Objective: Stress is associated with the onset, maintenance, and recurrence of depression. This study investigated the feasibility of stress management and resiliency training (SMART) for enhancing resiliency in a group of patients with major depressive disorder.
Methods: In an open-label study, patients with major depressive disorder were invited to participate in an adjunctive 8-week group therapy of SMART (from June 2017 to June 2018) that encompassed attention training and practice of gratitude, compassion, higher meaning, acceptance, and forgiveness. The primary outcome measure was baseline-to-endpoint change in resilience as measured by the Connor Davidson Resilience Scale (CD-RISC). Secondary outcome measures included baseline-to-endpoint change in stress using the Perceived Stress Scale (PSS) and in depression using the 17-item Hamilton Depression Rating Scale (HDRS-17) and 9-item Patient Health Questionnaire (PHQ-9).
Results: Twenty-three participants enrolled in the study (mean ± SD age = 46 ± 13 years, female = 91%). Baseline ratings of mood were of mild-to-moderate symptom severity (mean HDRS-17 score = 14.5 and PHQ-9 score = 12), resilience (mean CD-RISC score = 53.8), and perceived stress (mean PSS score = 23.5). Of the participants, 74% were study completers (attended ≥ 6 sessions). In an intention-to-treat analysis, at study endpoint there was a significant improvement in resilience (mean CD-RISC score = 61.1, P = .03), reduction in perceived stress (mean PSS score = 19.4, P = .002), and improvement in depression (mean HDRS-17 score = 9.1 and PHQ-9 score = 7.6, both P < .001).
Conclusions: A resilience training program focused on wellness is feasible for patients who are currently symptomatic with major depressive disorder. A larger randomized controlled trial is needed to establish efficacy of this intervention and explore the long-term impact of stress management and resilience training in depression.
Trial Registration: ClinicalTrials.gov identifier: NCT03275961
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
Feasibility Study of Stress Management and Resiliency Training (SMART) in Patients With Major Depressive Disorder
ABSTRACT
Objective: Stress is associated with the onset, maintenance, and recurrence of depression. This study investigated the feasibility of stress management and resiliency training (SMART) for enhancing resiliency in a group of patients with major depressive disorder.
Methods: In an open-label study, patients with major depressive disorder were invited to participate in an adjunctive 8-week group therapy of SMART (from June 2017 to June 2018) that encompassed attention training and practice of gratitude, compassion, higher meaning, acceptance, and forgiveness. The primary outcome measure was baseline-to-endpoint change in resilience as measured by the Connor Davidson Resilience Scale (CD-RISC). Secondary outcome measures included baseline-to-endpoint change in stress using the Perceived Stress Scale (PSS) and in depression using the 17-item Hamilton Depression Rating Scale (HDRS-17) and 9-item Patient Health Questionnaire (PHQ-9).
Results: Twenty-three participants enrolled in the study (mean ± SD age = 46 ± 13 years, female = 91%). Baseline ratings of mood were of mild-to-moderate symptom severity (mean HDRS-17 score = 14.5 and PHQ-9 score = 12), resilience (mean CD-RISC score = 53.8), and perceived stress (mean PSS score = 23.5). Of the participants, 74% were study completers (attended ≥ 6 sessions). In an intention-to-treat analysis, at study endpoint there was a significant improvement in resilience (mean CD-RISC score = 61.1, P = .03), reduction in perceived stress (mean PSS score = 19.4, P = .002), and improvement in depression (mean HDRS-17 score = 9.1 and PHQ-9 score = 7.6, both P < .001).
Conclusions: A resilience training program focused on wellness is feasible for patients who are currently symptomatic with major depressive disorder. A larger randomized controlled trial is needed to establish efficacy of this intervention and explore the long-term impact of stress management and resilience training in depression.
Trial Registration: ClinicalTrials.gov identifier: NCT03275961
Prim Care Companion CNS Disord 2020;22(3):19m02556
To cite: Seshadri A, Clark MM, Kung S, et al. Feasibility study of stress management and resiliency training (SMART) in patients with major depressive disorder. Prim Care Companion CNS Disord. 2020;22(3):19m02556.
To share: https://doi.org/10.4088/PCC.19m02556
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartments of Psychiatry and Psychology, Mayo Clinic, Rochester, Minnesota
bSchool of Psychology, Deakin University, Geelong, Melbourne, Australia
cDepartment of General Internal Medicine, Mayo Clinic, Rochester, Minnesota
dQueensland Brain Institute, University of Queensland, St Lucia, Queensland, Australia
eGlobal Center for Resiliency and Wellbeing, Rochester, Minnesota
*Corresponding author: Ashok Seshadri, MD, Department of Psychiatry and Psychology, Mayo Clinic, 1000 First Drive NW, Austin, Minnesota 55912 ([email protected]).
A hallmark of major depressive disorder is negative attentional and motivational bias, along with anhedonia, rumination, social isolation, and cognitive inefficiencies. These deficits impair the ability to exercise adequate cognitive reappraisal and behavioral strategies toward effective problem solving.1
The relationship between stress and depression is well established, and chronic accumulating effects of stress are associated with risk of developing major depressive disorder and are also associated with the maintenance and recurrence of depression.2-5 Additionally, depression may generate interpersonal stressful conditions that further exacerbate stress and cause chronic or intermittent depression.6,7
Resilience can be broadly defined as the capacity of an individual to resist negative psychological, biological, and social consequences of stress. Resilience represents an active and dynamic positive adaptive response to stress. The American Psychological Association8 defines resiliency as “the process of adapting well in the face of adversity, trauma, tragedy, threats, or even significant sources of threat.”(p1) Psychosocial factors can influence resilience and include ability to maintain cognitive flexibility and emotional regulation under stress, having previous successful experience of dealing with stress (ie, stress inoculation), presence of strong social support and role models, spirituality, and living with a sense of purpose and meaning.9,10
A meta-analysis10 of efficacy of resiliency training programs, focusing primarily on attention control and cognitive reappraisal, in diverse adult populations and people with chronic medical illnesses showed small to moderate effects for improving resilience (pooled standard mean difference = 0.37; 95% CI, 0.18-0.57; P = .0002), reducing stress, and decreasing depression symptom severity. Outside of this work, there is a paucity of research investigating the therapeutic effects of resilience-targeted interventions, especially as part of a treatment intervention for syndromal major depressive disorder. Therefore, the primary aim of this project was to investigate the feasibility of a stress management and resiliency training (SMART) program in patients with an active depressive disorder. We hypothesized that the intervention would be feasible and acceptable and lead to improved resilience, decreased perceived stress, and improvement in depression in patients receiving treatment for major depressive disorder.
METHODS
Sample Selection
The study protocol was approved by the Mayo Clinic Institutional Review Board. From June 2017 to June 2018, participants between the ages of 18 and 80 years were recruited for this study while they were seeking clinical care from the Mayo Clinic Depression Center, Mayo Clinic Family Medicine Clinics, or Behavioral Health Clinic at Mayo Clinic Health System, Austin, Minnesota. After identification through electronic health record review and obtaining approval to approach them from their psychiatric care primary provider, potential study candidates were contacted for possible participation. Study candidates identified in initial screening had a consultation with the principal investigator (A.S.) to establish clinical diagnosis. The study was registered in ClinicalTrials.gov (identifier: NCT03275961).
Inclusion Criteria
Patients with major depressive disorder confirmed by structured diagnostic interview11 with at least mild, but not severe, symptoms (ie, 9-item Patient Health Questionnaire12 [PHQ-9] score = 6-19, 17-item Hamilton Depression Rating Scale13 [HDRS-17] score = 8-24, or Quick Inventory of Depressive Symptomatology-Clinician Rated14 [QIDS] score = 6-20) and who were able to speak English provided written informed consent to participant in the study. Participants were encouraged to continue taking any prescribed medications from their clinical treatment team. Patients with comorbid secondary diagnoses of persistent depressive disorder and generalized anxiety disorders were included in the study.
Exclusion Criteria
Participants with bipolar disorder, active psychosis, active suicidal ideation, active substance abuse (except nicotine), obsessive-compulsive disorder, active panic disorder with agoraphobia or other phobic disorder, active posttraumatic stress disorder, and severe personality disorders were excluded.
Intervention
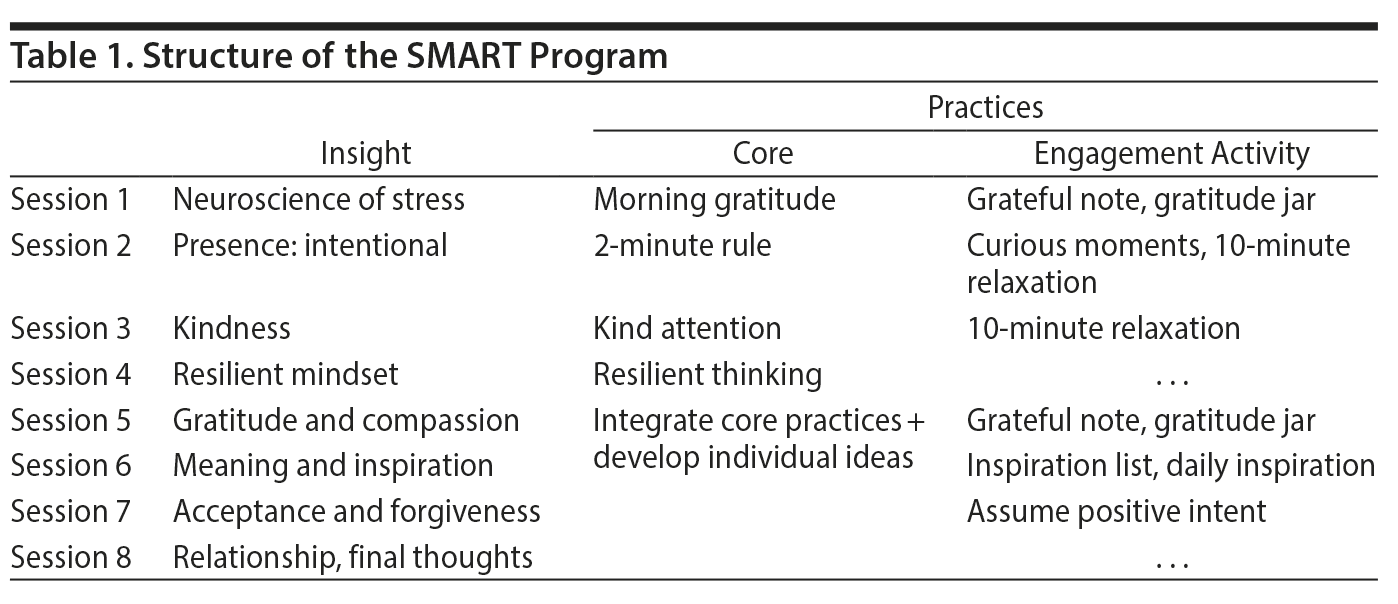
SMART15 is a resiliency training program created at the Mayo Clinic, Rochester, Minnesota. Key components of SMART include identifying emotional signs of stress and recognizing different thinking modes of the brain, such as the default mode and the focused mode. Participants learn attention training and practice finding novelty and using curiosity and kindness to view the physical world and the relationships within them. The cognitive aspects of training include intentional practice of the principles of gratitude, compassion, acceptance, forgiveness, higher meaning, and purpose to interpret and reframe day-to-day life experiences.

- Stress management and resiliency-building strategies may help patients with major depressive disorder.
- Brief intentional practice of attention to novelty and kindness can improve resilience.
- Maintaining a resilient mindset focused on gratitude, compassion, acceptance, meaning, and forgiveness can increase resilience and reduce perceived stress.
The SMART intervention was delivered by a single therapist (A.S.) for all groups (Table 1). Each session was 75-90 minutes, occurring weekly at the same time of the week (Monday afternoon), except on holidays or in the event of inclement weather. The sessions included a brief introduction and review of homework assignments followed by a presentation based on the book Mayo Clinic Guide to Stress Free Living15 and a group discussion of each topic presented. The project investigator (A.S.) developed the content of each presentation with guidance from the creator of SMART. To ensure fidelity of the intervention, the study team selected at random 1 session that was audio recorded to be reviewed by content experts within the research team. Each study intervention group was comprised of 3 to 8 participants. There was no comparison or control group.
Measures
Feasibility. The study aimed to assess feasibility by measuring patient acceptability with the goal of recruiting at least 25% of eligible participants approached and to assess adherence with the goal of 75% completion of the 8-session SMART therapy (attended 6 or more of the 8 sessions) and homework assignments.
Primary and Secondary Outcome Measures. The primary outcome measure was resilience, which was assessed with the Connor-Davidson Resilience Scale (CD-RISC).16 The CD-RISC 25-item scale has good internal consistency (α = .89) and test-retest reliability (intraclass correlation coefficient = 0.87).17 Validity of the CD-RISC was measured using Pearson correlations between resilience (CD-RISC) and perceived stress (Perceived Stress Scale [PSS]18), showing consistent negative correlations (r = −0.49, P = .02 at baseline and r = −0.67, P < .001 at study end) between the 2 constructs.
Secondary outcome measures included measures of perceived stress, depression, and anxiety. Perceived stress was measured using the PSS, a 10-item self-administered scale that measures the degree to which one’s life is appraised as stressful. Scores of 20 or higher are associated with high perceived stress.18 Treatment effectiveness was assessed utilizing the objective ratings of the HDRS-17 and self-reported PHQ-9. Anxiety was measured using the self-reported 7-item Generalized Anxiety Disorder scale (GAD-7).19
Internal consistency in our sample measured using Cronbach α at baseline, week 4, and week 8 was 0.9, 0.95, and 0.95 (CD-RISC); 0.84, 0.84, and 0.86 (PSS); 0.63, 0.58, and 0.84 (HDRS-17); 0.59, 0.85, 0.87 (PHQ-9); and 0.79, 0.78, and 0.8 (GAD-7), respectively.
Measurements were carried out at baseline and weeks 1, 4, 6 (± 1 week), and 8 (± 2 weeks) in person, electronically, or by telephone. All outcome measures were obtained by 2 research coordinators (K.C.D., J.A.R.) who had an interrater reliability of 0.86. They were not blind to study hypotheses.
Statistical Analysis
Statistical analyses were performed using IBM SPSS Statistics for Windows, version 24.0 (IBM Corp, Armonk, New York). Baseline characteristics between study completers versus noncompleters and between remitters versus nonremitters were analyzed using parametric tests for continuous variables and Fisher exact test for categorical variables. Preliminary data analysis revealed that missing data were largely accounted for by 6 participants who dropped out during the study. All remaining participants provided complete data, except in 2 instances wherein 1 (PSS) measure was inadvertently not provided to participants. We used the last observation carried forward as a conservative method to impute missing data. Data were checked for normality of distribution using the Shapiro-Wilk statistic. Heterogeneity of variance was checked using Levene’s test. Both of these tests revealed no significant concerns for nonnormal distribution of data. However, given the small sample, we performed both parametric (student t test) and nonparametric tests (Wilcoxon matched pairs signed-ranks test) to compare before and after intervention values on outcome measures. We report the results for the parametric tests, as both tests provided comparable results.
RESULTS
Baseline Demographic and Clinical Characteristics
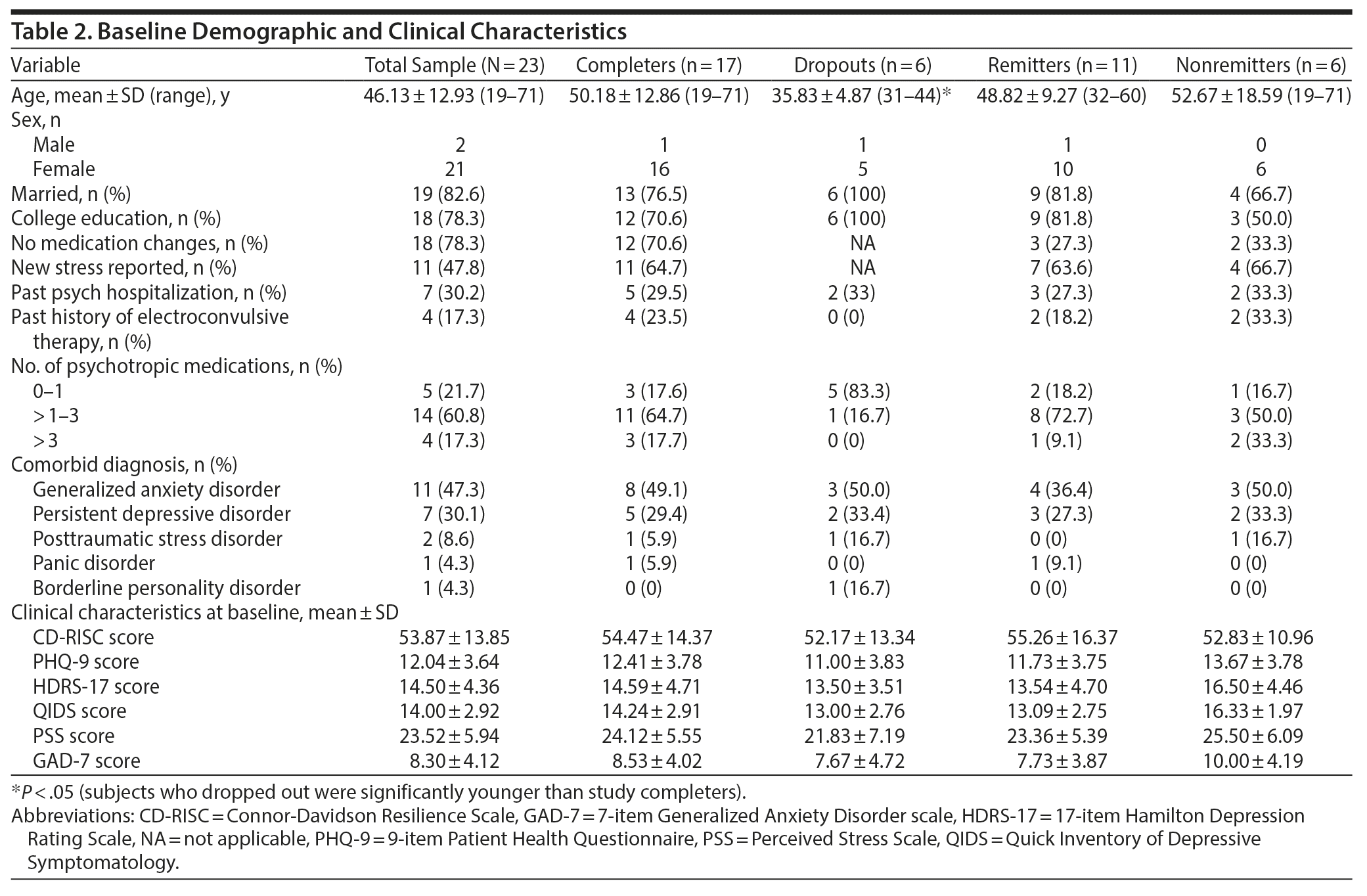
Demographics are presented in Table 2. The majority of study participants were married (82.6%), college educated (78%), employed (74%), and female (91%). Comorbid diagnoses included 11 (47.3%) with generalized anxiety disorder, 7 (30.1%) with persistent depressive disorder, 2 (8.6%) with posttraumatic stress disorder in partial remission, 1 (4.3%) with panic disorder without agoraphobia, and 1 (4.3) with borderline personality disorder. The comorbid diagnoses were not the active focus of clinical treatment at the time of the study.
Baseline clinical characteristics showed that the mean duration of diagnosis of major depressive disorder was 17.22 years (SD = 9.7). Seven participants reported history of previous inpatient hospitalization (38.2%), and 4 participants reported previous history of receiving electroconvulsive therapy (17.3%). Fourteen participants (60.8%) were on 2 to 3 psychotropic medications, while 4 (17.3%) participants were on at least 4 psychotropic medications.
Baseline scores on the resilience measure (CD-RISC) were 53.9 (SD = 13.8), consistent with other studies with outpatient populations with major depressive disorder.16 The overall severity of depression of the study sample was in the mild or moderate range. Baseline scores on perceived stress were 23.52 (SD = 5.9); scores above 20 are considered clinically significant.18
Feasibility
Thirty (58%) of 52 potential study candidates, who were contacted for possible participation, expressed interest in the study, which was significantly greater than the 25% participant acceptability goal defined at the start of the study. Five candidates did not meet study inclusion criteria. Twenty-five candidates met the research criteria, signed research informed consent forms, and were enrolled in the study. Two participants withdrew before attending any treatment sessions due to conflicts with their work schedules and were not included in further analysis.
Seventeen (74%) participants were classified as study completers, defined by attending at least 6 of 8 treatment sessions, comparable to our treatment adherence goal of 75% defined at the start of the study. The reasons for study withdrawal included childbirth (n = 1), move to a different town (n = 1), change of work status (n = 1), “too much going on” (n = 2), and unknown (n = 1). Two participants withdrew after 1 session, 1 after 2 sessions, 1 after 3 sessions, and 2 after 4 sessions. The mean number of sessions attended was 6.17 (SD = 2.33) out of 8 for the total sample. Homework assignment sheets were completed a mean of 5.22/7 (SD = 2.41) times. Five (21.7%) participants reported medication changes during the study. Eleven of the study completers reported the occurrence of new stressors during the course of the study.
Analysis of study completers versus noncompleters showed that noncompleters were significantly younger than the study completers (mean ± SD age of 35.2 ± 4.9 versus 50.1 ± 12.9, P < .05). No other differences in clinical or demographic profiles including medication changes occurred during the study. Comparison between study remitters and study nonremitters (remission defined by HDRS-17 scores ≤ 7 at study end) showed no statistically significant differences, although the numerical values suggested slightly worse depression, anxiety, resilience, and perceived stress scores in the nonremitted participants.
Primary and Secondary Outcome Measures
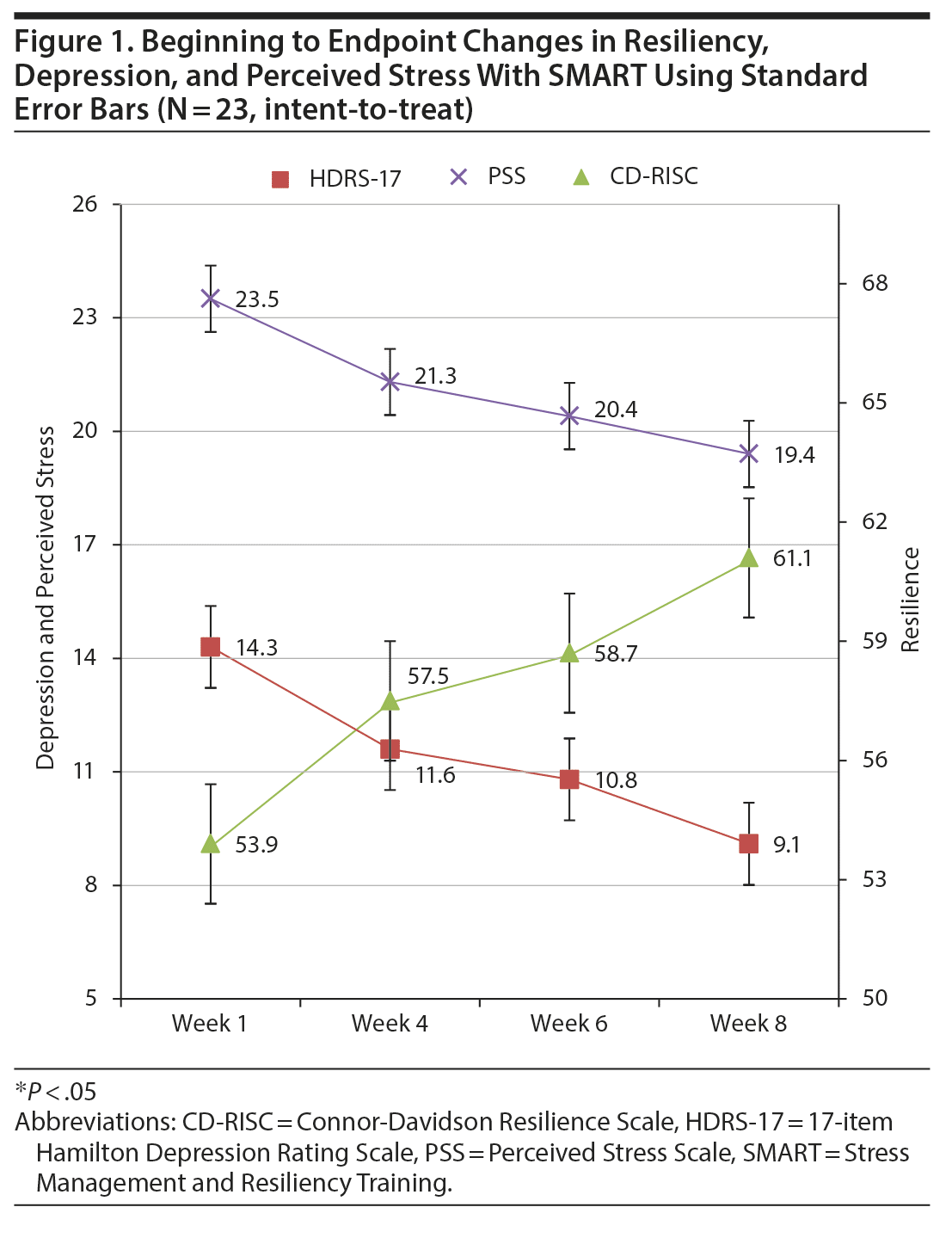
There was a statistically significant change from baseline in the primary outcome (CD-RISC mean score: baseline = 53.9 [SD = 13.8], endpoint/8 weeks = 61.1 [SD = 16.8], t = −2.3, df = 22, P = .03, Cohen d = 0.52). There was a statistically significant change in the secondary outcome measures (PSS mean score: baseline = 23.5 [SD = 5.9], endpoint = 19.4 [SD = 7.0], t = 3.4, df = 22, P = .002, Cohen d = 0.68; HDRS mean score: baseline = 14.3 [SD = 4.4], endpoint = 9.1 [SD = 5.4], t = 4.59, df = 22, P < .001, Cohen d = 1.18; and PHQ-9 mean score: baseline 12.04 [SD = 3.64], endpoint 7.61[SD = 5.5], t = 4.6, df = 22, P < .001, Cohen d = 1.2).
The time course of significant change was first evident in the HDRS-17 (weeks, 4, 6, and 8) followed by the CD-RISC, PSS, and PHQ-9 (weeks 6 and 8) (Figure 1). At baseline, there were significant negative correlations between perceived stress and resilience (r = −0.49, P < .02). At endpoint, there were significant correlations between resilience and perceived stress (r = −0.67, P < .001), resilience and depression (HDRS-17: r = −0.70, P < .001), and perceived stress and depression (HDRS-17: r = 0.65, P = .001) using Bonferroni correction. Participants who met remission criteria for depression at study end had a mean posttreatment CD-RISC score of 70.8 (SD = 13.4) in comparison to nonremitters (mean score of 50.2, SD = 11.6).
Follow-up data were available for 10 of the 17 study completers after therapy completion. PHQ-9 scores were collected through electronic medical record review. The mean PHQ-9 score was 7.1 (SD = 6.8, n = 10) at a mean duration of measurement of 5.5 months compared with a mean PHQ-9 score of 7.1 (SD = 7.1, n = 10) at study end (8 weeks). Six of the 10 participants continued to meet criteria for depression remission based on the criteria of PHQ-9 score ≤ 5.
DISCUSSION
The results of this single-arm pilot study show that a resiliency program (SMART) is feasible in a sample of patients with major depressive disorder. The results indicate that depressed patients who are willing to enroll in a resiliency program can engage and complete the program and achieve demonstrable improvement in resiliency, reduction in perceived stress, and improvement in depressive symptoms. If confirmed with randomized clinical trials using larger and more diverse samples, it is possible that a resiliency intervention could improve long-term depression treatment outcomes.
During the course of the 8-week period, participants demonstrated a gradual improvement in scores of resilience that reached statistical significance at week 6 with further improvement by week 8. We observed that the improvement in resilience scores followed the improvement in objectively rated depression scores (HDRS), which reached statistical significance by week 4. The improvement in subjective ratings for depression (PHQ-9) reached significance at week 6 along with perceived stress. Considering the lack of a control group, we cannot draw any directional conclusions based on these results.
Previous studies16 have shown that CD-RISC scores significantly increase with clinical improvement. We observed that participants who reached depression remission criteria at study end showed a mean 15-point increase in resilience CD-RISC score, representing a nearly 1 standard deviation change from baseline. In contrast, CD-RISC score showed no significant change from baseline in nonresponders. While our follow-up data were limited, they suggested that a majority of participants, who achieved remission at study end (60%), maintained remission at follow-up. This finding leads us to postulate that increase in resilience may have helped sustain depression remission in these participants, but this needs to be confirmed with larger randomized controlled trials.
The SMART program has been found to increase resiliency in stressed but not clinical patient samples.20,21 SMART emphasizes attention training and developing a core mindset to reinterpret life events. The techniques are based on intentional brief daily practices that can be adapted to daily life experiences. In contrast to conventional cognitive-behavioral therapy, the initial target with SMART is not identification of a negative automatic thought to challenge but a feeling of being stressed. Participants are taught to intentionally reframe or reinterpret the situation by using principles of directed attention such as “kind attention” and principles of gratitude (eg, “thankful for what’s right”), compassion (eg, “kindness to self and others”), acceptance (eg, “accept what went wrong while working to make things better”), higher meaning (eg, “what can I learn from this?”), and forgiveness (eg, “I choose to forgive to let go of my anger”).
The emphasis of SMART is on maintaining a resilient mindset using active eudemonic strategies for cognitive reframing and emotional regulation. This approach contrasts with other commonly used passive stress reduction strategies such as exercise, yoga, and relaxation training. In contrast to meditation-based strategies of mindfulness-based therapies, SMART emphasizes brief intentional practices. There are some parallels in the content of SMART with positive psychotherapy as designed by Seligman et al,22 but they differ in emphasis and timing of interventions. SMART emphasizes the focus on developing resilience as the core target with early attention training and cognitive reframing practices. All core concepts are introduced by the fourth week. SMART therapy is also relatively brief with 8 sessions.
With regard to what may have helped participants, opportunities to learn novel cognitive, emotional, and behavioral strategies may have provided a greater sense of control, well-being, and social connectedness. The group therapy setting may have provided opportunities for validation, socialization, and behavioral activation.
Our participants had difficulties in practicing self-kindness and self-compassion. These difficulties appeared to be influenced by negative self-esteem and feelings of guilt. Participants found the topics of acceptance and forgiveness challenging. These challenges may be unique to patients with major depressive disorder with their negative cognitive biases. While the emphasis of the course was to develop resilience-building strategies toward the present and future, participants showed a tendency to focus on the past and engage in rumination. Future studies may need to focus on self-compassion, self-acceptance, self-forgiveness, and anger as part of the coursework of modified SMART for depression.
The strengths of our study were the use of a novel therapeutic approach aimed at increasing resilience to stress as an augmenting strategy in the treatment of major depressive disorder. Participants represented an active clinical sample that was screened thoroughly using clinical and structured diagnostic interviews to establish the diagnosis of major depressive disorder.
Our study had several important limitations. We had a small sample, which increases the possibility of type II error. Additionally, high expectations of participants may have created a participant bias. Outcome assessors and participants were not blind to study hypotheses; hence, this could have created an observer bias and placebo effect, respectively. The sample was predominantly female of higher socioeconomic status, so how these results may apply to underserved populations is unknown. There was no control group, so no causative statement can be made.
CONCLUSIONS
In this pilot evaluation, a novel resiliency intervention, SMART (stress management and resiliency training) was found feasible in terms of patient acceptability and treatment adherence as part of a comprehensive treatment program for patients with major depressive disorder. The findings show promise in improving resiliency, perceived stress, and depression, but a larger adequately powered controlled study is required to assess treatment efficacy more accurately. It is also possible that there are some unique features of depression that will require modifications of the SMART program to tailor it to clinical needs during a depressive episode.
Submitted: October 17, 2019; accepted January 17, 2020.
Published online: April 30, 2020.
Potential conflicts of interest: Dr Clark has received consultant fees from Roche Diabetes Care GmbH. Dr Sood is the owner of Global Center for Resiliency and Wellbeing and the GRIT Institute. Dr Frye has received grant support from Assurex Health, Mayo Foundation, and Medibio; has received consultant fees from Actify Neurotherapies, Allergan, Intra-Cellular Therapies Inc, Janssen, Myriad, Neuralstem Inc, Takeda, and Teva; and has received fees for CME, travel, and honoraria from American Physician Institute, CME Outfitters, and Global Academy for Medical Education. Drs Seshadri, Kung, Fuller-Tyszkiewicz, Tye, and McGillivray; Ms Dammen; and Mr Rico report no conflicts of interest related to the subject of this article.
Funding/support: None.
Previous presentation: Presented in part at the Annual Meeting of the National Network of Depression Centers; Baltimore, MD; October 18, 2019.
REFERENCES
1.Chamberlain SR, Sahakian BJ. The neuropsychology of mood disorders. Curr Psychiatry Rep. 2006;8(6):458-463. PubMed CrossRef
2.Brown GW, Harris TO. Social Origins of Depression. New York, NY: The Free Press; 1978.
3.Kendler KS, Karkowski LM, Prescott CA. Causal relationship between stressful life events and the onset of major depression. Am J Psychiatry. 1999;156(6):837-841. PubMed CrossRef
4.Kessler RC. The effects of stressful life events on depression. Annu Rev Psychol. 1997;48(1):191-214. PubMed CrossRef
5.Monroe SM, Roberts JE, Kupfer DJ, et al. Life stress and treatment course of recurrent depression, II: postrecovery associations with attrition, symptom course, and recurrence over 3 years. J Abnorm Psychol. 1996;105(3):313-328. PubMed CrossRef
6.Hammen C. Generation of stress in the course of unipolar depression. J Abnorm Psychol. 1991;100(4):555-561. PubMed CrossRef
7.Hammen C. Interpersonal stress and depression in women. J Affect Disord. 2003;74(1):49-57. PubMed CrossRef
8.American Psychological Association. The Road to Resilience. Washington, DC: American Psychological Association; 2010.
9.Southwick SM, Charney DS. The science of resilience: implications for the prevention and treatment of depression. Science. 2012;338(6103):79-82. PubMed CrossRef
10.Leppin AL, Bora PR, Tilburt JC, et al. The efficacy of resiliency training programs: a systematic review and meta-analysis of randomized trials. PLoS One. 2014;9(10):e111420. PubMed CrossRef
11.First MB, Williams JBW, Karg RS, et al. Structured Clinical Interview for DSM-5—Research Version (SCID-5-RV). Arlington, VA: American Psychiatric Association; 2015.
12.Kroenke K, Spitzer RL. The PHQ-9: a new depression diagnostic and severity measure. Psychiatr Ann. 2002;32(9):509-515. CrossRef
13.Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. PubMed CrossRef
14.Rush AJ, Trivedi MH, Ibrahim HM, et al. The 16-Item Quick Inventory of Depressive Symptomatology (QIDS), clinician rating (QIDS-C), and self-report (QIDS-SR): a psychometric evaluation in patients with chronic major depression. Biol Psychiatry. 2003;54(5):573-583. PubMed CrossRef
15.Sood A. The Mayo Clinic Guide to Stress-Free Living. Boston, MA: Da Capo Press; 2013.
16.Connor KM, Davidson JR. Development of a new resilience scale: the Connor-Davidson Resilience Scale (CD-RISC). Depress Anxiety. 2003;18(2):76-82. PubMed CrossRef
17.Campbell-Sills L, Stein MB. Psychometric analysis and refinement of the Connor-Davidson Resilience Scale (CD-RISC): validation of a 10-item measure of resilience. J Trauma Stress. 2007;20(6):1019-1028. PubMed CrossRef
18.Cohen S, Kamarck T, Mermelstein R. A global measure of perceived stress. J Health Soc Behav. 1983;24(4):385-396. PubMed CrossRef
19.Spitzer RL, Kroenke K, Williams JB, et al. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092-1097. PubMed CrossRef
20.Loprinzi CE, Prasad K, Schroeder DR, et al. Stress Management and Resilience Training (SMART) program to decrease stress and enhance resilience among breast cancer survivors: a pilot randomized clinical trial. Clin Breast Cancer. 2011;11(6):364-368. PubMed CrossRef
21.Werneburg BL, Jenkins SM, Friend JL, et al. Improving resiliency in healthcare employees. Am J Health Behav. 2018;42(1):39-50. PubMed CrossRef
22.Seligman MEP, Rashid T, Parks AC. Positive psychotherapy. Am Psychol. 2006;61(8):774-788. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!