J Clin Psychiatry 2021;82(2):20ac13786
To cite: Hosanagar A, Cusimano J, Radhakrishnan R. Therapeutic potential of psychedelics in the treatment of psychiatric disorders, part 1: psychopharmacology and neurobiological effects. J Clin Psychiatry. 2021;82(2):20ac13786.
To share: https://doi.org/10.4088/JCP.20ac13786
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Michigan Medicine, Ann Arbor, Michigan
bVeterans Affairs Ann Arbor Healthcare System, Ann Arbor, Michigan
cDepartment of Pharmacy, Michigan Medicine, Ann Arbor, Michigan
dCollege of Pharmacy, University of Michigan, Ann Arbor, Michigan
eDepartment of Psychiatry, Yale University School of Medicine, New Haven, Connecticut
*Corresponding author: Rajiv Radhakrishnan, MBBS, MD, 300 George St, Ste 901, New Haven, CT 06511
([email protected]).
Psychedelics (Greek: “mind manifesting”), also referred to as hallucinogenic drugs, are a group of compounds that produce various (often profound) psychological effects characterized by altered states of perception, thoughts, feelings, and consciousness. Since the early 2000s, there has been a resurgence in clinical research into psychedelics with increasing interest recently among clinicians and patients to harness their therapeutic potential in treating psychiatric disorders. A review of the literature with a critical eye that may inform psychiatrists of the current state of the evidence is hence timely. This article is the first in a 2-part series1 on the psychopharmacology and therapeutic effects of psychedelics. In it, we provide a review of the psychopharmacology and neurobiological mechanisms underlying the use of psychedelic-assisted psychotherapy, with a focus on psilocybin, (±)-3,4-methylenedioxymethamphetamine (MDMA), lysergic acid diethylamide (LSD), and ayahuasca. While mescaline, a naturally occurring hallucinogen in peyote; salvinorin A, found in the plant Salvia divinorum; and ibogaine, an alkaloid found in the West African plant iboga, are other psychedelics with considerable therapeutic interest, the paucity of human clinical studies precluded their inclusion in this brief review. While there is no standard definition for “psychedelics,” these compounds produce profound alterations in the perception of reality and mystical experiences. Compounds such as ketamine, a dissociative anesthetic, are not typically included in this class.
Pharmacology
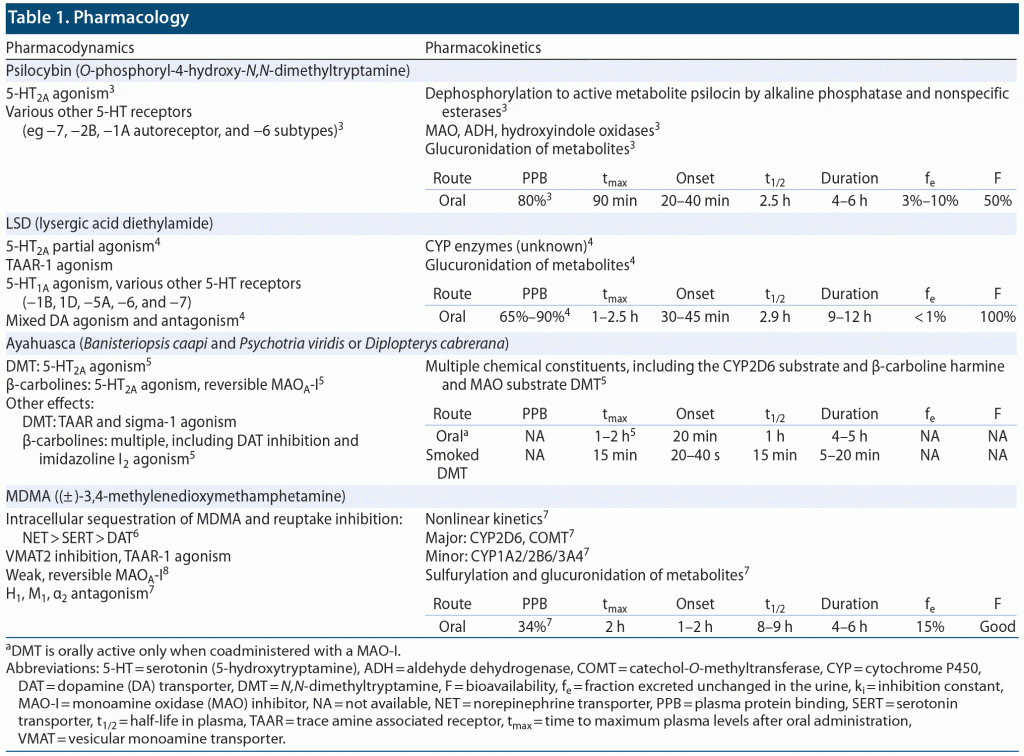
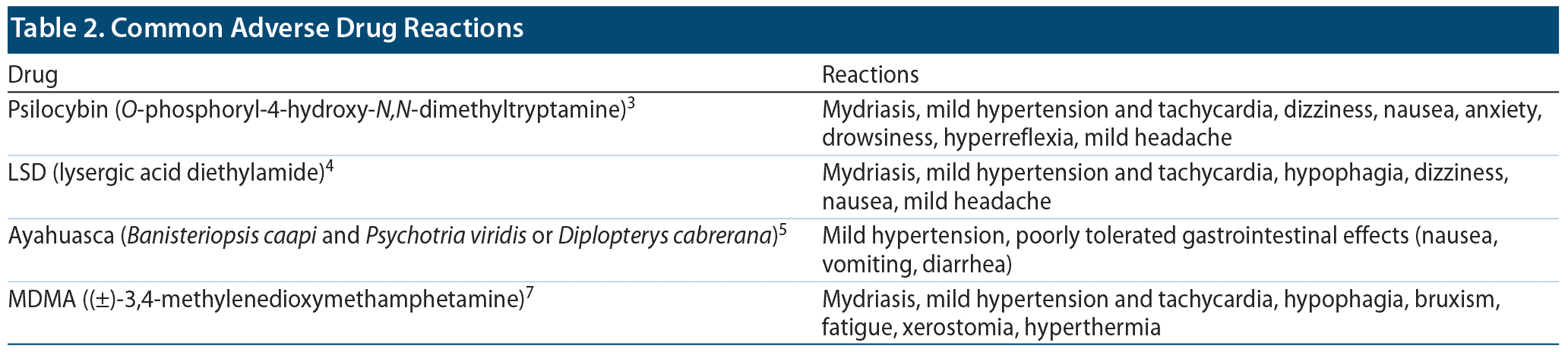
The “classical” psychedelics, consisting of indolamines (psilocybin), alkaloids (N,N-dimethyltryptamine [DMT], the active constituent contained in ayahuasca), and ergolines (LSD), act primarily via serotonin 5-HT2A receptor agonism. MDMA, a phenethylamine, acts via release of presynaptic serotonin and to a lesser extent norepinephrine and dopamine through interactions with the corresponding monoamine transporter, including trace amine-associated receptor 1 (TAAR1) and vesicular monoamine transporter 2 (VMAT2). These compounds have varied pharmacokinetics and pharmacodynamics2 (Table 1). Serotonergic hallucinogens produce “psychedelic” effects that are indistinguishable from each other, consistent with a shared primary mechanism of action.2 The typical effects include enhanced sociality, feelings of closeness to others, openness to new experiences, emotional empathy, trust, feelings of bliss, audiovisual synesthesia, derealization, depersonalization, profound mystical experiences characterized by feelings of boundlessness, enhanced introspection and occasionally anxiety, fear/panic, dysphoria, paranoia, and auditory hallucinations.9–11 MDMA, described as an “entactogen” (Greek: “touching within”; ie, increases empathy and feelings of closeness) and a psychostimulant (producing euphoria, anxiolysis, and a sense of inner peace), does not produce intense hallucinations as seen with classical psychedelics.7 Psychedelics are generally well tolerated at clinically relevant doses, although side effects are common (Table 2). In nonclinical/recreational settings, adverse psychiatric effects have been reported in 40% of users, with 7.6% reporting enduring psychological symptoms.12 There are few pharmacokinetic drug interactions, but the short half-lives of psychedelics decrease the risk for accumulation even in the setting of metabolic inhibition. Of greater relevance are pharmacodynamic drug interactions, such as those with serotonergic drugs (eg, selective serotonin reuptake inhibitors, dextromethorphan), which may increase the risk for serotonin syndrome.
In animal studies, psychedelics elevate glutamate levels in the cortex, increase regionally specific gene expression of brain-derived neurotrophic factor and immediate-early genes, and promote both synaptogenesis and neuroplasticity through a TrkB- and mTOR-dependent mechanism.13 Long-term administration of psychedelics has been shown to cause significant transcriptional changes that last long after stopping them.
Psilocybin
Psilocybin, derived from mushrooms belonging to the genus Psilocybe, and psilocin, its active metabolite, are indolamines. Recent studies have shown that psilocybin has effects on brain functional connectivity.14 Its effects include reducing negative affect and amygdala response to emotional faces at 1 week, with enduring changes in resting state functional connectivity (RSFC) at 1 month,15 along with reducing activity in the default mode network (DMN) (including the subgenual cingulate cortex) in healthy individuals16 and causing changes in synaptic plasticity.13 Contrary to the finding in healthy individuals, psilocybin was associated with increased resting state connectivity within the DMN between the ventromedial prefrontal cortex and the bilateral inferior-lateral parietal cortex after 2 psilocybin treatments in treatment-resistant depression patients and was predictive of clinical response 5 weeks posttreatment.17
LSD
First synthesized in 1938 by Albert Hofmann, LSD is an ergot alkaloid derivative that acts as a 5-HT2A partial agonist and 5-HT1A agonist with additional dopaminergic activity at moderate-high doses (75–200 µg).4 LSD, like other psychedelics, acutely increases plasma concentrations of cortisol, prolactin, oxytocin, and epinephrine.18 Neuroimaging studies show that LSD acutely increases global functional connectivity19 and reduces left amygdala and right medial prefrontal cortex reactivity to fearful faces.20 LSD’s subjective hallucinatory effects are associated with increased functional thalamic connectivity with the insula and the right fusiform gyrus.21 Similar to psilocybin, LSD decreases DMN integrity, which correlates with ratings of ego dissolution.22
Ayahuasca
Ayahuasca is the most popular name for an Amazonian decoction used in religious ceremonies prepared from the vine Banisteriopsis caapi (which contain β-carbolines such as harmine) and leaves of Psychotria viridis (which contains DMT).23 While harmine is a monoamine oxidase inhibitor that prevents peripheral metabolism and increases oral bioavailability of DMT, ayahuasca’s psychedelic effects are primarily due to DMT.24 Structurally similar to melatonin and serotonin, endogenous DMT and its metabolite, 5-OH DMT, are hypothesized to be responsible for dreams, creativity, and other mystical experiences.25 Interestingly, in animals, DMT has been shown to produce fear extinction and antidepressant effects with cellular and behavioral responses similar to ketamine.23
MDMA
Also known as “ecstasy,” MDMA’s exact mechanism as a psychotherapy adjunct for treating posttraumatic stress disorder is unknown, but its entactogenic effects may lower emotional barriers, dampen conditioned fear responses, and improve introspection to facilitate engagement with and extinction of traumatic memories during psychotherapy. Neuroimaging findings in healthy individuals include decreased neural activation of the left amygdala in response to angry vs neutral faces26; lower activation of the left anterior temporal lobe and greater activation of the superior frontal gyrus/dorsal medial prefrontal cortex, which correlated with worst autobiographical memories being perceived less negatively27; decreased RSFC between the prefrontal cortex and hippocampus; and increased RSFC between the hippocampus and amygdala.28
The Current State of the Field and Future Directions
While significant progress has been made in the understanding of the psychopharmacologic and neurobiological effects of psychedelics, several questions remain unanswered. For example, although 5-HT2A agonism has been shown to be important for the “psychedelic” effects of these compounds, it is unclear whether the therapeutic effects are also mediated via 5-HT2A receptors or by other mechanisms, such as 5-HT1, VMAT2, and TAAR-1. The understanding of the neurobiological effects of psychedelics is based on studies with small sample sizes in predominantly healthy adults. Replication and validation of these findings in larger studies in both normal and disease/pathological states are important. Furthermore, the mechanisms underlying the adverse outcomes observed in nonclinical settings remain to be understood.
The dose-response relationship between psychedelics and their therapeutic effects is not well established. Whether a linear dose-response relationship exists or if there is a narrow therapeutic window has yet to be determined. Additionally, while the therapeutic effects of psychedelics are thought to last up to 6 months following a single exposure, the mechanisms underlying these long-lasting effects remain to be deciphered.
Conclusions
Classical serotonergic psychedelics have commonalities in their pharmacology, psychological effects, and mechanism of action via 5-HT2A agonism. MDMA, however, has a distinct and complex neuroreceptor profile. Psychedelic and therapeutic effects may be mediated by more than one mechanism. The effects of psychedelics on brain functional connectivity and synaptic plasticity offer additional mechanisms that warrant further research.
Published online: February 23, 2021.
Potential conflict of interest: None.
Funding/support: None.

The ASCP Corner, edited by Leslie L. Citrome, MD, MPH, is a collection of brief peer-reviewed, evidence-based articles, authored by American Society of Clinical Psychopharmacology members, that examine the practice of psychopharmacology through the lens of clinical experience. The information contained herein only represents the opinion of the author(s).
References (28)

- Hosanagar A, Cusimano J, Radhakrishnan R. Therapeutic potential of psychedelics in treatment of psychiatric disorders, part 2: review of the evidence. J Clin Psychiatry. 2021;82(3):20ac13787.
- Halberstadt AL. Recent advances in the neuropsychopharmacology of serotonergic hallucinogens. Behav Brain Res. 2015;277:99–120. PubMed CrossRef NLM
- Tylš F, Páleníček T, Horáček J. Psilocybin: summary of knowledge and new perspectives. Eur Neuropsychopharmacol. 2014;24(3):342–356. PubMed CrossRef NLM
- Passie T, Halpern JH, Stichtenoth DO, et al. The pharmacology of lysergic acid diethylamide: a review. CNS Neurosci Ther. 2008;14(4):295–314. PubMed CrossRef NLM
- Malcolm BJ, Lee KC. Ayahuasca: an ancient sacrament for treatment of contemporary psychiatric illness? Ment Health Clin. 2018;7(1):39–45. PubMed CrossRef NLM
- Verrico CD, Miller GM, Madras BK. MDMA (Ecstasy) and human dopamine, norepinephrine, and serotonin transporters: implications for MDMA-induced neurotoxicity and treatment. Psychopharmacology (Berl). 2007;189(4):489–503. PubMed CrossRef NLM
- de la Torre R, Farré M, Roset PN, et al. Human pharmacology of MDMA: pharmacokinetics, metabolism, and disposition. Ther Drug Monit. 2004;26(2):137–144. PubMed CrossRef NLM
- Leonardi ET, Azmitia EC. MDMA (ecstasy) inhibition of MAO type A and type B: comparisons with fenfluramine and fluoxetine (Prozac). Neuropsychopharmacology. 1994;10(4):231–238. PubMed CrossRef NLM
- Dolder PC, Schmid Y, Müller F, et al. LSD acutely impairs fear recognition and enhances emotional empathy and sociality. Neuropsychopharmacology. 2016;41(11):2638–2646. PubMed CrossRef NLM
- Carhart-Harris RL, Kaelen M, Bolstridge M, et al. The paradoxical psychological effects of lysergic acid diethylamide (LSD). Psychol Med. 2016;46(7):1379–1390. PubMed CrossRef NLM
- Schmid Y, Enzler F, Gasser P, et al. Acute effects of lysergic acid diethylamide in healthy subjects. Biol Psychiatry. 2015;78(8):544–553. PubMed CrossRef NLM
- Carbonaro TM, Bradstreet MP, Barrett FS, et al. Survey study of challenging experiences after ingesting psilocybin mushrooms: acute and enduring positive and negative consequences. J Psychopharmacol. 2016;30(12):1268–1278. PubMed CrossRef NLM
- Ly C, Greb AC, Cameron LP, et al. Psychedelics promote structural and functional neural plasticity. Cell Reports. 2018;23(11):3170–3182. PubMed CrossRef NLM
- Carhart-Harris RL, Erritzoe D, Williams T, et al. Neural correlates of the psychedelic state as determined by fMRI studies with psilocybin. Proc Natl Acad Sci U S A. 2012;109(6):2138–2143. PubMed CrossRef NLM
- Barrett FS, Doss MK, Sepeda ND, et al. Emotions and brain function are altered up to one month after a single high dose of psilocybin. Sci Rep. 2020;10(1):2214. PubMed CrossRef NLM
- Nutt D. Psychedelic drugs: a new era in psychiatry? Dialogues Clin Neurosci. 2019;21(2):139–147. PubMed CrossRef NLM
- Carhart-Harris RL, Roseman L, Bolstridge M, et al. Psilocybin for treatment-resistant depression: fMRI-measured brain mechanisms. Sci Rep. 2017;7(1):13187. PubMed NLM
- Liechti ME. Modern clinical research on LSD. Neuropsychopharmacology. 2017;42(11):2114–2127. PubMed CrossRef NLM
- Tagliazucchi E, Roseman L, Kaelen M, et al. Increased global functional connectivity correlates with LSD-induced ego dissolution. Curr Biol. 2016;26(8):1043–1050. PubMed CrossRef NLM
- Mueller F, Lenz C, Dolder PC, et al. Acute effects of LSD on amygdala activity during processing of fearful stimuli in healthy subjects. Transl Psychiatry. 2017;7(4):e1084. PubMed CrossRef NLM
- Müller F, Lenz C, Dolder P, et al. Increased thalamic resting-state connectivity as a core driver of LSD-induced hallucinations. Acta Psychiatr Scand. 2017;136(6):648–657. PubMed CrossRef NLM
- Carhart-Harris RL, Muthukumaraswamy S, Roseman L, et al. Neural correlates of the LSD experience revealed by multimodal neuroimaging. Proc Natl Acad Sci U S A. 2016;113(17):4853–4858. PubMed CrossRef NLM
- Cameron LP, Olson DE. Dark classics in chemical neuroscience: N, N-dimethyltryptamine (DMT). ACS Chem Neurosci. 2018;9(10):2344–2357. PubMed CrossRef NLM
- Riba J, Rodríguez-Fornells A, Urbano G, et al. Subjective effects and tolerability of the South American psychoactive beverage Ayahuasca in healthy volunteers. Psychopharmacology (Berl). 2001;154(1):85–95. PubMed CrossRef NLM
- Dean JG. Indolethylamine-N-methyltransferase Polymorphisms: genetic and biochemical approaches for study of endogenous N,N,-dimethyltryptamine. Front Neurosci. 2018;12:232. PubMed NLM
- Bedi G, Phan KL, Angstadt M, et al. Effects of MDMA on sociability and neural response to social threat and social reward. Psychopharmacology (Berl). 2009;207(1):73–83. PubMed CrossRef NLM
- Carhart-Harris RL, Wall MB, Erritzoe D, et al. The effect of acutely administered MDMA on subjective and BOLD-fMRI responses to favourite and worst autobiographical memories. Int J Neuropsychopharmacol. 2014;17(4):527–540. PubMed CrossRef NLM
- Carhart-Harris RL, Murphy K, Leech R, et al. The effects of acutely administered 3,4-methylenedioxymethamphetamine on spontaneous brain function in healthy volunteers measured with arterial spin labeling and blood oxygen level-dependent resting state functional connectivity. Biol Psychiatry. 2015;78(8):554–562. PubMed CrossRef NLM
This PDF is free for all visitors!