Capacity Assessment and Involuntary Commitment in Psychiatric and Medical Settings:
Clinical, Legal, and Cultural Considerations

LESSONS LEARNED AT THE INTERFACE OF MEDICINE AND PSYCHIATRY
The Psychiatric Consultation Service at Massachusetts General Hospital sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.
Prim Care Companion CNS Disord 2019;21(3):19f02472
To cite: Yeung AS, Brandt AS, O’ Neill MA, et al. Capacity assessment and involuntary commitment in psychiatric and medical settings: clinical, legal, and cultural considerations. Prim Care Companion CNS Disord. 2019;21(3):19f02472.
To share: https://doi.org/10.4088/PCC.19f02472
© Copyright 2019 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts
*Corresponding author: Albert S. Yeung, MD, ScD, Department of Psychiatry, Massachusetts General Hospital, MGH DCRP, 1 Bowdoin Sq 6th Floor, Boston, MA 02114 ([email protected]).
Have you ever wondered what criteria need to be satisfied before a patient can be involuntarily admitted to a psychiatric hospital? Have you been puzzled when you learned your patients cannot be involuntarily committed to psychiatric facilities for alcohol use or abuse or for complications of head injuries? Have you been uncertain as to when you should embark on a capacity assessment and guardianship proceedings for those on medical and surgical services? Have you been unsure how cultural factors influence the expectations and attitudes of patients, family members, providers, and systems of care regarding involuntary admission? If you have, the following case vignettes and discussion should prove useful.
CASE VIGNETTES
CASE 1
Mr A, a 19-year-old man, was born and raised in a working-class neighborhood of Boston. He entered foster care at the age of 9, after his mother relapsed on heroin; his father was incarcerated for selling illicit drugs. He was adopted by his foster parents at age 14. At age 17, during his senior year of high school, he developed a sense that he was different from others. He believed he could identify the forces of good and evil in people, objects, and experiences, and he began spending less time with his friends. Shortly after starting college, his parents received a call from his school telling them that he had not returned to the dorm in several nights and had not attended class in several weeks. His family reported him missing to the police. The following night, he was found on the median of a busy street talking to himself. He matched the description of someone who had broken the window of a nearby car and his fist was bleeding.
Mr A was brought by police to an emergency department (ED) for evaluation. Shortly after his arrival, he attempted to leave the hospital and became combative with security staff. He was placed in 4-point restraints and given intramuscular injections of haloperidol, lorazepam, and diphenhydramine. In the ED, his speech made little sense. He was transferred involuntarily to a local psychiatric hospital.
During his hospitalization, he would neither speak to his parents nor allow the treatment team to speak with them. His speech and behavior remained disorganized, and he was unwilling to shower or to change his clothes. He ate in his room and refused medications. Following a court hearing and subsequent involuntary commitment, he began taking olanzapine, eventually receiving a dose of 20 mg per day. After starting this medication, he slowly became more comfortable and engaged with staff, started showering, began eating meals in the day room, and attended groups. He allowed his parents to visit and to speak with the treatment team. He continued to describe his perceived ability to sense good and evil, and he was more forthcoming about hearing voices, but he no longer felt a need to influence good and evil in the world and was less fearful.
CASE 2
Ms B, a 30-year-old Asian woman, came to the United States with her husband 8 years earlier. After they had a child 4 years ago, they purchased a home. Both Ms B and her husband obtained their advanced degrees 2 years later. She was employed as an information technology support person, and her husband found a job as a scientist. Everything seemed to be going well until 8 months ago, when Ms B’s supervisor became concerned. Ms B suspected that her coworkers were criticizing her behind her back, and she complained that people were taking credit for the computer programs she created despite lacking evidence for her suspicions. Later, Ms B heard voices saying that her colleagues did not like her, and she became argumentative with her colleagues as well as with her husband and young son. She had a poor appetite and lost a significant amount of weight. Ms B’s supervisor sent her to a human resources officer who required that she seek a psychiatric evaluation.
A psychiatrist in a local clinic diagnosed Ms B with schizophrenia and prescribed an antipsychotic medication, which she was reluctant to take. Her husband encouraged her to take the medication and warned that she risked losing her job if she did not collaborate with her psychiatrist. After Ms B took the medication, her paranoia, auditory hallucinations, and irritability subsided. Her performance at work improved, her body weight increased, and she experienced less conflict.

- To prevent recurrent psychotic decompensation and rehospitalization due to lack of adherence to treatment, some states allow time-limited outpatient involuntary commitment.
- Physicians can mandate treatment and hospital stay (medical incapacity hold) when medical inpatients lack the capacity to make such a decision.
- When involuntary psychiatric treatment is considered, patients’ and their family members’ value of autonomy versus the importance of symptom control should be taken into consideration.
Four months after her initial visit, Ms B stopped attending her outpatient psychiatry appointments. Her husband came to the clinic and told the psychiatrist that he was concerned his wife had discontinued her medications, as she did not believe she had a psychiatric illness. He reported that his wife’s paranoia toward her colleagues had returned, and her relationship with him and her son had deteriorated. She had stopped talking with her husband, and her son was afraid and would not go near her. A month after this report, the husband returned to the clinic, begging the psychiatrist to send his wife to the hospital. Since their last communication, Ms B had been fired from her job, became more withdrawn and socially isolated, acted strangely, and threw away beloved furniture. In frustration, her husband called the police, who said they could not force Ms B to go to the hospital against her will, as there were no signs that she was at imminent risk of harm to herself or others. Similarly, the psychiatrist told the husband that if Ms B did not want treatment, there was not much he could do, as she was still entitled to make decisions regarding her illness. The husband left the clinic feeling frustrated and disappointed.
CASE 3
Ms C, a 55-year-old former art teacher with a history of severe alcohol use disorder, hypertension, hyperlipidemia, and type 2 diabetes, was brought to the ED after her sisters called 911 after visiting her apartment and finding her unkempt and speaking illogically.
Ms C has a long history of alcohol use; she started drinking in her 20s and quickly began to drink throughout the day. Eventually, she lost her job and began to distance herself from her family; she felt ashamed of her lack of employment and living situation. She voluntarily attended detox treatment on multiple occasions and had 2 distinct periods of about 2 years of sobriety each. When sober, she spent more time with her family and was involved in her niece and nephews’ lives.
Over the last 5 years, Ms C was getting by, though with difficulties. She volunteered at an art studio occasionally and was receiving disability to support herself financially. She lived with her partner of 10 years, who also struggled with alcohol use disorder. However, Ms C’s sisters had become increasingly worried about her. Although she rarely answered their phone calls, her sisters heard from a neighbor that she had been seen sleeping outside in the cold on multiple occasions. When her sisters last visited her, she appeared gaunt, and her kitchen cupboards and refrigerator were bare. Intoxicated, Ms C became angry and threw a plate, narrowly missing one of her sisters. Her primary care physician (PCP) of 20 years had also become more concerned about her over the last few months. She had missed multiple appointments and had not picked up her last medication refills. She previously had consistently followed up with her PCP, although she was not always adherent with her insulin regimen for diabetes and had required 2 hospitalizations for diabetic ketoacidosis.
Concerned after not having heard from Ms C or her partner for several weeks, her sisters went to her apartment to check on her. They found her lying on the kitchen floor in soiled pants. Although awake, she made little sense when she spoke. The sisters called 911, and emergency medical technicians took her to the hospital. She was admitted for treatment of sepsis (due to a urinary tract infection), hyperglycemia, and alcohol withdrawal. On the second day of her hospitalization, she became more confused and agitated, and she pulled out her intravenous catheter, requiring soft restraints and haloperidol. On her third day in the hospital, Ms C requested to leave and was told that she was not permitted to do so, as the psychiatry consultation team had determined that her confusion was caused by delirium due to infection and hyperglycemia.
By the fifth day of hospitalization, her mental status had improved; she was alert and logical. She was evaluated by a physical therapist, who recommended a transfer to an inpatient rehabilitation facility due to physical deconditioning.
DISCUSSION
Although patients with severe mental illnesses, including substance use disorders, are usually managed by mental health providers, the boundary between comorbid medical and mental disorders is often blurred. Since the current trend is toward integration of primary care and behavioral health, it is important for PCPs to know when and how they should assess a patient’s capacity to make decisions regarding their medical treatment. If patients lack the capacity to decide, providers need to be familiar with the process of involuntary commitment and treatment of their acute medical condition against their will, as well as of severe mental illness, substance use disorder, or a mixture of these conditions.
Use of Involuntary Treatment
Standards for psychiatric involuntary commitment vary from state to state.1,2 To initiate involuntary commitment, a physician, psychologist, or (in some states) other licensed mental health professional must sign a mental health emergency certificate attesting that as a result of mental illness, a patient is a danger to himself/herself or to others. These patients are sent to an emergency department to be evaluated and to determine whether they meet criteria for an involuntary psychiatric hospitalization. Patients can then be held in the psychiatric hospital for that state’s legislatively specified time period. At the end of this time, the facility must decide whether to release the patient or to petition for a court-ordered involuntary hospitalization. Aside from psychiatric emergencies, in which there is an imminent risk of harm (to self or others), most states do not allow clinicians to force adult patients to take medication against their will, unless the clinician has been granted a court order to administer medications.3
In the case of those with new-onset psychotic disorders, such as Mr A and Ms B, the illness itself—in the form of paranoid delusions or the tendency to withdraw from others—prevents individuals from pursuing treatments and social connections that can improve their lives. Primary psychotic illnesses are often characterized by poor insight into the patient’s own degree of impairment and need for treatment. Both Mr A and Ms B showed a similar, clear pattern of illness behavior over time. When they discontinued antipsychotic medications, they withdrew from their social supports, became increasingly suspicious of those they usually trusted, and focused on their own internal experiences. The challenge facing the families and doctors of Mr A and Ms B is determining when it is reasonable and appropriate to intervene, while appreciating and respecting the individual’s autonomy.
In the case of Mr A, his involuntary psychiatric hospitalization took place after he demonstrated an imminent risk of harm to self or others. Prior to his hospitalization, he was disorganized, wandering the streets overnight and punching property. Mr A was committed for an evaluation at an ED, where he was deemed at imminent danger, justifying hospitalization. In contrast, Ms B’s nonadherence to medication treatment led to her losing her job and damaging her familial relationships when she became symptomatic, but she did not demonstrate risk to herself or others and was able to marginally care for herself. Therefore, her psychiatrist was unable to compel either involuntary hospitalization or outpatient treatment.
Arguably, an individual’s ability to fully express autonomy can be impaired by psychotic illness. To strike a balance between beneficence and respect for autonomy, some states provide additional measures to avoid repeated rehospitalizations due to treatment nonadherence. One such measure is involuntary outpatient commitment, a civil procedure by which a judge may order a person with severe mental illness to adhere to a time-limited outpatient treatment plan (usually 180 days) to prevent relapse and deterioration. Involuntary outpatient commitment can be invoked following release from involuntary hospitalization, as an alternative to involuntary hospitalization or as a preventive treatment for those who do not currently meet criteria for involuntary hospitalization.4 Adequate resources are required to ensure the statute achieves its intended goal, including the availability of medication management and psychosocial services, efforts to engage patients and their families in treatment, and the participation of law enforcement officers to assume physical custody of nonadherent patients. Criticisms of this type of approach include the problem of historically based distrust of law enforcement officers among certain minority and disenfranchised groups, as well as the possible disproportionate use of involuntary outpatient commitment among these groups. Mental health professionals are usually responsible for carrying out involuntary hospitalization or involuntary outpatient commitment. PCPs who have a personal relationship with the patient or family can greatly facilitate the patient’s treatment by either gaining the patient’s trust to agree to voluntary care or working with the family to engage the patient, including transporting the patient to an ED, providing relevant history on the patient’s condition, and assisting in immediate and long-term management when the patient is stable.
Some states allow psychiatric advance directives, which outline a patient’s preferences for treatment.5 In theory, these are completed when a patient is at their healthiest and are drawn upon only if and when the patient’s illness impacts his or her capacity to make decisions about treatment. Psychiatric advance directives assist doctors and families in ensuring that treatment decisions are in line with the patient’s values. However, they are less useful in the case of patients who, even at their healthiest, object to psychiatric treatment.
Use of Involuntary Treatment for Medical Patients
To provide involuntary treatment for medical patients, providers need to determine whether the patient has the capacity to make a medical decision. Capacity refers to an individual’s ability to make a specific decision, as determined by a physician. Capacity is different from competency, which is a legal judgment regarding an individual’s ability to make decisions globally; this must be determined by a judge. Someone may be competent in a general sense but lack the capacity to make a specific decision. They may also lack capacity for one decision but not another. For a clinician to demonstrate a patient’s capacity to make a medical decision, 4 legal standards must be met: (1) the patient expresses a consistent preference, (2) the patient is able to demonstrate a factual understanding of the illness and treatment, (3) the patient can convey appreciation for the situation and the likely outcomes of treatment options, and (4) the patient is able to rationally manipulate this information (ie, they can reason about treatment options and communicate the process by which they have made their decision).6
When Ms C became agitated, she was treated against her will in the hospital, as she most likely did not have capacity due to delirium. While capacity was not formally assessed at the time, it was evident from the case narrative that Ms C was unable to engage with the team, and, therefore, she could not demonstrate a factual understanding of her illness nor appreciation of the alternatives and outcomes. Additionally, there was insufficient time for a more formal assessment, as she was agitated and putting both herself and others at risk. In this scenario, involuntary treatment was necessary for both Ms C’s and her treatment team’s safety and thus appropriate. This type of scenario is common in inpatient medical settings when a patient declines ongoing treatment but is thought to lack the capacity to make a medical decision.
A medical incapacity hold occurs when patients are kept in the hospital for ongoing medical care despite their wish to leave but do not have the capacity to refuse medical treatment. Although this can clinically resemble an involuntary psychiatric hold, there are no legal statutes for a medical incapacity hold; this is true across the United States. Legal involuntary psychiatric holds are specifically for danger to self or others related to mental illness, not medical illness, and should not be used in settings in which there is a medical etiology driving a patient’s lack of capacity.7 Because there is no legal statute, physicians justify a medical incapacity hold by documenting the patient’s lack of capacity to make a specific medical decision and the clinical need for that medical treatment in the patient’s chart. To provide guidance in the absence of a clear legal framework, some hospitals develop an institutional policy or have an agreed-upon clinical approach to medical hold determination and documentation.7
An important component of a medical incapacity hold is that it is temporal in nature. An individual who is medically ill and lacks capacity is considered to only temporarily lack the capacity to make a specific medical decision. Treatment of their medical illness aims to restore that capacity. The medical incapacity hold differs from a psychiatric hold in that the standard for ending an involuntary hold is absence of imminent risk of harm to self or others. In a medical incapacity hold, an individual’s capacity must be reassessed frequently, particularly at new or recurring decision points. The temporal nature of capacity is relevant in the case of Ms C, as her delirium cleared with treatment of her urinary tract infection and hyperglycemia. Due to this assumption of capacity being temporal, medical incapacity holds do not apply as clearly in the setting of more permanently disabling medical illnesses such as underlying developmental delay or neurocognitive disorders.
Additionally, involuntary holds do not apply to substance use. In general, patients cannot be treated involuntarily due to substance use disorders, including alcohol use disorder. In multiple states, however, a family member or a physician can petition the court for an individual to be involuntarily placed in substance use disorder treatment.8 A pattern of high risk of harm to self due to substance use must be demonstrated; Ms C most likely met criteria for this, as the medical problems that led to her hospitalization were arguably a direct result of poor self-care in the context of alcohol use and abuse. This may be a course of action the treatment team can recommend to Ms C’s family.
How Does Culture of the Patient, Family, Clinician, and Society Play a Role in Involuntary Treatment?
Throughout most of the developed world, the standard for both involuntary psychiatric hospitalization and involuntary outpatient treatment is that the person has a mental illness and represents an acute threat to self or others and that less coercive measures (eg, acute outpatient crisis intervention, voluntary admission, home treatment) are insufficient.9 The specifics of legal regulations, clinical practice, and societal attitudes regarding the use of coercion, however, vary greatly around the globe.10,11 Internationally, the rate of involuntary hospitalizations varies widely.10,11 Large differences in the rate of involuntary hospitalizations can be found not only between culturally diverse regions, but also between countries with comparable legislation and attitudes toward coercion.12 Thus, even countries that may share broad cultural values, including respect for human rights, personal freedom, and autonomy, may exhibit important differences with regard to the specifics of clinical practice when it comes to involuntary hospitalization and assertive outpatient treatment.12 These differences become even more pronounced when patients’ and their families’ cultural backgrounds are taken into consideration, along with accompanying historical, economic, and social factors. Psychiatric clinicians inevitably hold a dual role—possessing both a duty to provide care for mentally ill persons on the one hand and an obligation to serve as society’s “safe-keepers” on the other. This dual role contributes to a constant tension between the treatment needs of the individual, the safety needs of society, and the individual’s civil liberties.13 Negotiation of these factors is shaped by cultural influences, legislation, and clinical practice patterns. For example, in the case of Ms B, her husband may have believed that he would have more influence over his wife’s treatment due to the importance of family preferences in the Chinese health care system. Before China’s first Mental Health Law took effect in 2013, involuntary psychiatric treatment in China was routinely initiated by a spouse or parents and was shaped by cultural factors prioritizing the authority of the family unit.
These considerations raise important challenges and questions in psychiatric treatment. How can one separate the person from the psychiatric illness and the illness from the person? For someone without clear evidence of a psychotic illness, we would attribute behaviors such as distancing oneself from family or not attending college classes, potentially jeopardizing one’s opportunities for future work, as personal choices in line with the individual’s own values. However, when considered in the context of an illness of thought and perception, our reaction most likely changes, and one wonders how the same individual’s decisions and behavior would differ had they not become ill.
When considering the use of involuntary psychiatric treatment, providers need to consider the patient’s preference when they were healthy and their judgment was not affected by illness. This includes taking into consideration cultural norms in terms of individualistic versus collectivistic values. In addition, it is important to understand how certain groups prefer to be treated based on their ability to trust the health care system and the law enforcement system. For example, in the case of Mr A, a 19-year-old, he was still early in the process of developing his goals and values. At the same time, he was independent, lived alone, and had been adamant that he wanted to make his own decisions regarding treatment and that he did not trust the law enforcement system. On the other hand, Ms B, a Chinese immigrant who was a mother and a wife, was from a culture that prioritized the collective good and family responsibility. How should these considerations be factored in when making a decision regarding involuntary psychiatric treatment?
Similar to preferences for medical and psychiatric treatment, considerations of involuntary treatment for medical and surgical patients can be influenced by the patient’s and family’s cultural norms and preferences. That being said, general techniques for forensic cultural evaluations have not received significant attention. Different approaches have been proposed to be utilized on the basis of group racial or ethnic characteristics. While this is a well-intentioned attempt to provide guidance for clinicians struggling with cross-cultural challenges, it also risks stereotyping.14 Generalizations can minimize individual differences and ignore how individuals select hybrid identities reflecting multiple characteristics.15 A more nuanced approach might be to elicit an individual patient’s and family’s preferences regarding involuntary hospitalization at the outset, much as one would regarding other treatment preferences. Cultural humility, the ability to maintain an interpersonal stance that is open in relation to aspects of cultural identity that are most important to the patient, has been proposed as a key attitude that predicts success within cross-cultural clinical encounters.16 Culturally humble clinicians do not assume competence in terms of working with a particular patient simply based on a shared cultural background or prior experience with other patients from similar backgrounds. Of note, this movement has gained favor in the field of health care over the previously widely used term cultural competence, which has been more recently criticized for implying that there is a finite and static goal to be attained, rather than an overall approach or attitude that considers the dynamic and multidimensional nature of culture. Useful tools for eliciting patient preferences for psychiatric treatment include the Cultural Formulation Interview (CFI) from the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5)17 and the Engagement Interview Protocol (EIP).18
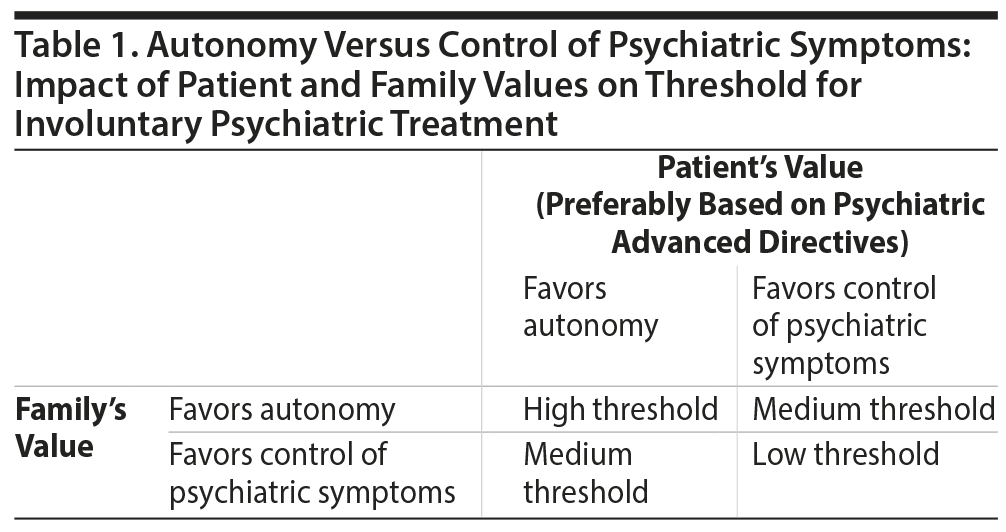
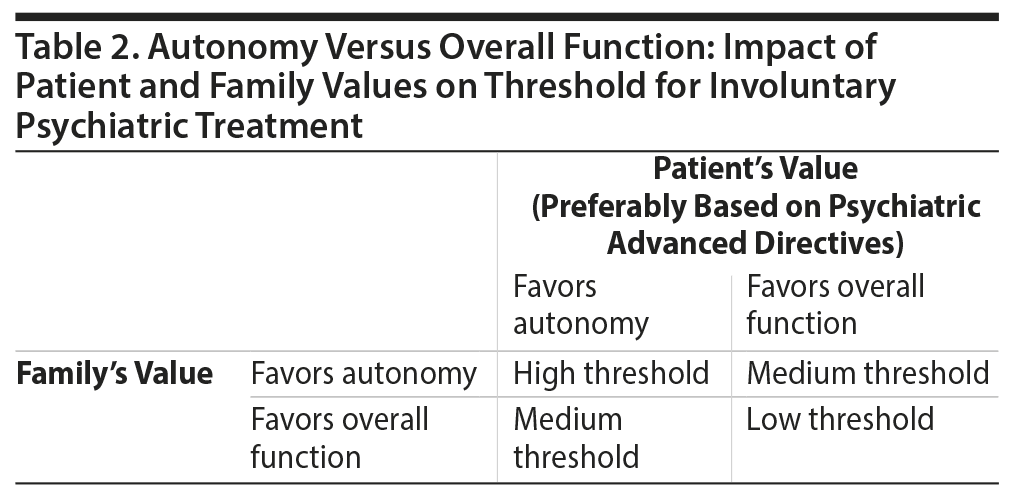
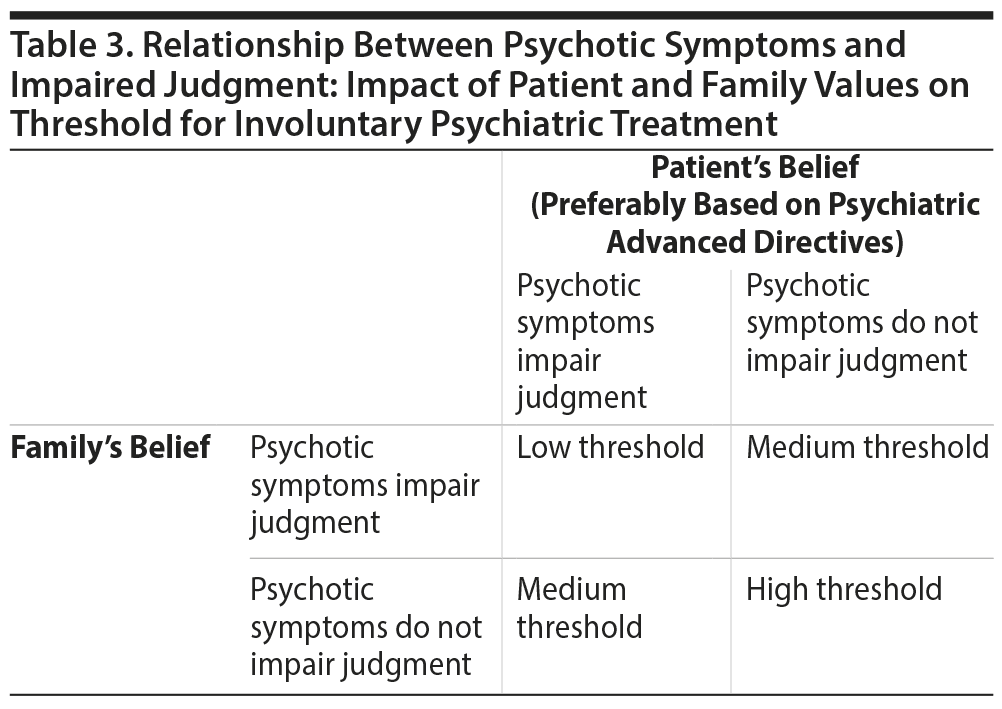
During the initial psychiatric evaluation and thereafter, using tools such as the CFI and EIP may improve clinicians’ cultural humility in considering involuntary treatment, as well as enhance communication between clinicians, patients, and families. Use of these tools expresses respect and a lack of superiority with regard to the patient’s culture. By providing a more nuanced, complete understanding of the patients’ cultural background, their understanding of their illness, and their beliefs regarding psychiatric care—specifically including involuntary treatment—clinicians can enhance their engagement of patients (Tables 1-3).
CONCLUSION
In this article, we used 3 cases to explore the complexities of involuntary treatment based on psychiatric, medical, and substance-related illness. Psychiatric involuntary treatment standards vary from state to state, but generally require that there is a demonstrable likelihood of harm to self or others as a result of untreated mental illness, and may apply to both inpatient and outpatient treatment. Medical involuntary treatment, on the other hand, is invoked in cases of immediate life-threatening medical illness or when patients have medical symptoms that temporarily impair their capacity to make a decision. The legal framework governing each of these approaches differs somewhat due to differing jurisdictions by the Departments of Mental Health and Public Health. Specifically, the medical hold that applies in cases of medical emergency is a clinical decision rather than a legal status. For historical reasons, substance use falls into a third category. Substance use disorder resembles psychiatric illness in terms of both chronicity and impairment of affect, behavior, and cognition and indeed is generally considered to be a psychiatric illness defined in the DSM, yet it cannot be utilized as grounds for involuntary psychiatric treatment. However, some states possess a legal mechanism whereby the family or providers can petition to have the patient involuntarily placed in time-limited treatment focused on the substance use disorder.
Involuntary treatment raises challenging questions about the boundary between self and illness, as well as about the appropriate role of society, psychiatry, and law enforcement to intervene on behaviors seen as abnormal or self-destructive. Additionally, all of these considerations are greatly influenced by differences in cultural norms and values regarding the relative importance of individual, family, and societal goals. Future studies should propose frameworks and guidelines to assist clinicians in how to approach the determination of the appropriateness of involuntary treatment for each of these categories of illness within different cultural contexts.
Submitted: April 21, 2019; accepted May 31, 2019.
Published online: June 27, 2019.
Potential conflicts of interest: Dr Stern is an employee of the Academy of Consultation-Liaison Psychiatry (as editor of Psychosomatics). Drs Yeung, Brandt, O’ Neill, Chen, and Trinh report no conflicts of interest related to the subject of this article.
Funding/support: None.
Additional information: The case vignettes are all either a composite of multiple cases or had their identifying and demographic information altered to protect patient identity.
REFERENCES
1. Gutheil TG, Appelbaum PS. Legal issues in emergency psychiatry. In: Gutheil TG, Appelbaum PS, eds. Clinical Handbook of Psychiatry and the Law. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2007:33-68.
2. Standards for Involuntary Commitment (Assisted Treatment) State-by-State. Mental Ilness Policy Org website. https://mentalillnesspolicy.org/national-studies/state-standards-involuntary-treatment.html. Accessed May 21, 2019.
3. Ostermeyer B, Shoaib AN, Deshpande S. Legal and ethical challenges, part 1: general population. Psychiatr Clin North Am. 2017;40(3):541-553. PubMed CrossRef
4. Swartz MS, Hoge SK, Pinals DA, et al. Resource Document on Involuntary Outpatient Commitment and Related Programs of Assisted Outpatient Treatment. 2015. American Psychiatric Association website. https://www.psychiatry.org/File%20Library/Psychiatrists/Directories/Library-and-Archive/resource_documents/resource-2015-involuntary-outpatient-commitment.pdf. Accessed April 3, 2019.
5. Nicaise P, Lorant V, Dubois V. Psychiatric advance directives as a complex and multistage intervention: a realist systematic review. Health Soc Care Community. 2013;21(1):1-14. PubMed CrossRef
6. Appelbaum PS. Clinical practice: assessment of patients’ competence to consent to treatment. N Engl J Med. 2007;357(18):1834-1840. PubMed CrossRef
7. Cheung EH, Heldt J, Strouse T, et al. The medical incapacity hold: a policy on the involuntary medical hospitalization of patients who lack decisional capacity. Psychosomatics. 2018;59(2):169-176. PubMed CrossRef
8. National Alliance for Model State Drug Laws. Involuntary Comittment for Individuals with a Substance Use Disorder or Alcoholism. 2016. https://www.mass.gov/files/documents/2018/11/15/Involuntary Commitment for Individuals with a Substance Use Disorder or Alcoholism (August 2016).pdf. Accessed March 27, 2019.
9. Salize HJ, Dressing H, Peitz M. Compulsory Admission and Involuntary Treatment of Mentally Ill Patients: Legislation and Practice in EU-Member States. 2002. http://www.mentalhealthalliance.org.uk/pre2007/documents/salize.pdf. Accessed April 3, 2019.
10. Bowers L, van der Werf B, Vokkolainen A, et al. International variation in containment measures for disturbed psychiatric inpatients: a comparative questionnaire survey. Int J Nurs Stud. 2007;44(3):357-364. PubMed CrossRef
11. Riecher-Rössler A, Rössler W. Compulsory admission of psychiatric patients: an international comparison. Acta Psychiatr Scand. 1993;87(4):231-236. PubMed CrossRef
12. Hotzy F, Kerner J, Maatz A, et al. Cross-cultural notions of risk and liberty: a comparison of involuntary psychiatric hospitalization and outpatient treatment in New York, United States and Zurich, Switzerland. Front Psychiatry. 2018;9:267. PubMed CrossRef
13. Dressing H, Salize HJ. Compulsory admission of mentally ill patients in European Union Member States. Soc Psychiatry Psychiatr Epidemiol. 2004;39(10):797-803. PubMed CrossRef
14. Aggarwal NK. Adapting the cultural formulation for clinical assessments in forensic psychiatry. J Am Acad Psychiatry Law. 2012;40(1):113-118. PubMed
15. Bibeau G. Cultural psychiatry in a creolizing world: questions for a new research agenda. Transcult Psychiatry. 1997;34(1):9-41. CrossRef
16. Hook JN, Davis D, Owen J, et al. Cultural Humility, Engaging Diverse Identities in Therapy. Washington, DC: American Psychological Association; 2017.
17. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
18. Yeung A, Trinh NH, Chang TE, et al. The Engagement Interview Protocol (EIP): improving the acceptance of mental health treatment among Chinese immigrants. Int J Cult Ment Health. 2011;4(2):91-105. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!