Objective: To examine whether childhood physical and sexual abuse is a significant predictor of suicide risk in veterans.
Methods: This study was a retrospective chart review of 4,709 patients admitted to a psychiatric ward (August 2004 through July 2014) at the Atlanta Veterans Affairs Medical Center (VAMC). Sociodemographic and clinical data and history of childhood (aged ≤ 18 years) physical and sexual abuse were obtained from the patients’ electronic health records. Suicide risk data of patients who attempted and completed suicide were obtained from the Atlanta VAMC suicide high-risk team. Binary logistic regressions with maximum likelihood estimation method were used to examine the association of demographic (age, sex, marital status, race, service) and clinical (psychiatric diagnoses, number of hospital admissions, and length of stay) variables and childhood physical and sexual abuse and type with suicide behavior.
Results: The combination of childhood physical and sexual abuse, number of admissions to a psychiatric inpatient unit, and major depressive disorder (MDD) were the best predictors of enhanced suicide risk (P < .001). This combination accounted for 9.9% variance in suicide risk and correctly classified 83% of cases into respective suicide versus nonsuicide risk groups. Additional significant predictors were bipolar disorder (P < .001) and cocaine use disorder (P = .02). Surprisingly, diagnosis of schizophrenia predicted a reduced risk.
Conclusions: To our knowledge, this study is the first to shed light on the interaction of childhood physical and sexual abuse and suicide risk in a large cohort of veterans. In the final model, childhood physical and sexual abuse, number of psychiatric admissions, and MDD were the best predictors of increased suicide risk. Schizophrenia was a protective factor in this veteran cohort.
Childhood Physical and Sexual Abuse Predicts
Suicide Risk in a Large Cohort of Veterans
ABSTRACT
Objective: To examine whether childhood physical and sexual abuse is a significant predictor of suicide risk in veterans.
Methods: This study was a retrospective chart review of 4,709 patients admitted to a psychiatric ward (August 2004 through July 2014) at the Atlanta Veterans Affairs Medical Center (VAMC). Sociodemographic and clinical data and history of childhood (aged ≤ 18 years) physical and sexual abuse were obtained from the patients’ electronic health records. Suicide risk data of patients who attempted and completed suicide were obtained from the Atlanta VAMC suicide high-risk team. Binary logistic regressions with maximum likelihood estimation method were used to examine the association of demographic (age, sex, marital status, race, service) and clinical (psychiatric diagnoses, number of hospital admissions, and length of stay) variables and childhood physical and sexual abuse and type with suicide behavior.
Results: The combination of childhood physical and sexual abuse, number of admissions to a psychiatric inpatient unit, and major depressive disorder (MDD) were the best predictors of enhanced suicide risk (P < .001). This combination accounted for 9.9% variance in suicide risk and correctly classified 83% of cases into respective suicide versus nonsuicide risk groups. Additional significant predictors were bipolar disorder (P < .001) and cocaine use disorder (P = .02). Surprisingly, diagnosis of schizophrenia predicted a reduced risk.
Conclusions: To our knowledge, this study is the first to shed light on the interaction of childhood physical and sexual abuse and suicide risk in a large cohort of veterans. In the final model, childhood physical and sexual abuse, number of psychiatric admissions, and MDD were the best predictors of increased suicide risk. Schizophrenia was a protective factor in this veteran cohort.
Prim Care Companion CNS Disord 2018;20(4):18m02317
To cite: Koola MM, Ahmed AO, Sebastian J, et al. Childhood physical and sexual abuse predicts suicide risk in a large cohort of veterans. Prim Care Companion CNS Disord. 2018;20(4):18m02317.
To share: https://doi.org/10.4088/PCC.18m02317
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry and Behavioral Sciences, George Washington University School of Medicine and Health Sciences, Washington, DC
bDepartment of Psychiatry, Weill Cornell School of Medicine, New York, New York
cDepartment of Family Medicine, Aultman Hospital, Canton, Ohio
dAtlanta Veterans Affairs Medical Center, Decatur, Georgia
eDepartment of Psychiatry and Behavioral Sciences, Emory University School of Medicine, Atlanta, Georgia
*Corresponding author: Maju Mathew Koola, MD, Department of Psychiatry and Behavioral Sciences, George Washington University School of Medicine and Health Sciences, 2300 I St NW, Washington, DC 20037 ([email protected]).
According to the US Department of Veterans Affairs, a veteran commits suicide every 65 minutes in the United States.1 In 2012, 349 active-duty service members committed suicide—almost 1 a day.1 More service members die by their own hands than in combat.2 In the US general population, suicide rates have increased recently despite prevention efforts.3 More than 800,000 people worldwide die by suicide each year, and 75% of these deaths occur in low- or middle-income countries.4 This rate corresponds to approximately 1 committed suicide every 40 seconds.4 According to the American Foundation for Suicide Prevention,5 approximately 39,000 Americans die from suicide each year, and 650,000 hospital visits are attributed to suicide attempts. Suicide is among the main causes of death in people aged 15 to 44 years old. Suicide is the fifth-leading cause of death among those aged 30–49 and the second-leading cause of death in those aged 15–29.5 Hence, suicide is a clinical problem of enormous importance. The identification of risk factors is very likely to help suicide prevention efforts. Several factors have been shown to predict suicide in psychiatric populations, including veterans. Specifically, comorbid depression, substance use disorders, and history of trauma were predictive of suicide or suicide attempts.6 History of childhood physical and sexual abuse was found to be associated with suicidal behavior in nonveteran samples.7–9
Our prior study10 in a subset (N = 603) of the current dataset (N = 4,709) reported that the prevalence of childhood physical and sexual abuse in patients admitted to the psychiatric inpatient ward at the Atlanta Veterans Affairs Medical Center (Atlanta VAMC) was 19.4% (117/603). However, the association between childhood abuse and suicide risk in veterans is unknown. Given the substantial rate of childhood abuse in our veteran population and the high rate of veteran suicide, the objective of this study was to examine whether childhood physical and sexual abuse is a significant predictor of suicide risk in veterans.
METHODS
This study was a retrospective chart review of 4,709 patients (4,105 men and 604 women) admitted to a psychiatric ward during a period of 10 years (August 2004 through July 2014) at the Atlanta VAMC. The admission history and physical note completed by the admitting psychiatry attending or resident physician contain information about childhood (aged ≤ 18 years) physical and sexual abuse. These data were read directly from the patients’ charts using the electronic clinician interface, and the information was entered into investigator-created databases in FilemakerPro for Macintosh version 11.0. When present, a note documenting the Addiction Severity Index,11 which also contains information on childhood physical and sexual abuse, was also reviewed, and the data were entered into the study databases. Additional admissions data were extracted from the Veterans Integrated Service Network (VISN7) Corporate Database: dates of admission and discharge, treating specialty for the admission, and discharge diagnoses were included along with identifying information to permit linkage to other tables of data. These data were extracted and imported into the customized databases, and scripts were created that compiled the length of each admission for each individual patient. We merged demographic information, including age, sex, race, era of service (period in which the veteran served in the military), VA service–connected status (whether the patient receives disability payment from the VA), and other variables that categorize the patient’s financial, employment, and marital status.
To monitor and prevent suicide in veterans, suicide high-risk teams have been formed at VAMCs across the United States. These teams maintain a list of VAMC patients who have attempted and completed suicide so that the attempters can be followed with enhanced frequency of contact. We obtained the data of patients who had attempted or completed suicide from the suicide high-risk team at the Atlanta VAMC to identify patients with a history of suicide attempt.
The Emory University Institutional Review Board approved this study and granted it exempt from requiring informed consent documents from the patients. The Atlanta VA Research and Development Committee and the VISN7 Corporate Database Committee also approved this study.
Statistical Analyses
Data from 4,709 veterans were included in the analysis. Binary logistic regressions (BLR) with maximum likelihood estimation method were used to examine the association of demographic (age, sex, marital status, race, service) and clinical (psychiatric diagnoses, number of hospital admissions, and length of stay) variables and childhood physical and sexual abuse and type with suicide behavior. These groups of variables were examined in separate analyses. Whereas childhood physical and sexual abuse was a binary variable, type of abuse was treated as a polytomous variable with 4 categories: none, physical, sexual, and both physical and sexual. Forward selection was used to identify the smallest set of demographic, clinical, and abuse-related variables needed to accurately predict suicide status. Nagelkerke R2 was used to estimate the proportion of variance accounted for in the assignment of veterans into either the suicide group (attempters and completers) or the nonsuicide group. We included the results of receiver operating characteristics analysis to estimate the classification accuracy of individual predictors.
Multivariate analysis of variance (MANOVA) was used to compare number and length of hospital admissions among veterans with and without a documented history of suicide attempts and completed suicide. A statistically significant MANOVA model, suggesting significant multivariate effects, was followed up with a post hoc evaluation of the significance of univariate effects. The post hoc univariate F tests allow a determination of the specific variable(s) that contribute to the significant multivariate effect. Potential associations among childhood physical and sexual abuse, psychopathology, and suicide risk were examined using mediated multiple regression models. All statistical analyses were carried out using SPSS Statistics version 17.1.
RESULTS
Sociodemographic and Clinical Characteristics
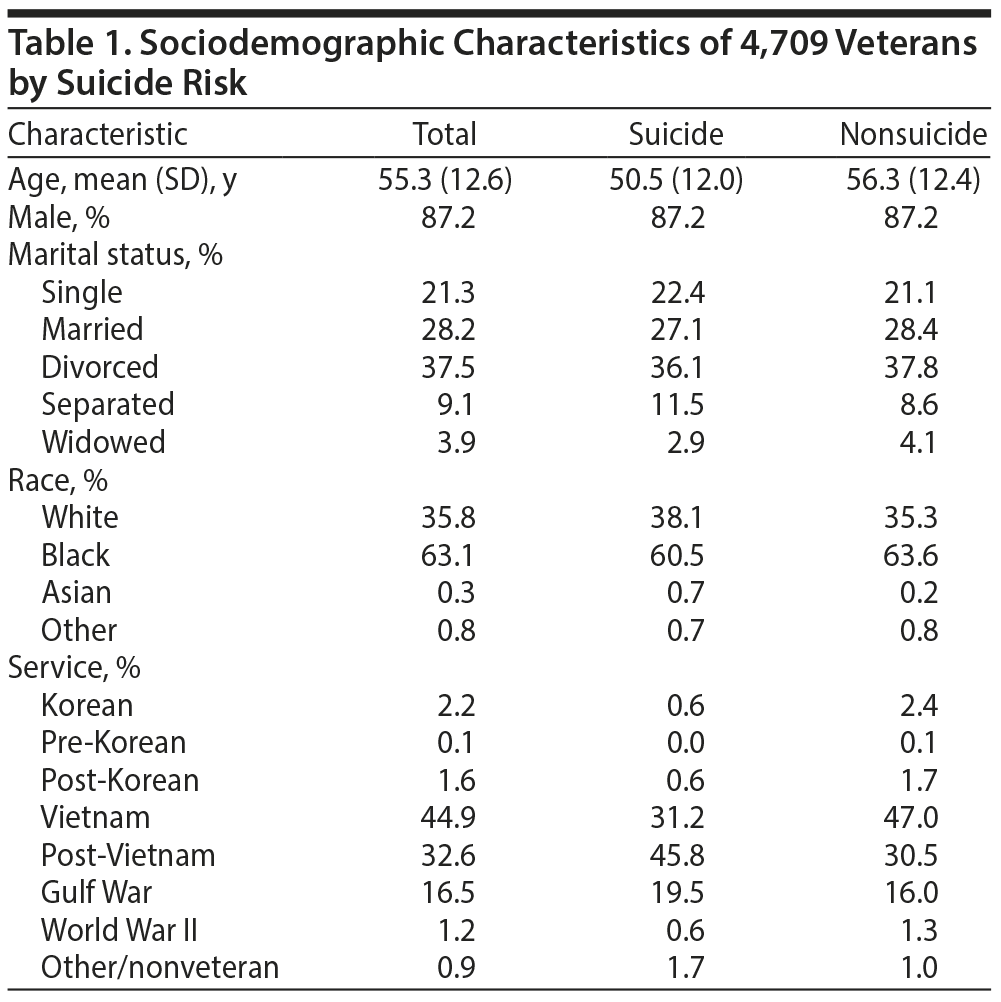
The sociodemographic characteristics of the sample are summarized in Table 1. The majority of the sample was men (87.2%) and black (63.1%). Most respondents were married (28.2%) or divorced (37.5%) and had served during the Vietnam era (44.9%). The sample included 772 (16.4%) individuals with a history of at least 1 suicide attempt. The most common (52.1%) psychiatric diagnosis among study participants was major depressive disorder (MDD). Substance use disorders (SUDs) were highly prevalent in the sample, including alcohol (33.8%) and cocaine (29.8%) use. Participants, on average, stayed in the hospital for a mean (SD) of 19.2 (29.4) days and had 1.8 (1.8) admissions to the Atlanta VAMC during the observation period of the study. Many of these participants (1,178; 29%) had experienced at least 1 incidence of childhood physical or sexual abuse.
Sociodemographic Correlates of Suicide Risk
Sex, race, and marital status were simultaneously entered into a BLR model as predictors with suicide risk as the binary dependent variable to determine if individuals with a history of suicide attempt differed from those without on sociodemographic variables. The overall regression model was significant (χ211 = 23.72, P = .01) and was a marginal fit to the data (−2logl = 4,176.67; Hosmer-Lemeshow χ27 = 4.56; P = .713). Although the model had 83.5% accuracy for classifying participants by suicide risk, it accounted for only 0.9% variance in the prediction of suicide risk. Race was a significant predictor of increased suicide risk among whites and Asians (Wald χ25 = 13.35, P = .02), whereas the effect of marital status was marginal (Wald χ25 = 10.68, P = .06). Regarding marital status, suicide risk was greater for individuals who were separated compared to those who were not.
Diagnostic Correlates of Suicide Risk
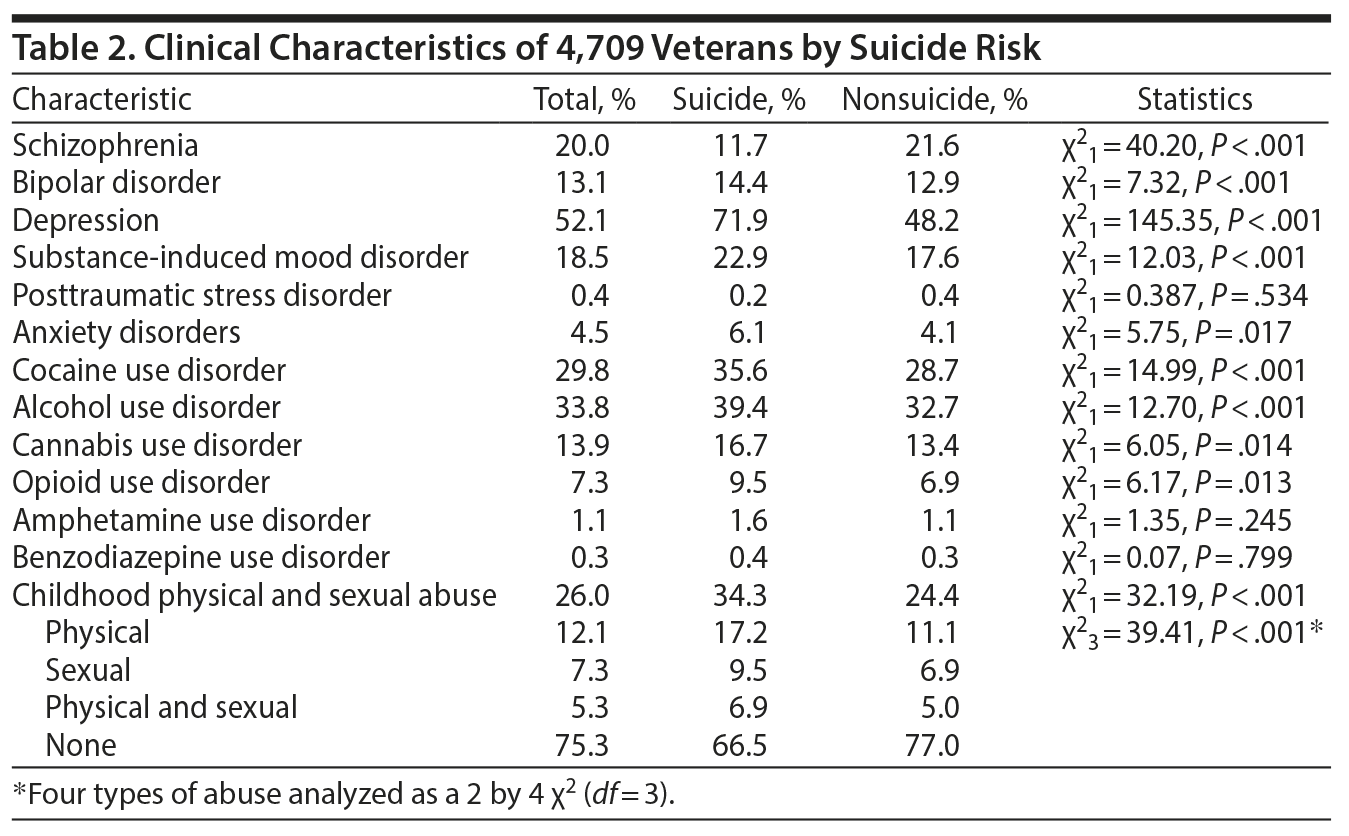
The clinical characteristics of 4,709 veterans by suicide risk are shown in Table 2. The diagnostic data were simultaneously entered into the BLR to determine if certain diagnoses increased suicide risk. Binary psychiatric diagnoses entered into the model included schizophrenia and psychosis, posttraumatic stress disorder (PTSD), bipolar disorder, MDD, and anxiety disorders. SUDs, including cocaine, alcohol, cannabis, opioid, amphetamine, and benzodiazepine use disorders, were also entered into the same model. The overall model was significant (χ213 = 167.83, P = .01) and adequately fit the data (−2logl = 2,457.26; Hosmer-Lemeshow χ28 = 10.10; P = .258). The model had 80.1% accuracy for classifying cases and accounted for 9.2% variance in suicide risk. Of the entered variables, schizophrenia (B = 0.323, Wald χ21 = 4.61, P = .03, Exp[B] = 1.38), MDD (B = –1.21, Wald χ21 = 98.90, P < .001, Exp[B] = 0.297), bipolar disorder (B = –0.52, Wald χ21 = 10.24, P < .001, Exp[B] = 0.594), and cocaine use disorder (B = –0.294, Wald χ21 = 5.34, P = .02, Exp[B] = 0.745) were significant predictors of suicide risk. Surprisingly, those with schizophrenia had decreased risk for suicide. As expected, patients with MDD, bipolar disorder, and cocaine use disorder had increased risk of suicide.
Hospital Status and Suicide Risk
The association of hospital admissions and length of stay with suicide risk was examined by entering the number of hospital admissions and the total number of days spent in the hospital as dependent variables in a MANOVA with suicide risk as the independent variable. The overall MANOVA model showed a significant association (Wilks λ =0.973, F2,4706 = 64.97, P < .001, ηp2 = 0.03). Follow-up univariate tests showed a significant group difference between suicide and nonsuicide groups on both the number of admissions (F1,4707 = 129.92, P < .0001) and the total number of hospital days (F1,4707 = 41.29, P < .0001). The suicide group had significantly (P < .0001) more mean (SD) admissions (2.44 [2.58]) than the nonsuicide group (1.65 [1.56]). The suicide group also spent significantly (P < .0001) more days (25.36 [32.17]) in the hospital than the nonsuicide group (17.96 [28.68]).
Childhood Physical and Sexual Abuse and Suicide Risk
The associations of childhood physical and sexual abuse with suicide risk were also examined with BLR. Whereas childhood physical and sexual abuse was a binary variable, type of abuse was treated as a polytomous variable with 4 categories: none, physical, sexual, and both physical and sexual. The overall model was significant (χ24 = 33.63, P < .001) and a good fit to the data (−2logl = 4,019.05; Hosmer-Lemeshow χ23 = 0.091; P = .993), suggesting an association with suicide risk. Abuse variables accounted for 1.2% variance in suicide risk. Among the entered variables, childhood physical and sexual abuse, but not type of abuse, had a significant association with suicide risk (B = 0.574, Wald χ21 = 10.86, P < .001, Exp[B] = 1.78) and was associated with an increased risk of suicide attempt.
All Predictors and Suicide Risk
Significant predictors in previous analyses were included in a BLR model to identify the best set of predictors of suicide risk in the sample. This final model, which used forward selection with likelihood ratio to select the best variables, was significant (χ24 = 248.04, P < .001). The model identified the combination of childhood physical and sexual abuse, number of admissions, schizophrenia (less risk), and MDD as the best predictors of suicide risk. This combination of variables accounted for 9.9% variance in suicide risk and correctly classified 83% of cases into respective suicide versus nonsuicide risk groups.
DISCUSSION
In this sample of VA patients with at least 1 psychiatric hospitalization, approximately 29% of the sample had childhood physical or sexual abuse, and 16% had at least 1 suicide attempt. The number of psychiatric admissions and the total number of days on the psychiatric inpatient unit were significantly higher in the suicide group compared to the nonsuicide group. As hypothesized, childhood physical and sexual abuse was a significant predictor of suicide risk; however, the type of abuse did not differentially predict suicide risk. In the final model, childhood physical and sexual abuse, number of psychiatric admissions, and diagnoses of MDD were the best predictors of suicide risk. These findings are consistent with previous studies.8,12,13 Although there are other similar studies,14,15 our study is the first among veterans that has predicted childhood physical and sexual abuse as an increased risk for suicide. To our knowledge, this study is the first to predict number of psychiatric inpatient admissions with an increased suicide risk.
In our study, although not significant in the final model, patients with cocaine use disorder and bipolar disorder had increased risk of suicide. Factors associated with increased risk of suicide among cocaine users include depression, cocaine withdrawal, comorbid alcohol or opioid use disorder, history of childhood trauma, physical disorders, personality traits (introverted, neurotic, and hostile), and family history of suicide.16,17 In a prior study,18 childhood traumas were found to be significantly associated with suicidal behavior among 100 adult male cocaine-dependent patients. This finding is consistent with our results in a veteran population. Consistent with our findings, other studies19,20 have shown increased risk of suicide in bipolar disorder.
Schizophrenia is typically associated with high suicide risk.21,22 In contrast, we found decreased suicide risk in those with schizophrenia, which is an intriguing finding. We speculate that veterans with schizophrenia are a different subset with different risks (eg, greater access to care, higher functioning, more support in the form of occupational therapy groups 1–2 times a week). The criteria for admission to a psychiatry inpatient unit at a VA hospital is less stringent compared to other hospitals. Also, the length of stay is usually longer compared to other hospitals because there is no pressure to discharge, as the stay is not paid by insurance. Another plausible explanation is that a substantial portion of our cohort had deficit (primary negative symptoms) schizophrenia, which is associated with a lower risk for suicide.23,24 This finding was recently corroborated in a study25 wherein deficit schizophrenia (N = 128) was associated with fewer suicide attempts compared to nondeficit (N = 578) schizophrenia. In a prospective study26 of carefully phenotyped participants with schizophrenia at the Atlanta VAMC, 57% (32/56) had deficit schizophrenia, which is an indirect estimate of the proportion of our Atlanta VAMC schizophrenia population with deficit syndrome. However, this explanation is only a speculation, because we did not analyze deficit versus nondeficit schizophrenia (no data were available). Significantly higher Childhood Trauma Questionnaire (CTQ) scores were reported in 50 people with schizophrenia who had attempted suicide than in 50 people with schizophrenia who had never attempted suicide.27
Consistent with our findings, research has shown childhood physical and sexual abuse to be associated with increased suicide risk. In the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC)28 with 34,653 US adults, childhood physical and sexual abuse was associated with suicide attempts in 2.64% of survey respondents. In the same survey,29 childhood maltreatment was significantly associated with an increased risk for attempting suicide and an earlier age at first suicide attempt, independent of psychopathology. In a cross-sectional study8 of subjects with a history of childhood abuse (N = 1,380), the prevalence of suicide risk was 11.5%. Suicide risk was significantly increased in subjects with a history of sexual abuse (odds ratio [OR] = 3.4) and physical abuse (OR = 3.1). The authors4 concluded that preventing early trauma may reduce suicide risk in young individuals. In a 30-year longitudinal study7 of 900 individuals, childhood sexual abuse was significantly associated with increased rates of suicidal ideation and attempts. In a study13 of 473 patients with MDD aged 18–60 years, suicide risk was observed in 16.3%. Suicide risk was independently associated with childhood emotional abuse and neglect and sexual abuse but not with physical abuse and neglect.13 This finding is important because the most common diagnosis in our study was MDD.
Childhood physical and sexual abuse is more common in women than men.10,30,31 In a meta-analysis32 of 9 studies, suicide rates were higher among female veterans than women in the general population. Women with SUD had a higher hazard ratio for completed suicide than men with SUD, particularly those with a psychiatric diagnosis.32 In the current sample, sex was not a significant predictor of suicide risk. However, the majority of our patients were male, as is expected in a VA sample.
In a meta-analysis33 of 7 longitudinal studies published in the last 10 years on the association between childhood trauma and lifetime suicide attempt risk, sexual, physical, and emotional abuse and physical neglect were significantly associated with suicide risk. Emotional neglect and a broken home were not significantly associated with suicide risk. The childhood traumas that contributed most to suicide risk in later life were (in order of frequency) physical, emotional, and sexual abuse and physical neglect.33 A limitation of our study is that we did not analyze emotional abuse and physical neglect because these data were unavailable.
Strengths of this study include the large sample size of 4,709 patients and that it is the first to examine childhood physical and sexual abuse and suicide risk in veterans. This study has several limitations. This was a retrospective study; hence, assessments with validated rating scales such as the CTQ were not performed. The patients may have underreported their abuse experiences34 because of guilt and shame. Also, patients may overreport to receive empathy or benefits. However, a prior study35 indicated that there was convergent validity for childhood abuse documented in clinical case notes versus self-report on a questionnaire. Because our study was retrospective, we cannot be sure how the admitting clinician asked the questions to gather information for the prompt in the admission write-up template. Because gathering the abuse history is a mandatory field in the admission note, it is likely to be elicited and documented. Hence, the possibility of reporting bias with clinicians asking these questions cannot be ruled out. In addition, abuse history was analyzed as a dichotomous variable; severity and frequency were not documented in a consistent manner that would have allowed these characteristics to be analyzed in our sample. For this reason, the effects of cumulative trauma could not be evaluated. Diagnoses included in this study were clinical diagnoses taken from the chart. The analyses were not adjusted for military sexual trauma, combat experience, and diagnoses with high rates of suicidal behavior such as depression and PTSD. Another limitation is that specific information about the perpetrator of the abuse was unavailable. We also did not examine adult physical and sexual abuse, which may be associated with suicide risk as well, because it would be difficult to separate the effects of this type of abuse from the veterans’ combat experience. Finally, we had no data on abuse and the severity and lethal modes of suicidal behavior.
CONCLUSIONS AND FUTURE DIRECTIONS
To our knowledge, this study is the first to shed light on the interaction of childhood physical and sexual abuse and suicide risk in a large cohort of veterans. The results from this study may lead to more focused programs with equal emphasis on psychotropics and psychosocial interventions. Such holistic programs are likely to help people with a history of abuse and prevent suicide.
Submitted: April 24, 2018; accepted June 7, 2018.
Published online: August 23, 2018.
Author contributions: Drs Koola and Duncan designed the study. Dr Koola collected the first year of data (2004–2005), and Dr Sebastian collected the latter 9 years of data (2005–2014). Dr Duncan constructed customized databases to process and compile the data. Dr Ahmed performed the statistical analyses. Drs Koola and Ahmed wrote the first draft of the manuscript, equally contributed to the manuscript preparation, and are joint first authors. All authors edited, made intellectual contributions, and approved the final version of the manuscript.
Potential conflicts of interest: Dr Duncan has received research support for work unrelated to this project from Posit Science, Auspex, and Teva. Drs Koola, Ahmed, and Sebastian report no conflicts of interest related to the subject of this article.
Funding/support: This material is the result of work supported with resources and the use of facilities at the Atlanta Veterans Affairs Medical Center, Decatur Georgia, including the Research, Mental Health, and Rehabilitation Research and Development Service Lines and the Center for Visual and Neurocognitive Rehabilitation. Dr. Duncan is a full time attending psychiatrist in the Mental Health Service Line at the Atlanta Veterans Affairs Medical Center, Decatur, Georgia. Additional infrastructure support was provided by the Department of Psychiatry and Behavioral Sciences of the Emory University School of Medicine, Atlanta, Georgia.
Role of the sponsor: The supporters had no role in the design, analysis, interpretation, or publication of this study.
Disclaimer: The content is solely the responsibility of the authors and does not necessarily represent the official views of the Department of Veterans Affairs.
REFERENCES
1. Reuters. US military veteran suicides rise, one dies every 65 minutes. https://www.reuters.com/article/us-usa-veterans-suicide/u-s-military-veteran-suicides-rise-one-dies-every-65-minutes-idUSBRE9101E320130202. Accessed August 3, 2018.
2. Nock MK, Deming CA, Fullerton CS, et al. Suicide among soldiers: a review of psychosocial risk and protective factors. Psychiatry. 2013;76(2):97–125. PubMed CrossRef
3. Centers for Disease Control and Prevention. Suicide rising across the US. More than a mental health concern. https://www.cdc.gov/vitalsigns/suicide/index.html. Accessed August 3, 2018.
4. World Health Organization. Suicide. http://www.who.int/news-room/fact-sheets/detail/suicide. Accessed August 3, 2018.
5. American Foundation for Suicide Prevention. Facts and figures. https://afsp.org/about-suicide/suicide-statistics/. Accessed July 27, 2018.
6. Nock MK, Hwang I, Sampson NA, et al. Mental disorders, comorbidity and suicidal behavior: results from the National Comorbidity Survey Replication. Mol Psychiatry. 2010;15(8):868–876. PubMed CrossRef
7. Fergusson DM, McLeod GF, Horwood LJ. Childhood sexual abuse and adult developmental outcomes: findings from a 30-year longitudinal study in New Zealand. Child Abuse Negl. 2013;37(9):664–674. PubMed CrossRef
8. Barbosa LP, Quevedo L, da Silva GG, et al. Childhood trauma and suicide risk in a sample of young individuals aged 14–35 years in southern Brazil. Child Abuse Negl. 2014;38(7):1191–1196. PubMed CrossRef
9. Harford TC, Yi HY, Grant BF. Associations between childhood abuse and interpersonal aggression and suicide attempt among US adults in a national study. Child Abuse Negl. 2014;38(8):1389–1398. PubMed CrossRef
10. Koola MM, Qualls C, Kelly DL, et al. Prevalence of childhood physical and sexual abuse in veterans with psychiatric diagnoses. J Nerv Ment Dis. 2013;201(4):348–352. PubMed CrossRef
11. McLellan AT, Luborsky L, Woody GE, et al. An improved diagnostic evaluation instrument for substance abuse patients: the Addiction Severity Index. J Nerv Ment Dis. 1980;168(1):26–33. PubMed CrossRef
12. Walsh G, Sara G, Ryan CJ, et al. Meta-analysis of suicide rates among psychiatric in-patients. Acta Psychiatr Scand. 2015;131(3):174–184. PubMed CrossRef
13. Dias de Mattos Souza L, Lopez Molina M, Azevedo da Silva R, et al. History of childhood trauma as risk factors to suicide risk in major depression. Psychiatry Res. 2016;246:612–616. PubMed CrossRef
14. Ursano RJ, Kessler RC, Naifeh JA, et al. Associations of time-related deployment variables with risk of suicide attempt among soldiers: results from the Army Study to Assess Risk and Resilience in Servicemembers (Army STARRS). JAMA Psychiatry. 2018;75(6):596–604. PubMed CrossRef
15. Guina J, Nahhas RW, Mata N, et al. Which posttraumatic stress disorder symptoms, trauma types, and substances correlate with suicide attempts in trauma survivors? Prim Care Companion CNS Disord. 2017;19(5):17m02177. PubMed CrossRef
16. Roy A. Characteristics of cocaine-dependent patients who attempt suicide. Am J Psychiatry. 2001;158(8):1215–1219. PubMed CrossRef
17. Sofuoglu M, Dudish-Poulsen S, Brown SB, et al. Association of cocaine withdrawal symptoms with more severe dependence and enhanced subjective response to cocaine. Drug Alcohol Depend. 2003;69(3):273–282. PubMed CrossRef
18. Roy A. Childhood trauma and suicidal behavior in male cocaine dependent patients. Suicide Life Threat Behav. 2001;31(2):194–196. PubMed CrossRef
19. Hawton K, Sutton L, Haw C, et al. Suicide and attempted suicide in bipolar disorder: a systematic review of risk factors. J Clin Psychiatry. 2005;66(6):693–704. PubMed CrossRef
20. Webb RT, Lichtenstein P, Larsson H, et al. Suicide, hospital-presenting suicide attempts, and criminality in bipolar disorder: examination of risk for multiple adverse outcomes. J Clin Psychiatry. 2014;75(8):e809–e816. PubMed CrossRef
21. Gut-Fayand A, Dervaux A, Olié JP, et al. Substance abuse and suicidality in schizophrenia: a common risk factor linked to impulsivity. Psychiatry Res. 2001;102(1):65–72. PubMed CrossRef
22. Iancu I, Bodner E, Roitman S, et al. Impulsivity, aggression and suicide risk among male schizophrenia patients. Psychopathology. 2010;43(4):223–229. PubMed CrossRef
23. Fenton WS, McGlashan TH. Antecedents, symptom progression, and long-term outcome of the deficit syndrome in schizophrenia. Am J Psychiatry. 1994;151(3):351–356. PubMed CrossRef
24. Tek C, Kirkpatrick B, Buchanan RW. A five-year follow-up study of deficit and nondeficit schizophrenia. Schizophr Res. 2001;49(3):253–260. PubMed CrossRef
25. Ahmed AO, Strauss GP, Buchanan RW, et al. Schizophrenia heterogeneity revisited: clinical, cognitive, and psychosocial correlates of statistically-derived negative symptoms subgroups. J Psychiatr Res. 2018;97:8–15. PubMed CrossRef
26. Taylor N, Hollis JP, Corcoran S, et al. Impaired reward responsiveness in schizophrenia [published online ahead of print March 8, 2018]. Schizophr Res. PubMed CrossRef
27. Roy A. Reported childhood trauma and suicide attempts in schizophrenic patients. Suicide Life Threat Behav. 2005;35(6):690–693. PubMed CrossRef
28. Hoertel N, Franco S, Wall MM, et al. Childhood maltreatment and risk of suicide attempt: a nationally representative study. J Clin Psychiatry. 2015;76(7):916–923, quiz 923. PubMed CrossRef
29. Hoertel N, Franco S, Wall MM, et al. Mental disorders and risk of suicide attempt: a national prospective study. Mol Psychiatry. 2015;20(6):718–726. PubMed CrossRef
30. Coverdale JH, Turbott SH. Sexual and physical abuse of chronically ill psychiatric outpatients compared with a matched sample of medical outpatients. J Nerv Ment Dis. 2000;188(7):440–445. PubMed CrossRef
31. Villagrá P, Fernández P, García-Vega E, et al. Dual diagnosis in prisoners: childhood sexual and physical abuse as predictors in men and women [published online ahead of print November 27, 2013]. Int J Offender Ther Comp Criminol. PubMed CrossRef
32. Chapman SL, Wu LT. Suicide and substance use among female veterans: a need for research. Drug Alcohol Depend. 2014;136:1–10. PubMed CrossRef
33. Zatti C, Rosa V, Barros A, et al. Childhood trauma and suicide attempt: a meta-analysis of longitudinal studies from the last decade. Psychiatry Res. 2017;256:353–358. PubMed CrossRef
34. Williams LM. Recall of childhood trauma: a prospective study of women’s memories of child sexual abuse. J Consult Clin Psychol. 1994;62(6):1167–1176. PubMed CrossRef
35. Fisher HL, Craig TK, Fearon P, et al. Reliability and comparability of psychosis patients’ retrospective reports of childhood abuse. Schizophr Bull. 2011;37(3):546–553. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!


