Background: Evidence has shown a significant association between bipolar disorder and prevalence of risky sexual behaviors. However, the relationship between bipolar disorder and risk for sexually transmitted infections (STIs) requires further investigation, as do the effects of bipolar disorder medications on STI risk.
Methods: In the present study, data from 26,028 adolescents and young adults with bipolar disorder (ICD-9-CM code 296 except 296.2x, 296.3x, 296.9x, and 296.82) and 104,112 age- and sex-matched non-bipolar-disorder controls from 2001 to 2009 were selected from the Taiwan National Health Insurance Research Database. Patients who contracted any type of STI—including human immunodeficiency virus, syphilis, genital warts, gonorrhea, chlamydial infection, and trichomoniasis—during the follow-up period (from enrollment to the end of 2011) were identified.
Results: Cox regression analysis with full adjustment for demographic data, psychiatric comorbidities, and bipolar disorder medications showed that bipolar disorder was an independent risk factor (hazard ratio [HR] = 4.11; 95% confidence interval [CI], 3.62-4.66) for contracting an STI. Patients with bipolar disorder and substance and/or alcohol use disorders were at highest risk of STI occurrence. Long-term use of mood stabilizers (HR = 0.54; 95% CI, 0.34-0.86) and atypical antipsychotics (HR = 0.82; 95% CI, 0.71-0.95) was associated with reduced risk for contracting STIs.
Conclusions: Adolescents and young adults with bipolar disorder exhibited an increased risk of subsequent STI during the follow-up period compared with those without bipolar disorder. Comorbidity of substance and alcohol use disorders further increased this risk. Long-term use of bipolar disorder medications (mood stabilizers and atypical antipsychotics) may reduce this risk.
‘ ‹
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation. A $10 processing fee will apply.
CME Objective
After studying this article, you should be able to:
- Assess and address sexual risks in adolescent and young adult patients with bipolar disorder
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1 hour of Category I credit for completing this program.
Release, Expiration, and Review Dates
This educational activity was published in March 2019 and is eligible for AMA PRA Category 1 Credit™ through April 30, 2021. The latest review of this material was February 2019.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Marlene P. Freeman, MD, Editor in Chief, has received research funding from JayMac and Sage; has been a member of the advisory boards for Otsuka, Alkermes, and Sunovion; has been a member of the Independent Data Safety and Monitoring Committee for Janssen; and, as a Massachusetts General Hospital (MGH) employee, works with the MGH National Pregnancy Registry, which is sponsored by Teva, Alkermes, Otsuka, Actavis, and Sunovion, and works with the MGH Clinical Trials Network and Institute, which receives research funding from multiple pharmaceutical companies and the National Institute of Mental Health. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
ABSTRACT
Background: Evidence has shown a significant association between bipolar disorder and prevalence of risky sexual behaviors. However, the relationship between bipolar disorder and risk for sexually transmitted infections (STIs) requires further investigation, as do the effects of bipolar disorder medications on STI risk.
Methods: In the present study, data from 26,028 adolescents and young adults with bipolar disorder (ICD-9-CM code 296 except 296.2x, 296.3x, 296.9x, and 296.82) and 104,112 age- and sex-matched non-bipolar-disorder controls from 2001 to 2009 were selected from the Taiwan National Health Insurance Research Database. Patients who contracted any type of STI—including human immunodeficiency virus, syphilis, genital warts, gonorrhea, chlamydial infection, and trichomoniasis—during the follow-up period (from enrollment to the end of 2011) were identified.
Results: Cox regression analysis with full adjustment for demographic data, psychiatric comorbidities, and bipolar disorder medications showed that bipolar disorder was an independent risk factor (hazard ratio [HR] = 4.11; 95% confidence interval [CI], 3.62-4.66) for contracting an STI. Patients with bipolar disorder and substance and/or alcohol use disorders were at highest risk of STI occurrence. Long-term use of mood stabilizers (HR = 0.54; 95% CI, 0.34-0.86) and atypical antipsychotics (HR = 0.82; 95% CI, 0.71-0.95) was associated with reduced risk for contracting STIs.
Conclusions: Adolescents and young adults with bipolar disorder exhibited an increased risk of subsequent STI during the follow-up period compared with those without bipolar disorder. Comorbidity of substance and alcohol use disorders further increased this risk. Long-term use of bipolar disorder medications (mood stabilizers and atypical antipsychotics) may reduce this risk.
J Clin Psychiatry 2019;80(2):18m12199
To cite: Chen MH, Wei HT, Bai YM, et al. Sexually transmitted infection among adolescents and young adults with bipolar disorder: a nationwide longitudinal study. J Clin Psychiatry. 2019;80(2):18m12199.
To share: https://doi.org/10.4088/JCP.18m12199
© Copyright 2019 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Taipei Veterans General Hospital, Taipei, Taiwan
bDepartment of Psychiatry, College of Medicine, National Yang-Ming University, Taipei, Taiwan
cBranch of Linsen, Chinese Medicine, and Kunming, Taipei City Hospital, Tapiei, Taiwan
dDepartment of Nursing, College of Medicine, National Cheng Kung University and Hospital, Tainan, Taiwan
eDepartment of Psychiatry, Cheng Hsin General Hospital, Taipei, Taiwan
fDepartment of Family Medicine, Taipei Veterans General Hospital, Taipei, Taiwan
gInstitute of Hospital and Health Care Administration, National Yang-Ming University, Taipei, Taiwan
‡Contributed equally.
*Corresponding author: Ju-Wei Hsu, MD, Department of Psychiatry, No. 201, Shih-Pai Rd, Sec. 2, 11217, Taipei, Taiwan ([email protected]).
Bipolar disorder is a recurrent, chronic, and severe psychiatric disorder characterized by alternating episodes of mania or hypomania and depression. A leading cause of disability, particularly among young people, bipolar disorder accounts for approximately 7% of the disability-adjusted life-years caused by mental and substance use disorders.1 Bipolar disorder is also associated with cognitive and functional impairment and increased mortality, particularly as a result of suicide.2-4 Bipolar disorder affects more than 2% of the world’s population regardless of nationality, ethnicity, and socioeconomic status.2-4 In Taiwan, bipolar disorder may be undertreated: one study5 reported that the treated prevalence of bipolar disorder in Taiwan is only 4.51/1,000.
Evidence has shown an association between bipolar disorder and health-risk behaviors, including risky sexual behaviors, and between bipolar disorder and risk of contracting sexually transmitted infections (STIs), such as human immunodeficiency virus (HIV).6-12 Hariri et al7 investigated risky sexual behaviors displayed by psychiatric outpatients with bipolar disorder and found that these patients were more likely than healthy controls to engage in risky sexual behaviors, including unprotected sex, sex trading, sexual acts with intravenous drug users, group-sex activities, and sexual activities under the influence of alcohol or other substances. Hariri et al7 also determined that patients with bipolar disorder were more likely to contract STIs. Marengo et al8 further reported that euthymic patients with bipolar disorder had casual partners, engaged in nonmonogamous sexual partnerships, and had sex with partners with unknown HIV statuses more frequently than did healthy controls. In another study, de Sousa Gurgel et al6 found that the prevalence of bipolar I disorder among patients with HIV was 5.6% and was therefore almost 6 times higher than prevalence of bipolar I disorder in the US general population. Meade et al9 reported that patients with bipolar disorder and HIV were more likely than controls to report unprotected sex and to report less than 95% adherence to antiretroviral medications. These studies were limited by their small sample sizes and lack of investigation of the effects of bipolar disorder medications on STI risk. Additionally, these studies employed cross-sectional rather than longitudinal study designs; therefore, they could not clarify the temporal association between bipolar disorder and STIs.
In our study, we analyzed a large sample size of data from the Taiwan National Health Insurance Research Database (NHIRD) and employed a longitudinal study design to investigate the risk of developing STIs—including HIV, syphilis, genital warts, gonorrhea, chlamydial infection, and trichomoniasis—in adolescents and young adults with bipolar disorder. We hypothesized that both adolescents and young adults with bipolar disorder are more likely to contract an STI compared with non-bipolar disorder controls. We further hypothesized that bipolar disorder medications, such as mood stabilizers and atypical antipsychotics, may reduce STI risk for these patients.
METHODS
Data Source
We used data from the NHIRD (https://nhird.nhri.org.tw/), which contains health care data from greater than 99% of Taiwan’s population and is audited and released by the National Health Research Institute for research purposes. The database includes comprehensive information on insured individuals such as demographic data, dates of clinical visits, disease diagnoses, and medical interventions. Individual medical records included in the NHIRD are anonymous to protect patient privacy. The NHIRD has been used in numerous epidemiologic studies in Taiwan.13-16 The diagnostic codes used in the present study are based on the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM). Taipei Veterans General Hospital institutional review board approved this study.

- Adolescents and young adults with bipolar disorder are more likely to contract sexually transmitted infections (STIs) than those without bipolar disorder.
- Patients with bipolar disorder and alcohol and/or substance use disorders were shown to be at especially high risk for STIs.
- Regular medication intervention for bipolar disorder may reduce STI risk.
Inclusion Criteria for Adolescents and Young Adults With Bipolar Disorder and for the Control Group
Adolescents aged between 12 and 17 years and young adults aged between 18 and 29 years who were diagnosed with bipolar disorder (ICD-9-CM code 296 except 296.2x, 296.3x, 296.9x, and 296.82) by board-certificated psychiatrists between January 1, 2001, and December 31, 2009, and who had no history of STIs, including HIV, syphilis, genital warts, gonorrhea, chlamydial infection, and trichomoniasis, before enrollment were included in the bipolar disorder cohort. The time of enrollment was defined as the time of bipolar disorder diagnosis. Members of the age-, sex-, and time-of-enrollment-matched (1:4) control cohort were randomly selected after eliminating the study cases, individuals who had been given a diagnosis of bipolar disorder at any time, and individuals with any type of STI before the enrollment. Diagnoses of STIs—including HIV, syphilis, genital warts, gonorrhea, chlamydial infection, and trichomoniasis—were identified during the follow-up period (from enrollment to December 31, 2011, or until death). In our study, the exclusion of individuals with a prior history of STIs was because we would focus on the temporal association between bipolar disorder and any new-onset STI. Psychiatric comorbidities—including attention-deficit/hyperactivity disorder (ADHD), disruptive behavior disorders, alcohol use disorders, and substance use disorders—were assessed as confounding factors in our study. Increasing evidence suggested the relationship of ADHD, disruptive behavior disorders, alcohol use disorders, and substance use disorders with bipolar disorder and STIs.17 The use of bipolar disorder medications (mood stabilizers and atypical antipsychotics) during the follow-up was also examined, and the study cohort was divided into 3 subgroups: nonusers (cumulative defined daily dose [cDDD] during the follow-up < 30), short-term users (cDDD = 30-364), and long-term users (cDDD ≥ 365). The DDD recommended by the World Health Organization is a unit for measuring a prescribed amount of drug (see https://www.whocc.no/atc_ddd_index/ for details). The DDD is the assumed average maintenance dose per day of a drug consumed for its main indication. We calculated the sum of the dispensed DDD (cDDD) of all bipolar disorder medications during the follow-up period. In this 10-year follow-up longitudinal study, cDDD < 30 was very small, so it was determined as the non-use of medications.18 Mood stabilizers included lithium and anticonvulsants (carbamazepine, oxcarbazepine, valproate, lamotrigine, topiramate, and gabapentin), and atypical antipsychotics included aripiprazole, risperidone, paliperidone, olanzapine, amisulpride, ziprasidone, clozapine, and quetiapine. The urbanization levels of patients’ residences (level 1 to level 5; level 1: most urbanized; level 5: least urbanized) were also assessed in our study.19
Statistical Analysis
In intergroup comparisons, the F test was used for continuous variables and Pearson’s χ2 test for nominal variables, when appropriate. Cox regression analyses with adjustment for demographic data (age, sex, income, level of urbanization), psychiatric comorbidities, and bipolar disorder medications were performed to calculate the hazard ratio (HR) with a 95% confidence interval (CI) for STIs among adolescents and young adults with bipolar disorder and for the control group. The risks of specific STIs for patients with bipolar disorder were further analyzed. Subanalyses stratified by age group (adolescents and young adults) were also conducted to further assess the relationship between bipolar disorder and STI risk. Sensitivity analyses were performed to investigate the association between bipolar disorder and STI contraction after excluding the first year or first 3 years of observation, which reduced the potential bias caused by the delayed diagnosis of STIs after the diagnosis of bipolar disorder. The specific effects of mood stabilizers and atypical antipsychotics on STI risk were investigated separately. A 2-tailed P value of less than .001 was considered statistically significant. All data processing and statistical analyses were performed using SPSS version 17 software (SPSS Inc.) and SAS version 9.1 (SAS Institute, Cary, North Carolina).
RESULTS
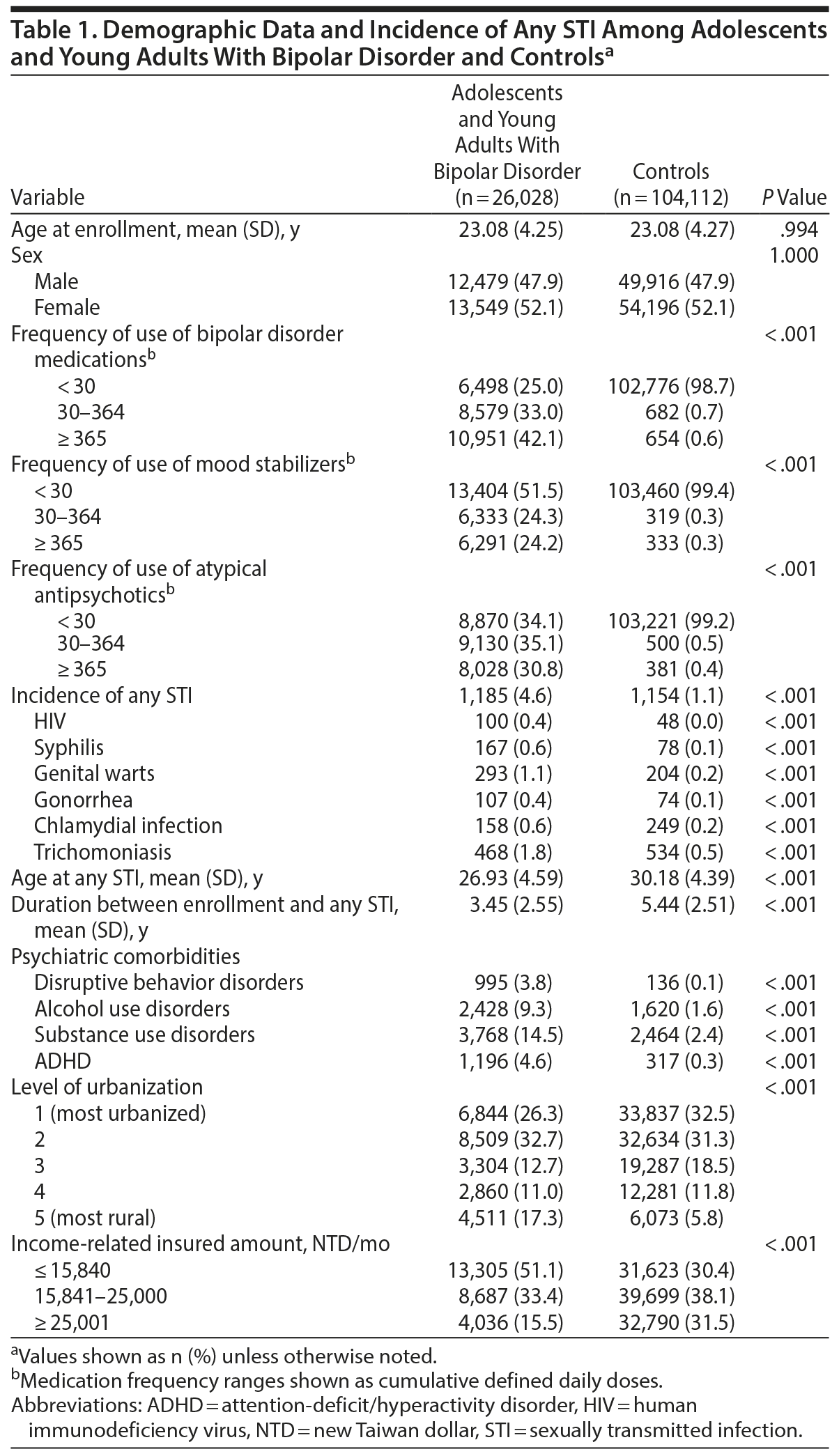
In total, 26,028 adolescents and young adults with bipolar disorder and 104,112 age- and sex-matched non-bipolar disorder controls were enrolled in the present study. The mean age of enrollees was 23.08 years, and the cohort contained more female patients than male patients (52.1% vs 47.9%). The patients with bipolar disorder also tended to reside in less urbanized regions (P < .001) and have lower income (P < .001) than the non-bipolar disorder controls (Table 1).
During follow-up, adolescents and young adults with bipolar disorder contracted STIs at an earlier age (mean ± SD = 26.93 ± 4.59 years vs 30.18 ± 4.39 years, P < .001) and at a higher incidence (4.6% vs 1.1%, P < .001) than the controls did (Table 1). In addition, the bipolar disorder group exhibited a higher prevalence of psychiatric comorbidities, including ADHD (4.6% vs 0.3%, P < .001), disruptive behavior disorders (3.8% vs 0.1%, P < .001), alcohol use disorders (9.3% vs 1.6%, P < .001), and substance use disorders (14.5% vs 2.4%, P < .001), compared with the non-bipolar disorder controls (Table 1).
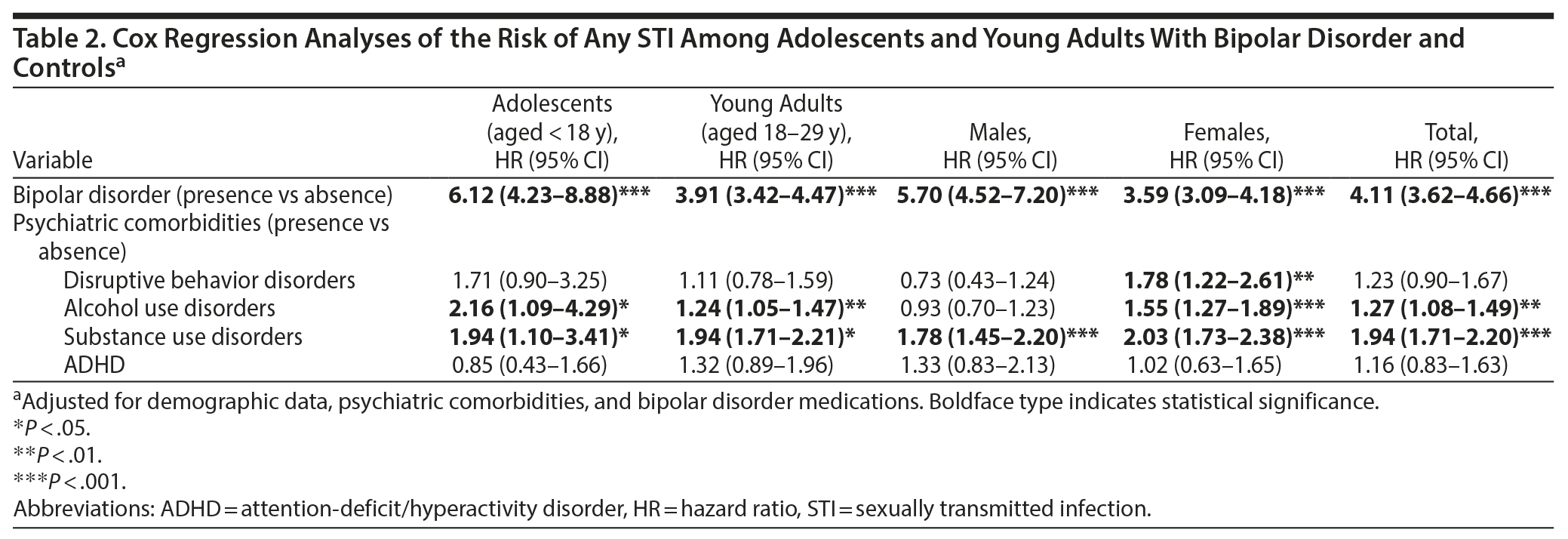
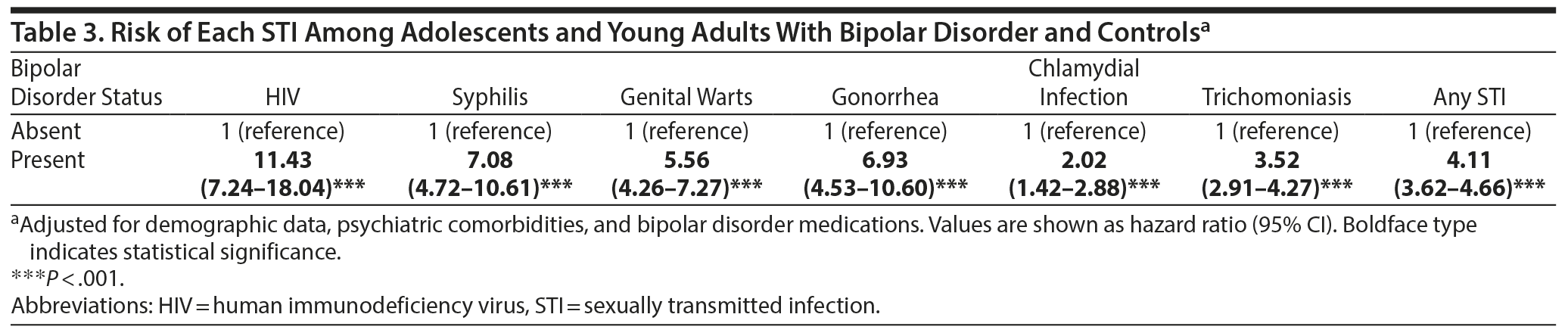
Kaplan-Meier survival analysis with the log rank test revealed a significant association between bipolar disorder and STI risk (P < .001). Cox regression analyses with adjustment for demographic data (age, sex, income, and level of urbanization), psychiatric comorbidities (ADHD, disruptive behavior disorder, and substance and alcohol use disorders), and bipolar disorder medications (mood stabilizers and atypical antipsychotics) showed that adolescents (HR = 6.12; 95% CI, 4.23-8.88), young adults (HR = 3.91; 95% CI, 3.42-4.47), and both males (HR = 5.70; 95% CI, 4.52-7.20) and females (HR = 3.59; 95% CI, 3.09-4.18) with bipolar disorder were more likely to contract an STI than were the non-bipolar disorder controls (Table 2). The relationships between bipolar disorder and risk of each STI were statistically significant (all P < .001), with the highest risk (HR = 11.43; 95% CI, 7.24-18.04) for HIV and the lowest risk (HR = 2.02; 95% CI, 1.42-2.88) for chlamydial infection (Table 3). Substance use disorders (HR = 1.94; 95% CI, 1.71-2.20) and alcohol use disorders (HR = 1.27; 95% CI, 1.08-1.49) were associated with risk of subsequent STI contraction (Table 2).
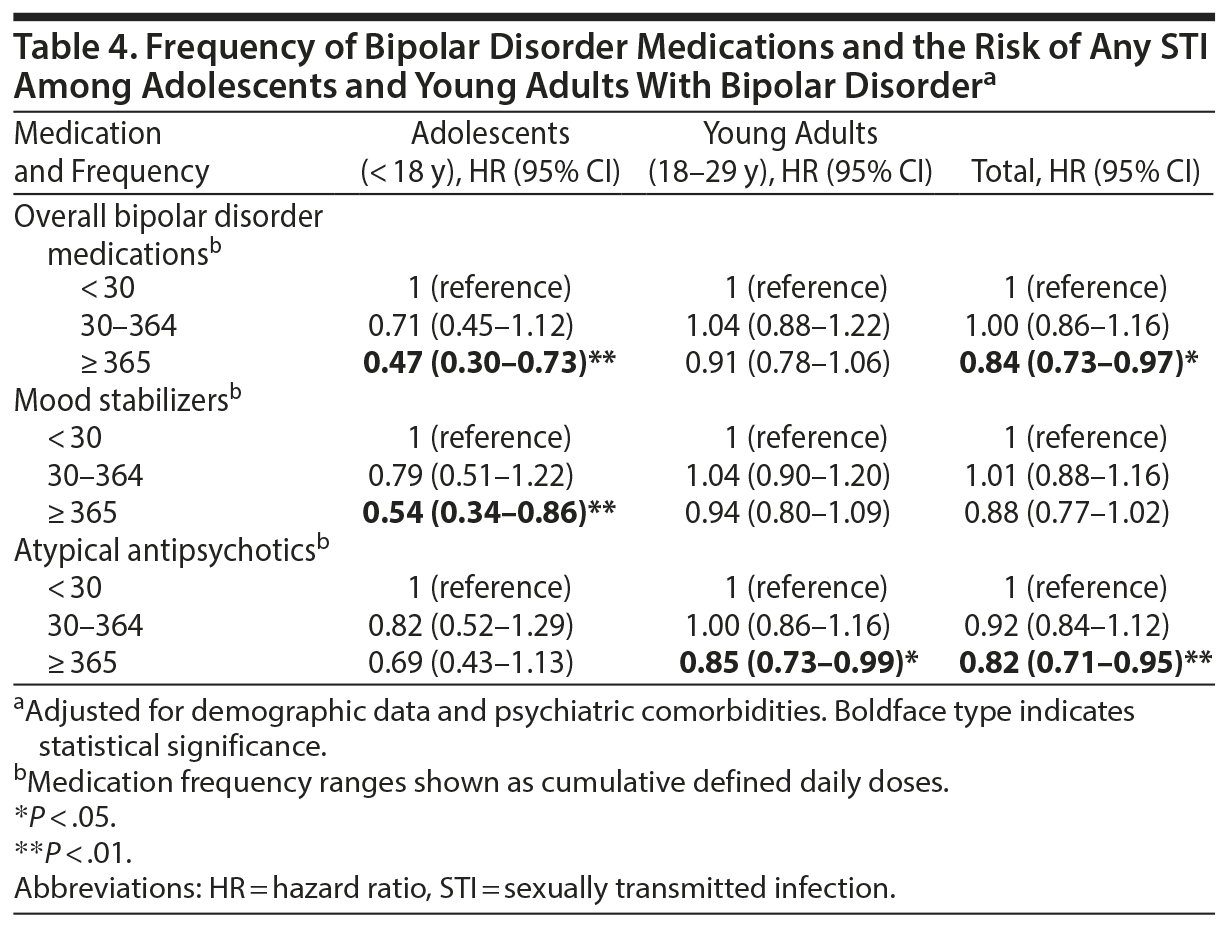
In addition, the long-term users of bipolar disorder medications (HR = 0.84; 95% CI, 0.73-0.97) were discovered to have a significantly lower risk of contracting any STI during follow-up (Table 4). Among adolescent patients with bipolar disorder, the use of mood stabilizers was associated with reduced risk (HR = 0.54; 95% CI, 0.34-0.86) of STI contraction, and among young adult patients with bipolar disorder, the use of atypical antipsychotics was related to a lower likelihood (HR = 0.85; 95% CI, 0.73-0.99) of STI contraction (Table 4). Sensitivity analyses performed after excluding the first year (HR = 3.56; 95% CI, 3.11-4.09) and the first 3 years (HR = 2.75; 95% CI, 2.32-3.26) of observation, respectively, showed findings consistent with the main findings (Table 5).
DISCUSSION
Our results supported the study hypotheses that adolescents and young adults with bipolar disorder are more likely to contract STIs including HIV, syphilis, genital warts, gonorrhea, chlamydial infection, and trichomoniasis compared with the control group. The patients with bipolar disorder and substance and/or alcohol use disorders were discovered to be at the highest risk for STIs. Long-term use of bipolar disorder medications, including mood stabilizers and atypical antipsychotics, was associated with reduced risk of STI occurrence.
As mentioned in the Introduction, clinical studies have suggested a significant association between bipolar disorder and risk of STIs.6,7 Manic, depressive, and euthymic states of bipolar disorder have all been associated with STI risk.8,20,21 A 15-month prospective study21 examined affective symptoms associated with risky sexual behavior among 61 patients with bipolar disorder and discovered that a higher average number of weeks of mania, but not depression, was associated with increased sexual risk-taking. Hutton et al20 assessed the relationship between HIV-related risk behaviors and depression among 671 STI clinic patients and demonstrated that patients with depression were more likely than those without to have had sex for money or drugs, to have had sex with an intravenous drug user, to have had sex when “high” on alcohol or drugs, to have had a greater number of sexual partners over their lifetimes, and to abuse alcohol or drugs. In addition, Marengo et al8 demonstrated that euthymic patients with bipolar disorder were in nonmonogamous sexual partnerships and had sex with partners with unknown HIV statuses more frequently than did controls. In our study, database limitations prevented us from clarifying which affective state of bipolar disorder was most predictive of STI risk. However, after adjusting for comorbid substance and/or alcohol use disorders, we were able to determine that, among the patients in our study cohort, bipolar disorder was an independent risk factor for STI contraction. Our results also suggested that patients with bipolar disorder and substance and/or alcohol use disorders were at the highest risk of contracting STIs. In addition, we found that long-term use of mood stabilizers and atypical antipsychotics may reduce the risk of contracting STIs.
Several underlying mechanisms may explain the association between bipolar disorder and STI risk, as well as the protective effects of bipolar disorder medications against STI risk. First, hypersexuality and goal-directed risky behaviors in manic states, as well as impulsivity in manic and depressive states, have been shown to be associated with risky sexual behaviors, thus contributing to STI risk among patients with bipolar disorder.20-22 One study23 also demonstrated that the antimanic and anti-impulsivity effects of mood stabilizers and atypical antipsychotics reduced the prevalence of mania- and impulsivity-related risky behaviors, such as violence. Our study found that long-term use of mood stabilizers was related to lower STI risk among adolescents with bipolar disorder, but also that among young adults with bipolar disorder, long-term use of atypical antipsychotics was associated with reduced STI risk. No studies have investigated the protective effects of mood stabilizers and atypical antipsychotics against risky behaviors in adolescent versus adult patients with bipolar disorder. Furthermore, fewer adolescents (n = 911, 25.5%) with bipolar disorder had long-term treatment with atypical antipsychotics, which may reduce the statistical power needed to detect the protective effects of atypical antipsychotics against STI risk among the adolescent group. Further clinical studies would be required to clarify this issue. Second, psychiatric comorbidities of bipolar disorder, such as substance use disorders and alcohol use disorders, have been shown to be significantly associated with risk of STIs,7,11,21,24 and these associations are further supported by our findings. Studies25-27 have suggested that both manic and depressive episodes may exacerbate substance and/or alcohol abuse, and vice versa, increasing mental and physical risks for patients with bipolar disorder. In our study, after adjustment for comorbid substance and alcohol use disorders, bipolar disorder was still found to be an independent risk factor for STIs. The maintenance of the euthymic state through use of mood stabilizers and atypical antipsychotics may reduce STI risk. Third, cognitive dysfunction resulting from bipolar disorder may increase the prevalence of health-related risky behaviors, including risky sexual behaviors.28-30 Cognitive impairment, including deficits in decision making and impulse control, has been commonly observed in patients in active and remitted states of bipolar disorder and may explain why manic, depressive, and euthymic states of bipolar disorder have all been shown to be related to risk of STI contraction.31,32 As previously mentioned, the anti-impulsivity and cognitive enhancement effects of mood stabilizers and atypical antipsychotics in patients with bipolar disorder may contribute to a reduction in the prevalence of risky behaviors, including risky sexual behaviors.
The present study had several limitations. First, the incidence of STIs may have been underestimated because only those individuals who seek medical help and consultation are identified in the NHIRD as having STIs. However, STI diagnoses in the NHIRD are assigned by board-certificated physicians and thus have diagnostic validity. Second, we could not identify what health-related risky behaviors may have led to increased risk for STIs in current study. This should be examined in a subsequent study as it could inform clinical practice. Third, the NHIRD does not provide information on the severity of bipolar disorder symptoms; therefore, we could not investigate the association between bipolar disorder severity and risk of STIs. Additional clinical studies are required to elucidate this association. Fourth, the opposite relationship between STIs and subsequent bipolar disorder was not assessed in our study. A review study reported that the higher rate of mania was noted with progression of HIV infection.33 However, STI-related bipolar disorder was not the primary bipolar disorder. Whether STIs would increase the risk of subsequent bipolar disorder needs further investigation. Fifth, the NHIRD does not provide information on psychosocial stresses, family history, personal lifestyles, or environmental factors; therefore, we were unable to investigate the potential influence of related factors on the study results.
In conclusion, adolescents and young adults with bipolar disorder are more likely to contract STIs than those without bipolar disorder. In the present study, after adjustment for demographic factors, psychiatric comorbidities, and use of bipolar disorder medications, we discovered that bipolar disorder was an independent risk factor for STIs. Moreover, patients with bipolar disorder and alcohol and/or substance use disorders were shown to be at especially high risk for STIs. In addition, long-term use of bipolar disorder medications—mood stabilizers and atypical antipsychotics—was shown to reduce risk for STIs. Given the increased risk for STIs, it appears that this should be a topic of frequent discussion in treatment with adolescents and young adults with bipolar disorder, and risky sexual behaviors should be regularly assessed and addressed as a focus of treatment with this population, especially when the patient is also abusing alcohol or other substances. We recommend that clinical psychiatrists focus on helping patients with bipolar disorder reduce their frequency of risky sexual behaviors and related risk for STIs. Our study shows that prompt and regular medication intervention for bipolar disorder may reduce STI risk.
Submitted: February 20, 2018; accepted September 24, 2018.
Published online: March 12, 2019.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, carbamazepine, oxcarbazepine, topiramate, gabapentin, paliperidone, and clozapine are not approved by the US Food and Drug Administration for the treatment of bipolar disorder, and amisulpride is not approved by the US Food and Drug Administration.
Author contributions: Drs M.-H. Chen, Wei, Hsu and Bai designed the study and wrote the protocol and manuscripts; Drs Su, Ko, Li, Tsai, Huang, and Lin assisted with the preparation and proofreading of the manuscript; and Drs Bai, T.-J. Chen, and M.-H. Chen provided advice on statistical analysis.
Financial disclosure: Drs M.-H. Chen, Wei, Bai, Huang, Ko, Su, Li, Lin, Tsai, T.-J. Chen, and Hsu have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: The study was supported by grants from Taipei Veterans General Hospital (V103E10-001, V104E10-002, V105E10-001-MY2-1, V105A-049, V106B-020, V107B-010, and V107C-181) and Ministry of Science and Technology, Taiwan (107-2314-B-075-063-MY3).
Role of the sponsor: The funding sources had no role in any process of this study.
Acknowledgments: The authors thank Mr I-Fan Hu, MA (Courtauld Institute of Art, University of London; National Taiwan University) for his friendship and support in English editing. Mr Hu has no conflicts of interest relevant to the subject of this article.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Whiteford HA, Degenhardt L, Rehm J, et al. Global burden of disease attributable to mental and substance use disorders: findings from the Global Burden of Disease Study 2010. Lancet. 2013;382(9904):1575-1586. PubMed CrossRef
2. Blanco C, Compton WM, Saha TD, et al. Epidemiology of DSM-5 bipolar I disorder: results from the National Epidemiologic Survey on Alcohol and Related Conditions-III. J Psychiatr Res. 2017;84:310-317. PubMed CrossRef
3. Grande I, Berk M, Birmaher B, et al. Bipolar disorder. Lancet. 2016;387(10027):1561-1572. PubMed CrossRef
4. Müller-Oerlinghausen B, Berghöfer A, Bauer M. Bipolar disorder. Lancet. 2002;359(9302):241-247. PubMed CrossRef
5. Bih SH, Chien IC, Chou YJ, et al. The treated prevalence and incidence of bipolar disorder among national health insurance enrollees in Taiwan, 1996-2003. Soc Psychiatry Psychiatr Epidemiol. 2008;43(11):860-865. PubMed CrossRef
6. de Sousa Gurgel W, da Silva Carneiro AH, Barreto Rebouças D, et al; Affective Disorders Study Group (GETA). Prevalence of bipolar disorder in a HIV-infected outpatient population. AIDS Care. 2013;25(12):1499-1503. PubMed CrossRef
7. Hariri AG, Karadag F, Gokalp P, et al. Risky sexual behavior among patients in Turkey with bipolar disorder, schizophrenia, and heroin addiction. J Sex Med. 2011;8(8):2284-2291. PubMed CrossRef
8. Marengo E, Martino DJ, Igoa A, et al. Sexual risk behaviors among women with bipolar disorder. Psychiatry Res. 2015;230(3):835-838. PubMed CrossRef
9. Meade CS, Bevilacqua LA, Key MD. Bipolar disorder is associated with HIV transmission risk behavior among patients in treatment for HIV. AIDS Behav. 2012;16(8):2267-2271. PubMed CrossRef
10. Meade CS, Graff FS, Griffin ML, et al. HIV risk behavior among patients with co-occurring bipolar and substance use disorders: associations with mania and drug abuse. Drug Alcohol Depend. 2008;92(1-3):296-300. PubMed CrossRef
11. Rai S, Mishra BR, Sarkar S, et al. Higher impulsivity and HIV-risk taking behaviour in males with alcohol dependence compared to bipolar mania: a pilot study. Community Ment Health J. 2018;54(2):218-223. PubMed CrossRef
12. Krantz M, Goldstein T, Rooks B, et al. Sexual risk behavior among youth with bipolar disorder: identifying demographic and clinical risk factors. J Am Acad Child Adolesc Psychiatry. 2018;57(2):118-124. PubMed CrossRef
13. Chen MH, Lan WH, Hsu JW, et al. Risk of developing type 2 diabetes in adolescents and young adults with autism spectrum disorder: a nationwide longitudinal study. Diabetes Care. 2016;39(5):788-793. PubMed CrossRef
14. Chen MH, Pan TL, Li CT, et al. Risk of stroke among patients with post-traumatic stress disorder: nationwide longitudinal study. Br J Psychiatry. 2015;206(4):302-307. PubMed CrossRef
15. Li CT, Bai YM, Huang YL, et al. Association between antidepressant resistance in unipolar depression and subsequent bipolar disorder: cohort study. Br J Psychiatry. 2012;200(1):45-51. PubMed CrossRef
16. Wang YP, Chen YT, Tsai CF, et al. Short-term use of serotonin reuptake inhibitors and risk of upper gastrointestinal bleeding. Am J Psychiatry. 2014;171(1):54-61. PubMed CrossRef
17. Culpepper L. The diagnosis and treatment of bipolar disorder: decision-making in primary care. Prim Care Companion CNS Disord. 2014;16(3):13r01609. PubMed
18. Chen MH, Hsu JW, Huang KL, et al. Sexually transmitted infection among adolescents and young adults with attention-deficit/hyperactivity disorder: a nationwide longitudinal study. J Am Acad Child Adolesc Psychiatry. 2018;57(1):48-53. PubMed CrossRef
19. Liu CY, Hung YT, Chuang YL, et al. Incorporating development stratification of Taiwan townships into sampling design of large scale health interview survey. J Health Management (Chin). 2006;4:1-22.
20. Hutton HE, Lyketsos CG, Zenilman JM, et al. Depression and HIV risk behaviors among patients in a sexually transmitted disease clinic. Am J Psychiatry. 2004;161(5):912-914. PubMed CrossRef
21. Meade CS, Fitzmaurice GM, Sanchez AK, et al. The relationship of manic episodes and drug abuse to sexual risk behavior in patients with co-occurring bipolar and substance use disorders: a 15-month prospective analysis. AIDS Behav. 2011;15(8):1829-1833. PubMed CrossRef
22. Khan MR, Kaufman JS, Pence BW, et al. Depression, sexually transmitted infection, and sexual risk behavior among young adults in the United States. Arch Pediatr Adolesc Med. 2009;163(7):644-652. PubMed CrossRef
23. Fazel S, Zetterqvist J, Larsson H, et al. Antipsychotics, mood stabilisers, and risk of violent crime. Lancet. 2014;384(9949):1206-1214. PubMed CrossRef
24. Brown JL, Gause NK, Northern N. The association between alcohol and sexual risk behaviors among college students: a review. Curr Addict Rep. 2016;3(4):349-355. PubMed CrossRef
25. Dervic K, Garcia-Amador M, Sudol K, et al. Bipolar I and II versus unipolar depression: clinical differences and impulsivity/aggression traits. Eur Psychiatry. 2015;30(1):106-113. PubMed CrossRef
26. Degenhardt EK, Gatz JL, Jacob J, et al. Predictors of relapse or recurrence in bipolar I disorder. J Affect Disord. 2012;136(3):733-739. PubMed CrossRef
27. Perlis RH, Ostacher MJ, Patel JK, et al. Predictors of recurrence in bipolar disorder: primary outcomes from the Systematic Treatment Enhancement Program for Bipolar Disorder (STEP-BD). Am J Psychiatry. 2006;163(2):217-224. PubMed CrossRef
28. Dvorak RD, Wray TB, Kuvaas NJ, et al. Mania and sexual risk: associations with behavioral self-regulation. J Affect Disord. 2013;150(3):1076-1081. PubMed CrossRef
29. Hıdıroğlu C, Demirci Esen ז, Tunca Z, et al. Can risk-taking be an endophenotype for bipolar disorder? a study on patients with bipolar disorder type I and their first-degree relatives. J Int Neuropsychol Soc. 2013;19(4):474-482. PubMed CrossRef
30. Lima IMM, Peckham AD, Johnson SL. Cognitive deficits in bipolar disorders: implications for emotion. Clin Psychol Rev. 2018;59:126-136. PubMed CrossRef
31. Solé B, Jiménez E, Torrent C, et al. Cognitive impairment in bipolar disorder: treatment and prevention strategies. Int J Neuropsychopharmacol. 2017;20(8):670-680. PubMed CrossRef
32. Cullen B, Ward J, Graham NA, et al. Prevalence and correlates of cognitive impairment in euthymic adults with bipolar disorder: a systematic review. J Affect Disord. 2016;205:165-181. PubMed CrossRef
33. Dubé B, Benton T, Cruess DG, et al. Neuropsychiatric manifestations of HIV infection and AIDS. J Psychiatry Neurosci. 2005;30(4):237-246. PubMed
This PDF is free for all visitors!