ABSTRACT
Objective: To determine the prevalence of sexual dysfunction in female patients with schizophrenia receiving olanzapine or risperidone and to understand its relationship with other psychosocial variables.
Methods: This cross-sectional descriptive study evaluated 57 female stabilized schizophrenia outpatients receiving risperidone (n = 28) or olanzapine (n = 29) in the psychiatric departments of a tertiary care hospital in South India from January to May 2019. Sexual dysfunction was assessed with the Changes in Sexual Functioning Questionnaire, severity of psychosis with the Brief Psychiatric Rating Scale, and level of improvement with the Clinical Global Impressions–Improvement and Severity scales.
Results: Among the subjects, 93% of women receiving risperidone experienced sexual dysfunction compared to 83% in the olanzapine group. Sexual responses such as pleasure, frequency of sexual contacts, desire, arousal, and orgasm were significantly low in both drug groups (P < .05). Logistic regression of sexual dysfunction as dependent variable with other important variables found no significant relationship.
Conclusions: This study suggests that sexual dysfunction is an important undetected problem in the majority of female schizophrenia patients. Risperidone was associated with more sexual dysfunction. Sexual dysfunction is an understudied yet important consideration in the treatment of schizophrenia.
Prim Care Companion CNS Disord 2021;23(4):20m02835
To cite: Kumar PNS, Radhika MK, Suresh R, et al. Comparative study of sexual side effects in female patients with schizophrenia receiving risperidone or olanzapine. Prim Care Companion CNS Disord. 2021;23(4):20m02835.
To share: https://doi.org/10.4088/PCC.20m02835
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, IQRAA International Hospital and Research Centre, Malaparamba, Kozhikode, Kerala, India
bDepartment of Psychiatry, Kerala Government Health Services, Calicut, Kerala, India
cDepartment of Medicine, Government Medical College, Cochin, Kerala, India
*Corresponding author: P. N. Suresh Kumar, MD, DNB, MRCPsych, PhD, Anaswara, Vazhathuruthi Rd, PO Civil Station, Kozhikode-673020, Kerala, India ([email protected]).
Sexual dysfunction is a commonly experienced but disturbing and often underrecognized problem associated with schizophrenia.1 Sexual dysfunctions in patients with schizophrenia are often related to their medications, but in many patients, other causes such as stigma, anhedonia, negative symptoms, sociocultural issues, and marital conflicts also coexist.2 Antipsychotic-induced side effects on sexual function are usually inhibitory in nature and may affect all phases of the sexual response cycle. These effects include decreased sexual desire and difficulties with erection, achieving orgasm, and sexual satisfaction, as well as ejaculation disorders. Treatment-emergent sexual dysfunction is known to result in physical and psychological distress and can negatively influence treatment compliance.3 Studies4 have found that between 16% and 60% of patients using antipsychotics experience sexual dysfunctions. Studies5,6 have also investigated sexual dysfunction due to typical antipsychotics and compared typical and atypical antipsychotic agents.
Research has shown that female patients with schizophrenia experience a significantly higher rate of sexual dysfunction compared to male patients.7 Antipsychotic-induced hyperprolactinemia and alterations in the levels of estrogen and thyroxine have been suggested as the potential reasons for female sexual dysfunction in schizophrenia.8 However, in conservative societies, women may not openly disclose their sexual problems with the therapist unless specifically asked. In India, it is often considered taboo for women to disclose and discuss their sexual dysfunction as a result of the male-dominated society and puritanical mindset.9 Hence, epidemiologic investigations regarding female sexual dysfunction in India are scant, and, to the best of our knowledge, there are no studies to date investigating sexual dysfunction in female patients with schizophrenia receiving atypical antipsychotics.
Two previous studies from India compared sexual dysfunction among male patients with schizophrenia taking risperidone and olanzapine. Nagaraj et al10 found that 96% of patients suffered from sexual dysfunction with risperidone and 90% with olanzapine. Kumar and Sinha11 found that 86% of patients reported sexual dysfunction in the risperidone group compared to 48.3% in the olanzapine group. However, such a higher prevalence of sexual dysfunction with risperidone among males may not be generalizable to the female population, as a study7 from Turkey found a high prevalence of self-reported sexual dysfunction in female patients with schizophrenia as well as controls. The authors7 argued that the dysfunction in female patients with schizophrenia cannot be attributed to their illness or to the medications they are taking. Hence, the aim of this study was to determine the prevalence of sexual dysfunction in female patients with schizophrenia receiving olanzapine and risperidone and to gain a further understanding of its relationship with other psychosocial variables.
METHODS
This study was conducted in the psychiatric departments of a tertiary care hospital in South India from January to May 2019. The subjects comprised stabilized outpatients who met DSM-IV criteria for schizophrenia.12 Patients included were aged ≥ 18 years and had received olanzapine or risperidone for at least 2 months prior to entering the study. Medications were prescribed by the patients’ psychiatrist using clinical judgment.
The exclusion criteria were other psychiatric disorders; patients receiving other antipsychotics, antidepressants, or mood stabilizers; pregnancy; and substance abuse or dependency. The study was approved by the institutional ethics committee and the study protocol was developed in accordance with the ethical standards of good clinical practice, and the Declaration of Helsinki.
Detailed explanations were given to patients about the purpose of the study. Confidentiality of the information was assured, and informed consent was taken prior to enrolling patients. Rapport was established, and an explanation of the study tools was provided. A semistructured interview schedule was used to collect the data. Total time taken for data collection was 1 ½ hours for each patient. Assessments were carried out by M.K.R. Information was obtained from both the patient and caregiver.
Sexual dysfunction was assessed using the Changes in Sexual Functioning Questionnaire (CSFQ).13 The CSFQ is a clinician-rated, structured interview/questionnaire designed to measure dysfunction and changes in sexual function during treatment with medication. The CSFQ consists of 35 questions for women and assesses components of sexuality pertaining to pleasure, desire/frequency, desire/interest, arousal, and orgasm. After collecting the sociodemographic and clinical data, patients were rated on the Brief Psychiatric Rating Scale (BPRS)14 to assess the severity of psychopathology. The Clinical Global Impressions–Improvement (CGI-I) and Severity (CGI-S) scales15 were also applied to assess the severity of illness and the level of improvement.
Analysis of Data
Descriptive statistics were applied to obtain the means and frequencies of the sociodemographic and clinical variables of the sample. Student t test was used to compare the continuous variables in the demographic data as well as mean chlorpromazine equivalent doses of the study groups. To compare sexual dysfunction and its components, nonparametric tests were used. The mean scores of the sexual functioning questionnaire on the domains of desire, arousal/erection, orgasm/ejaculation, and overall sexual impairment were also compared using t test. The CSFQ is designed such that the higher the score, the more severe the sexual dysfunction. Logistic regression was applied to determine the factors affecting sexual dysfunction.
RESULTS
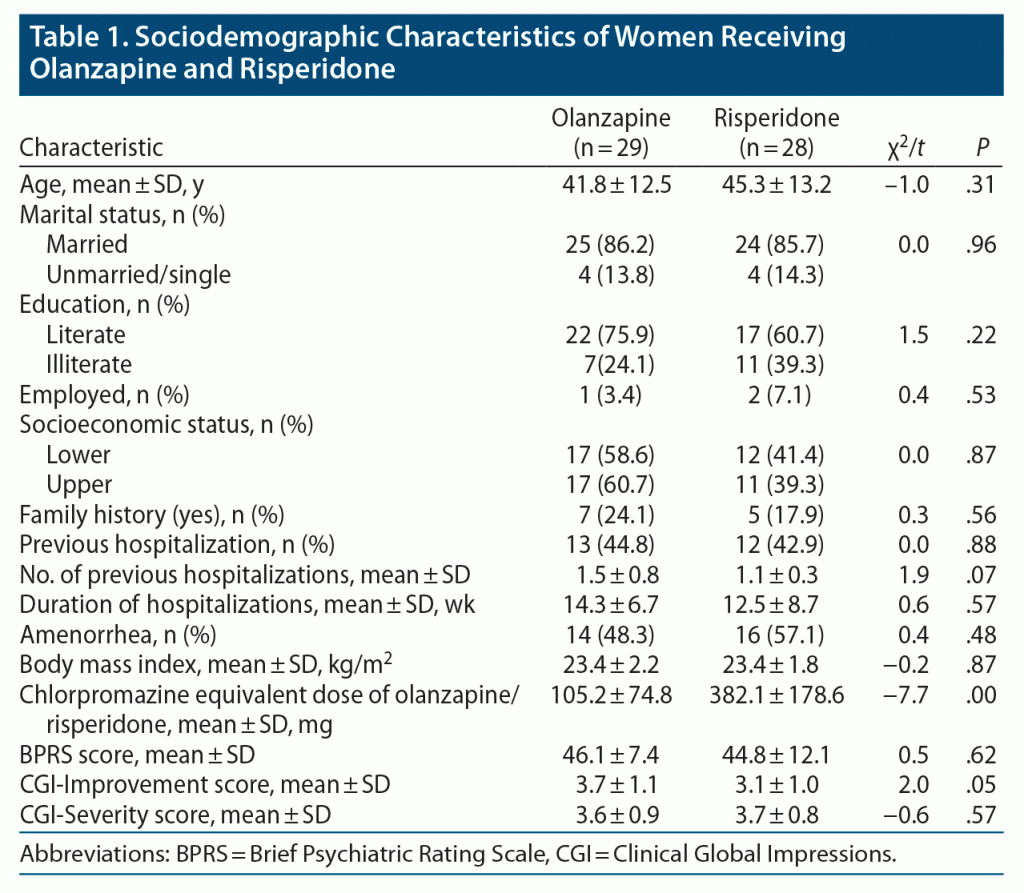
A total of 29 patients received olanzapine and 28 patients received risperidone. The mean ± SD age of the patient population receiving olanzapine was 41.8 ± 12.5 years and those receiving risperidone was 45.3 ± 13.2 years. The majority of the patients in both groups (olanzapine vs risperidone, respectively) were married (86.2% vs 85.7%) and literate (75.9% vs 60.7%). In the olanzapine group, 48.3% of patients reported amenorrhea compared to 57.1% in the risperidone group. The mean chlorpromazine-equivalent dose was significantly higher in the risperidone group (382.1 ± 178.6 vs 105.2 ± 74.8, P < .001). CGI improvement was higher in the olanzapine group (3.7 ± 1.1 vs 3.1 ± 1.0, P = .05). The comparisons of sociodemographic and clinical variables of the 2 groups are summarized in Table 1.
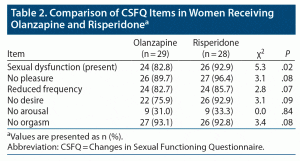
The comparison of CSFQ items in women receiving olanzapine and risperidone showed that those taking risperidone had a statistically significant higher rate of sexual dysfunction (92.9% vs 82.8%, P = .02). Other items such as frequency of sexual contacts, pleasure, desire, arousal, and orgasm were significantly low but comparable among both groups. The details are summarized in Table 2.
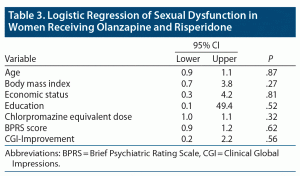
Step-wise logistic regression of all the important variables in this study with sexual dysfunction as dependent variable showed that none of these variables became significant in this analysis (Table 3).
DISCUSSION
In the index study, the majority of female patients reported impairment in sexual function. The risperidone group (93%) experienced a significantly higher rate of sexual dysfunction than the olanzapine group (83%). A similar finding was reported by Knegtering et al.16 In that study, less sexual dysfunction occurred in the group treated with olanzapine (12%) compared with the risperidone group (52%). The mean dose was 9.4 mg/d for olanzapine and 3.4 mg/d for risperidone. In our study, the mean equivalent dose of chlorpromazine was significantly higher in the risperidone group. Moreover, our study results are also similar to studies10,11 conducted with male patients with schizophrenia in India, in which sexual dysfunctions were reported more often with risperidone compared to olanzapine.
Other than sexual dysfunction, sexual responses like pleasure, frequency of sexual contacts, desire, arousal, and orgasm were significantly low in both medication groups (P < .05). A significant number of patients in the risperidone and olanzapine groups reported orgasmic dysfunction. This is an important finding with respect to sexual life satisfaction. Unfortunately, many female patients will not voice their sexual problems due to inhibition and cultural taboos.
The higher rate of sexual dysfunction in the risperidone group could be due to the following reasons. These patients were receiving a higher dose of antipsychotic than the olanzapine group. Research has shown that risperidone has more propensity to produce hyperprolactinemia due to dopamine antagonism than olanzapine.17 Hyperprolactinemia can produce sexual dysfunction and amenorrhea. However, none of the patients in either group had galactorrhea. The prevalence of amenorrhea was comparable in both groups. Hence, the contribution of hyperprolactinemia in the genesis of sexual dysfunction may be unlikely in our patients.
Reduced sexual activity may also be related to the underlying multiple pathologic processes of schizophrenia itself, including disturbed psychomotor performance, as well as to social consequences of the condition such as reduced sexual desire or inability to perform sexual activity.18 Research has shown that a majority of untreated schizophrenia patients have a reduced desire for sex—higher in females than males—although arousal and ejaculatory functions remain relatively intact.19 In the present study, comparison of severity of illness and the level of improvement was comparable in both groups. Hence, sexual dysfunction cannot be explained on the basis of severity of illness. Ideally, to clarify this point we need to assess the serum prolactin levels in both groups and measure confounding variables such as psychomotor and cognitive performance and social skills. Liu-Seifert et al,20 in a study of sexual dysfunction in schizophrenia patients treated with risperidone, reported a linear relationship between age and sexual dysfunction in male patients. There was an increase of sexual dysfunction by 40% with each 10-year age increase in males.20 Such a relationship could not be established in our study.
An important limitation of this study is that we did not include other atypical antipsychotic drugs. As the primary objective of the study was to evaluate prevalence of sexual dysfunction with risperidone and olanzapine, only those drugs were included. A second limitation is that the CSFQ has not been specifically validated in schizophrenia patients treated with antipsychotics. A third limitation is that the study allowed only a cross-sectional examination of sexual dysfunction. Assessment of serum prolactin level and other psychological variables affecting sexual performance would have provided better insight about sexual dysfunction. Prospective, controlled studies that follow patients over a period of time will be able to provide further insights on the time course of the development of sexual dysfunction and its impact on quality of life.
Overall, this study suggests that sexual dysfunction is an important undetected problem in the majority of female schizophrenia patients. Risperidone was associated with more sexual dysfunction than olanzapine. Sexual dysfunction is an understudied yet important consideration in the treatment of schizophrenia. More attention is warranted in this area, as it may provide opportunities for improved quality of life and adherence to treatment. Direct questioning about sexual functioning is necessary to avoid underestimating the frequency of sexual side effects in patients with schizophrenia.
Submitted: October 12, 2020; accepted December 29, 2020.
Published online: July 22, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Acknowledgments: The authors acknowledge the contribution of Jaison Joy, MSc (research coordinator, IQRAA Hospital) and T. P. Binsha, MSc and P. Thoohima, MSW (clinical psychologists, IQRAA Hospital) for their valuable assistance in data collection and manuscript preparation. Mr Joy and Ms Binsha and Mrs Thoohima report no conflicts of interest related to the subject of this article.
CLINICAL POINTS
- Sexual dysfunction is an important undetected problem in female patients with schizophrenia.
- Sexual responses such as pleasure, frequency of sexual contacts, desire, arousal, and orgasm were significantly low among female patients taking risperidone and olanzapine.
- Risperidone was associated with more sexual dysfunction among female patients than olanzapine.
References (20)

- Uçok A, Incesu C, Aker T, et al. Sexual dysfunction in patients with schizophrenia on antipsychotic medication. Eur Psychiatry. 2007;22(5):328–333. PubMed CrossRef
- Mendrek A, Stip E. Sexual dimorphism in schizophrenia: is there a need for gender-based protocols? Expert Rev Neurother. 2011;11(7):951–959. PubMed CrossRef
- Costa AM, Lima MS, Mari JdeJ. A systematic review on clinical management of antipsychotic-induced sexual dysfunction in schizophrenia. Sao Paulo Med J. 2006;124(5):291–297. PubMed CrossRef
- Serretti A, Chiesa A. A meta-analysis of sexual dysfunction in psychiatric patients taking antipsychotics. Int Clin Psychopharmacol. 2011;26(3):130–140. PubMed CrossRef
- Nagaraj AK, Nizamie HS, Akhtar S, et al. A comparative study of sexual dysfunction due to typical and atypical antipsychotics in remitted bipolar I disorder. Indian J Psychiatry. 2004;46(3):261–266. PubMed
- Byerly MJ, Nakonezny PA, Bettcher BM, et al. Sexual dysfunction associated with second-generation antipsychotics in outpatients with schizophrenia or schizoaffective disorder: an empirical evaluation of olanzapine, risperidone, and quetiapine. Schizophr Res. 2006;86(1–3):244–250. PubMed CrossRef
- Hocaoglu C, Celik FH, Kandemir G, et al. Sexual dysfunction in outpatients with schizophrenia in Turkey: a cross-sectional study. Shanghai Jingshen Yixue. 2014;26(6):347–356. PubMed
- Lodha P, Sousa AD. Female sexual dysfunction and schizophrenia: a clinical review. J Psychosexual Health. 2020;2(1):44–55. CrossRef
- Shetageri VN, Bhogale GS, Patil NM, et al. Sexual dysfunction among females receiving psychotropic medication: a hospital-based cross-sectional study. Indian J Psychol Med. 2016;38(5):447–454. PubMed CrossRef
- Nagaraj AK, Pai NB, Rao S. A comparative study of sexual dysfunction involving risperidone, quetiapine, and olanzapine. Indian J Psychiatry. 2009;51(4):265–271. PubMed CrossRef
- Kumar SVS, Sinha VK. Comparative study of sexual dysfunction and serum prolactin level associated with olanzapine, risperidone, and clozapine in patients with remitted schizophrenia. Indian J Psychiatry. 2015;57(4):386–391. PubMed CrossRef
- American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
- Clayton AH, McGarvey EL, Clavet GJ. The Changes in Sexual Functioning Questionnaire (CSFQ): development, reliability, and validity. Psychopharmacol Bull. 1997;33(4):731–745. PubMed
- Overall JE, Gorham DR. The Brief Psychiatric Rating Scale. Psychol Rep. 1962;10(3):799–812. CrossRef
- Guy W. ECDEU Assessment Manual for Psychopharmacology. Revised Edition. Washington, DC: US Department of Health, Education, and Welfare; 1976.
- Knegtering H, Boks M, Blijd C, et al. A randomized open-label comparison of the impact of olanzapine versus risperidone on sexual functioning. J Sex Marital Ther. 2006;32(4):315–326. PubMed CrossRef
- Kinon BJ, Gilmore JA, Liu H, et al. Prevalence of hyperprolactinemia in schizophrenic patients treated with conventional antipsychotic medications or risperidone. Psychoneuroendocrinology. 2003;28(suppl 2):55–68. PubMed
- Howes OD, Wheeler MJ, Pilowsky LS, et al. Sexual function and gonadal hormones in patients taking antipsychotic treatment for schizophrenia or schizoaffective disorder. J Clin Psychiatry. 2007;68(3):361–367. PubMed CrossRef
- Aizenberg D, Zemishlany Z, Dorfman-Etrog P, et al. Sexual dysfunction in male schizophrenic patients. J Clin Psychiatry. 1995;56(4):137–141. PubMed
- Liu-Seifert H, Kinon BJ, Tennant CJ, et al. Sexual dysfunction in patients with schizophrenia treated with conventional antipsychotics or risperidone. Neuropsychiatr Dis Treat. 2009;5:47–54. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!