Objective: To compare the rate of hospitalizations for pneumonia in patients with a psychotic or bipolar disorder who were prescribed 1 of 4 second-generation antipsychotics prior to admission.
Methods: This retrospective cohort study included patients who were medically admitted for pneumonia to a 2,059-bed academic medical center or its associated health system hospital. Medical records of 872 admissions from November 1, 2016 to December 15, 2018, were included for all adults with a diagnosis of schizophrenia, schizoaffective disorder, or bipolar disorder prescribed clozapine, olanzapine, quetiapine, or risperidone prior to admission.
Results: There was no significantly increased risk of pneumonia for patients taking olanzapine (odds ratio [OR] = 1.08, 95% CI, 0.48-2.41) or quetiapine (OR = 0.97, 95% CI, 0.42-2.25) prior to admission compared to risperidone. When controlling for various factors, treatment with a combination of antipsychotics including clozapine (OR = 2.28, 95% CI, 1.13-4.62, P = .022) and clozapine alone (OR = 2.37, 95% CI, 1.30-4.32, P = .005) was associated with an increased risk of pneumonia-related hospitalization compared to treatment with risperidone, olanzapine, or quetiapine alone.
Conclusions: The findings of this study in combination with other published literature support an association of an increased risk of pneumonia with the use of clozapine, although this cannot be interpreted as causal. These data show that use of clozapine alone or in combination with other antipsychotics significantly increases risk of pneumonia, although this finding cannot be deemed causal due to study design.
ABSTRACT
Objective: To compare the rate of hospitalizations for pneumonia in patients with a psychotic or bipolar disorder who were prescribed 1 of 4 second-generation antipsychotics prior to admission.
Methods: This retrospective cohort study included patients who were medically admitted for pneumonia to a 2,059-bed academic medical center or its associated health system hospital. Medical records of 872 admissions from November 1, 2016 to December 15, 2018, were included for all adults with a diagnosis of schizophrenia, schizoaffective disorder, or bipolar disorder prescribed clozapine, olanzapine, quetiapine, or risperidone prior to admission.
Results: There was no significantly increased risk of pneumonia for patients taking olanzapine (odds ratio [OR] = 1.08, 95% CI, 0.48–2.41) or quetiapine (OR = 0.97, 95% CI, 0.42–2.25) prior to admission compared to risperidone. When controlling for various factors, treatment with a combination of antipsychotics including clozapine (OR = 2.28, 95% CI, 1.13–4.62, P = .022) and clozapine alone (OR = 2.37, 95% CI, 1.30–4.32, P = .005) was associated with an increased risk of pneumonia-related hospitalization compared to treatment with risperidone, olanzapine, or quetiapine alone.
Conclusions: The findings of this study in combination with other published literature support an association of an increased risk of pneumonia with the use of clozapine, although this cannot be interpreted as causal. These data show that use of clozapine alone or in combination with other antipsychotics significantly increases risk of pneumonia, although this finding cannot be deemed causal due to study design.
Prim Care Companion CNS Disord 2020;22(4):20m02594
To cite: Milano VR, Kayhart BM, Morgan RJ, et al. Second-generation antipsychotics and pneumonia-related hospitalizations. Prim Care Companion CNS Disord. 2020;22(4):20m02594.
To share: https://doi.org/10.4088/PCC.20m02594
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Pharmacy, Mayo Clinic, Rochester, Minnesota
bDepartment of Psychiatry and Psychology, Mayo Clinic, Rochester, Minnesota
cDivision of Infectious Diseases, Department of Internal Medicine, Mayo Clinic, Rochester, Minnesota
dDepartment of Cardiovascular Diseases, Mayo Clinic, Rochester, Minnesota
eDivision of Biomedical Statistics and Informatics, Mayo Clinic, Rochester, Minnesota
*Corresponding author: Jonathan G. Leung, PharmD, 1216 2nd St SW, Rochester, MN 55902 ([email protected]).
In the United States, pneumonia is the most common cause of hospitalization other than childbirth, with an estimated 1 million adults having contact with a hospital for treatment.1 Despite treatment guidelines and ample medications, the mortality rate from pneumonia in the United States is estimated to be 5%.1,2 There are numerous risk factors for the development of pneumonia such as chronic obstructive pulmonary disease (COPD), smoking, and alcohol use.3 Patients with schizophrenia and related psychoses have higher rates of COPD, smoking, and alcohol use disorder compared to the general population, which may put them at increased risk for pneumonia.4–6 A study7 involving patients with schizophrenia found that advanced age, low body weight, smoking, use of a second-generation antipsychotic (SGA), and higher doses of antipsychotics were risk factors for pneumonia. These results add to growing evidence suggesting that treatment with antipsychotics may increase the risk of pneumonia in patients with psychiatric illness.8 While antipsychotics have been associated with increased mortality, with a large proportion of these deaths attributed to pneumonia in patients with dementia, there is less evidence of this association specifically in adults with psychotic or bipolar illness.9,10 This observation was highlighted in a recent meta-analysis11 of 19 studies in which only 5 specifically looked at patients with a diagnosis of a primary psychotic or bipolar disorder.
Of antipsychotics, clozapine, due to its pharmacologic receptor-binding profile and common side effect of sialorrhea, may be associated with the greatest pneumonia risk.8,12–15 One study16 that assessed the primary reason for medical hospitalization for patients prescribed clozapine reported that pulmonary illness was the leading cause, and pneumonia represented 58% of all pulmonary-related hospitalizations. While clozapine has been consistently associated with pneumonia, little is known about this risk relative to other agents. A retrospective cohort study was conducted to compare the rate of hospitalizations due to pneumonia in patients prescribed an SGA prior to admission and diagnosed with a primary psychotic or bipolar disorder.
METHODS
This was a retrospective cohort study involving patients medically admitted to a 2,059-bed academic medical center or its associated health system hospital. Medical records of admissions from November 1, 2016, to December 15, 2018, were included for all adults (aged 18 and older) who were prescribed clozapine, olanzapine, quetiapine, or risperidone at the time of a medical hospital admission. Additional inclusion criteria included a diagnosis of schizophrenia, schizoaffective disorder, or bipolar disorder. In the state of Minnesota, patients may indicate that their medical record cannot be used for any type of research purpose. These patients were excluded. This study was approved by the Mayo Clinic Institutional Review Board.
Patients with schizophrenia, schizoaffective disorder, or bipolar disorder taking clozapine, olanzapine, quetiapine, or risperidone at the time of hospital admission were identified using an electronic pharmacy database. Patients could have been admitted more than once during the study period.
Diagnoses and prescriptions were manually validated by chart review. Additionally, data pertaining to age, sex, admission diagnosis, length of stay, dose of antipsychotic, absolute neutrophil count, and tobacco use were collected. Tobacco use was defined by a diagnosis of tobacco use disorder, tobacco use on day of admission, or an order for nicotine replacement therapy on admission. Charlson Comorbidity Index17 score was calculated for each patient for purposes of baseline comparison. The medical records of patients with a diagnosis of pneumonia were reviewed further for classification of the pneumonia, date of antipsychotic initiation (if known or estimate), height, weight, and absolute neutrophil count.
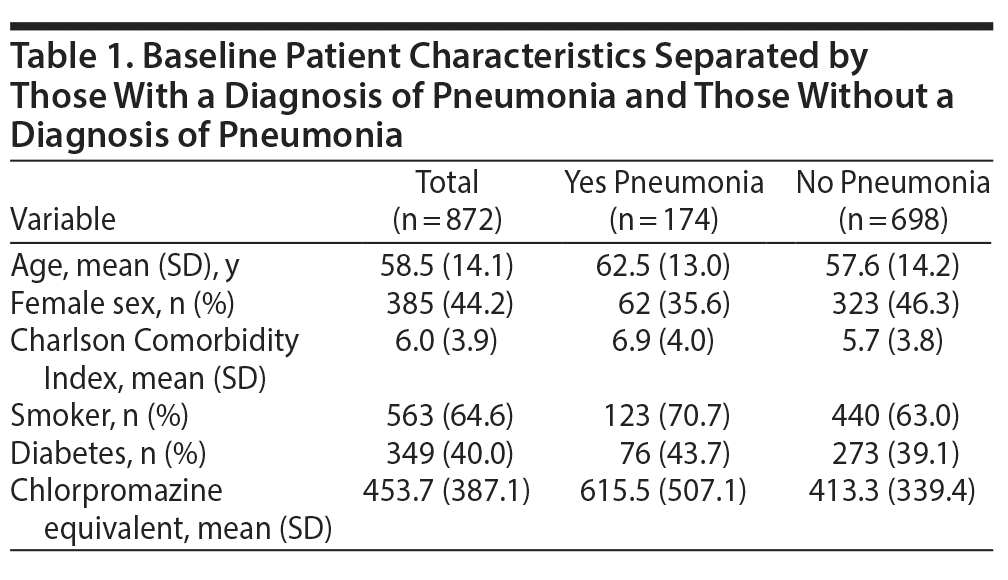
Continuous variables were described using means and SDs or medians and interquartile ranges (IQRs), and categorical variables were described using counts and percentages. Baseline characteristics (Table 1) were compared between drug groups using generalized estimating equation (GEE) to take into account that patients may have had more than 1 admission during the study period and that these admissions may be correlated with each other. The exchangeable correlation structure was used for these models. A univariate GEE model was utilized to assess the association between drug groups and diagnosis of pneumonia. Given a lack of antihistaminic and antimuscarinic receptor binding, risperidone was used as the baseline comparator, similar to another study.18 A multivariable GEE analysis was also conducted to control for age, sex, Charlson Comorbidity Index, smoking status, diabetes diagnosis, and antipsychotic dose in chlorpromazine equivalents. All tests were 2-sided, and P ≤ .05 was considered to be statistically significant. Statistical analyses were performed using SAS version 9.4 software (SAS Institute, Inc, Cary, North Carolina).
RESULTS
There were 872 patient hospitalizations identified and included in our analysis. The mean age was 59 years, and the majority of patients were male (n = 487, 55.8%). The demographic data of patients with and without pneumonia by Charlson Comorbidity Index scores, diabetes, tobacco use, age, and antipsychotic dose can be found in Table 2. In the multivariate analysis, tobacco use approached significance (P = .052) between those with (70.7%) and without (63%) pneumonia. There was a statistically significant difference in terms of home prescription chlorpromazine equivalents, with a mean ± SD dose of 615.5 + 507.1 mg in the pneumonia group and 413.3 + 339.4 mg in the group without pneumonia (P < .001). Mean ± SD absolute neutrophil count between the pneumonia (11,400/microL ± 7,200/microL) and nonpneumonia (6,900/microL ± 3,900/microL) groups was statistically significant but most likely not clinically significant. Among those with pneumonia, there were significant pairwise differences (adjusted for multiple comparisons): between the polypharmacy group (no clozapine) versus the clozapine-only group (9,000/microL ± 5,200/microL versus 14,000/microL ± 7,400/microL, P = .014) and clozapine-only group versus the olanzapine group (9,000/microL ± 5,200/microL versus 8,000/microL ± 5,600/microL, P = .014).
Of the 134 patients taking clozapine at admission, 39 (29.1%) had a pneumonia diagnosis compared with 23 of 172 (13.4%) in the olanzapine group, 21 of 172 (12.2%) in the quetiapine group, and 19 of 152 (12.5%) in the risperidone group. Patients who were taking any combination of antipsychotics exhibited the highest rates of pneumonia with 72 documented cases out of 242 patients (29.8%).
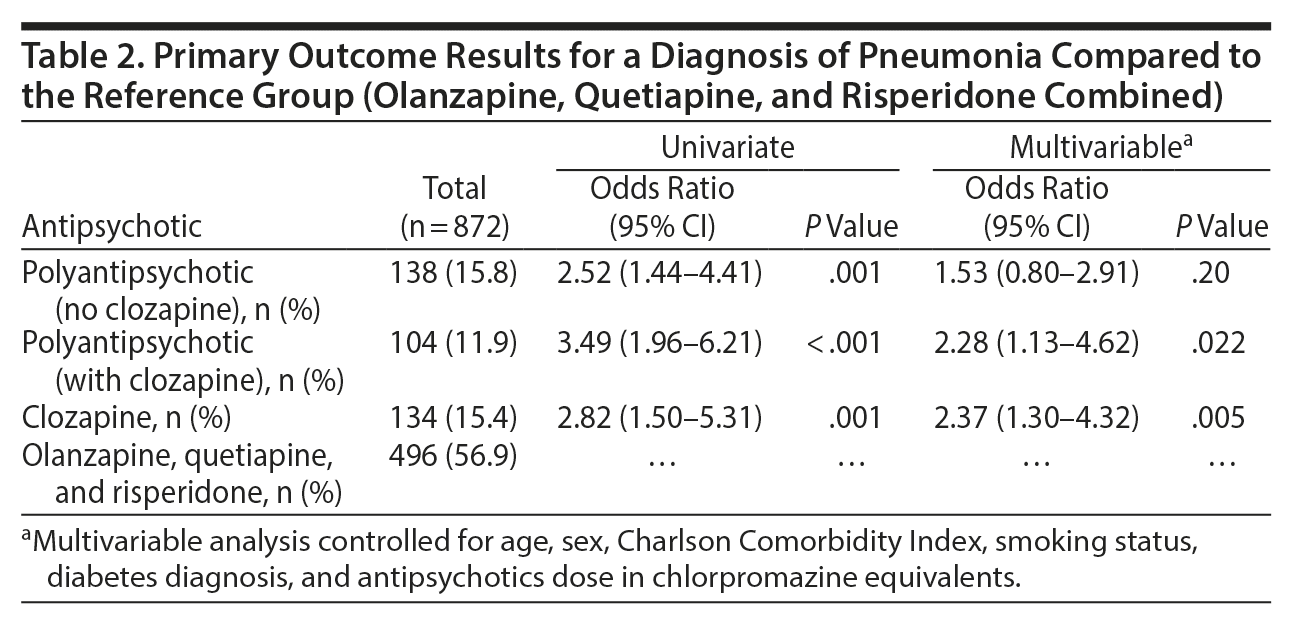
In the initial analysis, there was no significantly increased risk of pneumonia for patients taking olanzapine or quetiapine prior to admission compared to risperidone (odds ratio [OR] = 1.08, 95% CI, 0.48–2.41) or quetiapine (OR = 0.97, 95% CI, 0.42–2.25). Therefore, these 3 SGAs were combined into 1 group and compared to clozapine alone and a combination of antipsychotics both including and excluding clozapine. In the univariate analysis, combinations of antipsychotics excluding clozapine (OR = 2.52; 95% CI, 1.44–4.41; P = .001), combinations of antipsychotics including clozapine (OR = 3.49; 95% CI , 1.96–6.21; P < .001), and clozapine alone (OR = 2.82; 95% CI , 1.50–5.31; P = .001) were associated with an increased risk of pneumonia compared to the combined olanzapine, quetiapine, and risperidone group.
When adjusting for confounders in the multivariable model (accounting for age, sex, Charlson Comorbidity Index, smoking status, diabetes diagnosis, and chlorpromazine dosage equivalents), the combinations of antipsychotics including clozapine (OR = 2.28; 95% CI , 1.13–4.62; P = .022) and clozapine alone (OR = 2.37; 95% CI , 1.30–4.32; P = .005) remained significant compared to the combined olanzapine, quetiapine, and risperidone group. The combination antipsychotic group excluding clozapine no longer remained statistically significant when confounders in the multivariable model were applied.
DISCUSSION
This retrospective cohort study compared the rates of pneumonia hospitalizations in patients with schizophrenia, schizoaffective disorder, or bipolar disorder who were taking clozapine, olanzapine, quetiapine, or risperidone prior to admission. We found that the use of clozapine alone or in combination with other antipsychotics (including SGAs) was associated with a statistically significant increased risk of pneumonia hospitalizations compared to risperidone, olanzapine, and quetiapine alone.
A potential mechanism for the increased rate of pneumonia hospitalizations with clozapine is the receptor-binding affinities that clozapine possesses. The antihistamine and anticholinergic effects of clozapine cause sedation and decreased respiratory secretion clearance ability, leading to potential increased risk for aspiration.19 However, olanzapine is also a strong antagonist of histaminergic and muscarinic receptors, suggesting that this hypothesis is not complete or accurate given the lower rates of pneumonia seen with olanzapine. A second hypothesis is that clozapine-associated pneumonia is related to its common side effect of sialorrhea, leading to aspiration and secondary pneumonia.13,19–22 Sialorrhea more commonly associated with clozapine is in part explained by its agonist affinity at M4 muscarinic and antagonism at α-2 adrenergic receptors.23 Olanzapine has lower affinity for these receptors, possibly accounting for the differing pneumonia rates between the 2 agents. Esophageal dysmotility and dopamine antagonism may also play a role in the increased pneumonia rates seen when clozapine is combined with other antipsychotics.13,19
Our findings are similar to other published studies comparing the rates of pneumonia between SGAs, including in patients taking antipsychotics for indications other than a primary psychotic or bipolar disorder. Stoecker et al18 conducted a retrospective, case-matched study comparing the incidence of pneumonia in patients taking clozapine, risperidone, or no antipsychotics and found an increased rate of pneumonia with clozapine compared to risperidone, similar to our findings. Additionally, the authors found that use of risperidone did not significantly increase the risk of pneumonia compared to the general population. Kuo et al8 examined a large cohort of patients with schizophrenia in Taiwan and compared the rates of pneumonia between different SGAs. They excluded patients older than age 65 years and only included patients in the National Health Insurance Research Database in Taiwan. Similar to the findings from Kuo et al,8 our study found the highest pneumonia rates with clozapine and a combination of antipsychotics followed by olanzapine, quetiapine, and risperidone. Yang et al24 conducted a case-control study to compare the risk of pneumonia between individual antipsychotics and mood stabilizers in a Taiwanese bipolar patient population. The study included only patients enrolled in the National Health Insurance Research Database in Taiwan and found that antipsychotics, but not mood stabilizers, were associated with a higher risk of pneumonia. Additionally, a combination of antipsychotics and mood stabilizers led to increased risk for pneumonia. The findings from Yang et al24 differed from our study in that in a solely bipolar Taiwanese patient population, the rates of pneumonia in patients taking olanzapine were very similar to those taking clozapine. A systematic review and meta-analysis11 found that both first-generation antipsychotics and SGAs increase the risk of pneumonia compared to no antipsychotic use, but the majority of publications assessed in this article were related to those with dementia.
Our study has limitations. Due to its retrospective nature, we are reliant on information documented. Determining compliance with medication(s) prior to admission would be ideal but was not possible. Also, the diagnosis of a primary psychotic disorder or bipolar disorder was based on diagnostic coding. Patients taking clozapine may have had additional risk factors requiring presentation to the hospital for pneumonia treatment, and we may have missed patients that were treated for pneumonia in the community setting not requiring hospitalization. Medications, such as antibiotics prior to admission, were not taken into account. Clozapine levels were not available for the vast majority of patients. Patients taking clozapine and olanzapine are at higher risk for metabolic syndrome complications including diabetes, and a diagnosis of diabetes is associated with increased rates of pneumonia.25,26 We therefore included diabetes in the multivariable analysis to account for this association, and it did not appear that diabetes was a driver for pneumonia hospitalizations. We did not include a general population group and used risperidone as the reference group based on a prior study18 that found that patients taking risperidone had similar rates of pneumonia as the general population. However, comparisons to a general population would be difficult with regard to patients with schizophrenia, schizoaffective disorder, or bipolar disorder given potential differences in rates of smoking and medical comorbidities. Another weakness is the lack of adequate data on alcohol or substance abuse. Additionally, channeling bias and systematic bias are possible in that patients taking clozapine are more closely followed and often more severely ill, leading to potentially increased admissions to the hospital and increased findings of pneumonia, although we found no difference in Charlson Comorbidity Index scores in our study between different antipsychotic groups.
The use of clozapine alone and in combination with other antipsychotics was associated with an increased risk for hospitalization due to pneumonia compared to risperidone. These findings reinforce that patients taking clozapine require monitoring for signs and symptoms of pneumonia, and clinicians should be made aware of this adverse effect. Also, future studies should determine if treating sialorrhea in patients taking clozapine would reduce the incidence of pneumonia. Future studies should focus on preventive treatment strategies for clozapine-associated pneumonia.
CONCLUSION
Patients with schizophrenia, schizoaffective disorder, or bipolar disorder taking either clozapine alone or in combination with other antipsychotics had a statistically increased risk of pneumonia-related hospitalization compared to those taking other SGAs, although this finding cannot be deemed a causal relationship based on study design.
Clinical Points
- An association between clozapine and pneumonia exists.
- Additional research is needed to elucidate risk factors and potential prevention strategies for clozapine-associated pneumonia.
- Awareness of clozapine-associated pneumonia is important for clinicians, both in medical and psychiatry practices.
Submitted: January 17, 2020; accepted April 24, 2020.
Published online: August 6, 2020.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. American Thoracic Society website. Top 20 pneumonia facts—2019. https://www.thoracic.org/patients/patient-resources/resources/top-pneumonia-facts.pdf. Accessed July 13, 2020.
2. Centers for Disease Control and Prevention website. Health, United States, 2017—with special feature on mortality. https://www.cdc.gov/nchs/data/hus/hus17.pdf. Accessed July 13, 2020.
3. Torres A, Peetermans WE, Viegi G, et al. Risk factors for community-acquired pneumonia in adults in Europe: a literature review. Thorax. 2013;68(11):1057–1065. PubMed CrossRef
4. Centers for Disease Control and Prevention (CDC). Progress in increasing breastfeeding and reducing racial/ethnic differences—United States, 2000–2008 births. MMWR Morb Mortal Wkly Rep. 2013;62(5):77–80. PubMed
5. The NSDUH Report Data Spotlight. Adults with mental illness or substance use disorder account for 40 percent of all cigarettes smoked. Substance Abuse and Mental Health Services Administration website. https://www.samhsa.gov/data/sites/default/files/spot104-cigarettes-mental-illness-substance-use-disorder/spot104-cigarettes-mental-illness-substance-use-disorder.pdf. March 20, 2013. Accessed July 13, 2020.
6. Margolese HC, Malchy L, Negrete JC, et al. Drug and alcohol use among patients with schizophrenia and related psychoses: levels and consequences. Schizophr Res. 2004;67(2–3):157–166. PubMed CrossRef
7. Haga T, Ito K, Sakashita K, et al. Risk factors for pneumonia in patients with schizophrenia. Neuropsychopharmacol Rep. 2018;38(4):204–209. PubMed CrossRef
8. Kuo CJ, Yang SY, Liao YT, et al. Second-generation antipsychotic medications and risk of pneumonia in schizophrenia. Schizophr Bull. 2013;39(3):648–657. PubMed CrossRef
9. Schneider LS, Dagerman KS, Insel P. Risk of death with atypical antipsychotic drug treatment for dementia: meta-analysis of randomized placebo-controlled trials. JAMA. 2005;294(15):1934–1943. PubMed CrossRef
10. Ralph SJ, Espinet AJ. Increased all-cause mortality by antipsychotic drugs: updated review and meta-analysis in dementia and general mental health care. J Alzheimers Dis Rep. 2018;2(1):1–26. PubMed CrossRef
11. Dzahini O, Singh N, Taylor D, et al. Antipsychotic drug use and pneumonia: systematic review and meta-analysis. J Psychopharmacol. 2018;32(11):1167–1181. PubMed CrossRef
12. Leung JG, Nelson S, Barreto JN, et al. Necrotizing pneumonia in the setting of elevated clozapine levels. J Clin Psychopharmacol. 2016;36(2):176–178. PubMed CrossRef
13. Gurrera RJ, Parlee AC, Perry NL. Aspiration pneumonia: an underappreciated risk of clozapine treatment. J Clin Psychopharmacol. 2016;36(2):174–176. PubMed CrossRef
14. Galappathie N, Khan S. Clozapine-associated pneumonia and respiratory arrest secondary to severe constipation. Med Sci Law. 2014;54(2):105–109. PubMed CrossRef
15. Wu CS, Chen TY, Tsai SY, et al. Estimating the risk of pneumonia in patients with schizophrenia newly receiving clozapine: a nationwide cohort study. J Clin Psychopharmacol. 2019;39(4):297–304. PubMed CrossRef
16. Leung JG, Hasassri ME, Barreto JN, et al. Characterization of admission types in medically hospitalized patients prescribed clozapine. Psychosomatics. 2017;58(2):164–172. PubMed CrossRef
17. Charlson ME, Pompei P, Ales KL, et al. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–383. PubMed CrossRef
18. Stoecker ZR, George WT, O’Brien JB, et al. Clozapine usage increases the incidence of pneumonia compared with risperidone and the general population: a retrospective comparison of clozapine, risperidone, and the general population in a single hospital over 25 months. Int Clin Psychopharmacol. 2017;32(3):155–160. PubMed CrossRef
19. Kaplan J, Schwartz AC, Ward MC. Clozapine-associated aspiration pneumonia: case series and review of the literature. Psychosomatics. 2018;59(2):199–203. PubMed CrossRef
20. Herzig SJ, LaSalvia MT, Naidus E, et al. Antipsychotics and the risk of aspiration pneumonia in individuals hospitalized for nonpsychiatric conditions: a cohort study. J Am Geriatr Soc. 2017;65(12):2580–2586. PubMed CrossRef
21. Saenger RC, Finch TH, Francois D. Aspiration pneumonia due to clozapine-induced sialorrhea. Clin Schizophr Relat Psychoses. 2016;9(4):170–172. PubMed CrossRef
22. Trigoboff E, Grace J, Szymanski H, et al. Sialorrhea and aspiration pneumonia: a case study. Innov Clin Neurosci. 2013;10(5–6):20–27. PubMed
23. Bymaster FP, Felder CC, Tzavara E, et al. Muscarinic mechanisms of antipsychotic atypicality. Prog Neuropsychopharmacol Biol Psychiatry. 2003;27(7):1125–1143. PubMed CrossRef
24. Yang S-Y, Liao Y-T, Liu H-C, et al. Antipsychotic drugs, mood stabilizers, and risk of pneumonia in bipolar disorder: a nationwide case-control study. J Clin Psychiatry. 2013;74(1):e79–e86. PubMed CrossRef
25. Kornum JB, Thomsen RW, Riis A, et al. Diabetes, glycemic control, and risk of hospitalization with pneumonia: a population-based case-control study. Diabetes Care. 2008;31(8):1541–1545. PubMed CrossRef
26. Lean ME, Pajonk F-G. Patients on atypical antipsychotic drugs: another high-risk group for type 2 diabetes. Diabetes Care. 2003;26(5):1597–1605. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!