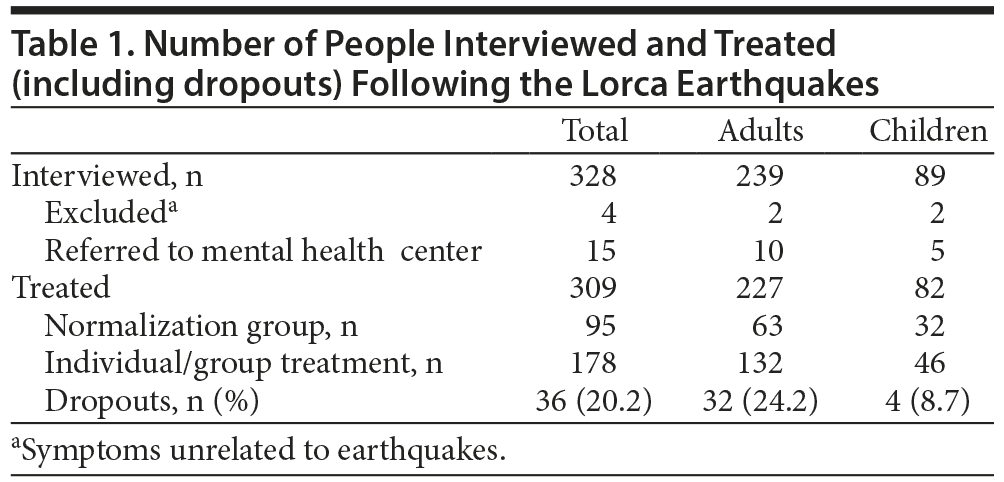
From June 12, 2011, to November 30 2011, 328 people, 239 of them adults (73%), were referred from the family physicians to the clinical psychologists. Only 4 people presented symptoms unrelated to the earthquake, and they were excluded from the study. Due to the severity of symptoms, 15 individuals were referred to the mental health center (4.6%). Therefore, 227 adults and 82 children began treatment. Sixty-three adults (27.8%) and 32 children (39%) were assigned to the normalization intervention. They were discharged after the first session (Table 1). All treatments were completed by February 2012.
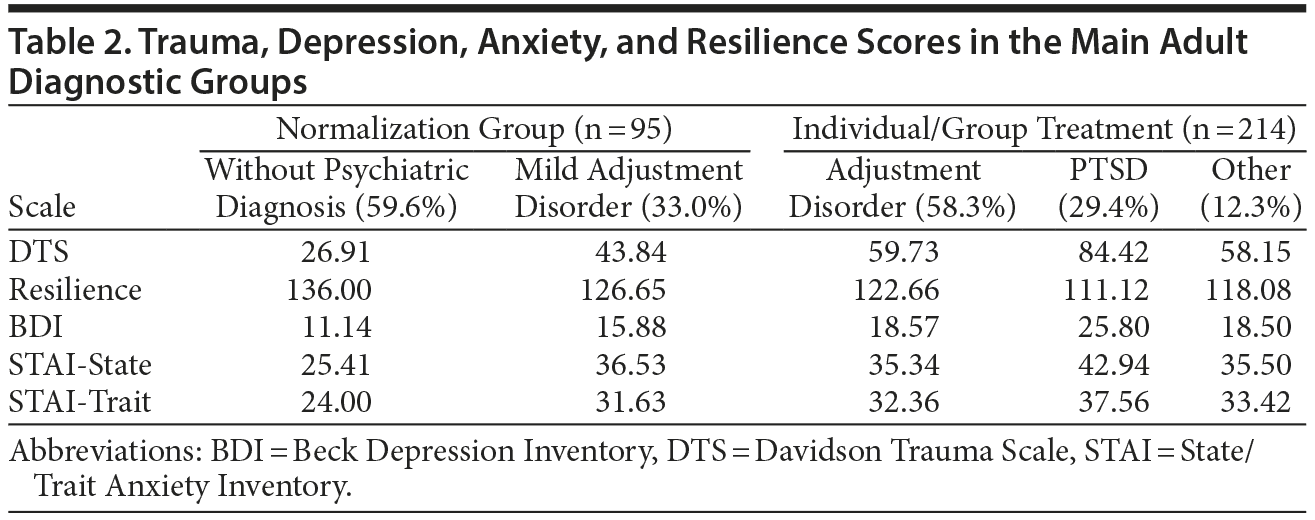
As previously reported,14 the profile of the adult patient was female (85.8%), Spanish (95.5%), married (67.7%) with a family of his/her own (73.2%), and basic education (elementary school: from 6 to 12 years old) (36.5%), illiterate/uneducated (25.1%), or high school education (23.3%). Regarding diagnosis, there was a clear difference between the normalization group (most without psychiatric diagnosis or mild adjustment disorder) and the treated groups (characterized by moderate to severe adjustment disorder and PTSD). Other anxiety and depressive disorders did not exceed 12.3% (Table 2).
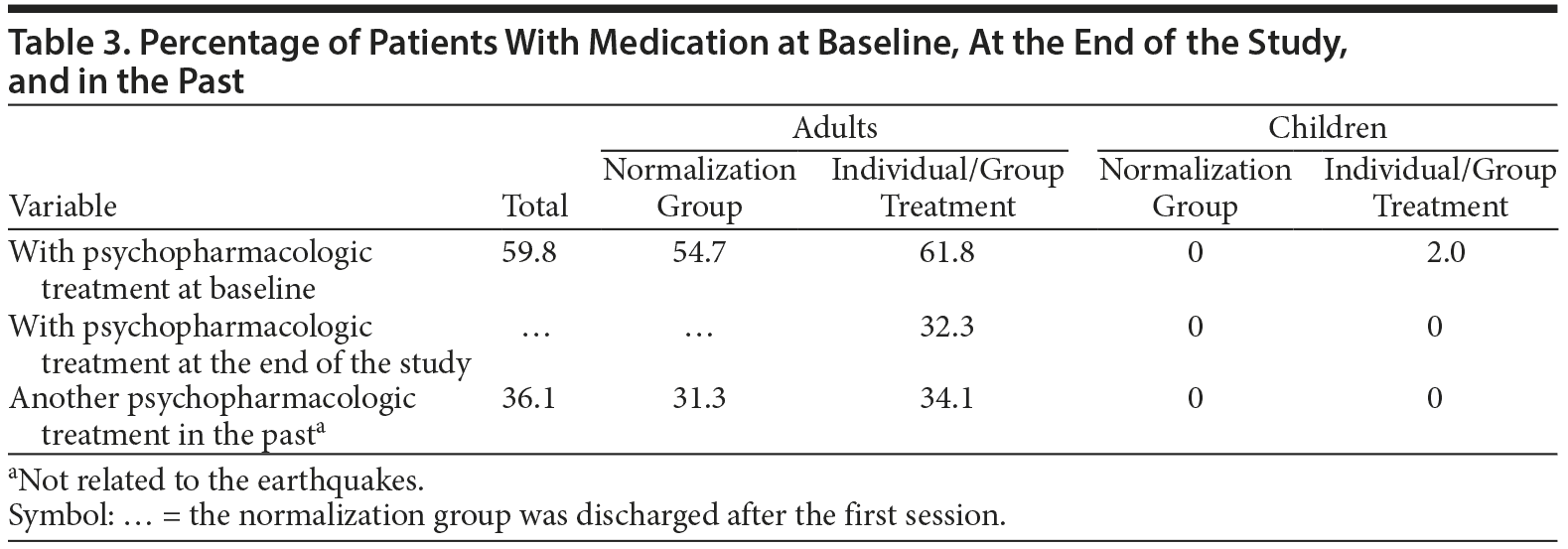
The proportion of treated patients taking medication at the beginning of the study was 61.8% and decreased to 32.3% by the end of the study (Table 3). In addition, 28 of the 43 patients in the treatment group taking medication at the end of the intervention decreased the dose (65%), 13 kept the same dose (27%), and 2 increased the dose (8%). There was a clear difference between children and adults in the use of medication as a result of the earthquakes: only 1 child was taking medication (not related to earthquakes). Even among the normalization group, 54.7% of adults were taking medication prescribed by their primary care physicians, but most had no psychiatric diagnosis (Table 3).
Clinical Scale Scores
The mean scores on the baseline DTS, Resilience Scale, BDI, STAI-State, and STAI-Trait were significantly higher in the treated group (individual and group therapy) than in the normalization group (P = .000, P = .001, P = .000, P = .000, P = .001, respectively). DTS score (baseline) was used as a criterion of severity to determine assignment between groups (Tables 4 and 5).
Patients who did not complete any scale (11.7%) because of illiteracy or lack of time were given the option of not returning for follow-up if they were improved; 32% of this group did not return after a month.
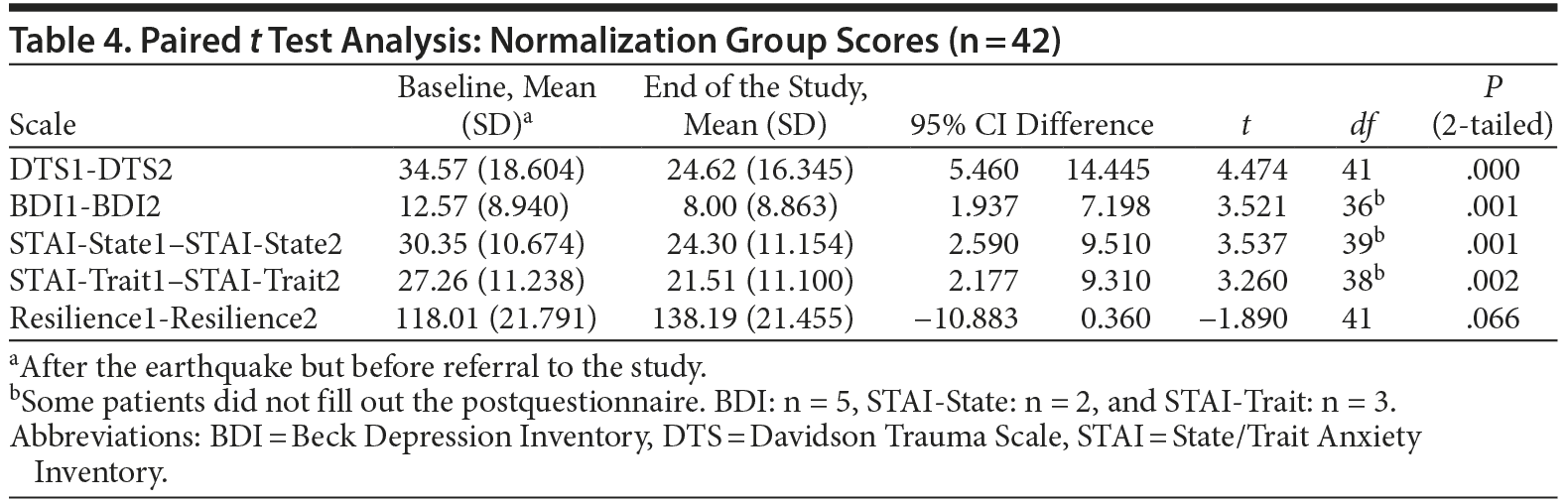
Normalization group (1 single session and optional 1-month follow-up). Among those who made a return visit, 60% had resolved the symptoms that motivated the initial consultation. Among those who came back to the 1-month follow-up, most improved further: there was a significant decrease in scores on the clinical scales. Resilience was increased (going from low to moderate), although the change was not statistically significant (Table 4).
Forty-two patients (44.2%) returned for a 1-month follow-up visit. Twenty of those patients were taking medication prescribed at the initial visit (47.6%), of whom 45% maintained the initially prescribed dose and 55% had decreased their dose; 52.4% were not taking medication. In only 2 cases were the initial symptoms unresolved (3.1%).
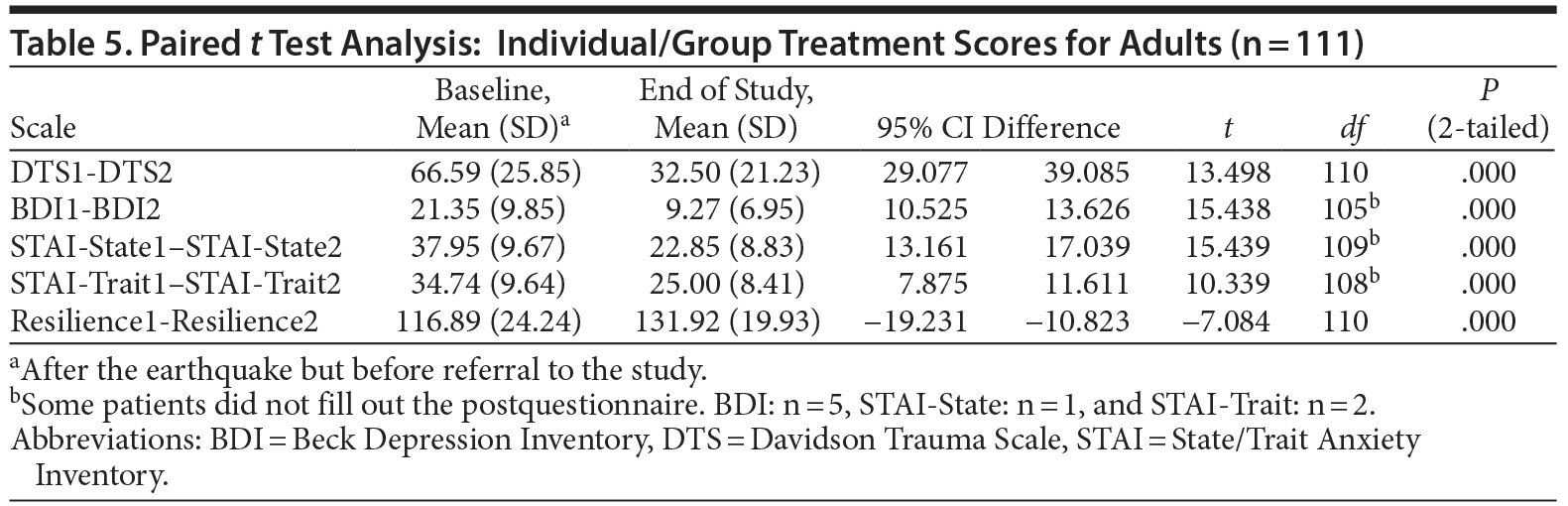
Treatment group. Patients included 111 adults and 41 children who were treated individually or in groups (Tables 5 and 6). Thirty-two people (19.8%) did not complete the scales at the end of treatment and are not included in the outcome assessment data. After treatment, the mean DTS score was below the cutoff point (40). The depression scores decreased from moderate to low. Initial STAI-Trait percentiles were high at 80% (males) and 81% (females) and decreased to 55% (males) and 57% (females); and initial STAI-State percentiles were 94% (males) and 89% (females) and decreased to 50% (males) and 48% (females). Conversely, preresilience scores were low, and postresilience scores were moderate (Table 5).
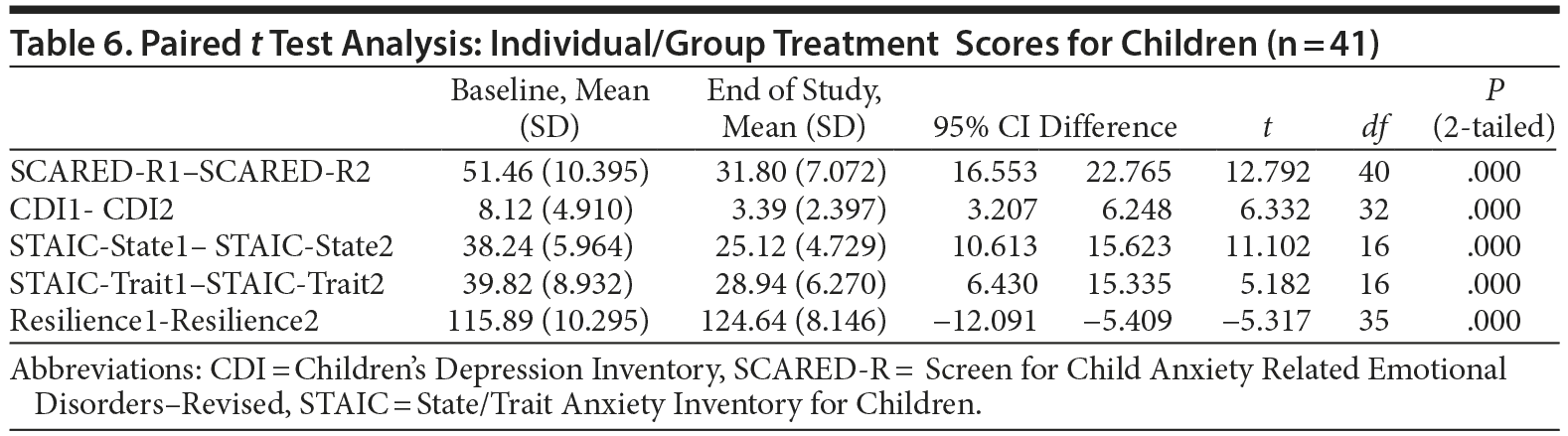
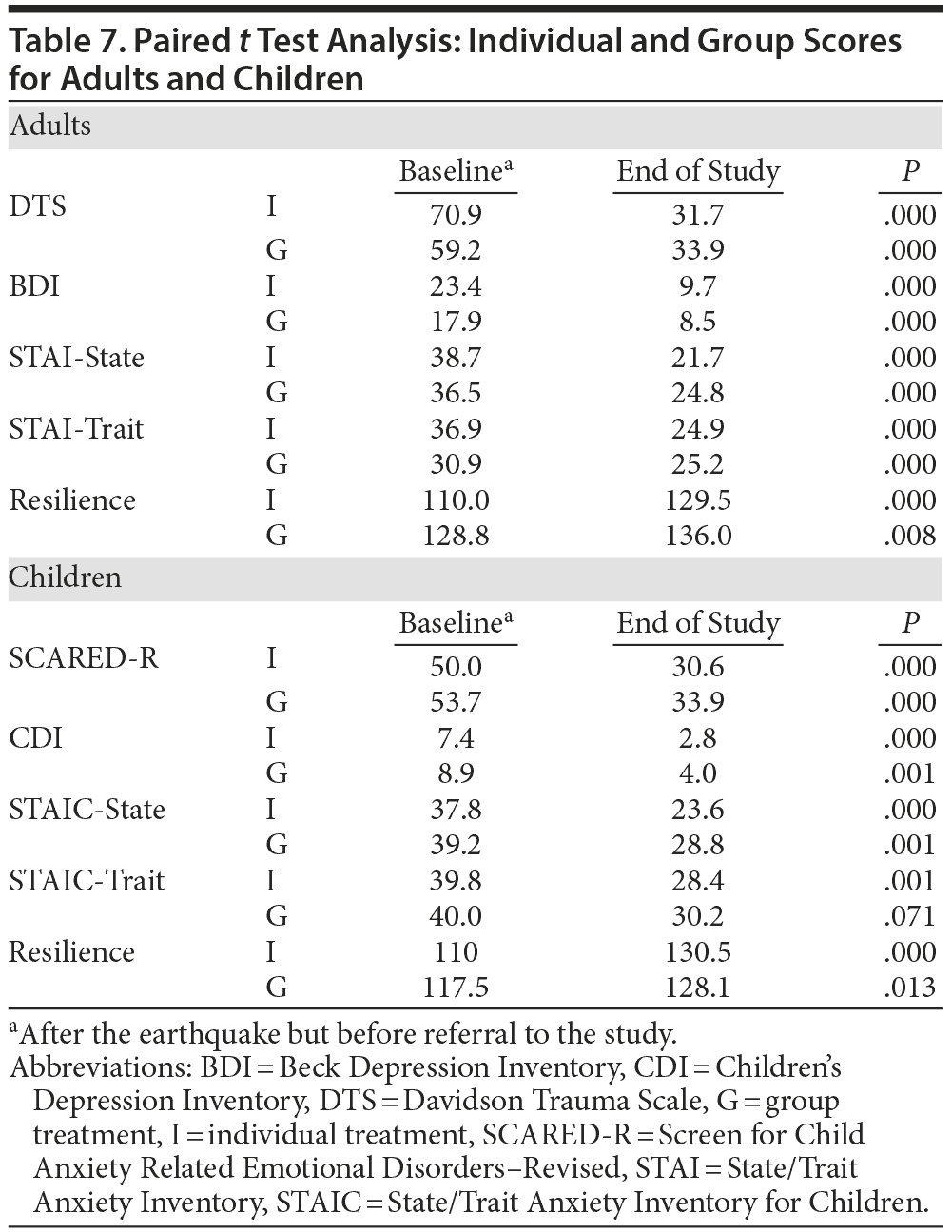
The baseline scores of adults in individual treatment are higher than those in group treatment. The postscores are similar. All differences are statistically significant (all P = .000, except for resilience in group treatment, which was P = .008). In children, the baseline scores are similar, but higher for those in group therapy (Table 7).
DISCUSSION
Our experience demonstrates that, after a natural disaster with a low number of deaths and injuries, it is feasible to provide a rapid and effective response using available personnel and a protocol of assessment and stepped intervention. By integrating personnel capable of providing psychological therapies in primary care practices, we increased access and made efficient use of resources, providing the minimum necessary care, based on clinical assessment and precise diagnosis. The mental health center in Lorca treated 27 patients affected by the earthquakes during the first month, compared to 170 treated at 3 health care centers during the following 45 days. No patient was referred to the mental health center in Lorca for reasons related to the earthquake between June and November 2011.
The strategy for allocation of patients to normalization or treatment groups seems to have been adequate, as indicated by the difference in diagnoses between both groups, the similarities between the prescores of the normalization and the postscores in the treatment group, and the small number of unresolved cases in the normalization group at 1-month follow-up (3.1%). As shown in Table 2, trauma, depression, and anxiety scores increased as diagnostic severity increased. Conversely, resilience scores decreased as diagnostic severity increased, from 136 (“without psychiatric diagnosis”) to 111 (PTSD).
The normalization intervention produced the desired effect by providing an explanation for symptoms and providing a course of improvement that was fulfilled later. This outcome does, in our view, reinforce our judgment of the appropriateness of the intervention itself.
In the treated group, the treatment proposed here significantly reduced trauma, depression, and anxiety scores. Conversely, mean preresilience scores were low and postresilience scores were moderate (Table 5). Individual and group treatments were effective. In adults, baseline scores were higher for patients in individual therapy (Table 7). This finding means that individual treatment was preferred for the most severe disorders. In children, more and less severe cases were mixed in group treatment in order to attain a better expression of fear and other emotions. However, in this case, the treatment protocol was not applied exactly.
Dropout was low in adults (24.2%) and children (8.7%) when compared to the figure of 50% cited by some reviews19,32 or the 60% dropout rate from psychotherapy after hurricane Katrina (up to 89% among those with neither serious nor mild to moderate mental illness).2 Two-thirds of the patients who dropped out did so after the first session, and up to 90% did so after the second session. Therefore, the normalization intervention resolved a large portion of cases and permitted us to dedicate more attention to the most affected patients, thus making efficient use of the available resources.
Unlike other studies,11,13 in the present study, there was no patient selection: all of the cases referred by family physicians were treated under conditions that match usual clinical practice. Our results demonstrate how we structured the intervention, which allowed for treatment of a large number of people of different ages in record time.
Finally, there was a clear difference in the use of psychotropic drugs for children and adults in primary care. Despite the guideline recommendations, psychotropic drugs were used in adults frequently, even among patients with no psychiatric diagnosis or mild adjustment disorders.
One limitation of the study is the lack of a control group, which prevents assessment of how much of the improvement was due to the application of drug therapy or the passage of time. In the case of children, pediatricians referred patients without medication, and similar results were obtained in terms of decreased scores on the clinical scales, using the same evaluation and treatment protocol. On the other hand, some longitudinal research of natural disasters has documented a decline of PTSD prevalence over time, but other studies showed an increase of prevalence.33 Anxiety and depression symptoms after natural disasters tend to decrease over time. However, PTSD can increase in the months following trauma.34 People in the Bam earthquake control group (waiting list) did not improve after 4 weeks.13 Those data support our view of normalization for mild symptoms and treatment of moderate to severe disorders.
Author affiliations: Mental Health Branch of Murcia Health Service, El Palmar (Mssrs Martin and Garriga) and La Viña Health Centre, Lorca (Ms Egea), Murcia, Spain.
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Rodriguez JJ, Kohn R. Use of mental health services among disaster survivors. Curr Opin Psychiatry. 2008;21(4):370–378. doi:10.1097/YCO.0b013e328304d984 PubMed
2. Wang PS, Gruber MJ, Powers RE, et al. Mental health service use among hurricane Katrina survivors in the eight months after the disaster. Psychiatr Serv. 2007;58(11):1403–1411. doi:10.1176/appi.ps.58.11.1403 PubMed
3. Davidson JRT, McFarlane AC. The extent and impact of mental health problems after disaster. J Clin Psychiatry. 2006;67(suppl 2):9–14. PubMed
4. Foa EB, Stein DJ, McFarlane AC. Symptomatology and psychopathology
of mental health problems after disaster. J Clin Psychiatry. 2006;67
(suppl 2):15–25. PubMed
5. Galea S, Nandi A, Vlahov D. The epidemiology of posttraumatic stress disorder after disasters. Epidemiol Rev. 2005;27(1):78–91. doi:10.1093/epirev/mxi003 PubMed
6. Norris FH, Friedman MJ, Watson PJ, et al. 60,000 disaster victims speak, part 1: an empirical review of the empirical literature, 1981–2001. Psychiatry. 2002;65(3):207–239. PubMed
7. Zhang Y, Ho SMY. Risk factors of posttraumatic stress disorder among survivors after the 512 Wenchuan earthquake in China. PLoS ONE. 2011;6(7):e22371. doi:10.1371/journal.pone.0022371 PubMed
8. Xu J, Wu Z. One-year follow-up analysis of cognitive and psychological consequences among survivors of the Wenchuan earthquake. Int J Psychol. 2011;46(2):144–152. doi:10.1080/00207594.2010.529908 PubMed
9. Hamblen JL, Norris FH, Pietruszkiewicz S, et al. Cognitive-behavioral therapy for postdisaster distress: a community-based treatment program for survivors of hurricane Katrina. Adm Policy Ment Health. 2009;36(3):206–214. doi:10.1007/s10488-009-0213-3 PubMed
10. Başoğlu M, Livanou M, Salcioğlu E, et al. A brief behavioral treatment of chronic posttraumatic stress disorder in earthquake survivors: results from an open clinical trial. Psychol Med. 2003;33(4):647–654. doi:10.1017/S0033291703007360 PubMed
11. Ehlers A, Clark DM, Hackmann A, et al. A randomized controlled trial of cognitive therapy, a self-help booklet, and repeated assessments as early interventions for posttraumatic stress disorder. Arch Gen Psychiatry. 2003;60(10):1024–1032. doi:10.1001/archpsyc.60.10.1024 PubMed
12. Duffy M, Gillespie K, Clark DM. Posttraumatic stress disorder in the context of terrorism and other civil conflict in northern Ireland: randomised controlled trial. BMJ. 2007;334(7604):1147. doi:10.1136/bmj.39021.846852.BE PubMed
13. Shooshtary MH, Panaghi L, Moghadam JA. Outcome of cognitive-behavioral therapy in adolescents after natural disaster. J Adolesc Health. 2008;42(5):466–472. doi:10.1016/j.jadohealth.2007.09.011 PubMed
14. Martín JC, Garriga A, Egea C, et al. Psychological intervention for survivors of the Lorca earthquakes: an experience of integration in primary care. Proceedings of the Thematic Conference “Mental Health and Family Medicine Working Together.” February 9–11, 2012; Grenada, Spain.
15. Esquitino M, Jesús MG-S, César J, et al. Ascensión. Tratamiento cognitivo conductual grupal de Trastorno de pánico en Atención primaria: una experiencia piloto. Psiquiatria.com. 2011;15(77). http://www.psiquiatria.com/
revistas/index.php/psiquiatriacom/article/view/1367/1243/. Accessed July 25, 2012.
16. García-Sancho JCM. Intervención psicológica en salud mental tras un seísmo: la experiencia de Lorca. Libro de resúmenes de los trabajos aceptados en el V congreso internacional y X nacional de psicología clínica. Asociación Española de Psicología Conductual (AEPC). Granada, Spain; 2012; 136–140.
17. Valera J, Albacete A, Sánchez A, et al. Intervención psicológica grupal en un centro de salud mental con afectados por los seísmos de Lorca (Murcia). Libro de capítulos del V Congreso Internacional y X Nacional de Psicología Clínica. Asociación Española de Psicología Conductual (AEPC). Granada; 2012: 947–950.
18. Bower P, Gilbody S. Managing common mental health disorders in primary care: conceptual models and evidence base. BMJ. 2005;330(7495):839–842. doi:10.1136/bmj.330.7495.839 PubMed
19. Bisson J, Andrew M. Psychological treatment of posttraumatic stress disorder (PTSD). Cochrane Database Syst Rev.2005;(2):CD003388. PubMed
20. National Collaborating Centre for Mental Health (Grande-Bretagne), National Institute for Clinical Excellence. (Grande-Bretagne). Posttraumatic Stress Disorder : the Management of PTSD in Adults and Children in Primary and Secondary Care. London, UK: Published by Gaskell and the British Psychological Society; 2005.
21. Australia. National Health and Medical Research Council. Australian Guidelines for the Treatment of Adults With Acute Stress Disorder and Posttraumatic Stress Disorder. Melbourne, Australia: Australian Centre for Posttraumatic Mental Health; 2007.
22. Foa EB, Rothbaum BO. Treating the Trauma of Rape: Cognitive-Behavioral Therapy for PTSD. New York, NY: Guilford; 1998.
23. Davidson JRT, Tharwani HM, Connor KM. Davidson Trauma Scale (DTS): normative scores in the general population and effect sizes in placebo-controlled SSRI trials. Depress Anxiety. 2002;15(2):75–78. doi:10.1002/da.10021 PubMed
24. Bobes J, Calcedo-Barba A, García M, et al; Grupo Espanol de Trabajo para el Estudio del Trastornostres Postraumático. Evaluation of the psychometric properties of the Spanish version of 5 questionnaires for the evaluation of posttraumatic stress syndrome [article in Spanish]. Actas Esp Psiquiatr. 2000;28(4):207–218. PubMed
25. Seisdedos Cubero N, Spielberger CD. STAI : Cuestionario de Ansiedad Estado-Rasgo. Madrid, Spain: TEA; 1997.
26. Beck AT, Ward CH, Mendelson M, et al. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4(6):561–571. doi:10.1001/archpsyc.1961.01710120031004 PubMed
27. Heilemann MV, Lee K, Kury FS. Psychometric properties of the Spanish version of the Resilience Scale. J Nurs Meas. 2003;11(1):61–72. doi:10.1891/jnum.11.1.61.52067 PubMed
28. Muris P, Merckelbach H, Van Brakel A, et al. The revised version of the screen for child anxiety related emotional disorders (SCARED-R): further evidence for its reliability and validity. Anxiety Stress Coping. 1999;12(4):411–425. doi:10.1080/10615809908249319 PubMed
29. Spielberger CD, Edwards CD. STAIC: cuestionario de autoevaluación ansiedad estado/ rasgo en niños. Madrid, Spain: Tea; 2001.
30. Kovacs M. CDI: Inventario de depresión infantil: Manual. Madrid, Spain: TEA Ediciones; 2004.
31. Saavedra E, Villalta M. Escala de Resiliencia SV-RES para jóvenes y adultos. Santiago de Chile: CEANIM; 2008.
32. Bisson JI, Roberts NP, Andrew M, et al. Psychological therapies for chronic posttraumatic stress disorder (PTSD) in adults [published online ahead of print December 13, 2013]. Cochrane Database Syst Rev. doi:10.1002/14651858.CD003388.pub4 PubMed
33. Neria Y, Nandi A, Galea S. Posttraumatic stress disorder following disasters: a systematic review. Psychol Med. 2008;38(4):467–480. doi:10.1017/S0033291707001353 PubMed
34. Wang X, Gao L, Shinfuku N, et al. Longitudinal study of earthquake-related PTSD in a randomly selected community sample in north China. Am J Psychiatry. 2000;157(8):1260–1266. doi:10.1176/appi.ajp.157.8.1260 PubMed
Enjoy this premium PDF as part of your membership benefits!

